
Selecting the best gait device for a young patient can be similar to buying a new car. First, we are attracted to a car we see on the road or in ads. Then, we listen to the opinions of friends’ first-hand experiences, or read reviews in consumer reports or online to help make comparisons. But the ultimate step in making a purchasing decision is the test drive.
At Kennedy Krieger Institute, therapists actively help patients navigate the decision-making process for gait assist devices. Our physical therapy clinic receives referrals from medical programs that serve the needs of children with developmental and physical disabilities, as well as those with very rare conditions. As a result, we are often faced with identifying very special needs and finding gait devices with unique features. Patients would like devices that can be used in the home, school, and community settings, and their parents often want to compare every possible option. It is not uncommon for a family to come to a PT with an assistive device in hand, acquired through another facility or vendor. Often the device is inappropriate for the patient, and the families frequently report that they were never given the opportunity to walk in the device and try it out before purchase.
In our clinic we work with many durable medical equipment (DME) vendors, as well as the manufacturers and their representatives, and consider them as our partners in the test-drive or decision-making process—the patient is on one end, the manufacturers on the other, and the therapist is right in the middle.
A CASE IN POINT
Recently, I worked with a 9-year-old girl with a rare condition. She and her family had been living abroad for some time, and the girl had outgrown much of her current equipment. The girl’s mother wanted my input on several therapy issues, and was especially interested in finding a gait device that her daughter could safely use for home and school (with the help of her one-on-one aide). I recommended devices based solely on my examination of the patient. When I shared one of the first suggestions that came to my mind—an expensive custom gait assist device that functions like a reciprocal gait orthosis—the mother replied: “Oh, we have one of those. It didn’t work.” She went on to describe the efforts to get insurance to approve the device, a burdensome fitting procedure, and a long process that took entirely too much time and effort. Afterward, the mother said that her daughter could not use the device, and that her care providers were intimidated by its complexity. As with many new patients, this girl had not been given the opportunity to try the device before it was purchased.
This incident was an important reminder for me of how necessary it is for all patients to try a device—to test drive it—before ordering. Ideally, “test driving” a new piece of gait assist equipment should occur over several occasions, in a variety of settings. This enables finding a device that is a good fit for the patient, and gives the caregiver a sense of the responsibility that will fall to them, as well as the extent of training they will need.

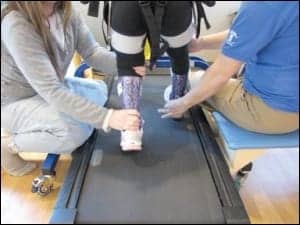
Author Karen Good, PT, OCS (foreground), examines a young patient to determine an appropriate gait device for her needs.
This wonderful little girl would continue to challenge me to think broadly and out of the box. We tried several gait assist units, all with various components and add-on features. She seemed to need more support than these devices provided, but every attempt to add a sling or seat component resulted in her sitting. I considered alternatives that could provide increased patient safety and security, as she had a specific fear of falling, while also addressing her mother’s desire to have a device that was easy for the school aide to use. We finally tried an assist device that had a dynamic body weight support component. I was fortunate to be able to have the inventor of the unit and the owner of the company come to Kennedy Krieger Institute to help us fit the child in the device, as well as trial some of the newer components available. This opportunity helped to illustrate the critical value of a test drive; while my patient could walk longer distances and more safely in a dynamic partial weight-bearing unit, her gait pattern was better in the other devices.
As a result, I turned my attention to other options—and even a different plan of care. I tabled the gait assist device decision for a later date and focused on her impairments. We began a bout of body-weight-supported walking on the treadmill, using a therapy device with a suspension system to provide proper upright posture, balance, weight-bearing, and safety during therapy. This enabled the patient to reach a higher level of function. She gained endurance, symmetry, and a significant reduction in caregiver assistance to walk. I was astounded by her increase in walking distance, and she seemed to gain a higher level of confidence in herself. This training has allowed us to now consider a wider variety of devices. We continue to try various devices; because we have the opportunity to trial them multiple times, I know that we will arrive at a better decision in the end than would have been otherwise possible. There is tremendous value to a test drive.
MAKING TEST DRIVES AVAILABLE TO PATIENTS
Unlike auto dealerships, therapy clinics cannot stock their closets with a variety of assist devices—especially since a single device might be used only once or twice a year. We also cannot afford to have all of the adaptations, features, and sizes of every walker. However, resourceful clinicians can increase the variety of equipment options we can offer our patients to test drive.
Here are a few ideas:

