Traditional rehabilitation approaches for neurological injuries have primarily focused on teaching compensatory strategies to overcome one’s deficits. Specifically, conventional models for persons with spinal cord injury have had adaptation as a central component with little treatment aimed at remediation of impairments or “relearning.” Significant growth in the evidence base indicates that the central nervous system has the ability to modify itself in the presence of appropriate inputs even after a neurological insult. Therefore, treatment strategies are shifting to target facilitation and recovery of function. The goal of facilitating the injured nervous system is to either circumvent (reorganize) the original lesion site by developing alternate pathways/process centers for the communication of information or to use intact tissues that were spared during the original insult to promote recovery of lost function. This adaptive response or neuroplasticity of the nervous system is largely activity dependent and the specificity of the activity is also considered to be a primary driver for motor learning. The use of new technologies has made it easy for the clinician to target therapies toward the goal of recovery of lost function.
FES: TARGETING THE NERVOUS SYSTEM
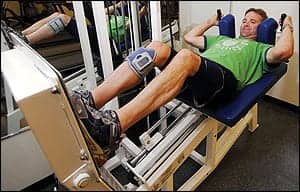 |
| Athlete Duane Morrow works out on a fitness system at Shepherd Center’s Beyond Therapy Program. Photos courtesy of Shepherd Center, Altanta. |
There are many different treatment algorithms and strategies being developed in the clinic to provide facilitation of the injured nervous system that often include various forms of motor patterned activity and intensive strengthening, as well as incorporating modalities such as electrical stimulation. Accompanying the philosophical transition from compensation to recovery in rehabilitation programs, various forms of rehab technologies have been developed and implemented in the clinic environment to provide safe and efficient ways to stimulate the injured nervous system. Having access to these types of technologies can often afford clinicians the ability to get their patients who have sustained a serious neurological injury upright, weight-bearing, and moving much sooner after their injury than could have been previously accomplished in the rehabilitation setting. This ability to decrease the amount of time that a client spends immobilized after any injury addresses the disuse issues these patients suffer from inactivity such as muscle atrophy and tissue shortening. Additionally, this activity, especially in the context of function, is thought to be an important aspect in promoting plasticity of the injured system and could potentially lead to improved long-term outcomes for these clients.
Neuromodulation, or the concept of stimulating the nervous system to effect change and recovery from neurological disaster, is a fairly new, but growing field. Functional electrical stimulation (FES) refers to a subset of neuromodulation that focuses electrical impulses at activating specific muscles with sequencing or timing mimicking “normal patterning” during functional activity to control paralyzed limbs. By directly stimulating both sensory and motor nerve fibers as well as providing additional sensory feedback through joint movements in the context of functional patterns, FES can potentially address musculoskeletal limitations as well as facilitate plastic changes in the nervous system.
Some examples of FES technologies that have recently been introduced in the rehabilitation center are:
1) FES bike—FES is applied to the quadriceps, gluteal, and hamstring muscles in order to produce a contraction in those muscles and create enough force to propel a lower-extremity ergometer.
2) An FES system for advanced foot drop, designed to use FES to lift the foot to help the patient walk more safely and easily.
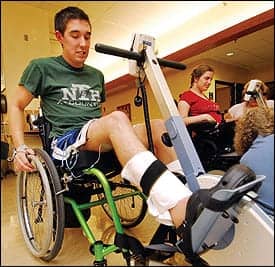 |
| A client works out on an FES bike. The electrical stimulation applied to certain muscles creates enough force to propel a lower-extremity ergometer. |
Access to these technologies can be extremely helpful to the treating clinician in designing a safe, comprehensive, and often intensive treatment program aimed at maximizing both neurological and functional recovery. However, it is important to remember that these technologies are part of the many tools that clinicians have available to make their treatment plans effective, efficient, safe, and training specific. However, they are not a substitute for appropriate clinical decision-making. Even though these technologies are becoming more common in the rehab setting, they are only as beneficial to injured clients as the decision-making process that goes into what modality to use for each client and at what phase of the recovery process. There is no one modality or treatment protocol that will promote recovery in every client with a neurological injury. It is, therefore, the responsibility of the treating clinician to determine the most appropriate timing and use of these technologies based on the client’s current clinical presentation. Previous interventions/outcomes and, most important, their long-term goals should be considered in developing a comprehensive treatment plan.
