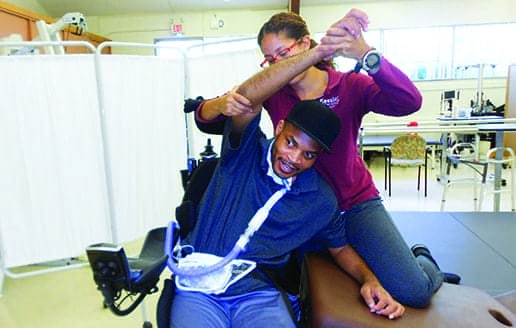
Joe vocalizing phoneme combinations while the occupational therapist stretches him in lateral forearm prop position.
by Barbara Garrett, PT, NCS, Lorena Salas, OTR/L, and Alyson Golding, CCC-SLP
One of the most devastating injuries causing long-term impairment is a traumatic cervical spinal cord injury with significant neurologic impairment. This case study highlights the effectiveness of a collaborative therapy approach as part of an overall inpatient interdisciplinary rehabilitation plan of care for a patient with a severe spinal cord injury (SCI).
Joe, a 41-year-old male, was at work when a heavy package fell from a shelf and struck him on the head. He required CPR on the scene and was transferred to a nearby hospital, where a neurologic examination revealed a C2 AIS A spinal cord injury. Unable to breathe on his own, Joe was placed on a ventilator and underwent numerous surgical interventions including placements of a halo vest, tracheostomy tube, and feeding tube. He demonstrated no skeletal strength and also experienced bradycardia and episodes of hypotension while in the hospital.
Two weeks after the injury, Joe was deemed medically stable and transferred to Kessler Institute for Rehabilitation in West Orange, New Jersey. Kessler is one of only 14 centers in the United States to hold federal designation as a Model System for the treatment and research of spinal cord injuries, and offers a highly specialized ventilator-dependent program. During his inpatient rehabilitation stay, Joe participated in a comprehensive, integrated program of occupational, physical, and speech therapies. These interventions combined with specialized medical and nursing services resulted in a successful discharge to home.
Developing a Plan of Care
Upon admission to Kessler, Joe was evaluated by a physiatrist, a board-certified physician specializing in physical medicine and rehabilitation, who is also board certified in SCI medicine. He was then assigned to an interdisciplinary rehabilitation team that included a primary nurse, respiratory therapist, case manager, dietitians, and psychologist, as well as physical (PT) and occupational (OT) therapists and a speech language pathologist (SLP). Based on the comprehensive evaluation of his medical, physical, and functional needs, the team developed an integrated plan of care with short- and long-term goals that was subsequently updated as Joe progressed. The primary objective was to create a safe and effective discharge plan for Joe and his family. Communication between the lead PT, OT, and SLP was critical not only to set realistic therapeutic goals, but to initiate the interventions that would enable Joe to maximize access to his environment and optimize his quality of life.
Innovative Treatment Innovations
With a medically complex patient, members of the interdisciplinary team must exchange information continuously to assist one another in providing goal-directed care and to allow those goals to be modified as the individual progresses. For Joe, the initial therapeutic focus was to establish effective methods for communication, train him on use of assistive technology to access his environment, engage him in patient and family education and training, and provide the appropriate durable medical equipment.
At the beginning of his stay, Joe was on a mechanical ventilator and his speech was not audible. As the SLP concentrated on tolerance of tracheostomy cuff deflation and coordination of ventilator cycles with vocalization during deflation trials, the PT and OT worked on maximizing speech to improve use of electronic aids to daily living (EADLs), instruction of care, and socialization by incorporating the strategies learned. The OT also incorporated mass practice of phoneme combinations with guidance from the SLP in sessions during positioning (eg, iron cross, posterior prop, anterior trunk flexion, upright in wheelchair). Across all disciplines, the therapists instructed Joe on secretion management techniques to improve phonation when experiencing decreased vocal quality.
Of paramount importance was Joe’s ability to communicate with as much independence as possible. Given Joe’s impaired phonation combined with his inability to move his head because of the halo, the OT trained Joe how to utilize a tongue switch for a call bell. Once the halo was removed, he learned how to use a head switch to access his phone when in bed through the use of a Bluetooth switch interface.
