
Pediatric mobility users may progress through more than five wheelchairs and seating systems, as well as additional and multiple attachments and upgrades. The number of attachments may impact a child’s use of the mobility system, such as the multiple items this young male user requires.
by Todd S. Danos, MBA, LOTR, FACHE, and Lori Boyter, PT
We often hear the phrase, “Kids are just like little adults,” from many different clinicians in the healthcare field. Clinicians who have experience working with children would certainly argue against that, and make everyone realize that pediatrics is a completely different world, with different challenges than treating adults. We realize that pediatric patients are still developing physically, and we must pay special attention to growth and developmental issues that are not typically present in adult care. Add to this, intellectual, emotional, and social growth, which makes pediatric patients present a mixture of complex issues clinicians must learn to balance in their care. We also must include family dynamics and in many cases having to advocate for patients who cannot make their own decisions. Pediatric mobility is just one area in the complex world of pediatric care where all these factors apply.
Setting
Children’s Hospital New Orleans is a 224-bed, not-for-profit pediatric medical center offering a complete range of healthcare services for children from birth to 21 years of age. The facility is the only full-service hospital exclusively for children in Louisiana and the Gulf South, and has more than 40 pediatric specialties and more than 400 physicians. In 2009, Children’s formed Louisiana Children’s Medical Center, now called LCMC Health. The system has become a local, community-minded healthcare leader that operates Children’s Hospital, Touro, University Medical Center, West Jefferson Medical Center, and New Orleans East Hospital.
Children’s Rehab Program consists of inpatient and outpatient services provided at the main campus and throughout the New Orleans area. The facility has the only CARF-accredited Inpatient Pediatric Rehab Program in the Gulf South. The Rehab Department established a specialized wheelchair and seating clinic more than two decades ago and continues to have a clinic twice a month for specialized pediatric seating and mobility needs.
Who Has Mobility Assistance Needs?
There are many different reports that specify the percentages of the population that are disabled or who need assistance with mobility. What is known is that the volume of adults needing mobility assistance is far greater than the volume of children needing assistance. The percentage of people in the United States affected by a disability has held steady from 2008 to 2015 at approximately 12.2%.1 When broken down further, the age distribution of the population age 17 years and younger with a disability is 6.2%, whereas the age distribution of the population 18 years of age and older is 45.8%.1 Obviously, the statistics consider the aging population and their need for assistance as they get older. The number of people age 15 years and older who used a wheelchair for mobility is slightly more than 3.6 million.2
Reason 1. Mobility Progression
Pediatric patients requiring the use of wheelchairs for mobility will progress through many stages during their development that will impact the type of wheelchair they use, as well as the features they could need as they age. Depending on the age at which the child receives his or her first wheelchair or mobility system, they could progress through more than five different wheelchairs and seating systems, or more and multiple attachments and upgrades. The main factors in this are the growth and developmental needs of children as they age. This is not seen in adult care and must be considered as a major factor.
An important point for the child and family is for them to remain consistent in the seating clinics in which they participate. Sometimes this cannot be avoided, but having therapists or clinicians who have worked with the child for years as they grow helps better determine what their needs will be and predict future needs for the child and family.
Wheelchair and seating clinics should involve either physical or occupational therapists who have experience in seating, mobility, and positioning of patients. During the first assessment and all intermittent assessments afterwards, the therapist will typically assess some key areas to help determine the child’s needs for mobility and positioning, as well as help predict and plan for what they might need in the future as their growth progresses. Some of these key areas of assessment are cognition, range of motion and strength of upper body and lower body, sitting balance and body symmetry, and overall interaction of the child with the environment.
