
Meghan Fahey, physical therapist at the Shirley Ryan AbilityLab, guides a patient through an obstacle course that simulates the skills needed for everyday walking, including steps and ramps.
By Meghan Fahey, PT, DPT
Currently, 86% of scientific discoveries—countless approaches, treatments, and even potential cures—never make it out of the lab. The Rehabilitation Institute of Chicago (RIC)—a specialty, nonprofit hospital serving patients with the most severe, complex conditions—sought to change this statistic in a profound way. On March 25, 2017, RIC officially became known as the Shirley Ryan AbilityLab, opening the doors to its cutting-edge research hospital of the same name. The hospital is aiming to utilize translational research at its highest level. And, as a physical therapist, I have a front-row seat.
A Radical Approach to Rehabilitation
By embracing a translational model, the Shirley Ryan AbilityLab incorporates research into clinical practice throughout the system of care. Inside the 1.2 million-square-foot research hospital are doctors, scientists, physical therapists, speech therapists, occupational therapists, wheelchair specialists, engineers, and technologists all working together in common spaces.
In the traditional model, it may take many years for research findings to be incorporated into clinical care. This new hospital has been explicitly designed to enable translation of research into care faster. Conversations between researchers and clinicians are ongoing and happen at the ground level, as they work in tandem to identify and prioritize problems that need solving now. Research is inspired by the clinical challenges that scientists, themselves, observe. Patients receive treatment right next to researchers, offering these scientists a firsthand view of clinical problems. Clinicians are aware of research findings more quickly. As a result, more patients are involved in research, and more research is translated into patient care.
Far too often in healthcare, collaboration among researchers and clinicians happens by chance. At the Shirley Ryan AbilityLab, the novel, open-concept space is meant to allow collaboration among these groups to happen instead by choice.
Patients have always been the focus of the entire team. Now, they stand to gain even more as a result of heightened collaboration between researchers and clinicians. The goal: better, faster outcomes.
A Tested Model
Integrating scientists and clinicians—great in theory, but can it work in reality? Will cultures truly merge, and will the process of scientific inquiry be altered?
In 2012, a mission was established to answer these questions and began a living experiment by outfitting the old hospital with an “ability lab,” an applied research and therapeutic space, on one floor. The setup allowed researchers to work shoulder-to-shoulder with patients, doctors, and therapists.
The space was equipped with the latest rehabilitation technologies, from an anti-gravity gait track that covered the entire floor, to sophisticated robotic equipment to assist with walking and arm therapy for a range of patients, including those recovering from brain or spinal cord injuries, stroke, or neuromuscular deficits. The singular focus was to accelerate the translation of research discoveries to achieve the best recoveries for patients.
I was one of the therapists on the floor, and had an opportunity to study the shift that took place firsthand. I observed transformations in many forms.
For instance, one of the scientists had an idea: What if training regimens were individualized for patients, focusing on intensity, practice, and time? It is known that more is better, and that it is related to outcomes. Instead of waiting to read about this epiphany several years later once a study had been published, more stepping opportunities were integrated into therapy sessions right away, leveraging body-weight-supported treadmills, a hallway gait track system, and a dedicated team of physical therapists. It was found that steps trump all variables (age, strength of key muscles, etc), and that early, intensive practice is key to recovery. As a result, patients began to get 1,500 steps per session—six times more than the average.
This is one example of how a translational approach to research has directly benefited patients. It has also influenced the approach and technology the clinical staff leverages today. For 5 years, the ability lab served as a dynamic test bed—and key validation tool—shaping the vision and design for the new hospital.
A Novel Structure
This spring, vision became a reality when the Shirley Ryan AbilityLab opened, embracing this integrated approach throughout. Out of the gate, the facility’s patient capacity increased by 40%, and that was just the beginning.
The Shirley Ryan AbilityLab is designed with five Innovation Centers focused on areas of biomedical science with great promise. These centers include the Brain Innovation Center; Spinal Cord Innovation Center; Nerve, Muscle & Bone Innovation Center; Pediatric Innovation Center; and Cancer Rehabilitation Innovation Center. Patient care takes place in these Centers, aided by the latest smart-room, bed-surface, electronic, technical, mobility, and therapeutic devices and equipment.
The ability lab model that was piloted in the old hospital has been replicated in five unique lab designs. Each is configured based on a targeted function and the type of experimentation taking place therein:
• Think + Speak Lab: Treatment for fundamental brain functions—arousal, lucidity, awareness, thinking, communication, perception, memory, and learning.
• Legs + Walking Lab: Improvement of locomotion, gait and walking via trunk and pelvis stability; positioning and control of the hips, knees, and ankles; as well as stepping and propulsion.
• Arms + Hands Lab: Improvement of hand function and movement, body and upper-limb coordination, strength, reaching, shoulder biomechanics, and hand/finger control.
• Strength + Endurance Lab: Improvement of stamina and resilience, complex motor and endurance activities, coordination, and higher-level activities of daily living (eg, cooking, housekeeping, exercise, sports).
• Pediatric Lab: Treatment for all of the above, with a customized approach for the developing brains, bodies, and conditions unique to children (infants to teens).
In each of these working labs, interdisciplinary teams develop new research and insights to help patients gain more function, achieve better outcomes, and enjoy greater ability and independence. They feature current technology specifically tailored to the patient populations served. For example, overhead gait tracks allow therapists to facilitate gait training for patients who require significant amounts of assistance or body-weight support to advance their legs. These tracks also allow physical therapists to challenge patients working on higher-level balance activities with obstacles and variable stepping (sideways, backward, stop/start, etc), all while maintaining confidence that patients cannot fall while inside the track system.