The author, center, fits her young client in a body-weight supported gait device for a “test drive.”
- Share equipment among programs in a large organization, or share between small clinics (including competitors).
- Encourage an equipment-recycling program, whereby patients who have outgrown the need for a device can donate it to the clinic. This is a great way to secure rarely used devices or customized gait assist devices.
- Record and share patient testimonials including a rating on features and caregiver burden.
- Create relationships with manufacturers’ representatives or vendors. These individuals can request “demo” equipment for your patient to try on a limited basis.
- Ask the manufacturer. When I first became a physical therapist, I researched some specialized gait devices that I wanted to try with my patients. I naively wrote a letter stating my intentions, the device I wanted, and my reasoning, explaining that my clinic had not budgeted for specialized gait devices. I asked the manufacturer to send me devices to try with patients and was astounded by the walkers, canes, crutches, and specialized gait devices I received in return.
HOW IT ALL COMES TOGETHER
Physical therapists assess children’s issues across the spectrum of neurological, genetic, or post-traumatic. Patients and families value the therapists as experts and advocates. The physical therapist is uniquely suited to use the International Classification of Function (ICF) model and consider all of the variables at play for the best DME recommendations, leading up to the “test drive.”
WHAT TO CONSIDER WHEN RECOMMENDING DME:
Patient specific (intrinsic) characteristics:
- Current and projected level of function
- Diagnosis (progression)
- Patient preference
- Age/projected growth
Environmental/modifiers (extrinsic) characteristics:
- Funding/benefits
- Caregiver (capacity to lift or fold device, assist patient)
- Transportation (what device will fit)
Additionally, it is helpful to consider some general rules of thumb when focusing on durable medical equipment:Walkers: Walkers are for youngsters who can bear their own weight through their legs, yet often have compromised balance and the ability to move their feet when standing. Available in a variety of styles to suit a child’s needs, walkers are portable and usually feature height adjustment. They can be purchased with two to four wheels (or no wheels), with or without hand grips and brakes, and can be pushed by the user from inside or behind the frame. The benefits of walkers are numerous, as they help youngsters with the ability to stand and the ability to experience independent mobility.
Gait trainers: Designed for beginning gait and pre-gait advancements, these devices will help the pattern of walking, while offering trunk support. They encourage early cognitive and learning development, help increase spatial awareness and head control, and develop cardiopulmonary strength and condition, while helping to improve balance and functional gait. These systems are available with numerous features, from weight-bearing to partial weight-bearing to those offering anterior and posterior support. Gait trainers can help improve a child’s confidence and independence and decrease the amount of assistance the child requires.

Standing frames: Intended to reduce or prevent contracture and/or integumentary complication, these devices help teach a child the skills and postural control needed for standing and independent mobility. Standing devices also help young patients improve vertical access for psychological, cardiovascular, musculoskeletal strength, and a variety of other reasons. In addition, standers are available in several types to suit a child’s specific needs, including: sit-to-stand standers; prone, supine, and multiposition standers; mobile standers; and active standers.
Strollers: These devices offer the opportunity for adaptability or safety options for the disabled patient to be transported dependently. Available in folding and lightweight models, tilt-in-space, fixed and upright positions, and fix tilt, pediatric strollers are portable, and can be customized with a variety of accessories for a child’s specific upper body and trunk stabilities, as well as physical conditions that require special positioning.
While it is hard to predict how much time and how many visits it will take to prescribe the perfect gait assist device, therapists should take their time; there is no benefit in rushing a decision. Prescribing a gait assist device must be based on empirical evidence and adhere to the ICF.
And that means a test drive.
Karen Good, PT, OCS, is a senior physical therapist at the Kennedy Krieger Institute (www.KennedyKrieger.org) in Baltimore, and boasts more than a decade of experience helping individuals with a range of disabilities, including cerebral palsy, spinal cord injury, spina bifida, and other neurological injuries and disorders. Her special clinical interests include the analysis of gait and therapies to improve walking, functional electronic stimulation, and aquatic therapy. In addition, Good is an instructor in body-weight-supported gait therapy for Mobility Research. For more information, contact .