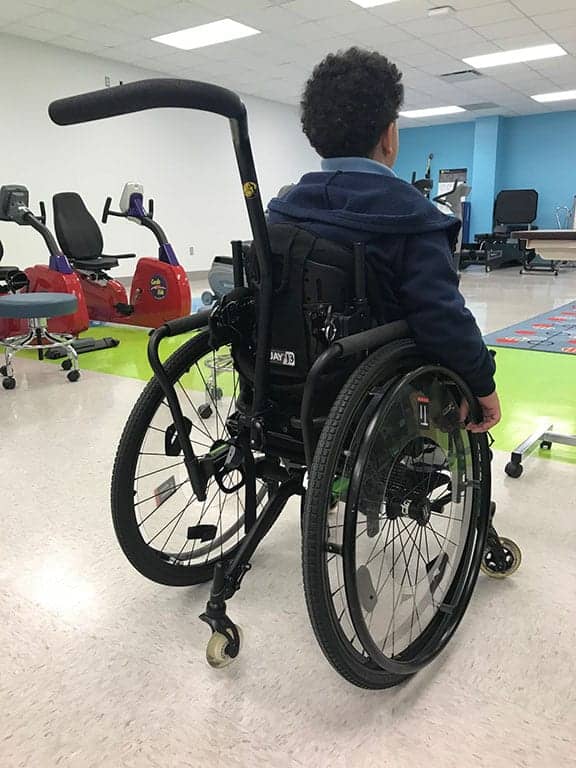
Patient D.B., who is featured in the case study that appears below, is shown here using his manual wheelchair.
Lori Boyter is a physical therapist at Children’s Hospital New Orleans and has participated in the specialized wheelchair clinic for close to 15 years. When assessing the current needs and potential needs in the future as the child progresses and grows, Boyter focuses on the cognitive state of the child. If the child presents in a good cognitive state, then many more opportunities with wheelchairs, features, seating, and other options are available for the child to be as independent as possible as they age and their mobility needs progress. It opens opportunities for them to control their environment, participate in sport and leisure activities, and have great success within the community and school.
One important point to note when examining mobility progression and the continued needs of the child as he or she grows over the course of many years, is to strive to provide the least amount of wheelchair and seating required to give the most ability to interact with the environment. Also, providing more features to a wheelchair than the child can coordinate and actively use usually ends up being a hinderance for the child. Any age or stage of development they are in, children should interact with their peers and environment as naturally as possible. This may mean a wheelchair system that is fairly basic and without many features, which promotes that independence. Examples of some features that might allow more independence are:
• Adjustable height of the braking system, allowing ease of reach.
• Wheel configuration. Children may work better with a reverse configuration with the large wheels in the front.
• Level of posture support needed, as more support tends to limit mobility.
• Can we do without a headrest? Some schools require the child to have a headrest on their wheelchair even though they do not need it.
• The less equipment needed for the wheelchair, the better. Is suction, oxygen, feeding, etc, needed on the wheelchair? The more you add, the less independent mobility they will have.
As the child ages, usually every 2 to 3 years, certain adjustments are needed to account for growth and any new options as their mobility progresses. This can happen quicker or later. Every child is different and progresses at his or her own pace. The adjustments can be minor, such as different wheels or placement of attachments. They can also be major and include an entirely new specialized wheelchair and seating system. One important point to note is that anytime they are evaluated for a wheelchair and seating system and anytime upgrades or adjustments are needed, a qualified therapist or specialized professional should participate. A child who ends up in a specialized system that does not work well for them is impacted for a long time, and the child will be limited in terms of what can be corrected or in the possibility of obtaining a new system.
Reason 2. Power to Manual/Manual to Power
Wheelchair progression in pediatrics tends to move along a continuum based on the type of mobility system that was originally prescribed: power or manual. Typically, if a patient starts out with a manual wheelchair, that person’s subsequent mobility devices are likely to also be manual models. However, there are instances where a pediatric patient may transition from manual to power, or power to manual.
Power mobility to manual mobility is certainly not common. If a patient starts in a power mobility system and then must move to a manual system, it is likely that some type of event triggered this change. The cause could be something medical or the patient may have became cognitively compromised, thereby affecting the safe use of a power wheelchair and its components. For example, Boyter had a patient with Duchenne muscular dystrophy who functioned well in a power system. The patient had a hypoxic event which caused significant cognitive issues and was no longer able to function in the power system. The patient had to move to a manual system that was better for the caregivers to use.
Transitioning from a manual system to a power system happens with great frequency among individuals affected by progressive neuromuscular disorders. These could include Duchenne’s and spinal muscular atrophy, among others. Throughout the progression, these patients may start out ambulatory, and then at certain ages—such as 7 to 9 years of age—progress to a manual wheelchair with basic functions. After some time, around 11 to 13 years of age, they begin to progress to power mobility. This includes a custom seating system, cushioning, tilt-in-space features, and possibly head or joystick controls. The back supports with these patients will change as well, from basic to custom as their level of trunk support decreases.
