 |
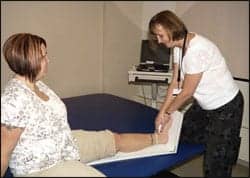
| A therapist (above, right) measures a lymphedema patient’s leg to track limb volume and percent of reduction. |
To health care providers, quality improvement, or QI, is often viewed as a necessary burden to ensure regulatory compliance. Nevertheless, at Mary Free Bed Rehabilitation Hospital, Grand Rapids, Mich, the staff has developed a QI program that has made an extraordinary difference in treatment outcomes for lymphedema patients, as well as employee performance and satisfaction.
DEVELOPING BENCHMARKS
Mary Free Bed, an 80-bed, not-for-profit, acute rehabilitation center, offers a lymphedema program that has been around since 1996, and is based on the Vodder’s manual lymphatic drainage and complete decongestive physiotherapy (CDPT) techniques developed in the 1930s by Danish husband-and-wife therapists Emil and Estrid Vodder. CDPT is a combination of manual lymph drainage, remedial exercise therapy, compression bandaging or compression garments in the maintenance phase, and therapeutic skin care. (It may also include breathing and aquatic exercises as well as dietary measures.)
A DATABASE OF EXPERIENCE
QI provides a timely evaluation of outcomes in the face of changing practice demands. One of the most difficult changes professionals must deal with is the constantly evolving rules put forth by Medicare, Medicaid, and other managed care plans. The staff at Mary Free Bed implements the protocols of QI to “keep score” of lymphedema treatment successes and to determine how to be more efficient. In a nutshell, standards of care are monitored without changing philosophy or straying from what evidenced practices have proven works.
Thanks to Mary Free Bed’s QI program, the staff have been able to build a database of clinical program outcomes that can be used to measure performance improvements. Every patient is compared to the benchmarks so their treatment programs can be adjusted as necessary. (After discharging patients, we do not ever want to find ourselves saying that we should have done something different to help them reach their potential.)
Mary Free Bed’s QI program collects multiple types of data, both nominal variables (eg, gender, diagnosis, and comorbidities) and ordinal variables (eg, stage of lymphedema, function scale, pain scale, and severity of skin integrity problems). An ordinal scale was also developed for end of treatment and 6 months post adherence on each portion of the home management routine: bandaging, alternate nighttime compression, self-massage, exercise, and skin care. In addition, patient satisfaction data is collected, and interval measurements are taken to track limb volume and percent of reduction. When wounds are present, ratio data is obtained for changes in wound size.
NO PATIENT LEFT BEHIND
One of the biggest obstacles to Mary Free Bed’s QI program occurred when Medicare (and the majority of other managed care programs in our area) changed the regulation governing lymphedema treatment, stipulating that therapy could be applied only by PTs or PTAs. At the time, daily treatment was being carried out by certified MLD (manual lymph drainage) specialists with a background in massage therapy—specialists who consistently exceeded the facility’s treatment benchmarks.
A big challenge was figuring out how to maintain excellent outcomes given the restrictions on using only PTs or PTAs to carry out treatment, which was previously addressed by massage therapists. The facility’s PTs and PTAs were somewhat reticent to jump into lymphedema treatment. They had heretofore applied a variety of treatment techniques on a variety of diagnoses, but had little familiarity with lymphedema. Once insurance regulations mandated the use of PTs and PTAs for lymphedema treatment, the facility was unable to keep massage therapists on staff. Meanwhile, many of its PTs expressed concerns about becoming MLD specialists. As a compromise, PT staff responsibilities were structured so that lymphedema treatment was just part of the caseload—not the sole task—as was the case with the MLD specialists. Thanks to Mary Free Bed’s QI program, this compromise did not adversely affect treatment outcomes.
Our QI program provides both the expectation for outcomes, as well as help when those expectations are not being met. New MLD practitioners who had never performed treatment on anyone other than students in their certification class were able to judge the progress of their patients against 12 years of experience established by prior MLD specialists. In the meantime, benchmarks based on research and internal analysis of comorbidities from past experience have been set. When a patient is not meeting those benchmarks, the staff can troubleshoot the problem and determine how to correct it, perhaps by introducing compression alternatives or new strategies to improve adherence.
 |
| Above, physical therapists demonstrate a program that converts circumferential measurements into volume and calculates changes. |
EVALUATING ALTERNATIVE TREATMENT OPTIONS
We also use our QI program to evaluate new products and treatment techniques, including multichamber compression pumps, alternatives in nighttime compression therapy, and the taping of limbs to address lymph flow deficits. By following patients for 6 months, it can be determined which products work well and experiences about the pros and cons of products outside the traditional CDPT regimen can be shared.
