Advancements in technology have provided wheelchair clinics with an array of options for patients who have complex seating and positioning needs. This can be overwhelming and intimidating to clinicians, RTs, and ATPs without an adequate understanding of the technology or the advantages and disadvantages of each type of system. In addition, just keeping up-to-date with products available on the market can be daunting.
The goals for custom seating usually include:
- Improving functional postures for participation in self-care, educational, and social activities
- Increasing comfort
- Minimizing the progression of current deformities
- Controlling abnormal reflexes and muscle tone
- Evenly distributing pressure for skin protection and reducing pressure points
- Improving trunk and head control
- Increasing upper extremity function and manipulation
- Improving eye gaze and visual tracking
Custom seating includes a wide range of products that can be further categorized. This consists of plaster molds, foam-in-place seating (FIPS), digital technology, and aftermarket or manufactured custom-contoured seat cushions and backs. Furthermore, durable medical equipment providers can opt to fabricate their own custom seating systems in their on-site workshops; however, if they choose to manufacture their own seat cushions and backs, funding may be limited without proper PDAC (Medicare Pricing, Data Analysis, and Coding) approval.
For the purpose of this article, the various types of custom molded seating systems will be analyzed in an attempt to outline the technology, and the benefits and drawbacks of each type.
PLASTER MOLDING
It has been reported that custom seating supports have been utilized since the late 1960s. Early inventions in custom molds included a vacuum forming plastic around a plaster mold, which was developed by Douglas A. Hobson, PhD, and colleagues.1 Today, plaster molds are still available and utilized in wheelchair clinics. This method includes taking a plaster cast of a mold formed from rubber bead-filled bags controlled through a vacuum/air compressor. The bag is usually placed in a wheelchair-like frame with some of the air removed to allow it to be preshaped. The patient is placed on top of the rubber bag while maintaining the maximal spinal correction or accommodation to achieve function and comfort. When the final shape takes place, the air is removed from the bag, compressing the beads, and making it rigid in order to maintain the shape. The patient is then transferred out of the wheelchair to either another wheelchair or a mat surface. From here, a plaster-casted image of the mold is taken from the shaped rubber bag using multiple layers of plaster bandages. Once a successful plaster image has been made, the cast of the custom molded seat cushion or back can be fabricated into an actual seat or back from material such as polyurethane foam.
ADVANTAGES AND DISADVANTAGES
Plaster cast molds are easily used for patients who have hypotonia and mild to moderate spinal or orthopedic deformities, such as those with cerebral palsy, spina bifida, and muscular dystrophy. They can also be used for patients with spinal cord injuries and lower extremity amputees. However, they are messy and the fabrication process is time-consuming. The process of fabricating the mold takes multiple steps in itself even before the patient returns for the first fitting. In addition, if the air compressor malfunctions or is disconnected accidentally prior to completing the plaster cast shell, the mold will be lost and the patient will have to return to the wheelchair clinic for a second mold. Modifications to the foam molds once they are fabricated from the plaster image can be time-consuming and may involve several visits with patients who have complex deformities. This technology requires advanced skill, technique, and experience to adequately fabricate a custom mold in a timely and efficient manner. Furthermore, the vacuums/air compressors can be loud and noisy. Ultimately, some patients who have cognitive impairments or spastic muscle tone, are easily agitated, or have sensory impairments may not be able to tolerate the noise and time involved with systems that utilize powered air compressors.
