 |
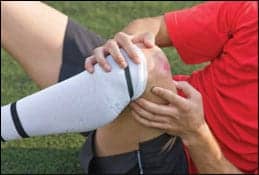
| Continuous passive motion, or CPM, is often used to help individuals regain motion following ACL surgery, resulting from sports-related and other injuries. |
Weekend warriors trudge onward and outward to make their mark, with highlight reels of (insert your favorite sport here) spooling through their brains. On the continuous cerebral loop: World Series standouts, Kerri Walsh/Misty May-Treanor’s net battle for Olympic gold, Rafael Nadal’s midyear tennis trifecta, and Tiger snagging the US Open after a 19-hole playoff.
Like their pro brethren, amateurs nick the cartilage—through trauma or arthritis—and continuous passive motion therapy (CPM) helps restore it after surgeries, such as microfracture or articular cartilage paste grafting, when needed. CPM is decidedly low (or no) tech, and sportswise, it fosters the best outcome when used to help cells remodel.
“It is [probably more] for people who have this one surgery, which has articular cartilage work,” says Laura Keller, MPT, who heads the rehabilitation department at the sports orthopedic, San Francisco-based Stone Clinic. “Studies have shown that, when you use it for up to 6 hours a day, the articular cartilage heals better because of that passive motion, as if it knows what to do and what it’s supposed to respond to.”
CPM devices debuted in the 1970s and have changed little since then. Devised for joints of the upper and lower extremities, they are most often prescribed for postsurgery use for knee and shoulder injuries. The machines mimic the body’s movements, bending and flexing the joints at a specified setting for several hours, with no active participation from the patient. The process usually starts the day surgery is performed or on the following day, and may continue for up to a month. The device has been shown to help relieve stiffness, swelling, and pain, and it lessens fluid retention, deep venous thrombosis, and the potential for scar tissue formation. Its merits generally help shorten the overall rehab period and speed recovery.
After joint surgery, range of motion is a key function for patients to regain because the joints grow stiff if they are immobilized. “The real point is to prevent cartilage breakdown, essentially from having a joint in a very stiff or fixed position for prolonged periods of time,” says Carlos Guanche, MD, of the Southern California Orthopedic Institute (SCOI), Van Nuys, Calif, a full-service orthopedic center. Some 80% to 90% of patients who seek Guanche’s expertise have some difficulty restoring their range of motion.
IN THE JOINT
Anterior cruciate ligament (ACL) reconstructions and rotator cuff repair surgeries are typically outpatient, but replacement-type operations are inpatient. In general, outpatient surgery is more probably arthroscopic or less invasive surgery, so in general I would say if they’re using CPM from an outpatient perspective, it would probably not be used for more than a couple of weeks or 3 weeks, as opposed to 6 weeks in a replacement, he says.
Cartilage resurfacing offers another use for CPM. “We go in there and take cartilage from either another area of the knee or another area of the body or actually grow the cartilage in test tubes and then insert it into the knee joint or some other joint,” Guanche says.
Occupational therapists and physical therapists are familiar with use following ACL surgery. Keller says she uses it for younger, return-to-field athletes if they have arthrofibrosis, which is like an autoimmune dysfunction. Arthrofibrosis may affect knee joints that have been injured or operated on, and it begins when the trauma causes the knee to form internal scar tissue, followed by shrinkage and tightening of the knee-joint capsule. Tendons outside of the joint may also become stiff, and the internal and external tightness may eventually inhibit the motion between the femur and tibia. Some patients may no longer be able to fully extend or bend the knee. “It’s almost like treating a frozen knee, as if the scar tissue is laying down really thick overnight,” she says. “We’ll put the machine on people for that. It ends up creating a lot of good stimulus to the knee that helps decrease that freezing response of the knee.”
Non-return-to-sports patients who have had total knee replacement use CPM as a matter of course. But Keller says some gain its full benefit during the hospital stay and no longer need it after they return home. Guanche notes that some patients say they experience less swelling and less dysfunction in the leg and, probably indirectly, less pain. Keller says CPM can be tapped for its potential analgesic-type effect, helping to calm knee pain for a patient with out-of-control pain and swelling that does not react to medication.
However, while its value is acknowledged, its scope is limited. Guanche says he does not believe CPM impacts the overall healing rate. And Keller says that for ACLs and some of the major return-to-sports type of injuries, it is pretty much accepted that CPM is ineffective in any of the future outcomes. “So, we don’t really use it unless somebody is having a problem with arthrofibrosis after surgery, which we find very, very rarely, because the way we approach postoperative patients is direct physical therapy with hands-on treatment to immediately decrease the swelling and edema and control the pain. If all of that doesn’t cascade, then we usually don’t see the arthrofibrosis.”
SIMPLE MAGIC
A traumatic event is usually the culprit when a young person’s knee cartilage is damaged. The articular cartilage—not the entire joint—will require repair if an area of the femur or tibia reveals a divot or bare spot. This differs from normal osteoarthritis, where the whole joint surface is worn down. Surgeons perform grafts to plug the void, which covers and merge with the healthy cartilage of the knee. Keller says the cells heal, but don’t know what to do. “Because there’s a certain amount of form equals function,” she says. The CPM, with its slight bending, retrains the cells. “They found at around that 6-hour window the cells actually began to organize and figure out how they need to lay down, much better than if you didn’t use the machine.”
