|
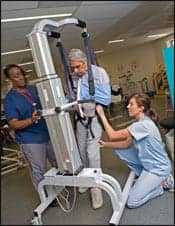
Vestibular function, gait, and balance are important components of spinal cord injury (SCI) and traumatic brain injury (TBI) rehabilitation. Patients who experience one of or a combination of these injuries often present with vestibular, gait, and balance issues and/or deficits. At Craig Hospital in Denver, we offer many different ways to assist and manage the patients with deficits in these areas.
EVALUATION PROCESS
When a patient is admitted to Craig, a thorough evaluation is completed by an interdisciplinary team, including a physiatrist, occupational therapist, physical therapist, speech language pathologist, therapeutic recreation specialist, dietician, neuropsychologist, and family services counselor. One person from each of these disciplines is assigned to work with the same patient throughout their entire length of stay for inpatient rehabilitation. At approximately 1 week into a patient’s stay, the team will convene, without the patient, to discuss the specific findings of each of the evaluations. Each team member presents the significant findings as well as hypothesized long-term goals to be achieved by discharge. As a team, with the physician in the lead, a consensus is reached for an appropriate date of discharge. This information is shared with the patient and/or their family at approximately 2 weeks into a patient’s length of stay at a patient/family conference. Such conferences then occur approximately every 4 weeks after the initial conference.
EVALUATION PROCESS—PT
Physical therapy will complete the appropriate evaluations on the patient, depending on the diagnosis. A patient with an SCI will have American Spinal Injury Association (ASIA) testing, sensory testing (light touch, pain, and proprioception), motor testing, range of motion (ROM) testing, tone assessment, functional mobility assessment, postural evaluation, skin evaluation in coordination with nursing, wheelchair evaluation, and pain assessment. A patient with a diagnosis of TBI will have ROM testing, manual muscle testing, neurological assessment (including sensation, tone, pathological signs, and cerebellar signs), functional assessment, developmental sequence testing, skin assessment in coordination with nursing, and postural evaluation. Balance and gait assessments are completed if appropriate for the patient with either diagnosis. Each evaluation is specific and tailored to the patient. Not all evaluations are completed on each patient.
OUTCOME MEASURES
|
Treatment Planning. Following the evaluation and utilizing the findings, the therapists discuss long-term goals with the patient and the patient’s family. The patient needs to be involved in the long-term goal setting to better engage them in the treatment plan. Alignment of expectations for discharge is achieved by setting long-term goals in conjunction with the patient and the patient’s family. Often, a patient’s long-term goals may not be possible by discharge so that requires education by the therapist in a delicate manner so as to never take away a patient’s hope of a full recovery, but to get the patient to accept what will be the goal by discharge from inpatient rehabilitation.
IMPACT OF VESTIBULAR DYSFUNCTION
Many patients experience vestibular dysfunction after a traumatic brain injury or spinal cord injury. They often complain of dizziness at some point in the recovery process. It is important that therapists are aware that just because a patient complains of dizziness, it does not mean that the therapist should avoid those positions that cause that complaint. Often, the position or movement that provokes the dizziness is the treatment that leads to the resolution of symptoms. Avoiding positions can make the dizziness worse. Also, the therapist must screen the visual system as that can often be the cause or at least a component of the patient’s complaints. Dizziness may also arise from the cervical spine issues, so the c-spine must be evaluated. An essential component of the vestibular evaluation of a patient is to determine when the patient has complaints of dizziness or imbalance. The PT must evaluate eye-head coordination and postural control as that adds valuable information to the evaluation.
Patients experiencing vestibular issues will be evaluated by their primary PT. If a patient presents with more complex vestibular issues, they can be referred to the vestibular clinic, which is conducted by an OT and a PT with further training in the areas of vision and vestibular rehabilitation. In addition, if the answers to the patient’s vestibular issues are not managed by the clinicians in the vestibular clinic, consultants, such as ENTs with specialization in neurotology, can be accessed.
