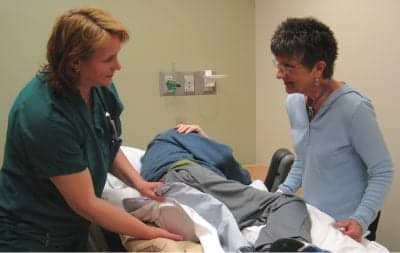
Patient is placed on a static air mattress overlay to protect skin integrity as Sharon Lucich, PT, CWS, at left, conducts a routine assessment
In October 2008, the Centers for Medicare and Medicaid Services (CMS) announced they would no longer provide reimbursement for a variety of hospital-acquired conditions, including pressure ulcers. Facilities continue to be held accountable and are responsible for treating any pressure ulcers that develop during a patient’s hospital stay. The magnitude of these policy changes is reflected in a statistic that reveals an average 4.8-day hospital stay turns into a 13-day stay when a pressure ulcer occurs, costing the facility an average of $43,180 to treat only the wound.
As pressure ulcers continue to develop more frequently nationwide—with a 63% increase over the past 11 years—understanding their seriousness and complexity has never been more important for physical therapists. Now and into the future, it is integral that they develop appropriate medical practice guidelines and address government regulations, legal responsibilities, and financial implications. To do so, physical therapists must receive a proper education about pressure ulcers, which includes mastery of identification and prevention methods, as well as treatment strategies proven to enhance the quality of care for their patients.
Because pressure ulcers can develop within 2 hours to 6 hours, it is important for all therapists to know what to look for and how to properly identify and classify a potential pressure ulcer when assessing patients. A pressure ulcer is defined as a localized injury to the skin and/or underlying tissue that usually develops over a bony prominence as a result of pressure, or pressure in combination with shear. The “bony prominence” particularly refers to the heel, sacrum/coccyx, greater trochanter, ischial tuberosity, lateral malleoli, elbows, and occiput. These areas of the body should be closely monitored at all times and routinely checked throughout every assessment because of their potential for increased pressure, friction, and shear.
When pressure ulcer detection, prevention, and treatment are discussed in the acute care setting, these tasks are often delegated to registered nurses (RNs) and certified wound and ostomy care nurses (CWOCNs) and depend on routine patient assessments. With that said, there are a multitude of preventive measures physical therapists can and should initiate to help play a more active and complementary role in hospital-wide pressure ulcer prevention strategies. To begin, skin assessment screens can be added to all initial evaluations as part of the systems review. When looking for potential or developing pressure ulcers, it is of the utmost importance for therapists to roll patients in each direction to allow for a full view of all high-risk areas, including bony prominences. Upon thorough analysis of the skin, one must closely analyze the pliability or texture, color, integrity, and presence of scar formation. All findings must then be documented and shared with all members of the health care team. It is during these assessments that therapists can take accountability for identifying, documenting, and reporting issues regarding skin integrity.
Pressure ulcers are known to have many contributing factors, although the significance of these factors is yet to be elucidated. Physical therapy personnel must understand the role that age, impaired sensation, malnutrition, and restricted mobility play in pressure ulcer incidence. Elderly, immobile patients are more susceptible to pressure ulcers because of their atrophied muscle, diminished inflammatory response, and limited protective sensation reaction. Similarly, malnourished patients often exhibit increased potential for pressure ulcer occurrence due to the state of their body and its decreased ability to heal itself. Finally, patients with impaired sensation are unable to recognize pressure-related pain. All of these factors require the expertise and education of the physical therapy staff in order to prevent and/or treat incidence of pressure ulcers in a timely, effective manner.
Upon identification of at-risk or questionable areas on the skin’s surface, it is necessary for physical therapists to properly categorize the sore in order to extrapolate the most effective care plan for treatment. The different types of pressure ulcers and their corresponding descriptions are:

Therapist explains the use and benefits of a static air seat cushion.
1. Stage I: Intact skin with non-blanchable redness of localized area that is usually over a bony prominence. Patients with darkly pigmented skin may not have visible blanching. Its color may differ from the surrounding area.
- Stage I pressure ulcers are painful, can be firm or soft, warm or cold, and are difficult to detect in dark skin.
2. Stage II: Partial thickness loss of dermis presenting as a shallow open ulcer with a red pink wound bed without slough. It may also present as an intact or open/ruptured serum-filled blister.
- Stage II pressure ulcers are shallow ulcers without slough or bruising that can appear shiny or dry.
3. Stage III: Full thickness tissue loss where subcutaneous fat may be visible but bone, tendon, or muscle is not exposed. Slough may be present but does not obscure the depth of tissue loss.
- Stage III pressure ulcers’ depth varies by anatomical location and may include undermining and tunneling.
4. Stage IV: Full thickness tissue loss with exposed bone, tendon, or muscle. Slough or eschar may be present on some parts of the wound or bed.
- Stage IV pressure ulcers’ depth also varies by anatomical location and often includes undermining and tunneling. They can extend into muscle and/or supporting structures to make osteomyelitis possible.
