 |
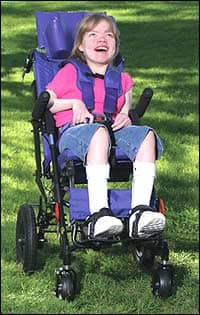
| A mobility device, with proper seating and positioning features, can vastly improve a child’s development. |
The incidence of premature births has increased dramatically over the past decade. Contributing factors include in vitro fertilization, multiple births, maternal age (over 35), unmanaged diabetes or high blood pressure, previous premature birth, cervical incompetence, and exposure to certain viruses. Some reports cite the current United States rate of 20% to 25% of all births occurring at or before 36 weeks of gestation. Recent studies (presented at the American Academy for Cerebral Palsy and Developmental Medicine) show that more than 50% of these babies will have long-term physical, visual, cognitive, and/or language challenges. There also has been an increase in the rate of cerebral palsy.
A Seattle-based study on sudden infant death syndrome (SIDS) showed that the rate of death could be decreased by having babies sleep on their backs. This led to the back-to-sleep program. The result was intended to be that babies just slept on their backs, but the reality was that babies spent all of their time on their backs. The incidence of torticollis, plagiocephaly, and developmental delays skyrocketed. One study has shown that this led to a dramatic upward shift in the age of attainment of gross motor milestones.
Now more than ever, we need to make sure that infants move and learn the effects of their actions on the world as soon as possible. All parents need to make sure that their infant has at least 15 minutes of tummy time every day. The best baby shower gift is a floor system that provides a roll for under the arms of the child (to promote prone on elbows and prone play), a kick-activated mobile (the feet actually can manipulate toys before the hands), and a toy bar for the car seat. Studies have shown that some premature infants have learning issues right from the start. We need to build in mobility as early as possible. A 3 month old, with direct supervision, can wear a ribbon loosely tied to their wrist or ankle and then attached to their overhead mobile for 10 minutes a day. Studies have shown that the child learns in just a few trials that their movement makes the toy move. This is one of the earliest opportunities to encourage mobility and learning.
If by age 5 months (adjusted age) the child is 25% (or more) delayed, we need to use augmentative mobility. The first step is to support sitting. Begin by supplying head and trunk support. Use this supported position to teach midline and tracking. Slowly reduce the amount of head support so you actually teach head control. If you wait much past 6 months to introduce sitting, you have lost valuable time to get the eyes working together.
At 8 to 9 months (adjusted age), it is time to introduce standing and crawling. Karen E. Adolph, PhD, a professor of psychology and neural science who specializes in perceptual cognition development and perception at New York University, has shown that crawling has nothing to do with learning to walk. If you want walking, you have to teach walking. But Rosanne Kermoian, PhD, at Stanford University, presents data that shows that crawling changes the way weight is borne on the palm and impacts handwriting and fine motor skills later on. Here again, positioning devices can really help you. There are a few crawling devices out there, and some are better at supporting the child than others. You also can use your treadmill and walking harness to do some crawling. Have the child wear knee pads and gloves and use manual guidance to get the crawling pattern you want. (Long Island, NY-based Phil Koch, PT, is the master of this intervention and has some wonderful case studies.)
THE STANDING ADVANTAGE
When it comes to standing, the choices are numerous. If the child has Medicaid assistance, you may be limited to one of three devices that fit the reimbursement amount. There are standers that can accommodate severe knee flexion contractures, as well as models that go from sitting to standing with no lifting, and others that a child can move on his own (like a wheelchair). Some children need to have their head lower than their feet for postural drainage, or need a stander that can change from prone to supine to upright—and these options are available, although a letter of medical necessity might be necessary.
 |
| This stander is for children aged 1 to 5 years. It can be used for supine, prone, and upright positioning. |
If a 3 year old is still not ambulating independently, you need to make sure they have an assistive mobility device that allows them some form of independent mobility. The child may be destined to be an independent ambulator, but to maximize cognitive and language development, they need an independent form of mobility beside commando crawling. Studies have shown that commando crawling does not afford the child the same cognitive and spatial benefits of belly-off-the-ground crawling. This means that a child who needs help in their walker needs to be in a gait trainer at least 30 minutes a day (that is not evidence based—just my opinion). This is a great time to ramp up body weight support gait therapy! If you do not think the child will be an independent ambulator for long distances by age 6, now is the time to start power mobility training. There are many studies showing that 18-month-old children can successfully learn to use power mobility. I usually do some trials at that age so they have the experience and exposure, but wait until they hit preschool (ie, wide hallways) to start daily training.