GAIT PROGRAM
Prior to initiating a gaiting program, patients may be participating in tilt table, standing table, or stall bars standing. Patients can also work on body weight-supported treadmill training and/or participate in the aquatic therapy program prior to beginning a gaiting program. When a patient is ready to begin ambulation after SCI and/or TBI, it is a very exciting time in the rehabilitation process. Depending on the objective information the PT has obtained from ongoing evaluation on a patient, the data will guide the appropriate intervention to begin a patient’s gaiting program. The PT often begins working with a patient in the parallel bars to develop static standing balance and good postural alignment. A PT strives for upright posture with neutral hip position, knees soft (not in hyperextension), heel contact with the floor, and a well-aligned foot under the patient. If that is not the case, the PT may need to do more treatment interventions with the patient prior to progression of the standing.
Working toward more dynamic standing balance, weight shifting is often the next step. Lateral and anterior-posterior weight shifting is beneficial training for the patient as well as the ability to return to midline standing. All work in weight shifting should be done with good postural and joint alignment. Again in the parallel bars, the patient can progress from requiring bilateral UE support to unilateral to weight shifting without UE support.
BRACING CONSIDERATIONS
Bracing a patient can be another invaluable tool when working on balance and gait. If the patient does not have the necessary muscle strength to maintain proper joint alignment, the PT must be willing to look at bracing to protect a patient’s joint integrity for the long-term. During a PT session, the PT may be able to protect the joints through manual handling skills. However, if the patient leaves a session and does not have the hands-on facilitation of the PT, the patient’s joints are at risk and bad habits can be developed. One hour of hands-on training with a PT does not equate to a patient maintaining proper gaiting technique throughout the entire day. What happens when a patient is fatigued? What happens when a patient’s attention is not 100% focused on the quality of their gait? Most likely, gait deviations happen. It is better to control and manage as many of the gait deviations possible through bracing so the patient practices with good gait mechanics.
EVIDENCE
After weight shifting is at an appropriate level, stepping in the parallel bars can be initiated. As forward and backward steps are practiced, heel-toe contact is analyzed while the patient maintains good posture and joint alignment. This training may be initiated with UE support and, depending on the patient’s abilities, may or may not progress to unilateral UE or no UE support on the parallel bars.
When a patient progresses to gaiting outside the parallel bars, clinical observation skills and visual analyses are the tools the therapist utilizes to analyze a patient’s gait. Gait should be assessed in different situations (hallway without people versus hallway filled with moving people), as well as gait on different surfaces, gait without and with head turns, gait at varying speeds, patient’s ability to change gait speed while ambulating, patient’s ability to walk forward, backward, side step, stop, and turn.
A physical therapist will be observing a patient’s posture, joint stability and alignment, gait deviations, losses of balance, and the subjective report from the patient of how they feel while gaiting. The therapist also should assess distance, level of assist required, and speed of gait. Multitasking while ambulating is also of importance as that is what happens in the real world. A ball-throwing activity may be added, or a cognitive challenge can provide a therapist with valuable information as well as provide the PT with beneficial treatment techniques. A patient’s ability to navigate around and over objects should also be observed. Starting and stopping on the PT’s verbal cue can provide valuable information for treatment.
GAIT CLINIC
At Craig, there is a gait clinic that occurs at specified times during the week that the patient and primary PT can attend for guidance and assistance with treatment ideas and bracing needs. A certified orthotist and PTs are involved in running the clinic. Treatment ideas and recommendations are provided to the primary PT. In the gait clinic, a referral form is sent with information including ROM, MMT, proprioception, PT’s current gaiting status, any bracing or assistive devices trialed, and any limitations affecting gaiting. After analysis and discussion among the therapists and orthotist, a patient stands in the parallel bars, assist as needed, without shoes and socks. A PT should never forget to look at the patient in standing without shoes and socks. The foot is the ground-body interface and must be in alignment before analysis up the chain or body can occur. Walking in the parallel bars is assessed and analyzed with discussions and decisions about the appropriate course of treatment recommended. That may include stretching and/or strengthening, and/or bracing if needed for joint protection.
Treating patients with such complex injuries as TBI and/or SCI is challenging and requires specialized expertise and experience. Therapists must use their training to analyze the objective findings in order to assist the patient to maximal functional independence and safety that will allow the patient to move onto the next step of rehabilitation. The rehabilitation of patients with these diagnoses is rarely straightforward and easy. It requires ongoing assessment and analysis to achieve the best possible outcome.
Lisa A. Childs, MS, PT, is a physical therapy supervisor at Craig Hospital, Denver, where she has worked for 10 years. For more information, contact .