 |
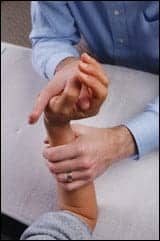
| Hand therapies can range from simple and effective manipulation and massage, as shown, to electrical stimulation modalities. |
The separate roles of occupational therapists and physical therapists in rehab medicine are usually very clearly defined. But when it comes to hand therapy, the distinctions are not as clear. Hand therapists not only focus on muscle function and strengthening, but also must be able to help clients regain the functionality to perform everyday activities.
“Hand therapy is a blending—the best of both occupational therapy and physical therapy,” says Paige E. Kurtz, MS, OTR/L, CHT, president of the American Society of Hand Therapists (ASHT), who practices at In Motion Rehab, Virginia Beach, Va.
Since entering the specialty, Kurtz has noticed a growing appreciation in the medical field for the specific treatment hand therapists have to offer. “It’s becoming a little more recognized as a specialty,” she says. “Working with hand surgeons as well as general physicians, I think they realize the value of hand therapy as opposed to just general occupational therapy or physical therapy for patients with hand injuries.”
TARGETING TREATMENT
Hand injuries range in scope from mild to severe. Some are common traumatic injuries, such as lacerations, broken bones, or crush injuries, which result from tripping, falling, or work-related accidents. Hand therapists also treat conservative-management injuries, such as arthritis or tendonitis. Most injuries can be attributed to overuse; for example, tennis elbow, golfer’s elbow, de Quervain’s, carpal tunnel, and “trigger fingers.”
Hand therapy can be beneficial to all age groups, although children are less likely to need this type of treatment as they are fast healers and usually have not yet built up cumulative trauma. Lately, Kurtz has noticed that a greater number of healthy retirees are taking advantage of this therapy.
“They want to stay active a lot longer, and they may be more likely to have ‘wear-and-tear’ problems such as tennis elbow or arthritis, if they are active,” she says, adding that seniors often want to keep up activities such as tennis and bowling. “The use of their hands and wrists into later years is very important to them.”
Treatment plans differ depending on the condition and the individual client’s needs, which is why a thorough initial evaluation is crucial. However, typical treatments focus on reducing pain and inflammation first, which is often accomplished with modalities, such as ice, iontophoresis, electrical stimulation, or ultrasound.
For example, Kurtz typically uses heat or active warm-up on the affected area to promote mobility and flexibility during the appointment. Next, she guides clients through range-of-motion exercises that target the hand, wrist, or elbow. Then, she moves to functional exercises.
“It may be grasping and releasing exercises or more traditional methods, such as picking up pegs, holding marbles in the hand, writing, and manipulating small objects,” she says. “We may then progress to coordination, endurance, and strengthening exercises, as appropriate.”
 |
| Hand therapy plans are devised to promote mobility and flexibility, as well as to increase strength and endurance. |
Therapy protocols do evolve over time and often depend on advances on the surgical side. “We get driven by the surgeons,” says Stacey L. Doyon, OTR/L, CHT, of Orthopaedic Associates of Portland, PA, Portland, Me. “As new surgical procedures come out, we need to then figure out the therapy.” For example, developments such as carbon implant arthroplasties or new wrist-joint replacement procedures require new approaches on the therapy side.
Advances in pharmaceuticals also have had an impact on how conditions such as rheumatoid arthritis are treated. “Some of the medicines are staving off some of the joint destruction and problems that people had 10 or 20 years ago,” Kurtz says. “About 18 years ago, I saw a lot of joint replacements for arthritis, and I’m seeing fewer of those.” She notes that there has also been success with conservative preoperative-therapy interventions and alternative surgeries in this area.
To stay abreast of changes like these, many hand therapists turn to online learning and national conferences. Doyon encourages therapists to attend these educational sessions, even if they have to pay out of their own pockets. “If you want to be a hand therapist, you definitely need to educate yourself more,” she says.
Educational sessions and networking forums also give hand therapists a glimpse into the future. Kurtz anticipates there could be an expanding role for the use of new modalities such as lasers in treating hand injuries. She also notes that recent research into war injuries will have an impact on the development of prosthetic limbs. “There is such good body armor, but the extremities may still be exposed,” she says. “So, I think some therapists are seeing more hand, arm, and leg injuries. The changes to prosthetics and the research coming out of that are pretty amazing.”
