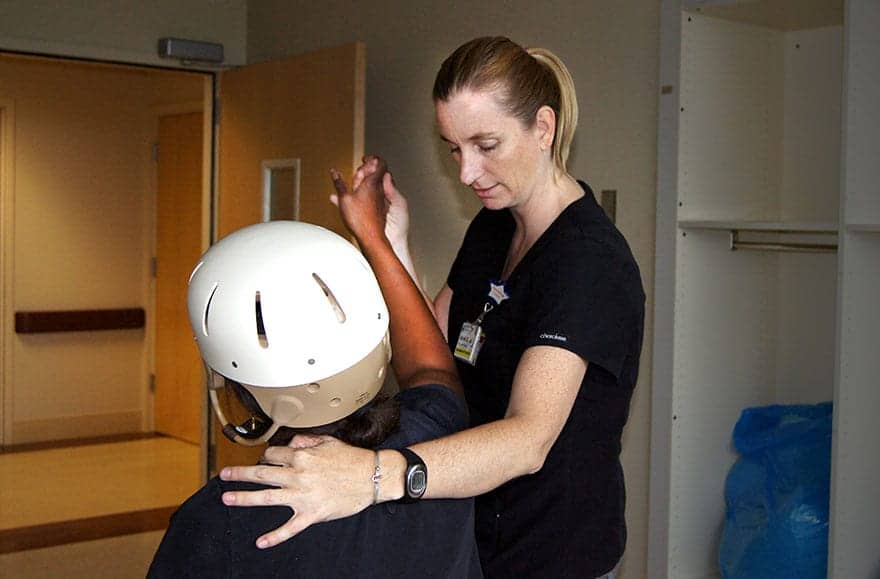
Controlling the aspects of sensation can smooth recovery for patients who exhibit challenging behaviors post-injury.
by Sarah Sanderman, MOTR/L
“Possibly, he was in a state of second growth and recovery, and was constantly assimilating nutriment for his spirit and intellect from sights, sounds and events which passed as a perfect void to persons more practiced with the world.”
—Nathaniel Hawthorne
Through life experiences, we learn to filter out the excess or noncontributory stimulation from the stimulation we need to attend to. Imagine suddenly losing that filtering ability. When adults experience an acquired or traumatic brain injury or a cerebral vascular incident, they are looking at months and years of recovery, not days and weeks. The first few weeks and months will play an important part in overall rehabilitation. One critical factor in this rehabilitation is the environment in which the patient is allowed to recover.
Patients who are most appropriate for trialing a controlled stimulation unit are those who exhibit behaviors including restlessness, agitation, aggression, hallucinations (auditory or visual or both), confabulation, or sleep/wake disturbances. This is not a complete list, but a good indication of who may be most appropriate. Patients who are moving through the Rancho Los Amigos Scale and are at a Level IV rising to a V or VI will benefit from this type of structure. This setting is used for both acquired and traumatic brain injuries when the Rancho scale is not a factor.
THE PHYSICAL SPACE
In designing a room for a controlled stimulation unit, it is important to keep in mind the more aspects of sensation that can be controlled, the better the room will suit the patient. This sounds as if it could be difficult in an established hospital or rehab setting, but in actuality can be easier and less costly than one might imagine. Natural light should be available and regulated with the use of tinted windows, shades, blinds, or curtains. Use nonharsh lighting such as a table lamp or a tall deflecting halogen lamp, instead of fluorescent lighting or spot lighting. For the acutely injured, remove any wall art, calendars, clocks, televisions, or radios. A favorite blanket or pillow may be used on the bed.
An attached, private bathroom will limit the possibility of increased stimulation in a shared bathroom or shower room. The bathroom should be fitted with the most appropriate adaptive equipment for bathing and toileting, such as grab bars, shower chairs, commode chairs, and transfer devices. All bathroom safety items should be designated for that patient’s sole use to limit traffic in and out of the room.