Furthermore, to improve efficiency with phone and computer access, Joe worked with his OT and SLP, who introduced voice activation technology, such as iOS Siri on a cell phone and speech recognition software on a laptop, which helped provide biofeedback for vocal functioning and served as a functional task to work on high-level cognition. The OT also helped Joe order a smartphone, Bluetooth switch interface, laptop, speech recognition software, and a switch to carry over these skills once discharged from inpatient rehabilitation. Improving his ability to access his phone and computer would allow him to potentially control his home environment, such as lights and television, and enable him to perform tasks on his computer related to any potential work leisure or personal activities, such as managing his finances.
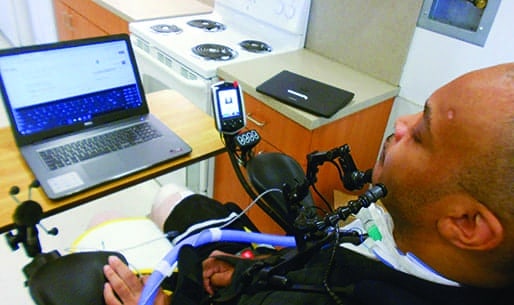
Joe trialing the Bluetooth mouse feature in his personal power wheelchair using the mini joystick at his chin to control his personal laptop.
Working Together to Restore a Voice
The OT, PT, and SLP also encouraged the coordination of ventilator-supported speech by having the patient speak during the inspiratory phase of the vent cycle to have him both direct his care and communicate his needs during therapy sessions. On a weekly basis, the PT and OT had Joe verbalize the weight shift protocol, stretching techniques, how to identify medical emergencies related to respiratory status and blood pressure management, and positioning in both the wheelchair and bed. The OT also had Joe practice instructing mechanical lift transfers, assistance required for dressing, and setup of his assistive technology for use.
Joe was not a candidate for weaning from the ventilator due to the level and severity of his injury. However, a nerve conduction study/EMG assessment revealed the possibility of diaphragmatic pacing with electrical stimulation that would allow time off the ventilator. He underwent placement of the diaphragmatic pacer at a nearby acute care hospital and returned to Kessler to continue his rehabilitation, where he was able to spend increasing time off the ventilator. At first, Joe participated in weaning only when in his therapy sessions or one-on-one with the respiratory therapist who collaborated with the PT, OT, and SLP in sharing observations and management strategies.
With the device placed, Joe worked with the SLP on tolerance of the pacer when speaking, as well as speaking valve placement and eventually capping tolerance. He had to be trained to speak on the exhalation while pacing, in contrast to speaking on the inhalation when he was on the ventilator. The OT and PT also worked on his breathing while weaning by incorporating bubble blowing to improve diaphragmatic strength. Working closely with the psychologist, the therapists were able to wean the patient in a variety of settings, which helped alleviate some of his anxiety and encourage maximal weaning time.
Mobility and Standing
Physical therapy’s wheelchair specialist focused on selecting an appropriate wheelchair seating system for Joe, one that included head and trunk support. Pressure mapping was conducted to ensure adequate pressure relief and offer evidence-based direction in choosing the optimal system. In addition, to increase Joe’s tolerance to upright and seated positioning, the PT and OT used a variety of strategies and tools, such as a tilt table. Upon delivery of his customized power chair, the wheelchair specialist and OT joined forces to train Joe to operate the mini joystick to drive, to perform positional changes, to use the mouse on his laptop, and to access his phone through the chair’s Bluetooth.
As Joe’s neuromuscular recovery progressed, marked by returning motor function especially in his left upper and lower extremities, his team introduced higher-level therapeutic interventions. For example, with removal of the halo vest, he was able to trial more durable medical equipment, including low air loss turning mattresses designed to reduce the risk of pressure injuries and a roll-in tilt shower/commode chair to provide necessary support during toileting and bathing once he returned home. The PT was also able to trial a standing frame as well as supported standing in a platform walker to provide Joe with additional options.
Preparing for Discharge Home
Having imparted the skills, strategies, and technologies to enable Joe to return home, his team focused on planning a safe discharge. As noted, patient and family education is an integral part of both the rehabilitation and discharge process, and much of that training is provided by the therapists, along with nursing staff. Joe’s external case manager, fiancée, and his entire Kessler team participated in meetings and training sessions to better plan and facilitate this process. Although Joe was going to have care provided by aides/nurses, the therapy team taught his fiancée all aspects of care, as well as the use and maintenance of his equipment. Having received this specialized training and education, she could assist Joe in instructing hired caregivers on SCI-specific issues. Given the extent of information and hands-on extensive training required, the therapists divided the topics to ensure all aspects of care were covered.
