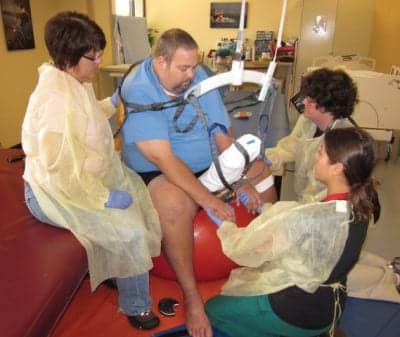
Traditional treatment for bariatric cases can be restricted by a patient’s pain and size. In this example upright sitting is achieved using an overhead lift and weight-accommodating therapy ball.
In 2009, approximately 26.7% of the US population were classified as obese with an even larger number of individuals categorized as overweight. Treating bariatric patients with spinal cord injury (SCI) can be a unique challenge that requires a team approach as well as appropriate equipment for both the safety of the patients as well as the staff. This article explores the barriers to treating a bariatric SCI patient and the innovative solutions required to overcome these obstacles.
In addition to the comorbidities associated with obesity, the clinical staff must be prepared and have structurally sound equipment and clinic surroundings (large beds, wide doorways and halls) to accommodate these individuals. Typical equipment for treating SCI patients (locomotor devices, mats, therapy balls, mobile arm supports, and wheelchairs) may accommodate obese individuals but is often not rated for individuals who weigh more than 300 to 350 pounds. Many adjunct modalities and activity-based therapies that benefit patients with SCI may not be appropriate because of weight/width limits and comorbidities. These include body-weight supported devices, aquatics (open airway), electrical stimulation, FES bikes, mobile arm supports, and standing frames. However, over the course of rehabilitation as patients lose weight, appropriate equipment and devices can be incorporated into therapy. Another consideration is the number of clinical staff required to safely mobilize the patient.
Case Presentation: The patient is a 6’5″ 38-year-old male status post-motor vehicle collision resulting in C3-4 central cord injury. Three weeks after the accident, he transferred from acute care to a rehabilitation hospital. According to the referral, he weighed 401 pounds. Upon admission, however, he weighed 477.8 pounds. He presented with an open airway. He also had neurogenic dysesthesia throughout his body and pain in all extremities at end range, particularly in his hips and shoulders. He had no functional movement and presented with only trace contractions in his bilateral biceps, triceps, and left hip adductor. Upon admission, the plan of care included a full evaluation, gathering equipment with proper weight ratings, mobilizing the patient through passive range of motion (PROM) to his extremities while in bed, and positioning him in a power tilt wheelchair to begin building his sitting tolerance in preparation for rehab.
Barriers to a traditional rehab course included turning and positioning in bed, equipment that did not accommodate his weight, and difficulties providing PROM secondary to pain and excessive limb weight. He required the assistance of several people for turns and positioning and for passively ranging his limbs safely. In addition, evaluation was limited secondary to excess adipose tissue, which made palpation for trace contractions and trialing electrical stimulation difficult, and problems positioning him comfortably in bed in order to maximize his ability to move his limbs in a gravity-eliminated position for muscle testing.
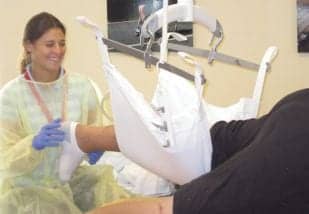
Figure 1
In addition to his size, he was grossly edematous and was placed on a bariatric bed with a specialty mattress. The bariatric bed presented new concerns for staff safety as the width of the bed created positioning and turning difficulties and made general nursing/therapy care challenging to perform with proper body mechanics. Commonly, a draw sheet is used for positioning patients in bed. However, this can create shearing and lead to skin breakdown as well as staff injuries. In this case, a Guldmann repositioning sling and the overhead lift were used to position the patient instead. This not only provided increased comfort and skin protection for the patient, but helped to alleviate the burden on staff and the potential for injury while turning and positioning him.
Given the difficulties and safety issues presented when handling the patient’s limbs, particularly his lower extremities, occupational therapists fashioned a sling made with two pillow cases sewn together. Webbing loops were attached so the sling could be connected to the overhead lift, and a foam egg crate was placed inside the pillow cases to provide structure and comfort to the sling. When the pillow case sling was connected to the lift, the patient’s extremities could be placed safely in the sling, allowing him to attempt to move his joints and activate his muscles in a gravity-eliminated position (Figure 1). This also alleviated the strain on staff caused by supporting his limb while evaluating for trace muscle contractions and providing P/AAROM. His trunk musculature was evaluated by placing him on a tilt table inclined to 55º-60º with two therapists controlling his upper extremities while he actively flexed his trunk forward by attempting to perform a situp. Although he was able to activate his trunk in this position, back pain was a limiting factor and he did not tolerate further sessions on the tilt table.
Mobilizing the patient from the bed to a wheelchair required a sling and an overhead lift. Caution must be taken with the sling sizing to ensure the straps are long enough to provide adequate support under the thighs while not shearing or pinching the skin in the groin. A foam cushion was used to protect the groin in this case as the patient had preserved sensation throughout his body (Figure 2).