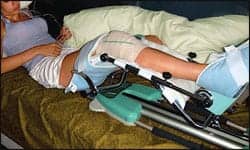 |
| CPM can help restore movement, as well as relieve swelling, stiffness, and pain. It is recommended that treatment begin immediately following surgery. |
The main CPM use for the upper extremities is for the shoulder—if a patient has a frozen shoulder (adhesive capsulitis)—and second, it would be used at the elbow for articular work, or if there was a case of arthrofibrosis. However, upper-extremity use of CPM is a fraction of what is used for the lower extremities, Keller says. The same considerations are used for the shoulder and elbow as the knee—namely, surgery-specific, pain and swelling control, and avoiding/fighting arthrofibrosis.
Guanche says CPM helps mold the new cartilage in a more congruent way, so it looks more normal. “The cartilage needs motion for it to have the proper physiology and the proper nutrients around it, so what CPM tends to do, theoretically, is that it stimulates a more normal environment for cartilage to at least be healthy, or regenerate, or heal, depending on the situation,” he says.
Most patients use the device for a month or 6 weeks. If patients use it during the prescribed time for fewer than 6 hours daily, the results are not as good, but 8 hours of daily use showed no better results than 6 hours, she says. Keller says most people divide their CPM time in 2-hour chunks, before and after work and in the evening. Some lucky users sleep during use, but most people cannot. “The most common complaint we have is people put it on and it crawls down the bed,” Keller says with a chuckle. “So the people who are the best with it have a bed that’s against the wall.”
Stone Clinic provides a hinged neoprene brace to support and shield the knee, and deep-water/stationary bike workouts are begun immediately for the noninvolved side, and recommended for both legs after 2 weeks. Non-weightbearing strengthening exercises for the involved side are introduced, and continued strengthening for the opposite side is performed. Patients may gradually return to full sports after 3 months, but impact exercises are discouraged, since the grafts’ maturity continues to improve during the initial 12 months.
FROM POINT A TO POINT B
“It’s a sled that you put your leg in and it goes back and forth. That’s it,” Keller says. “Out of every single piece of equipment, it’s probably one of the least exciting pieces of equipment in rehab that you could possibly pick.” The device executes a single-plane motion, with the patient’s heel in a little hammock and the thigh strapped in. The device moves the heel back and forth, sliding it. Some models feature a readout for PTs. “I’ve never seen an accurate reading for range of motion, for what the range of motion actually is,” Keller says. “And you could go variable speeds, but still it’s all extremely slow.”
Some sleeker designs have been introduced, but besides synching it up and monitoring if a patient is using the device, few upgrades have been made in CPM’s 30-year history. A company once introduced an inflatable machine. “It would blow air up, which would create a triangle under the knee to bend the knee, and then it would deflate,” Keller says. “But I think that was short-lived. We tried it. It was totally clumsy and the foot stuck, and the air didn’t blow up equally and it was just really silly.”
CPM plays a supporting therapeutic role—Keller emphasizes it is never the marquee player—and it is not used for gaining range of motion or in place of any manual treatment at the Stone Clinic. “It’s definitely a supplement, and it is necessary for certain procedures and protocols to have the best outcome; however, it’s never a substitute.” The clinic’s protocol is to use the device for a solid, black-andwhite month. The microfracture and the articular cartilage base graph are used regularly.
When asked if a product lies just beyond the horizon to replace CPM, Guanche says no. “Probably the thinking is pushing more toward the physical therapy aspects, to have patients actually do it for themselves rather than having a device—only because of the time constraints,” he says.
INSURANCE REIMBURSEMENT
Insurance coverage policies may vary, depending on the carrier. For example, Aetna covers the use of CPM machines as medically necessary in a number of cases, such as improving the range of motion for patients who are unable to undergo physical therapy and as an adjunct to ongoing physical therapy, says Wendy Morphew, the company’s spokeswoman. Aetna’s clinical policy bulletin, which details coverage for CPM machines and the science underlying the policy, is found on the Web site www.aetna.com. Search for clinical policy bulletin No 0010.
Aetna considers CPM machines medically necessary durable medical equipment to improve range of motion in any of the following circumstances: during the postop rehabilitation period for those who have received a total knee arthroplasty or replacement, as an adjunct to ongoing physical therapy; for those who have had an anterior cruciate ligament repair, until they are participating in an active physical therapy program; for individuals who are undergoing surgical release of arthrofibrosis/adhesive capsulitis or manipulation under anesthesia of any joint (knee, shoulder, and elbow the commonest) until they are participating in an active physical therapy program; or to promote cartilage growth and enhance cartilage healing during the non-weight-bearing period following any of the following procedures, until the individual begins the weight-bearing phase of recovery.
The covered procedures include surgery for intra-articular cartilage fractures, chondroplasties of focal cartilage defects, surgical treatment of osteochondritis dissecans, after abrasion arthroplasty or microfracture procedure, treatment of an intra-articular fracture of the knee (such as tibial plateau fracture repair), autologous chondrocyte transplantation, or for those who have undergone certain surgeries (such as procedures for reflex sympathetic dystrophy, Dupuytren’s contracture, and extensive tendon fibrosis) and may not be able to benefit optimally from active physical therapy.
Use of the device must begin within 2 days after surgery to meet medical necessity guidelines when CPM is used for surgical rehabilitation, Morphew says. Though the usual duration is 7 to 10 days, up to 3 weeks of CPM therapy may be considered medically necessary on a case-by-case basis, and the company says use of the CPM machine beyond 21 days after surgery is not supported by the medical literature. Insufficient evidence exists to justify use of the devices for longer periods or for other applications, Aetna says.
Aetna considers CPM machines experimental and investigational for the treatment of low back pain or trauma, for rehabilitation following back surgery, and for rehabilitation of distal radial fractures.
Judy O’Rourke is associate editor of Rehab Management. For more information, contact .





