 |
| Young Ethan enjoys the playground. |
What is mobility? Is there a difference between functional mobility and physical activity or exercise? What is different when prescribing mobility devices for pediatric clients versus adults? How do we, as providers, account for these differences? Or do we? What about the current funding environment and changes in our industry? Do these changes affect what we, as clinicians, are recommending for our patients’ mobility needs?
EXERCISE VERSUS MOBILITY
People, including children, need to be able to get around effortlessly and in a reasonable amount of time throughout their day, accessing the same environments as all other children without becoming fatigued. Sometimes moving a manual wheelchair or walking requires too much energy, making it nonfunctional. For example, if a child requires excessive energy just to get to the classroom, that child may not be able to pay attention and learn effectively after getting there. Powered mobility is an ideal option to provide efficient functional mobility when walking or using a manual wheelchair proves to be nonfunctional.
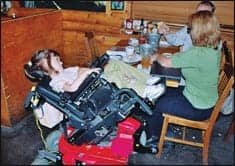
For example, Emily is a 7-year-old girl with spina bifida. She was using an ultra-lightweight manual wheelchair, which, on the surface, appeared to be meeting her functional needs. However, her mother reports that Emily would come home from school, eat dinner, and then be so tired she went directly to bed. This is not typical behavior for a 7-year-old. Emily was so tired from pushing her manual chair (getting help from her friends to get around the school and limiting her activities on the playground) that she couldn’t “be a kid” when she got home. Emily’s therapy team decided she needed a power wheelchair to be independent and efficient with her mobility needs. After receiving her power chair, Emily is now able to be a kid again!
 |
| Seven-year-old Emily’s power wheelchair increases her independence and mobility in a variety of environments. |
When considering power mobility, parents often wonder, “Isn’t my child going to lose strength due to using a power wheelchair? Won’t a power wheelchair keep my child from walking?” Exercising is important for everyone; however, mobility and exercise are not the same. Think of your routine—you drive to the gym to get on the treadmill. You drive to the park to ride your bicycle. We even drive around wasting time just to find the nearest parking spot at the mall. There are many ways for children with disabilities to develop strength and endurance. Studies have found that children typically do not lose gross motor function due to power wheelchair utilization. On the contrary, it has been shown that after receiving independence through power mobility, gross motor skills actually improve as children are more motivated to move and do things for themselves!
WHAT IS DIFFERENT ABOUT PEDIATRICS?
Anyone who is involved with pediatric health care will attest to the fact that kids are not simply tiny adults. Children have distinct needs and deserve to have equipment that specifically meets those needs. Many times pediatric mobility equipment is simply adult products with smaller seating systems. Whether you are a part of the medical therapy model, the school therapy model, a teacher, or a parent, or just enjoy the company of young people, we want kids to be kids! Allowing a differently abled child to have the opportunity to interact at the same level and do the same types of activities as their peers is essential for their overall development, improving their self-image and confidence, and helping them feel less isolated or different. Whether a child is in need of crutches, a manual wheelchair, or a powered wheelchair, we need to be aware of that child’s specific needs when prescribing their mobility equipment and seat functions.
 |
How do we decide what type of equipment is the most appropriate to meet the needs of our pediatric clients? The Medicare algorithm is a good framework to help decide what general class of equipment is most indicated. However, with children, we need to consider not only their home environment, but all areas of their life: the classroom, the playground, the backyard, the ball field, the garden, and wherever else that child needs to be.
We must remember that a child’s job is to play and explore their world in order to develop skills that children without mobility restrictions do frequently every day. We shouldn’t restrict a child to the home environment when their peers are out and about seeking experiences in the world! Our goal as a therapy team should be to integrate the child as much as possible into their world, allowing them to function with their peers independently. We also need to keep them safe in the process … from accelerating their disease progression, reducing the risk of developing secondary complications such as contractures, scoliosis, etc, but only to the extent that they remain functional. It is a fine balance between position and function, and the challenge is to find the most appropriate device that can effectively manage both. As I heard a representative from a Belleville, Ill-based seating and positioning company say, “There comes a point in seating where skin wins.” Likewise, there’s also a point when function prevails over positioning. Let’s face it—if someone is not comfortable or functional in their mobility device, they won’t use it. Or even worse, they’ll use it inappropriately, which places them at risk for further injury or worsening secondary complications.
 |
| Six-year-old Kendle uses the seat tilt (above) and elevation (below) functions of her power chair to adjust her posture support, comfort, and access levels. |
CAREGIVER ASSISTANCE VERSUS INDEPENDENCE
We hear it all the time from funding sources, “Children have 24-hour caregiver assistance.” Sometimes funding sources see this is a justification to deny power seat functions for young children or possibly even deny power mobility or ultra-lightweight manual wheelchairs altogether. Studies have shown that without independent mobility, people develop dependency on others—”learned helplessness.” Mobility opens doors for opportunity as well as responsibility—both prerequisites for independence, confidence, and a positive self-image and attitude.