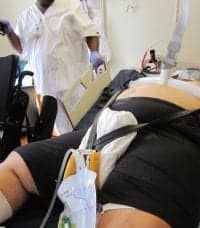
Figure 2
In addition to being familiar with weight limits for wheelchairs and wheelchair accessories such as cushions, it is important to be familiar with the specified weight limits for tilting mechanisms as a tilt generally may be rated at a lower limit than the wheelchair itself. In this case, the wheelchair had a 500-pound weight limit but the tilt mechanism was limited to 400 pounds. For this patient, the seating clinic was consulted early to acquire a wheelchair and cushion with an appropriately rated tilt mechanism. In the interim, to avoid placing the patient on bedrest, pressure relief was achieved by suspending him using the overhead lift rather than using the wheelchair tilt mechanism. It is also important to note that pressure mapping a patient while sitting upright in addition to mapping in a reclined position is recommended as weight shifts in some obese individuals do not guarantee pressure relief. Frequent and thorough skin checks should still be performed even if pressure mapping indicates adequate pressure relief. Another consideration to keep in mind when providing equipment is cushion weight limits, which can vary based on the dimensions of the cushion required. In this case, a high profile cushion was used for two reasons: weight capacity (650 pounds) and comfort (Figure 3).
Moisture in skin folds can be a challenge for skin protection and integrity so proning for extended periods of time provides full weight relief of the posterior and allows airflow to promote drying of the skin. Initially, the patient’s sitting time was limited in an effort to provide skin protection. In addition to using the overhead lift to provide some pressure relief, proning was used. Other benefits of proning include prolonged stretching of the hip flexors, which can become tight from prolonged supine, side-lying, or upright seated positions; weight-bearing through the upper extremities; and strengthening of the scapular and peri-scapular musculature. In patients with skin issues, this also allows an opportunity to get off the wound, provide for more thorough skin inspections than what can be achieved when rolling side to side in bed, and promote wound healing.
However, proning a patient of this size requires a great deal of planning. In this case, the challenges in addition to his size included an open airway, pain, and his inability to assist with positioning himself. Proning initially required four therapists, a nurse, and a respiratory therapist to be present. To prepare for proning, two height-adjustable mats with appropriate weight limits were placed side by side. A platform was fashioned on one mat using wedges, pillows, and a head support. To protect his trach during proning, a high wedge was used to “float” his neck. A positioning sling was placed over the top of the platform for returning the patient to his original position. The other mat had no gym equipment but had a positioning sling placed on it. It was raised to meet the level of the platform on the second mat so the two surfaces were level. The patient was transferred from his bed or wheelchair using the overhead lift onto the first mat in supine and placed on the positioning sling. One side of the sling was attached to the overhead lift. The lift was used to roll the patient from supine on the first mat and place him in prone onto the platform on the second mat. Several therapists were required to manage his limbs during the transfer and to ensure he rolled safely into the proper position with his airway floating (Figure 4).
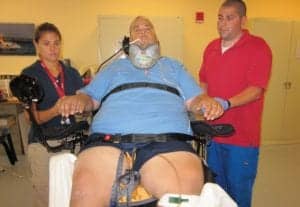
Figure 3
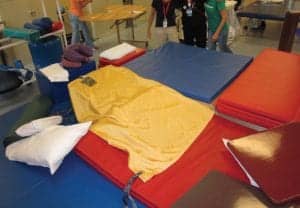
Figure 4
Managing spasticity and hypertonicity presented its own challenges as dynamic weight-bearing and facilitation were limited by the patient’s back and extremity pain and, again, by his size. This restricted the use of traditional treatments such as tilt table, standing frame, and sitting on the edge of the mat with his extremities in weight-bearing positions. Upright-sitting was accomplished by using an overhead lift to position the patient on a large, weight-accommodating therapy ball, which was positioned between two high-low mats to provide stability. Once he was positioned in sitting on the ball, the overhead lift and sling remained in place but on slack, serving as a safety net in addition to having three therapists present for his safety. In sitting, dynamic weight-bearing was achieved using a combination of tables, additional therapy balls, and other gym equipment. This also allowed the lower extremities to be placed in weight-bearing to evaluate for activation of stabilizing muscles such as the quadriceps, hamstrings, and gastroc-soleus complex when small perturbations were applied to the patient (Figure 5).

Figure 5

Figure 6
Managing bariatric patients with SCI presents many challenges for safe and effective rehabilitation. It requires innovative use of available equipment and staff to maximize function while minimizing patient discomfort and safety risks to patient and staff. Over the course of this patient’s rehabilitation he lost 130 pounds (Figure 6) and began to meet both weight and width limits of additional equipment. Early and innovative interventions accommodated his size and pain limitations, and helped prepare for the introduction of additional therapies and modalities that would advance him toward functional goals He has returned to his previous home and work and continues to make progress functionally through outpatient therapy services.
Carol Ardanowski, MSPT, has 4 years’ experience in physical therapy at the Shepherd Center, Atlanta, treating a range of patients with neurological injuries including ABI, SCI, MS, stroke, transverse myelitis, and Guillain Barre syndrome. Ardanowski currently works in the ICU at Shepherd Center.
Patti Pasch, OTR/L, is a master clinician with 31 years’ experience in occupational therapy. She has practiced at the Shepherd Center for the past 24 years. Her experience includes the ICU, inpatient SCI rehab, outpatient SCI rehab, inpatient and outpatient MS, and SCI outpatient clinic. Pasch currently works in the ICU at Shepherd Center. For more information contact