Again, with all these scenarios, being included in a specialized seating clinic and followed by consistent staff helps facilitate good seating outcomes.
Reason 3. New Technology
One of the benefits of being involved in a specialized seating clinic is that the clinicians and vendors stay up to date on new devices and technology that is available as the patient grows and continues to progress in their level of use. An important point to consider is that new technology also usually means cost, as more advanced systems and adaptations are expensive and many times not covered by insurance.
Within the industry, more technology governed by computers tends to be available for power systems. As pediatric patients age and their cognitive levels continue to advance, new features can be added to help the child at school and at home, and to interact and control their environment. This certainly promotes independence with patients and increases their confidence.
Environmental controls allow the patient to control most anything in their environment, from lighting and opening doors to performing certain daily living tasks. With today’s technology the sky is almost the limit. Along with this, Bluetooth and WiFi technology help control their music and computers through either physical or voice commands, and even eye gaze systems.
Technology available for manual systems tends to be geared toward physical activities. These are mainly adaptations to either their current system or additional manual systems that are set up for a specific purpose. Many active patients may have certain wheels for their chair to participate in sports such as basketball or tennis. They may have adaptations for skiing. They might also have an entirely different racing wheelchair that is specifically designed for speed.
Reason 4. How About a Gait Trainer?
Gait trainers help to serve a wide range of mobility challenges. Many pediatric patients, who spend most of their time in a wheelchair, also may utilize a gait trainer if they have the ability. Using these devices helps the child with balance, ambulation, strength, endurance, and in achieving mobility milestones.
The child can use either an anterior or posterior gait device when performing ambulation activities outside of the wheelchair. Anterior devices are typically seen in kids for temporary use in orthopedic situations. These are usually used to unload one of the extremities. These devices put the child in an anterior position, which is not an ideal position for the long term.
Posterior devices offer more flexibility and ability to adjust to allow more community and school ambulation. Many of our children in wheelchairs use posterior ambulation trainers as well to help provide some of the benefits listed above. In certain situations, children may progress from the wheelchair to a posterior gait trainer as their main mobility device. The posterior devices are typically seen in children with cerebral palsy (CP), spina bifida, and traumatic brain injury (TBI).
Reason 5. Should We Stand?
The short answer to the question of “Should we stand?” is, “Of course.” Standing as a weight-bearing activity is critical to physical and mental development. The use of pediatric standers for children who have difficulty standing provides not only good weight-bearing in the lower extremities, but also the following:
• Respiratory function and voice control;
• Facilitate formation of the hip joint;
• Normal muscle stretch, aiding in the prevention of contractures;
• Skin integrity;
• Promote better bowel and bladder function; and
• Overall increased energy, alertness, and cognitive development.
More and more models of standers are available for use. Supine standers offer the most flexibility and use with more various patient types. These depend on trunk control, but are typically used with small children, SCI, CP, and others.
Sit-to-stand standers require some additional trunk control and head control but offer the same benefits. Mobile standers are typically used for the more cognitively intact kids and allow the child to explore his or her environment in standing, promoting play, and interaction with others. Anytime we have the opportunity to get the child out of the sitting position, like in a wheelchair, and allow them the freedom to be standing upright, we should. There are many benefits to standing.
Reason 6. What About Strollers?
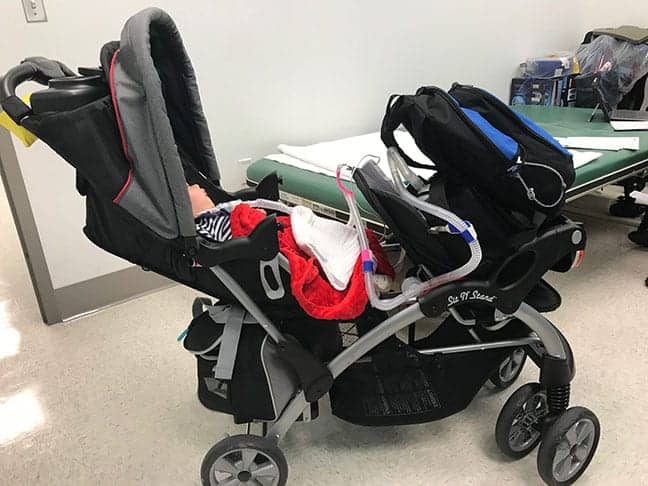
Pediatric patient who presented in a regular stroller. She is evaluated for a custom seating system stroller attachment that will place her in an upright position and allow her to visualize better as well as breath better.