A CASE STUDY
An example of the variety of types of rehabilitation technologies that can be implemented in a treatment program to promote functional recovery can be seen in Duane Morrow, a 37-year-old male diagnosed with a C7 incomplete spinal cord injury ASIA class B resulting in cervical myelopathy due to a herniated nucleus pulposus (HNP) that occurred after a rugby game on October 8, 2004. Morrow’s injury occurred while he was working in England, but he was transferred to Shepherd Center Catastrophic Care Hospital in Atlanta within days of the original injury for his rehabilitation care. Morrow completed acute care rehabilitation and outpatient rehab programs at the Shepherd Center and currently remains involved in the Beyond Therapy Program where his primary focus is on a complete recovery.
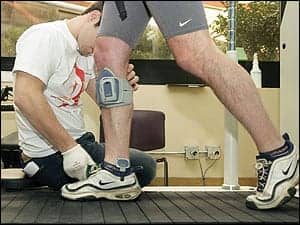 |
| Wearing an FES system, Morrow works out on a treadmill system, as a therapist watches his progress. |
From the beginning, Morrow has been extremely motivated. During his inpatient stay, he would complete his 3 hours of traditional therapy and then actively seek out other opportunities for more therapy. He soon received the nickname “super quad” as he was independent with his own care, including transfers from the floor to his wheelchair just a few weeks after his injury. His attitude remained positive and his outlook bright even though he was not moving any muscles below his level of injury. He asked the nurses to get him up early every morning so that he could work out on his own in the community-based fitness center on the hospital grounds before his formal rehabilitation schedule began for the day as well as inquiring about new technologies in the research department. He soon learned that Shepherd Center had recently obtained a FES bike and asked to begin using it about a month after his original injury as he still had no active movement in his trunk or lower extremities and wanted to maintain the girth of his legs as well as slow down the atrophy process. He began using the FES bike three times a week for 1-hour sessions and, after the fifth session, demonstrated voluntary movement in the toes of his left foot. This was almost 6 weeks to the day after his original injury had occurred. Morrow then developed voluntary movement in the toes of his right leg 4 weeks after the initial movement had been documented in his left leg. As the strength in his lower extremities and trunk increased, Morrow began standing and taking assisted steps in the parallel bars with appropriate bracing. However, as Morrow’s voluntary movement strengthened in his lower extremity and trunk musculature, the spasticity in his body also became significantly stronger. After 5 weeks of using the FES bike three times weekly, his spasticity became so strong that he was unable to cycle on the FES bike any longer. Morrow attempted participation on the manual body-weight supported treadmill system, but again due to his extensive spasticity, he was unable to achieve a quality gait pattern even with the manual assistance of three therapists. Approximately 20 weeks after Morrow’s initial injury, his spasticity had worsened to the point that he could no longer produce isolated movement in either lower extremity and he spent most of his time in bed locked in a fetal position unable to even transfer into and out of his wheelchair independently.
Morrow chose to have a baclofen pump surgically placed to manage his spasticity in September 2005 as he was already maxed out on his oral antispasmodics and had failed all other conservative measures for controlling his spasticity. Morrow then returned to therapy and began participating in an activity-based therapy program called Beyond Therapy that had recently been established at the Shepherd Center. During his initial evaluation, he verbalized the following goals:
1. Walk full-time in the community and eliminate the need for a wheelchair.
2. Walk independently without an assistive device or any orthosis.
3. Return to running.
His program consisted of a combination of 6 to 9 hours a week of intensive strengthening, locomotor training, and electrical stimulation targeted at improving the isolated strength and movement in his lower extremities and trunk to maximize his functional independence and mobility. After returning from his baclofen pump placement, Morrow was trialed again with manual body-weight supported treadmill training. However, his spasticity was still too severe to achieve a high-quality gait pattern using this modality, and he was transitioned to the robotic-assisted treadmill system in which he completed 45 minutes of actual stepping two to three times a week for 12 weeks. The remainder of his therapy hours per week included dynamic strengthening activities with and without electrical stimulation, upper/lower extremity ergometry with and without electrical stimulation, developmental sequencing exercises, and over ground gait training using appropriate assistive devices and orthosis. All treatment sessions were under the direct supervision of a physical therapist, but actual treatment time was divided between the team consisting of both exercise physiologists and PTs.
