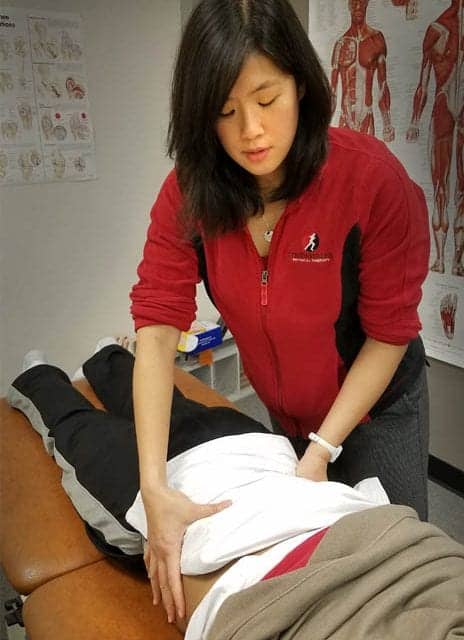
Alice Holland, DPT, applies a cold pack to a patient affected by pain symptoms. One of the most economical and easiest pain-management techniques is to apply hot or cold packs to an injured and painful area.
by Alice Holland, DPT
Every physical therapist’s role in patient care, from acute care rehabilitation to outpatient physical therapy, is to increase functional capacity and reduce disability in our patients. To do this, we dissect down to our patients’ impairments—their range of motion, strength, flexibility, and endurance. With this quantified knowledge of their impairments, we prescribe manual therapy and exercise therapy in a graduated fashion to increase our patients’ tolerance for functional activities and motion.
The trouble happens when manual therapy and exercise therapy doesn’t always improve a patient’s function because of the underlying symptoms of pain that prevent a patient from being able to endure those modalities. What then? How can physical therapists administer exercise therapy, while controlling for symptoms of pain? How best can a practitioner encourage a patient to move when movement hurts? How are physical therapists able to gauge a patient’s level of pain and ensure that exercises prescribed stay within the therapeutic range rather than spilling over to a harmful range?
Measuring Pain
The most standard method of tracking a patient’s pain level is by using a numerical grading system. The practitioner typically asks their patient to grade their pain levels from 0 through 10, 10 being “emergency room pain” and 0 being no pain. When numbers rise above a level the patient or PT is comfortable with, the intensity of therapy can be altered to bring down the patient’s pain level.
Although this method of tracking pain is standard operating procedure in most medical clinics, this method may not be clinically reliable in cases of chronic pain—where numerical values rarely fluctuate because of the patient’s psychosomatic attachment to the expression of pain. The clinics at Stride Strong Physical Therapy use the Visual Analog Scale, which does not contain gradations or markers that could interfere with the patient’s perception of pain, or memory of a previous pain number. This produces a similar effect much like the Wong Baker Face Scale, which uses a series of happy and sad faces to denote how patients are feeling.
Another method that clinicians have used to discern between therapeutic and non-therapeutic ranges of exercise progression is to prepare the patient in differentiating “soreness” and “muscle work” versus the “original pain” that prompted them to seek medical help. A difference in use of terminology by the patient may help the practitioner gauge whether an exercise is staying within the bounds of effective pain management.
Cultural and personality differences play a big role in quantifying and communicating pain. For example, there is a prevalent notion that there will not be “gain without pain” and some cultures may take this mantra more literally than others, increasing the risk of reinjury in the clinic if a manual or exercise modality is dosed higher than what is considered therapeutic. Often, practitioners would need to rely on nonverbal cues generated by their patients to properly assess acceptable ranges of exertion. Things to watch out for are: sweating, redness, hyperventilation, Valsalva maneuver, guarding, and tremors.