IMPACT ON STAFF SATISFACTION
What’s more, Mary Free Bed’s staff satisfaction has been greatly enhanced by the QI approach. Every quality improvement report asks staff to analyze their treatment strategies with an eye toward identifying what they might do differently next time around. As a result, the initial evaluation form has been modified to include checklists of comorbidities, precautions, and contraindications to reduce the risk of inappropriate treatment. The way the staff assess changes in function and pain experienced by patients has also been revised. This had been a source of frustration to therapists and administrators, who often had to appeal denials because this information was not clear to third-party payors. In addition, the facility developed adherence training programs to help therapists who were frustrated by patients who were not showing up for treatment or following through on home programs.
The bottom line? All team members now know they have a say in how the lymphedema program is put together and an invitation to suggest improvements. There has been no staff turnover in the lymphedema program since the PT staffing model was implemented. Mary Free Bed therapists generally report a great deal of satisfaction with their work.
RESEARCH AND QI
In a look toward the future, Mary Free Bed intends to use its QI database as a tool for research. In fact, the staff recently submitted a suggestion to the National Lymphedema Network that massage be avoided over fluid-filled sacs such as seromas. Through measurements obtained during the QI process, the staff have noted that edema does not improve in those areas. Consequently, we are suggesting that massaging them may be counterproductive.
BROADER BENEFITS
Other elements within our organization also use the QI database. Mary Free Bed’s administrative team uses the database to produce dashboard presentations and make more informed decisions. Meanwhile, the marketing department uses it to publicize the success of our program to internal and external customers.
TECHNOLOGY
LYMPHEDEMA QI PROCESS |
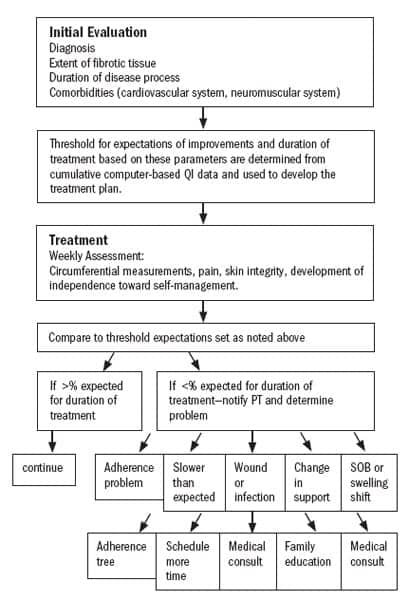 |
Aside from the computerized database that constitutes the heart of the QI program, the therapists also rely on software that converts circumferential measurements into volume and calculates volume changes between measurements. For bilateral patients, the volume measurement compares the limb on successive assessments. Meanwhile, the unilateral volume measurement compares the affected limb to the unaffected limb.
STAYING AHEAD OF THE COMPETITION
Competitors without similar QI programs have had a difficult time keeping pace in the local lymphedema market. One of the facility’s primary competitors could not retain full-time PTs or PTAs in its lymphedema program and has begun offering CDPT just one to three times per week. In fact, Mary Free Bed has experienced an increase in referrals from its competitors, especially for complex cases involving severe lymphedema or multiple comorbidities.
At the very least, a reliable QI program provides therapists and patients with the peace of mind that comes from knowing a mechanism is available to help determine when a treatment outcome is not what it should be.
In an interview for a physical therapy magazine, James Glinn, Jr, PT, OCS, STC, president of San Luis Sports Therapy & Orthopedic Rehabilitation, San Luis Obispo, Calif, says, “If you ask 100 physical therapists if they provide quality care in their practice, they are all going to give a resounding ‘yes.’ But ask them about their processes and systems and the way they measure quality, and the room will become very quiet.”1
This author is proud to say that if the same question were asked of the Mary Free Bed lymphedema team, it would take quite a while for the room to become quiet.
Jennifer McWain, MHS, PT, is a certified manual lymph drainage specialist and physical therapist at Mary Free Bed Rehabilitation Hospital, Grand Rapids, Mich. For more information, contact .
REFERENCE
- Muir J. The quest for quality. PT Magazine. 2004;12:7.