PRACTICING PREVENTION
Because so many hand injuries are related to overuse, teaching clients about prevention is key. Work-related injuries often develop as a result of repetitive tasks, but there are steps clients can take to reduce their risk.
“We recommend that they stop and take a break, do some stretches, and change their positioning,” Kurtz says. “Little changes that break up the repetition—thousands and thousands of repetitions one after the other—are certainly helpful for people in industry.”
Following safety protocols, including OSHA standards, is also a major prevention factor. It is imperative to be aware of hand placement during any task, especially when operating machinery or other electronic devices. “We get people every year who cut off their fingers with snow blowers just because of their misunderstanding of how they operate,” Doyon says.
It is also important to determine the cause of a problem that might lead to injury. “If they notice something that hurts, they should try to figure out what position or motion caused it and either avoid it or slightly modify the way they do things,” Kurtz says.
Of course, finding the root of the problem is not always straightforward for clients, most of whom aren’t familiar with the anatomy. “They don’t realize that elbow pain is usually being caused by something they’re doing in their wrist with their hands,” Doyon says.
Educating patients about these relationships also means teaching what types of motion will trigger the pain. When Doyon herself developed tennis elbow, she noticed that some of her home activities aggravated the problem, even if they weren’t direct contributors. “Our bodies never get a rest anymore, and I think that’s contributing to a lot of the problems,” she says.
This led her to educate patients about how to perform routine tasks in the home without aggravating or inducing injuries (see sidebar). “Not only do I review the ergonomics at their workstation, but I also review their ergonomics of everyday living,” she says. “It’s amazing with our fast-paced world how many of us carry all five grocery bags in at once.”
Doyon targets very specific, everyday activities that most people never even consider twice. “They don’t realize that the way they grab their coffee cup every morning—if they’re grabbing it on top—is going to aggravate that elbow,” she says.
She gives clients a tip sheet that includes pointers on how to perform a variety of tasks—from dusting and vacuuming to driving and writing—ergonomically. For new moms, she also has a separate lists of dos and don’ts that center on the logistics of child care, from feeding positions to baby clothing features that are easier on a parent’s hands.
These prevention tips also apply to hand therapists themselves. “A lot of hand therapists do tend to have wear-and-tear injuries, and we are more aware of how to use our hands,” says Kurtz, who adds that she uses joint protection daily.
Doyon attributes her own experience with tendonitis to the width of her treatment table at the time, and she now uses a narrower table. She notes that concerns about osteoarthritis may lead her to consider using different lever systems instead of her own fingers when working with patients as well.
While Doyon acknowledges that hand therapists are susceptible to these types of injuries, having a variety of cases that require different motions can help lower the risk. “I treat the wrist and forearm and elbow, so I get a little bit more variety in my day,” she says. “And that helps. I do see some differences depending on what my case load is.”
SERVING SPECIALISTS
For more than 30 years, the American Society of Hand Therapists (ASHT) has served as a resource for occupational therapists and physical therapists performing hand therapy. Most of the 3,300 members are certified hand therapists (CHTs), although this is not a membership requirement. The association’s ultimate goal is to become the go-to resource for all hand therapy-related information.
In addition to offering access to published research from the field, ASHT promotes networking through Web boards and listservs. It also allows clinicians who are new to the field to interact with their peers and find mentors. “I would encourage people to join ASHT even before they become a CHT,” Kurtz says.
A major area of concentration for ASHT is working to educate insurers such as CMS and other private corporations about hand therapy. These days, insurance companies require more documentation of services than before, and many are paying less per visit. Some even impose restrictions on which specialist can perform a certain service. For example, in some states, only orthotists—not OTs or PTs—may make splints. The problem, Doyon says, is that orthotists are not necessarily familiar with hand-therapy-specific details such as the protective splint required immediately after a tendon repair.
“Fortunately, here in Maine, we were successful in fighting that, and now we’re again allowed to do it,” Doyon says. “But that’s not so simple in every state.”
To help address these issues, ASHT provides several tools allowing hand therapists to inform insurance providers about the specialty. The organization’s Web site includes a PowerPoint presentation they can use as well as contact information for the various companies.