Three of the five ability labs are 25,000 square feet and two stories high. At the focal point of each is a staircase—a powerful symbol and tool for improving movement, strength, and function. Chicago Flyhouse, a company known for building rigging systems for theaters, was chosen as a partner to design a one-of-a-kind four-point suspension system over these “Ability Stairways.” It is equipped with an antigravity lift track to support patients’ weight as they relearn to climb stairs. This system is the first of its kind in rehabilitation, safely facilitating stair training earlier in the course of patients’ recoveries.
The Legs + Walking Lab touts a robotic treadmill. Patients, suspended in a harness, are attached to straps that move the legs in a natural walking pattern while a computer controls the pace of walking and measures the body’s response to movement. By controlling the repetitive walking pattern, the robotic treadmill helps the brain and spinal cord work together to reroute signals that were interrupted by injury or illness.
Multiple labs include functional electrical stimulation bicycles. These bikes, which provide electrical stimulation to targeted muscle groups on both the upper and lower extremities, promote circulation and bone density in the affected muscle groups. Importantly, they also reinforce the long-term benefits and new opportunities for exercise after an illness.
I participate in various research studies as a blinded rater to help assess if the research variable is making a clinical impact on the patient. With the help of principal investigators and other research scientists, I have written grants and manuscripts to continue to publish new discoveries from the Shirley Ryan AbilityLab.
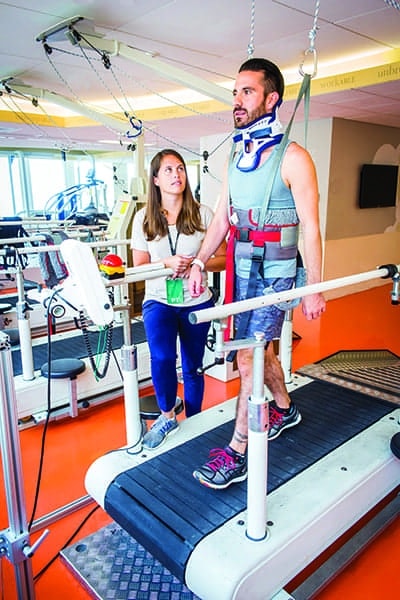
A patient at the Shirley Ryan AbilityLab is encouraged by physical therapist, Meghan Fahey, as he practices his walking ability and endurance.
Specialized Focus
With the comprehensive design of labs and Innovation Centers, the Shirley Ryan AbilityLab is equipped to serve a wide variety of patient populations, including those recovering from stroke, spinal cord injury, traumatic brain injury, and cancer, as well as those with degenerative conditions (eg, Parkinson’s disease, multiple sclerosis), amputation, cardiovascular disease, and those who are considered medically complex.
Patients also benefit from programs and centers specializing in various conditions. For example, the Intensive Aphasia Therapy Program is a month-long program offering therapy that leverages the latest evidence-based information and research from the hospital’s Center for Aphasia Research and Treatment. A “Second Look” program is also offered for those with spinal cord injuries (SCI). Designed by the facility’s team of SCI experts, this program evaluates individuals to assess their current condition and make recommendations for next steps in treatment. The program leverages advancements in everything from spasticity management to new walking exoskeleton devices. Additionally, the facility’s doctors and scientists have been working on bionic limbs for more than a decade with very early-stage funding from the Defense Advanced Research Projects Agency and the Army, creating the first bionic arm, hand and leg—all of which are mind-controlled devices. We now have several matured generations of these high-tech prosthetics in use today.
There are myriad diseases, conditions, and injuries presenting that can only be solved at the cellular level. Similarly, what we are learning about the brain’s ability to heal is very exciting. To patients with conditions like cerebral palsy, Parkinson’s disease, or traumatic brain injury, staff members at the facility are accelerating research to unlock these mysteries. Notably, the new hospital has a “wet” lab right inside, which equips staff members to study living human cells, to use biologics, pharmacologics, stem-cell and other technologies—all areas holding immediate and exciting promise. In this wet lab, scientists work on stem-cell biology and muscle physiology. Live tissue samples can now be taken from willing patients for study. This will increase the number and speed of discoveries because scientists are co-located with patients.
A biologics lab is a very unusual space for a hospital to have, let alone a rehabilitation hospital. Generally, work of this nature is conducted off-site in a research building, but the desire here was to bring research closer to patients so they may benefit from it sooner. The fact that the Shirley Ryan AbilityLab created its own custom wet lab within its facility is a distinguishing mark of the facility.
As a physical therapist engaged in this radically new model of care, I am eager to continue offering evidence-based practice to our various patient populations. By utilizing our researchers’ scientific insight and integrating it with my clinical insight, we are finding solutions sooner, helping patients faster. At the end of the day, patients are getting stronger, more independent, and achieving their goals more efficiently because research has been added to the clinical teams that provide their care. RM
Meghan Fahey, PT, DPT, earned a Doctorate in Physical Therapy from University of Illinois at Chicago and a bachelor’s degree in Rehabilitation Psychology from University of Wisconsin-Madison. She practices at the Shirley Ryan AbilityLab (formerly Rehabilitation Institute of Chicago), and specializes in treating patients with neurologic conditions in the inpatient setting. She is a member of the American Physical Therapy Association and Illinois Physical Therapy Association. For more information, contact [email protected].