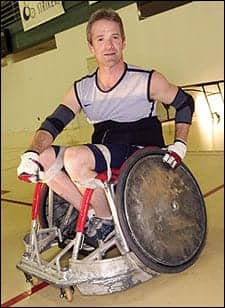 |
| In his rugby wheelchair, Morrow continues to enjoy such sports as wheelchair rugby and wheelchair racing. |
By January 2006, Morrow was walking household distances independently with a rolling walker and was spending the majority of his day using the walker as his primary source of mobility rather than his wheelchair. The strength in his left lower extremity was approximating normal by this point in his recovery process, but his right leg remained significantly weaker with no active isolated movement noted in his lower leg and significant spasticity in the right hip and lower leg limiting normal movement during gait. Morrow dropped his therapy hours down to 3 hours per week at this point so that he could better manage his work and family responsibilities. This required Morrow to begin completing more of his rehabilitation program on his own, and his wife soon took away his wheelchair so that his walker was his only choice for mobility. During the 3 hours per week he participated in therapy at Shepherd Center, his locomotor training program was transitioned back to the manual system as his improved strength and spasticity management allowed him to achieve a quality gait pattern with the manual assistance of therapists. Because one of his primary goals was to return to over ground running, it was important to transition him back to the manual system as quickly as possible in order to provide an environment to practice this. Another primary goal of his was to increase his gait speed so that he no longer relied on his wheelchair for community mobility. Therefore, a significant amount of his therapy time was spent on plyometric training in gravity-eliminated and full-gravity positions as well as locomotor training while still incorporating intensive core strengthening exercises.
By December 2006, Morrow had stopped using his wheelchair even for community mobility and now relied only on bilateral straight canes along with an ankle foot orthosis (AFO) for independent mobility. However, Morrow continued to require the use of an AFO on his right leg for walking due to weakness and spasticity. He didn’t like using the AFO because he felt that it left his lower leg muscles dormant while walking and did not allow him to work on strengthening them. However, without the AFO, he was not safe walking and would often trip and fall. The lower extremity FES system was introduced for clinic use in January 2007, and Morrow demonstrated a successful trial and purchased one for full-time use on his right leg to replace his AFO.
The FES system has a gait sensor that is placed in Morrow’s shoe. This sensor activates electrodes placed on the peroneal nerve and tibialis anterior to provide a dorsiflexion response at the appropriate time during the gait cycle to allow foot clearance while stepping. Morrow began using the FES system at all times when ambulating and quickly progressed from ambulating with bilateral straight canes to using just one cane and the FES system. He reported being more confident when ambulating outdoors and over uneven terrain with the FES aid versus his AFO. This device also allowed his treating team to begin working on short bouts of running on the manual body-weight support treadmill as it assists in decreasing the amount of extensor hypertonicity apparent at increasing speeds of locomotor training and assists in providing foot clearance while stepping, which decreases the labor-intensive work by the therapists on the manual locomotor system. Morrow continues to prefer the FES system over using an AFO because he feels he is actually strengthening the weakened muscles causing his continued debility as well as decreasing the spasticity in his plantarflexors, also known to be a contributing factor to his inefficient gait pattern.
Although weak dorsiflexors and spastic plantarflexors remain the primary factors limiting his progress in running over ground and walking without an assistive device, he is now able to demonstrate active isolated movement in the muscles that dorsiflex his foot and his spasticity continues to improve on a weekly basis. Morrow continues to walk full-time in the community using just one cane and the FES system, but often walks household distances with only the use of the FES system. He continues to run for short bouts on the manual body-weight supported treadmill system and continues to pursue the goal of running over ground.
Throughout Morrow’s entire rehab process, he has kept a positive attitude and demonstrated an amazing work ethic. He has been fortunate to complete his rehabilitation process in a hospital committed to providing people with neurological injuries the most up-to-date technology and resources and has benefited from using many different types of these technologies during different phases of his recovery.
Morrow is the loving and very involved father of five beautiful children and the husband of an amazing and supportive wife. He continues to work full-time in the investment industry while playing wheelchair rugby and participating in wheelchair racing. His recovery process has not been easy, but he’s continued to be an inspiration to those around him with his ability to demonstrate a driven work ethic to always strive for more, but at the same time exuding a calm peace in being thankful for how far he has come and all that he has achieved.
 |
Candy Tefertiller, MPT, ATP, NCS, is the clinical coordinator of the Beyond Therapy Program at Shepherd Center Catastrophic Care Hospital in Atlanta. For more information, contact .




