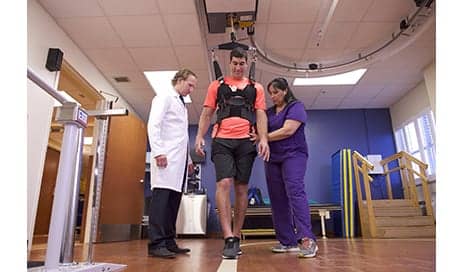
The benefits body weight support provided to gait training at the Memorial Rehabilitation Institute were observed immediately. Treatment required fewer therapists, and patients who were being treated with the technology had a decreased fear of falling.
The benefits body weight support provided to gait training at the Memorial Rehabilitation Institute were observed immediately. Treatment required fewer therapists, and patients who were being treated with the technology had a decreased fear of falling.
by Anna Maria Castaneda, PT, DPT, and Rania Margonis, PT, DPT
During the past 25 years, technology has had an undeniably profound impact on both inpatient and outpatient rehabilitation facilities. As a result, clinicians are constantly challenged to evaluate and incorporate new equipment into their knowledge base and interventions to optimize patient outcomes.1
At the Memorial Rehabilitation Institute, Hollywood, Fla, the staff has effectively utilized new technology to promote balance and gait for patients at a rapidly growing inpatient rehab facility.
The institute’s acute rehab unit at Memorial Regional Hospital South has grown considerably in the last 5 years. As a result of that growth the facility now features two therapy gyms, two community re-entry simulation rooms, and 79 private beds, with another floor currently being converted to house 18 new beds for an oncology specialty being developed.
The facility’s staff consists of 28 physical therapists, 29 occupational therapists, eight speech therapists, one recreation therapist, and one music therapist. Four therapists are NDT-certified. The facility, which is part of the Memorial Healthcare System in Hollywood, Fla, attracts a population of patients comprised of individuals who are recovering from orthopedic injuries, organ transplants, traumatic brain and spinal cord injuries, and stroke. The stroke population accounts for 40% of the facility’s patients.
DEVELOPING A CULTURE OF TECHNOLOGY
The numbers are important because while everyone embraces new equipment on an intellectual level, therapy staff was initially neither confident nor competent in using the new technology. It was critical that the facility first fostered a change in treatment culture before fully implementing the body weight support (BWS) system in 2013 and functional electrical stimulation (FES) 3 years later. With gait training, for example, staff had grown accustomed to traditional techniques that involved parallel bars and the deployment of three or four therapists to assist lower-functioning patients. Using BWS marked a significant change.
The technology was gradually introduced within the department. Structured classroom instruction was provided with opportunities to develop hands-on mastery of skills, practice with real patients, and receive professional guidance. This formalized process accelerated the staff’s development of competence and confidence, and the healthcare system invested heavily in this process.2 Training in both the aforementioned technologies was rolled out with select staff members being initially certified as “super users.” These users trained their peers and developed competency among staff members to assure that all could safely use the new technology.
An aquatics facility provides a versatile option for therapists to partially unload patients and treat conditions that affect gait and balance.
BODY WEIGHT SUPPORT TRAINING
With the prevailing evidence showing that combinations of different rehabilitation strategies are more effective than over-ground gait training alone,3 the therapy staff at Memorial was instructed to incorporate BWS training into patient treatments for all diagnoses. This included stroke, spinal cord and brain injuries, critical illness myopathy, and even amputation. The benefits BWS provided to gait training (over ground and/or treadmill) were observed immediately: treatment required fewer therapists, patients who were being treated with BWS had less fear of falling, and safety for the therapists and patients alike was increased.
Additionally, the opportunity to partially unload patients has allowed for increased walking speeds, task-specific training (such as curb and stair negotiation), and safe progression to a less restrictive device. The facility has also incorporated a variety of pre-gait and neuromuscular re-education activities—sit to stand practice, fall recovery, static and dynamic balance training, and the transition to developmental positions (quadruped, tall kneeling, half-kneeling). While the long-term efficacy of BWS training continues to require more research,4,5,6 the staff’s perspective is that patients in this facility have seen definite improvement in their overall gait safety and quality with the use of the system.