FOAM-IN-PLACE SEATING (FIPS)
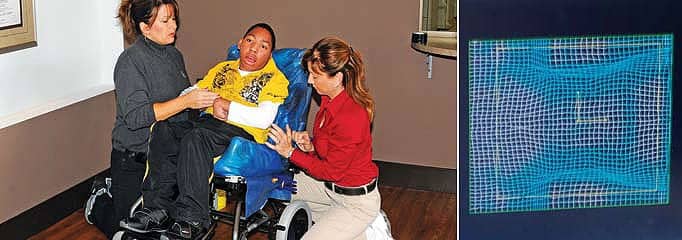
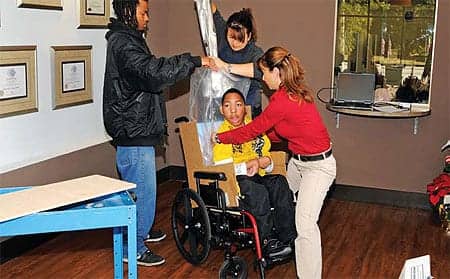
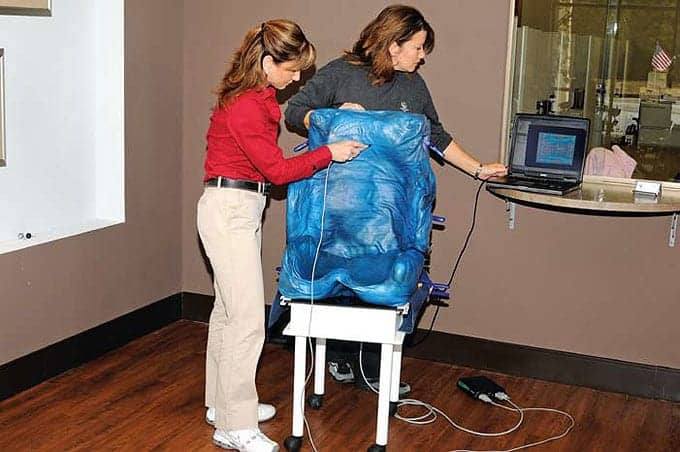
Polyurethanes are widely used in high resiliency flexible foam seating. The foam-in-place kits consist of two-part (polyol and catalyst) chemicals. Once the two are mixed, a chemical reaction causes an expansion or foaming action that creates polyurethane memory foam. This foam begins to harden after 5 minutes and can take approximately 10 minutes to completely set. In order to complete this type of mold, the wheelchair seat and back pans are usually made of wood, aluminum, or ABS plastic material. Clear plastic bags are used to contain the chemical mixture while the foaming process takes place. As the mixture begins to expand, the patient is placed on top of the bags to allow the foam to fill in the mold and capture the desired posture and spine alignment. Cardboard can be used on each side of the wheelchair base to prevent excessive foaming around the outside of the base. Because the foam begins to expand within minutes, the molding process has to be completed quickly and accurately. Once the foam begins to harden, the patient’s desired posture must be maintained, while manipulating the foam’s expansion at the same time. This may require several people to assist in the molding process depending on the severity of the patient’s deformities, muscle tone, and abnormal reflexes.

Authors Mary Hitt Young, ATP, RRTS (left), and Cindi Petito, OTR/L, ATP, CAPS (right), employ the foam-in-place technique to create customized seating for their young client.
ADVANTAGES AND DISADVANTAGES
Foam-in-place systems are good in obtaining instant results. Because this process allows the foam to expand, the foam has the ability to fill in deep concave spinal curves and asymmetries, and capture severe deformities such as scoliosis with rib hump and lordosis. If the mold is successful, modifications can be made soon after it has hardened. However, if an adequate mold is not obtained and it cannot be modified to meet the patient’s seating needs, the process has to be started all over again with a new foam-in-place mixture. Basically, it’s a one-time shot to get it right. So, just as with plaster molds, they require advanced skill, technique, and experience. The foaming process gives little time for the patient’s posture to be properly aligned before the foam begins to harden. Because a chemical reaction occurs when the fluids are combined to start the foaming process, some heat is generated that can be felt on the surface of the bags. Patients with impaired skin sensation may be irritated by this warming sensation. Patients with impaired cognition and behavioral or sensory impairments may become agitated by the tactile sensation of the heat and the amount of manipulation required during the molding process. Patients with significant hypotonia may be challenging to mold if adequate assistance is not available due to limited fabrication time.
As stated above, we have found in our clinic that patient populations with profound physical and mental disabilities, such as cerebral palsy with mental retardation, can be extremely challenging to custom mold with plaster. This is also true of foam-in-place molds because of severe spastic or mixed muscle tone, startle reflex, and other abnormal reflexes. These patients may present with high agitation, constant and repetitive movements, and socially inappropriate behaviors that make these types of molds difficult for the rehab team.
DIGITAL TECHNOLOGY
The integration of computer-aided design and manufacturing (CAD/CAM) has been around for decades. Originally developed in the mid-1950s for use in the US military, CAD/CAM technology quickly spread throughout the orthotic and prosthetic industry. However, capabilities were partially limited due to existing computer technology at the time. Today, these digitizing systems are widely used throughout the custom wheelchair and seating industry to capture 3D images of a patient’s spinal and orthopedic deformities within a wheelchair-based seating simulation, resulting in a precise custom-contoured mold. The shapes are first captured by using the bead-filled bags and a powered or nonpowered air pump. Just as the vacuum and bead-filled bags are used with plaster molds, the air is removed from the bags to compress the beads, making the mold rigid in order to maintain their shape. The image of the mold is captured by using the CAD/CAM digitizing software, which can be modified immediately to the desired specifications and stored in the computer. The saved 3D computer image is then sent as a digital file to a computer-controlled carver to produce the foam mold.