This is also the time to introduce 24/7 postural management. The new trend (it is “old hat” in Europe) is special beds that enable the caregiver to maintain the child’s spine, hips, and knees in the desired position. The Tardieu method has shown that it takes 6 hours of stretching to impact a spastic muscle in a child with cerebral palsy. Nighttime is the best time to do this. Studies also have shown that these sleep systems improve the child’s (and thus the caregiver’s) sleep.
If you do not expect the child to be able to sit independently before they reach 40 pounds, do not forget to order a car seat. There are three main choices. One is easy to clean, one is way cushy, and one is great for aggressive positioning (and the only one that goes up to 140 pounds). If you choose the one that reclines, make sure you have the seat depth in the car it will be in. Also make sure the family has hooks to attach the tethers.
EQUIPMENT IS YOUR FRIEND
Now the challenge is balancing educational and medical goals. The child is in school to learn. Who is responsible for stretching? Standing programs? Toileting? Transfers? Mobility? I believe that equipment is your friend. The recipe for success is picking equipment that requires the least amount of lifting and adult intervention. If the child is able to use a switch interface and uses power mobility, get a system that stands the child. A seat elevator or one that partially angles to assist with transfers may mean the child can toilet independently. A power system that lowers the child to the floor or a seat that tilts side to side so the child can reposition themselves independently is invaluable.
The family also will need to address exercise. Studies have shown that children with disabilities need to exercise as much as typically developing children. These devices are not usually covered by third-party payors. Bikes, treadmills, and elliptical trainers are all available for almost all children at all functional levels.
There are a great many choices in power mobility. Can any single person know them all? There is no substitute for good advice and experience. A good rule of thumb is to start with a provider who is NRTTS or RESNA certified. Another trick is to meet regularly with your local manufacturers’ representatives. All the big manufacturers have education programs and will send you a qualified physical or occupational therapist to demonstrate the latest trends. Most of these courses are not product specific and can earn you free CEUs. In addition, these sessions provide the opportunity to expand your knowledge and give you time with new equipment. My favorite courses are those that do a half-day lecture, and then help you fix your equipment (and clients’ equipment) for the second half of the day. These trainers are world class experts and love the challenge of solving your biggest problems.
If a child’s home has any steps to the entrance, the manual or power chair may have to stay at school or in the car. You may need a separate activity chair for the home. There are a number of excellent chairs on the market. My favorite ones go up and down, so they can be used for floor time, or at the dining room table. I want the chair to easily tilt and recline. I also like a good headrest, a tray, and a fabric that cleans easily. One of my favorite chairs has independently adjustable leg supports and back pad so you can help the femoral head stay in the socket, as well as support the sacrum and lumbar spine.
ADDRESSING ADULT NEEDS
Cushions are getting better and better. We can now choose different densities and materials and make conglomerate setups that capture and stabilize the pelvis, support the femoral heads, and relieve the bony prominences. Linear systems made of medium-density foam are receding from rehabilitation. A biangular back can be a user’s best friend. This innovative design allows the pelvis to stay back in the chair, while supporting (rather than pushing) the lumbar curve. By enabling the trunk to be semi-immersed in a breathable material, we may see a decrease in the progression of scoliosis and improved respiratory function.
Push rims destroy shoulders. Old-fashioned wire spoke wheels and round handrims are being replaced by ergonomic handrims and power assist propulsion. As people with disabilities live longer lives (almost equal to those of the whole population), studies are showing that 30 years of self-propulsion can lead to painful frozen shoulders in later years.
Supported walking is another big trend for adults. Gait trainers and walkers that support the trunk and pelvis are now available from at least five different companies. These devices enable marginal ambulators to gain independence and function that were not previously possible.
Exercise for people with disabilities has been identified by the Department of Health and Human Services and the American Physical Therapy Association as a top priority. Hippotherapy, aquatic therapy, weight lifting, elliptical trainers, stationary bikes, and treadmills are all good ways to stay healthy and strong. The best evidence-based choice is probably a body weight-supported treadmill system. At least seven systems are available, starting from harnesses that attach to the ceiling all the way to expensive computer-driven robotic systems.
Before you order, talk to the client’s therapists, teachers, and caregivers. Show them at least three different models to choose from. Bringing in demo models is always a plus.
Rockville, Md-based pediatric specialist Ginny Paleg, PT, teaches CEU courses for equipment manufacturers. She serves on the editorial board of Rehab Management. For more information, contact .