To support a smooth transition home, staff from the home nursing agency met with members of Kessler’s team in order to become familiar with Joe’s daily needs, focusing primarily on his bowel/bladder and respiratory requirements. Although the diaphragmatic pacing trials successfully allowed Joe to be off the ventilator for hours at a time, the respiratory therapist did help to procure the necessary respiratory equipment, including a portable ventilator that fits on Joe’s wheelchair, a speaking valve for daytime use, and an in-exsufflator for secretion management.
Extensive home modifications were completed based on the recommendation of the rehabilitation team. Ramps were installed to stairs, an accessible bathroom with roll-in shower was constructed, and an accessible bedroom was created to provide Joe with as much independence and comfort as possible.
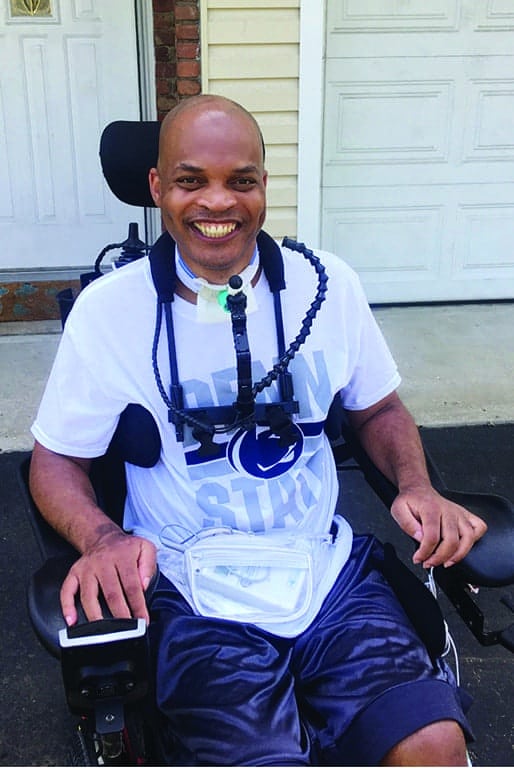
Joe sitting in his personal custom power wheelchair with mini joystick drive outside of his remodeled home, after discharge.
Summary
In many cases, a medically complex, spinal cord-injured patient who is ventilator dependent is discharged to a long-term care or nursing facility. For Joe, however, the unwavering support of his fiancée, an effective insurance plan, home modifications and home health care, and the interdisciplinary approach to treatment by his Kessler Institute team allowed for a successful discharge to home. And despite his life-changing injury, Joe admits that it is great to be home again.
A Follow-Up Note
Joe received home therapy and then attended outpatient therapy where he participated in therapeutic ambulation trials and has continued to make functional gains with strength returning to his trunk and extremities. He is now able to utilize the diaphragmatic pacer throughout the day and night, and relies on the ventilator only sporadically. RM
Barbara Garrett, PT, NCS, is a Board-Certified Clinical Specialist in Neurologic Physical Therapy. She graduated from Thomas Jefferson College of Allied Health and is an advanced specialist at Kessler Institute for Rehabilitation—employed for 31 years with a specialty in spinal cord injury, ventilator dependent, and other neurological disorders.
Lorena Salas, MSOTR/L, received her Master of Science in Occupational Therapy at Stockton University and is a Senior Occupational Therapist at Kessler Institute for Rehabilitation. She has been practicing for 4 years and specializes in the evaluation and treatment of neurological disorders.
Alyson Golding, MS CCC-SLP, completed her Bachelors of Science in Speech, Language and Hearing Sciences and Masters of Science in Speech-Language Pathology at Boston University. She has been practicing for 3 years and works at Kessler Institute for Rehabilitation where she primarily works with the Spinal Cord Injury, Ventilator Dependent and Brain Injury populations. For more information, contact [email protected].
This article appears in the 2018-19 Rehab Management Fall Product Directory as “Returning Home.”





That’s amazing that such a team helped Joe with his rehabilitation process, including a respiratory therapist, dietitian, and psychologist. You don’t always think about how much a spinal injury can affect so many different parts of the body. If I had a member of my family get in a similar accident, I’d like to think they could get some rehabilitation that will improve their quality of life.
Can go beyond living at home; vocational rehabilitation services are possible & can be explored with options for training, retraining with accommodations if necessary.