While the majority of members are CHT certified, Kurtz stresses that this is by no means a membership requirement. ASHT provides the information interested clinicians need to learn about and stay abreast of the field. “Even if you’re not ever going to become a CHT, ASHT has got a great wealth of resources and information for anybody who treats hands, even if it’s just a small percentage of their practice,” Kurtz says.
STIMULATING SUCCESS
While hand therapy is a subspecialty in its own right, every occupational therapist and physical therapist works with hands to some extent. This is especially true of clinicians specializing in upper motor neuron injuries to the central nervous system.
Terry Walton, MS, OTR, of the Neurosciences Rehabilitation Outpatient Program at Froedtert Hospital, Milwaukee, uses a functional electrical stimulation (FES) device when working with patients who present with a stroke, a spinal cord or brain injury, or even multiple sclerosis. The device is essentially an orthosis that supports the wrist and delivers electrical stimulation through five electrodes. The electrodes stimulate the fingers, thumb, and wrist to enable patients to grasp, release, and pinch during functional exercises.
Patients generally wear the portable unit for several hours daily, and most even use the unit as part of their home program in addition to their traditional therapy sessions. “You can use it in a lot of different positions,” says Walton, explaining that patients can be standing, sitting, walking, or even on their stomachs when using the device.
The unit features several programs to facilitate the prescribed activity, such as weight-bearing exercises, unilateral or bilateral activities, or grasping and pinching exercises. “You can close the hand so that they can hold something for as long as they need to, and then you can push a button, and they can open it up,” Walton says. “There are some programs just for tone management and spasticity management.”
Clinicians are trained by the manufacturer on how to fit the device to patients. The unit comes in small, medium, and large sizes—with the small size accommodating patients as young as age 14. In fact, Walton sees several young patients with cerebral palsy, stroke, or a traumatic brain injury, who are referred from a children’s hospital. Many of these patients purchase the unit for use in the home, and most make the effort to use it as prescribed. “They’re pretty compliant,” Walton says.
Walton has also had many successes with adults. For example, one patient was unable to use her affected arm for years. She kept it in a sling, which meant the arm was contracted and painful. Along with teaching her stretches and functional exercises as part of her treatment, the use of the FES device enabled her to regain most of the functionality in her hand. “She can use her hand for all activities,” Walton says. “Her posture also improved because her arm wasn’t bent and at her side. She actually got back to dancing again.”
While positive results like these have been documented in the literature, reimbursement for the device is not yet universal. “The biggest frustration is that insurance companies don’t always pay for it,” Walton says. There is hope for this to change, however. Several professional associations, such as the American Heart Association and the American Stroke Association, endorse FES as the standard of care for stroke patients. Large payors such as CMS may be slow on the uptake, but some smaller payors are beginning to reimburse for the device.
While Walton champions the use of the device, she is quick to note that it is only one part of the overall treatment plan. As in all other areas of rehabilitation, clinicians must tailor the program to the individual, including stretching techniques, functional exercises, and even fitting splints in some cases. The FES device, depending on the patient’s level of severity, may prove beneficial when used in tandem with these other techniques. “It’s just one piece of the puzzle,” Walton says.
Ann H. Carlson is a contributing writer for Rehab Management. For more information, contact .
FIVE TIPS FOR HEALTHY HANDS
Stacey L. Doyon, OTR/L, CHT, of Orthopaedic Associates of Portland, PA, Portland, Me, encourages clients to think beyond the workplace when it comes to their hand health. Here are some of her suggestions to avoid aggravating injury during routine chores:
- Smart shopping. Opt for a cart, rather than hefting awkward handheld baskets. Use two hands to lift heavy items, including the loaded grocery bags themselves.
- Laundry lessons. Use two hands to pull small bunches of wet clothes out of the washer. Do not overload the laundry basket, and be sure to hold it up with your arms rather than by the small handles.
- Careful cleaning. Dusting and vacuuming can require some “elbow grease,” so limit yourself to one room per day. Move your whole body with the vacuum rather than using only your arm to direct the device. Wearing a sock on the hand is preferable to using dust cloths.
- Dish duty. When scrubbing pots and pans, make sure to soak thoroughly, then use a scouring pad.
- Opening options. Cutting open bags of chips or other sealed packages of food saves wear and tear on the thumbs, wrists, and elbows. Consider buying an electric jar opener or a rubber gripper to help open stubborn lids.
 |
—Ann H. Carlson



