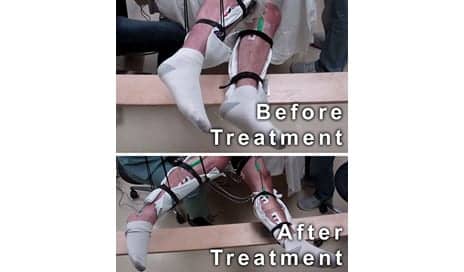
A man with complete motor paralysis moves his legs voluntarily while receiving electrical stimulation to his spinal cord via electrodes placed on his back. The subject’s legs are supported in braces so that they can move without resistance from gravity. The electrodes on his legs are used for recording muscle activity. (Photo courtesy of Edgerton laboratory/UCLA.)
According to a National Institutes of Health (NIH) study, a new strategy that delivers noninvasive electrical stimulation to the spinal cord has reportedly helped enable five men with complete motor paralysis to voluntarily generate step-like movements.
Per a news release from the National Institute of Biomedical Imaging and Bioengineering, part of the National Institutes of Health, the strategy is called transcutaneous stimulation, and it delivers electrical current to the spinal cord via electrodes placed on the skin of the lower back.
The study, published in the Journal of Neurotrauma, was conducted by a team of researchers from the University of California, Los Angeles; the University of California, San Francisco; and the Pavlov Institute, St Petersburg, Russia, according to the release.
The research team was led by V. Reggie Edgerton, PhD, a professor of integrative biology and physiology at UCLA, and Yury Gerasimenko, PhD, director of the laboratory of movement physiology at Pavlov Institute and a researcher in UCLA’s Department of Integrative Biology and Physiology, per the release.
The release explains that in the study, five men — each paralyzed for more than 2 years — underwent a series of 45-minute sessions, once a week, for approximately 18 weeks, to determine the effects of noninvasive electrical stimulation on their ability to move their legs.
In addition to stimulation, the men received several minutes of conditioning each session, during which their legs were moved manually for them in a step-like pattern. The goal of the conditioning was to assess whether physical training combined with electrical stimulation could enhance efforts to move voluntarily.
For the final 4 weeks of the study, the men were given the pharmacological drug buspirone, which mimics the action of serotonin and has been shown to induce locomotion in mice with spinal cord injuries. While receiving the stimulation, the men were instructed at different points to either try to move their legs or to remain passive, the release continues.
When the study began, per the release, the men’s legs only moved when the stimulation was strong enough to generate involuntary step-like movements. However, when the men attempted to move their legs further while receiving stimulation, their range of movement significantly increased.
After just 4 weeks of receiving stimulation and physical training, the men were able to double their range of motion when voluntarily moving their legs while receiving stimulation. The researchers suggest that this change was due to the ability of electrical stimulation to reawaken dormant connections that may exist between the brain and the spinal cord of patients with complete motor paralysis, the release explains.
Surprisingly, by the end of the study, and following the addition of buspirone, the men were able to move their legs with no stimulation at all and their range of movement was — on average — the same as when they were moving while receiving stimulation, per the release.
“It’s as if we’ve reawakened some networks so that once the individuals learned how to use those networks, they become less dependent and even independent of the stimulation,” Edgerton says in the release.
The researchers also made extensive recordings of electrical signals generated in the calf muscle and the muscle directly below the calf while the men attempted to flex their feet during stimulation. Over time, these signals increased with the same amount of stimulation, further supporting the hypothesis of re-established communication between the brain and spinal cord, the release states.
Though noninvasive stimulation could offer advantages over a surgically implanted device, Edgerton says both need to continue to be developed. For example, a non-invasive stimulator might be useful in determining whether a patient will be receptive to neuromodulation, which could then help determine whether undergoing surgery to implant a stimulator is warranted.
Alternatively, Edgerton speculates it may be possible early after an injury for non-invasive stimulation to help patients achieve a certain level of motor control that then allows them to continue to improve with physical rehabilitation and avoid surgery altogether, the release continues.
“All patients are going to need something slightly different, and maybe noninvasive stimulation is going to be best in some cases and epidural stimulation in others,” Edgerton states in the release.
“What we need to do is maximize the clinical tool box that we have so that the physician and the patient can select a therapy that is best for them,” he continues.
[Source: National Institute of Biomedical Imaging and Bioengineering, part of the National Institutes of Health]