One commonly used method in medicine to manage pain in patients is by way of pharmacological use of oral analgesics. Though patients are sometimes encouraged to take analgesics before entering their physical therapy clinic, misuse of opioids could increase undesired side effects such as blood pressure changes, or increased drowsiness and decreased alertness. Patients are warned not to “operate heavy machinery” while taking opioids and unfortunately, leg press machines and treadmills do qualify in this category. Moreover, with $55 billion dollars in health and social costs related to prescription opioid abuse each year, and with $20 billion dollars spent in emergency department and inpatient care for opioid poisonings, it is prudent for the healthcare practitioner to avoid encouraging constant use and dependency on analgesics and opioids.
So what can be done to treat and manage the pain our patients sometimes experience during movement and exercise? The answer lies in non-pharmacological physical therapy modalities. Following are a few common methods used in physical therapy clinics and their applications.
Ultrasound Therapy
Ultrasound can be used as a thermal modality to provide deep heating into muscle and tissues. Ultrasound therapy relies on acoustic energy that generates molecular collision during its transmission through tissue. Molecules in biological tissue will vibrate with ultrasound’s mechanical wave, and this vibration will in turn increase temperature of the tissue through alternating compression and rarefactions. At 1 cm below the fat surface of a limb, the ultrasound head transmitting at 3 MHz can raise the tissue’s temperature by 4?C in 4 minutes. This heat can stimulate large-diameter myelinated nerve fibers (sensory nerves) and reduces pain by way of the gate mechanism of pain relief. Since ultrasound’s Effective Radiating Area is small, the largest clinical efficacy of the use of ultrasound would be to heat up smaller areas on the body that need pain relief.
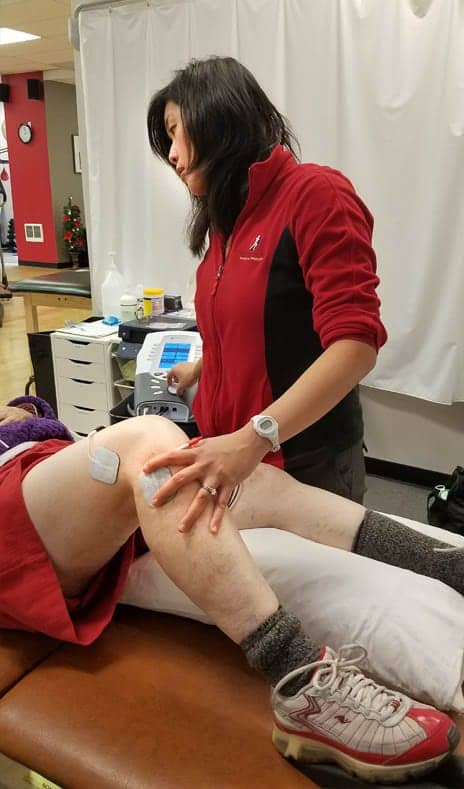
Electrical stimulation evokes the gate control mechanism and reduces the perception of pain by making the brain’s recognition area more aware of the sensory stimulus rather than the pain signals.
Electrical Stimulation
Electrical currents are used on the patient for pain modulation by way of sensory stimulation. This electrical stimulation evokes the gate control mechanism and reduces the perception of pain by making the brain’s recognition area more aware of the sensory stimulus rather than the pain signals. Known for its acronym TENS, this type of stimulation is the most popular and easiest to apply, and it’s something that patients can choose to apply to themselves at home. Intensities are adjusted to tolerance but not high enough to cause a muscle contraction. Pulse duration should be 75 to 100 µsec, at 80 to 125 pps continuously. Total treatment time with the machine should correlate to the patient’s pain and should be left on for the duration of their painful activity. Clinically, TENS can be used to reduce pain while performing an activity or exercise that is painful, but beneficial (such in the case of active range of motion exercises for a painful joint).
Superficial Hot and Cold Therapy
One of the most economical and easiest pain management techniques is to apply hot or cold packs to an injured and painful area. The clinical benefits of thermal application are numerous: increased blood perfusion, increased tissue metabolic rate, decreased joint stiffness, muscle relaxation, and heightened pain thresholds. However, heat therapy has the tendency to increase inflammatory responses in greater temperatures, so it would be contraindicated for continuous use in acute injuries. Acute injuries are best suited for cold therapy applications, in that cryotherapy has a large effect in controlling hemorrhage and edema. Additionally, cryotherapy decreases nerve conduction velocity and therefore numbs pain signals. The most common contraindication to cryotherapy is for use on areas of the body with impaired circulation.