Silencing overhead pages and muting the audible alarms on monitors are often the most challenging aspect of decreasing sound in a room. The hallway should be designated as a “No Talking” zone, and if noisy carts and transport have a different access route, it should be utilized.
FAMILY OR CAREGIVER TRAINING
Family or caregiver training begins before the patient arrives in the specialized unit or room. Family and visitor adherence to controlled stimulation therapy settings is vital to the patient’s outcome. Traditionally, visits are limited to two people at a time for 15 minutes’ duration. No children are admitted until the patient’s tolerance with stimulation is monitored. While visitors are with the patient, they should refrain from using cell phones or cameras and use quiet voices. It is beneficial for families and caregivers to receive printed information regarding the use of a controlled stimulation unit, how it affects the brain healing process, and why it has been chosen for their loved one. Visiting hours, guidelines, and special requests should be provided as well. Families are often overwhelmed with the patient moving to a new level of care and becoming more alert, responsive, and potentially agitated. Families should be given the opportunity to be educated by a staff member, who provides written materials so they can make notes for future reference. This allows the family to take home and share the information with other loved ones.
As the patient is better able to interact with their environment, the family may bring in clothing, photos, or preferred soft music. It is important for the entire rehabilitation team to involve family members in as much of the recovery process as is practical—this may increase and decrease throughout the patient’s stay.
THERAPEUTIC INTERACTIONS
Often hospitals and medical settings will do their best to keep consistent the number of staff and therapists working with patients in a controlled stimulation unit. With shift changes and other complicating factors, it is simply not possible for a patient to see a truly limited number of people during a stay, but all staff should be trained in working with easily overstimulated or agitated patients.
Many patients may have a 1:1 or sitter until their agitation and disorientation recede. The attendants’ primary role is assisting the patient with any transfers, giving safety cues as necessary, and documenting behaviors and sleep/wake cycles and other information that will be important for timing of medication and therapy sessions. While care and safety of the patient is primary, this is an opportunity to engage the patient in pen and paper games, orientation with family photographs, card games, or other quiet ways to pass time between meals and therapy sessions.
Therapy sessions—including occupational therapy, physical therapy, and speech-language pathology—will most likely take place in the patient’s room for the first few days. If the patient is not showing signs of increased agitation during sessions or sundowning, the patient may trial sessions outside of the room. These should begin in a quiet day room, in a therapy gym during a meal when it may be empty, or in a dining room during off-meal hours. The treating therapist should pay special attention to the patient’s engagement with the new environment, by being aware of new noises, bright lights, new smells, or movement.
It is important to try to offer rest breaks or quiet time before behaviors begin, or before signs of emotional lability, aggression, anxiety, frustration, or irritation present themselves.
SUPPORTING RESEARCH
A 2008 study by Chelboun, Hux, and Snell documented the impact variations in sound can have on a patient. It was discovered that type of sound does matter. There is more brain activation with music rather than simple tones, and sound with emotional content (for instance, hearing your name) will elicit more of a response than “meaningless” sound. Auditory stimulation can have different effects on different patients, and it is not discriminatory to their particular brain injury. The most significant increase in response was to familiar voices of family or friends and the least level of responsiveness was seen with preferred music. Nature sounds and nonpreferred music were considered neutral without a significant change in brain activation or response.
Familiar voices using calm, nonstartling volume and simple, soothing commands allow the patient to react on their own. Appropriate time must be given to process and respond.
The Defense and Veterans Brain Injury Center has completed extensive research about the physical setting in which neurorehab is conducted as well as the effects of stress on neuroplasticity during the healing process. They have shown that “forced aerobic exercise or involuntary exposure to environmental stimuli can increase [psychological stress levels] and impede neuroplasticity [worsening] deficits from the original injury.” By creating environments that are soothing and safe, yet not confining with balanced schedules of rest and therapy (be it physical, occupational, speech, or psychological), a patient recovering from brain injury can actually tolerate a higher level of therapy without the negative responses associated with overstimulation.