ADVANTAGES AND DISADVANTAGES
As computer technology has improved, so have digitizing programs. Once the premold is completed with the bead-filled bags, the digitizing process that captures the 3D image is quick and easy. The fabrication time is decreased due to less materials needed and the ability to make modifications within the digitizing software during the molding process. Modifications, such as soft spots for protruding boney prominences, can be seamlessly incorporated into the mold’s image through the software. If there are time constraints with visits, the 3D images are saved in the computer and can be revisited at a later time. Communication is also improved because of the ability to share computer files with other members of the rehab team. Additionally, no messy foams or chemicals are used, and patients do not experience the discomfort (heat and manipulation) compared to foam-in-place. In patient populations with profound physical and mental disabilities, we find this type of system to be more comfortable and more compatible for use in the wheelchair clinic, in community settings, and in the home. This allows us to meet the needs of a wide range of patient populations with congenital disorders, neuromuscular diseases, spinal deformities and injuries, and orthopedic conditions. Typically, when using digital technology, efficiency, accuracy, and versatility are greatly increased while labor, cost, and unforeseeable environmental risks and restrictions are greatly reduced.
OFF THE SHELF
When it comes to wheelchair seating, it is critical to maintain function, comfort, and support, and protect against any pressure-related issues. There are many important variables to consider when choosing the appropriate custom seating. Some of these include pelvic and lumbar support, pressure relief, trunk and head support, angle adjustment, and comfort. For those patients who need more than standard aftermarket products, but not custom molded seating, clinicians and seating specialists have the option of using aftermarket custom-contoured cushions and backs with separate positioning kits that may be added for a more customized fit.
Aftermarket seat cushions are manufactured in a variety of different materials and support surface combinations that include foam or flexible polyurethane, rubber latex, honeycomb plastic, viscous fluid, gel, and air. Aftermarket seat cushions can be customized by using separate kits that include additional support pads, such as foam lateral hip and thigh guides, foam medial thigh supports, and foam or gel pelvic obliquity pads. Some seat cushion bases are made of foam that can be cut and modified in the field during the fitting process to accommodate deformities, such as leg length discrepancies, hip flexion contractures, and posterior pelvic tilts. Seat cushions may also include built-in support by the manufacturer ranging from mild contouring to max contouring depending on the amount of pelvic and thigh support needed. Another type of built-in custom support includes the adjustable air-filled seat cushions that allow for support of pelvic obliquities or relief off an area where skin breakdown or boney prominences are present.
Back supports are generally molded from aluminum or hard plastic shells and memory foam pads. The backs can support the trunk laterally using two different types of support systems, which include separate swing-away or fixed lateral pads, and built-in wrap-around shells that are molded into the back by the manufacturer. To customize these backs to fit the end user and support spinal or postural deformities, extra pads can often be added to the back under the upholstery or foam pad. These include foam or gel pads for lumbar and mid to upper thoracic spinal deformities, such as hyperlordosis, kyphosis, scoliosis, trunk rotation, and pelvic rotation. Just as with seat cushions, some backs offer a foam support that can be cut and modified during the fitting process to accommodate spinal deformities and protruding boney prominences.
Aftermarket custom seat cushions and backs, with their extra support pads and adjustable features, can be fit in the field easily. There are a wide variety of seat cushions and backs to choose from on the market today to meet individuals’ needs and properly fit for function.
PRESSURE MAPPING
When using any of the custom seating systems mentioned above, pressure mapping is an important component and should be considered in the process. It can be used for comparison of peak pressures before and after custom seating is completed, patient and caregiver education regarding the importance of weight shifts and prevention of skin breakdown, medical documentation, and justification for funding sources. It can assist clinicians and seating specialists in determining if custom molded seating is needed with complex patients and which foams and fabrics will best alleviate pressure.
Working together as a team is essential to choosing the right seating system for patients with complex seating and positioning needs. Completing a comprehensive evaluation of patients, their family and caregiver needs, and their environment will assist the rehab team in the decision-making process. Funding can be an obstacle in this process. However, there are many options to choose from for custom molded and custom-contoured seating. Choosing the right custom seating is important to maximizing function, support, and comfort.
Cindi Petito, OTR/L, ATP, CAPS, owner of Seating Solutions Inc, Orange Park, Fla, has been a private practitioner for 12 years, specializing in the area of complex rehab seating, mobility, and home modifications for adults with neurological injuries and diseases. Mary Hitt Young, ATP, RRTS, with more than 15 years of experience, is employed by Wheelchairs Plus Inc, Middleburg, Fla. She specializes in the area of complex rehab seating and mobility for those with severe physical and neurological disabilities.
REFERENCE
- Hobson D, Driver KD, Hanks S. Foam in place seating for the severely disabled: preliminary results. In: Proceedings of the Fifth Annual Conference on Systems and Devices for the Disabled; June 1978; Texas Institute of Rehabilitation and Research, Houston; page 154.