5. Unstageable: Full thickness tissue loss in which the base of the ulcer is covered by slough (yellow, tan, gray, green, or brown) and/or eschar (tan, brown, or black) in the wound bed.
- Unstageable pressure ulcers have true depth, therefore stage cannot be determined.
6. Deep Tissue Injury (DTI): Purple or maroon localized area of discolored, intact skin, or blood-filled blister due to damage of the underlying soft tissue from pressure and/or shear.
- DTIs may be preceded by tissue that is painful, firm, mushy, boggy, warmer, or cooler as compared to adjacent tissue.
THERAPEUTIC INTERVENTIONS
As soon as a pressure ulcer has been detected or a patient has been designated at risk, it is important for physical therapists to initiate therapeutic interventions that will prevent occurrence or progression of the ulcer. Sometimes this can be as simple and cost-effective as adding a static overlay mattress or cushion to help redistribute the pressure. In addition to being cost-effective, a static air mattress can be used when mobilizing patients (ie, transferring, turning, and rolling), as this method of mobilization ensures that the patients’ skin remains protected at all times and escapes further damage. Furthermore, static air devices are available for the bed, seat, or foot to ensure continuous pressure redistribution. An advantage associated with the use of static air devices is that they can be sent home with the patient or to the next level of care for proper prevention and/or healing.
Often, the presence of pressure ulcers warrants use of a specialty bed for added protection and pressure redistribution, depending on the depth of injury and associated comorbidities and risk factors. When considering the options for a new bed purchase, patients’ function, mobility, and pulmonary status must be assessed, warranting a multidisciplinary decision-making process that takes into consideration the high cost generally associated with use of specialty beds.
Physical therapists must also address incontinence, which places a patient at higher risk for pressure ulcer development. Urinary incontinence adds moisture to the skin and decreases the skin’s integrity, making a patient more likely to experience friction, shear, and erosion. Fecal incontinence also affects the skin’s integrity by disrupting the normal microflora on the skin and creating an opportunity for pathogenic colonization. Medical literature continues to illustrate a strong association between fecal incontinence and pressure ulcers. To best address incontinence issues, physical therapists must respond immediately, instead of waiting for the availability of a nurse. To properly cleanse and protect the affected skin, therapists should proceed with gentle cleansing measures, while avoiding any form of scrubbing. The use of cleaning wipes to cleanse the problem area is preferred to using soap and water, which can change the pH of the skin and cause damage to lipid barriers.
In summary, pressure ulcer prevention and treatment strategies can be implemented among all caregivers in a medical setting, including physical therapists. By increasing awareness, education, and implementation, physical therapists are given the opportunity to play a proactive role in helping to reduce hospital-wide pressure ulcer incidence. Due to the severity and cost implications associated with pressure ulcers, facilities can no longer rely on a few wound care specialists. Pressure ulcer prevention and treatment should be on the minds of all acute care personnel and encouraged across the continuum of care. In health care, the goal is the highest possible caliber of patient care, which includes incorporating the measures discussed in this article that will result in pressure ulcer prevention and enhanced quality of life for patients.
Sharon Lucich, PT, CWS, has over 23 years of clinical experience at Indiana University Health Methodist Hospital, a level one trauma center in Indianapolis, where she was integral in developing a physical therapy presence in wound care in the acute care setting. Lucich serves as adjunct faculty in the doctorate physical therapy program at Indiana University in Indianapolis, as instructor of the integumentary practice patterns course.
Jaimee Haan, PT, CWS, is the team leader of the Physical Therapy Wound Management Department at Indiana University Health Methodist Hospital-Outpatient Physical Therapy Wound Management Department in Indianapolis. Haan has played a central role in the development and growth of inpatient and outpatient physical therapy wound management programs. For more information contact .
RESOURCES
Armstrong DG, Ayello E, Capitulo K, et al. New Opportunities to Improve Pressure Ulcer Prevention and Treatment: Implications of the CMS Inpatient Hospital Care Present on Admission (POA) Indicators/Hospital-Acquired Conditions (HAC) Policy: A Consensus Paper from the International Expert Wound Care Advisory Panel. Adv Skin Wound Care. 2008;21:469-478.
Bolton L, Girolami S, Slayton S, et al; Association for the Advancement of Wound Care Guideline Subcommittee. Assessing the need for developing a comprehensive content-validated pressure ulcer guideline. Ostomy Wound Manage. 2008;54:22-29.
Fleck CA. The new CMS pressure ulcer guidelines. ECPN. January-February 2005:36-4.
Gray M. Moisture associated skin damage and its relationship to IHI Pressure Ulcer Prevention and Interventions. Presented at: VHA Central: IHI 5 Million Lives Pressure Ulcer Intervention Program. September 2007.
National Pressure Ulcer Advisory Panel. Pressure ulcer stages revised by NPUAP. Available at: www.npuap.org/pr2.htm. April 2008.
Pemberton V, Turner V, VanGilder C. The effect of using a low-air-loss surface on the skin integrity of obese patients: results of a pilot study. Ostomy Wound Manage. 2009;55:44-48.