Let’s specifically discuss power seat functions for children. Often, we might be tempted to save some money by providing manual seat functions on a power wheelchair base, but at what cost to the patient? Sometimes manual seat functions are appropriate, but this is typically the exception rather than the rule. Just like learned helplessness develops with dependent mobility, the same applies to children who cannot effectively reposition themselves, or reach objects without the assistance of someone else. If children have the ability to operate their own seat functions, they should be given that opportunity for independence. By giving children the ability to reposition themselves independently, they no longer need to ask for help (learning helplessness) but are empowered to fidget in their chair—just like their peers do. Whether it’s for postural stability, for pressure relief, or simply for sensory stimulation, kids should have the right to move.
 |
For example, Kendle is a 6-year-old with congenital muscular dystrophy. She has normal sensation and is extremely weak (especially proximally). When recently talking to Kendle about her power seat functions (seat elevator and tilt), she had much to say. We had dinner together, and throughout the meal, she used both seat functions multiple times independently! I asked Kendle why she needs her power tilt feature. She responded, “When my butt gets sore, I tilt. Or, when I am going down the ramp at our house, I tilt so that my head leans back.” Even a 6-year-old can figure out that when gravity assists her posture, she doesn’t have to work as hard and therefore has more energy to participate in her daily activities. Kendle loves to draw and hopes to one day become a professional artist. There is a problem . . . her shoulder weakness requires her upper extremities to be supported in order to effectively complete her drawings. Thankfully, that’s no longer a problem for Kendle; she uses her power seat elevator to access various table heights to give her arms proper support and still allow her to be integrated in society. Actually, during dinner, she needed to elevate her seat to access the table so she could feed herself (after completing her drawing, of course—which will go on my desk as a reminder of her beautiful spirit!). Thanks, Kendle, for teaching me about how important independence is and how effective power seat functions can be, even in young children.
WHAT ABOUT FUNDING AND THE CHANGES IN OUR INDUSTRY?
Unfortunately, federal regulations such as HR 6331 and the competitive bidding delay have made it extremely difficult for us to provide equipment that our patients need. Additionally, insurance programs are making medically necessary items “noncovered” for many policies. This is forcing clinicians to complete many time-consuming appeals, and may even require families to pay out of pocket or use fundraisers to get equipment that their child needs and deserves. As an industry, our initial response is to decrease the quality of products so we can reduce the overall price. Or even worse, we’re providing items as standard when they can and should be justified for reimbursement, proving the value of these features. If we, as an industry, continue to lower the bar for the quality of equipment, what will we end up with? A bunch of mediocre products that work okay for some things, but limit our patients from doing things they would like to or need to do?
 |
| Amy Meyer |
Thankfully, in pediatrics, we are not directly affected by HR 6331, but it is something to consider as Medicare policies tend to trickle down to other programs. The good news: children are protected under Medicaid EPSDT programs. Medical care and services must be provided in a manner consistent with the best interests of the Medicaid recipient, 42 USC § 1396a(a)(19). While a state has some latitude in designing its Medicaid program, it may not unreasonably or arbitrarily reduce the scope of coverage for a requested service so as to discriminate against a specific condition or deny necessary medical coverage. See Beal, 432 US at 444; Blue v Bonta, 99 Cal App 4th 980, 990 (Cal App 1 Dist, June 26, 2002); 42 CFR § 440.230(c). Thus, states may only place appropriate limits on a covered category of service based on criteria such as medical necessity or utilization control. 42 CFR § 440.230(d). Even when such limits are imposed, the services provided must be sufficient in amount, duration, and scope reasonably to achieve their purpose, 42 CFR § 440.230(b).
Furthermore, we need to keep pushing the envelope and advocating for our patients and fighting funding sources to approve the mobility equipment that our patients need and deserve to be fully independent. We will get through this crisis and there is light at the end of the tunnel. But we need to make sure our voice is heard, and we continue to raise the bar for quality products in our industry!
Amy Meyer, PT, ATP, is the pediatric and standing specialist for Permobil Inc, Lebanon, Tenn. For additional information, contact .