Topical Analgesics
Topical analgesics perform similarly to hot and cold therapy by utilizing the gating mechanism of distracting the brain from pain signals. Some topical analgesics use capsaicin to stimulate a soothing or menthol feeling to do this. Other topical analgesics use lidocaine to numb sensory nerves, but efficacy of this may be limited to superficial pain rather than deeper pain in muscles and joints. Topical analgesics are a useful and convenient method of managing pain for patients to use at home, to keep them compliant with home exercises and mild irritation from activity.
Biofeedback
Biofeedback is the use of a measuring instrument that gives moment-to-moment, real-time information and status. The most used of its type is the electromyographic feedback, typically in the form of a handheld device with electrodes that measure the electrical activity that a muscle contraction makes. The clinical application for this device is in muscle re-education, in training a muscle to fire at appropriate times of an exercise or activity, but it can also be used for reducing muscle guarding and pain. With proper placement of electrodes in guarded muscles, the physical therapist can train the patient to reduce muscle contraction by reducing real-time electrical feedback from the device. This way the patient can relax guarded muscles, and thus reduce pain. Biofeedback is a useful tool to use in the clinic if the physical therapist suspects a high level of fear or anxiety in a certain movement or exercise. This has been shown to be effective in reducing pain in the low back or for patients with headaches.
Another cheaper use of biofeedback is through use of a pulse oximeter that measures heart rate. To reduce anxiety and promote focus and/or relaxation, the patient can be cued to diaphragmatic breathing or intermittent meditation when the pulse oximeter reads a high heart rate (determined by the practitioner) to reduce the sympathetic nervous system response. Examples of this application would be when a patient is preparing to perform an activity or movement that induces nervousness or fear—such as getting ready for gait training, when a lower-extremity injury is acute.
Therapeutic Laser
Low-power lasers have shown some efficacy in reducing pain. Their action is still being studied, but their effects are more on the cellular level of a wound or injury. Dosage of the laser largely relies on the type, make, and model of the device, so specifics should be consulted with a manufacturer. Low-level lasers have direct effects on tissues 1 to 2 cm in depth, and have indirect effects as deep as 5 cm, so therapeutic lasers may be effective in deeper soft tissue injuries. Low-level lasers are known to have an effect on the acceleration of collagen synthesis, increased vascularization, and decreased inflammation. This may be clinically useful in patients with painful nerve damage, where nerve healing is of utmost concern.
Meditation and Cognitive Behavior Therapy
Much of pain is psychological. Whether the pain is chronic in nature, or acute from tension and guarding, a large reason for why pain exists is to trigger the fight-or-flight mechanism of the sympathetic nervous system. By using meditation or cognitive behavior therapy, the patient can be taught to let go of memories and programmed physical responses to trauma. Meditation can happen in a short amount of time in the clinic, or while doing an exercise such as diaphragmatic breathing. The physical therapist can also seek consult from a cognitive behavior specialist for cases that require more exploration in the patient’s sympathetic triggers.
Though each clinician’s main concerns for his or her patients in physical therapy is in maximizing function and disability through exercise, the patient’s sensation of pain during these activities cannot be ignored. Therapists must be able to identify signs that indicate a patient’s pain may be impeding exercise progression as well as identify the source of the pain—whether physiological or psychological. From that point, the different tools available to clinicians can be used to reduce the perception of pain and coax a patient little-by-little toward physical recovery. RM
Alice Holland, DPT, is a director of Stride Strong Physical Therapy, a physical therapy clinic in Portland, Ore. She is ASTYM Certified and has a special interest in treating runners and postsurgical patients. For more information, contact [email protected].