FUNCTIONAL ELECTRICAL STIMULATION TRAINING
Memorial acquired an FES unit for lower extremity foot drop in 2016, and the facility’s clinicians recognized a positive orthotic effect during gait and pre-gait training. This technology uses electrical stimulation to promote lower extremity clearance during very task-specific, functional activity for patients with upper motor neuron disorders (most commonly stroke and multiple sclerosis). FES assists patients with increasing gait speed, improving single-leg stance stability, decreasing fall risk, and progressing to safer overground ambulation.7,8 Similar to the BWS system, FES does more than solely gait training. The technology has been found to be effective during static and dynamic balance training, providing biofeedback for weight shifting and limits of stability, and strengthening transitional movements such as sit to stand.
With further expansion of Memorial’s inpatient rehab unit, department leaders are considering additional technologies for patients that create objective and measurable data that provide evidence of the impact of skilled therapy services. These technologies include a BWS treadmill training system that incorporates virtual reality with a gait mat. Among the gait mat technologies available are those designed as modular walkways of various dimensions embedded with pressure sensors that can collect data from static standing, straight walking assessments, and turning. Gait mats such as these can be used with standard tests such as Figure 8, 10-meter walk, sit to stand, basic TUG, as well as other maneuvers such as zig zag turn walks. These technologies, which are available as portable systems or for use in a facility office, are also capable of gathering data about pressure generated by assistive devices such as canes and walkers.
While traditional rehabilitation for treating conditions that affect gait and balance continue to produce satisfactory outcomes, there is good reason for therapists to embrace and adopt some of the latest technologies available in this area. By providing the opportunity for therapists to learn how to use these technologies, master their features, and become champions of those technologies to their colleagues, rehab facilities promote a culture of technology that improves the safety and productivity associated with the environment in which therapists and patients strive to reach their goals. RM
Anna Maria Castaneda, PT, DPT, is clinician of rehabilitative services at Memorial Regional Hospital South. She has been a physical therapist for 27 years, worked with both pediatric and adult patients, and has a focus on treating the adult neurologically involved patient.
Rania Margonis, PT, DPT, is supervisor of rehabilitative services at Memorial Regional Hospital South. She also serves as an adjunct faculty member for the neurological curriculum at Nova Southeastern University, where she received her Doctor of Physical Therapy degree in 2009. Rania is also a graduate of the University of Pennsylvania. For more information, contact [email protected].
REFERENCES
1. Rothstein JM. Preparing to use technology. Physical Therapy. 1990;70(2):63-64.
2. Ulrich B, Krozek C, Early S, Ashlock CH, Africa LM, Carman ML. Improving retention, confidence, and competence of new graduate nurses: Results from a 10-year longitudinal database. Nursing Economics. 2010;28(6):363.
3. Belda-Lois JM, Mena-del Horno S, Bermejo-Bosch I, et al. Rehabilitation of gait after stroke: a review towards a top-down approach. J Neuroeng Rehabil. 2011; 8(1):1.
4. Swinnen E, Beckwée D, Pinte D, Meeusen R, Baeyens JP, Kerckhofs E. Treadmill training in multiple sclerosis: can body weight support or robot assistance provide added value? A systematic review. Mult Scler Int. 2012.
5. Moseley AM, Stark A, Cameron ID, Pollock A. Treadmill training and body weight support for walking after stroke. The Cochrane Library. 2005.
6. Hesse S. Treadmill training with partial body weight support after stroke: a review. NeuroRehabilitation. 2008;23(1):55-65.
7. Kottink AI, Oostendorp LJ, Buurke JH, Nene AV, Hermens HJ, IJzerman MJ. The orthotic effect of functional electrical stimulation on the improvement of walking in stroke patients with a dropped foot: a systematic review. Artificial Organs. 2004;28(6):577-586.
8. Fritz S, Lusardi M. White paper: “walking speed: the sixth vital sign”. J Geriatr Phys Ther. 2009;32(2):46-49.