CASE STUDY
As cognition, attention, and voluntary participation increase in patients within our controlled area, different types of stimulation are added. The room starts off very bare, and the patient is allowed to move around the space as safety and ability allow. Initial added stimulation may include short visits from family and friends, a radio, or family photos brought in. After trialing that increase, a patient may be taken out of the room to a therapy room or quiet area of a therapy gym. Any time a new stimulation is introduced, the patient should be monitored during and hours after for any change in mood, attention, alertness, or restlessness.
A 47-year-old woman, Marlene, who had sustained a traumatic brain injury after a mountain biking accident, presented to our controlled stimulation unit disoriented, hallucinating, but fairly physically sound. Sleep-wake cycles were managed both with medication and with purposeful activity spread throughout the day. As Marlene was better able to respond to her nurses and therapists and follow simple one-step commands, she was taken out of her room to a day treatment room where she had visual stimulation, but auditory stimulation was still controlled. In this room, we could start working on tabletop activities, transfers to functional household furniture, and tolerating a new environment for short periods of time. In working with Marlene, it was important to have familiarity with her, as she would perseverate on conversations around her profession, as well as reiterate given instructions and seek constant feedback about how she was doing in the moment.
Marlene began her stay at the closed end of our controlled stimulation unit, and as she progressed with stimulation, tolerance, and awareness, her room was moved closer to the open end of the unit. This allowed for more natural interruption to her day with sights, smells, and noises. She began by having meals in her room, progressed to eating in the day therapy room (perhaps with music or conversation), and eventually trialed eating in the patient dining room. Her transition from room to day room to inpatient gym was also monitored closely by her team, consisting of a registered nurse, physical therapist, occupational therapist, speech-language pathologist, clinical psychologist, and physiatrist. Consensus between at least two members of her team was reached before changes in her care were made. This could also occur during daily or weekly rounding meetings.
When therapists reported Marlene was participatory, partially or fully oriented, and able to follow simple commands in the morning, nursing would often have a very different picture in the late afternoon or overnight. Reporting sundowning, increased evening agitation, or sleepless nights was an instrumental piece in determining what may have contributed to these signs of overstimulation. Creating “up/down” schedules, so patients have therapy and rest breaks on a consistent schedule, greatly helped with the regulation of Marlene’s days.
Marlene was eventually able to tolerate longer visits from her husband and children and transitioned from our inpatient unit to our outpatient Day Rehab Program. Her husband and children were able to receive hands-on training from our therapy team, as well as meet with the clinical psychologist prior to her discharge. With the support of outpatient therapy and an adapted work schedule, Marlene was able to return to her job and preferred activities.
Marlene’s story is just one of the successful rehabilitation cases that have had questionable prognoses yet gone on to have very positive outcomes. The regulation and reintroduction of stimulation for someone with a significant brain injury should be a primary concern when establishing a therapy plan.
The University of Queensland looked at patient and family perceptions of brain injury rehab settings and determined that without proper education from the staff, the therapy areas and patient rooms can seem bleak, boring, and “prison like.” The day seemed incredibly long with a lack of purposeful activities and a lot of “waiting around” for therapy. With proper education and written structure, patients and family can better understand the goals and plans of inpatient brain injury rehabilitation, leading to a more successful transition from an acute rehabilitation setting to a less restrictive environment. Keeping the “less is more” philosophy, an appropriate environment and therapy plan can easily be implemented in an existing setting. RM
Sarah Sanderman, MOTR/L, has 4 years of experience working with brain injury patients in a controlled stimulation unit or outpatient setting. She works for Spalding Rehabilitation Hospital in Aurora, Colo, and specializes in brain injury and stroke recovery. Sanderman is also co-Director of the Spalding Brain Injury Support Group. For more information, contact [email protected].