Strollers are the most common form of mobility for children. We all understand the need for strollers for kids who have no mobility issues, but many times, regular strollers are being used for pediatric patients who have medical or developmental problems. Regular or medical strollers can be used in certain situations where the pediatric patient does not have immediate mobility issues. They can be used for kids who are affected by autism or another diagnosis where safety awareness is needed. They also can be used for children who experience endurance problems—for example, cardiac, Heme Onc, and some Down syndrome.
Pediatric patients who have significant mobility issues or certain medical diagnoses and are usually younger than age 2 years could be appropriate for stroller-based custom seating. These systems would have tilt-in-space capability, seating and lateral support, and hip guides, if needed. These patients typically will have mobility impairment throughout their life and progress from stroller to power mobility as they age. However, many times therapists see these patients in the clinic in a regular stroller, mainly due to cost issues or lack of knowledge provided to the parent about the need for these types of equipment.
Successful Progression
Pediatric mobility is an ever-progressing area where specialized knowledge is needed to assure that the child receives the right equipment for their ever-changing needs. Consistent participation in a specialized seating clinic, assessing the developing cognitive state of the child, and monitoring their medical issues ensures that the child has a successful progression with mobility and facilitates the health benefits of proper mobility. RM
Todd S. Danos, MBA, LOTR, FACHE, is the director of rehab services at Children’s Hospital New Orleans. He is a licensed occupational therapist, has a Master’s degree in business administration, and is board certified in healthcare management. He has more than 28 years of experience in the field of rehabilitation, and more than 22 years of leadership and management experience in both the pediatric and adult environments.
Lori Boyter, PT, is a physical therapist at Children’s Hospital New Orleans. She has been at Children’s for 14 years and has more than 20 years of experience in both the pediatric and adult environments of rehabilitation. She has organized and participated in the specialized seating clinics at Children’s during her tenure. For more information, contact [email protected]
Case Studies: DB and ZS
DB is a 7-year-old male with a history of cerebral palsy and spastic quadriplegia since birth. Initially, his mobility consisted of a regular stroller until age 2 years. He was assessed for a specialized wheelchair and seating system shortly thereafter, which also include specialized seating for cushioning purposes. As he continued to grow, he was again assessed for a new manual wheelchair at the age of 5 years, and continues in this seating system today for most of his mobility.
Along with physical therapy, DB performs ambulation each day. As he continues to grow he will, again, be assessed to upgrade his seating system and mobility. He participates in multiple sports for his age, and upgrades for his wheelchair will include certain wheels, a lightweight frame, and other options to make his participation in sports easier.

For patient ZS, the wheelchair clinic team makes seating adjustments as well as special adjustments in preparation for his eye gaze unit.
ZS is a 12-year-old male with a history of Adrenoleukodystrophy and spastic quadriplegia since birth. He initially started in a regular stroller and then progressed to a manual system. He was not considered initially for power mobility because of his cognitive state, which restricted him from using controls. His manual mobility has consisted of specialized wheelchairs with tilt-in-space features and custom seating systems.
As he has grown, this has been updated three times to accommodate him. Through extensive rehab, he has progressed to being able to communicate via an eye gaze unit, which he is being fitted for at this time to attach to his wheelchair. If his cognition continues to improve, power mobility will be tested with him.
Editor’s Note: This article appears in the April 2019 print issue of Rehab Management under the title Pediatric Mobility Growth.
References
1. 2016, US Census Bureau, American Community Survey Annual Report, “Disability Statistics & Demographics.” Available at: https://disabilitycompendium.org/sites/default/files/user-uploads/2016_AnnualReport.pdf. Accessed April 5, 2019
2. Americans with Disabilities: 2010 Available at: https://www.census.gov/prod/2012pubs/p70-131.pdf. Accessed April 5, 2019






