 |
The use of continuous passive motion (CPM) to treat patients is nothing new to the physical rehabilitation field. But its staying strength as a front-line therapy for certain injuries and postsurgical applications says much about its usefulness during the rehabilitation process.
The philosophy behind the therapy is the same now as it was when Robert Salter, MD, first introduced the use of CPM in the 1970s: Passive motion without resistance on the part of the patient improves healing. Although passive, it is in fact the continuous motion—not immobility, as was once thought by health care professionals—that is believed to help speed up the rehabilitation process after injuries and surgeries.
The use of CPM devices is, of course, not intended to replace the traditional hands-on treatments that therapists provide to their patients, but rather to act as a supplemental treatment in the initial stages of the overall rehabilitation plan.
While some studies have shown that, at 1 year out, range of motion and function are the same among patients who have received CPM therapy and those who have not, many PTs who use the treatment say they are swayed by the positive results they have observed firsthand with their patients.
REPLICATING THE BODY’S MOVEMENTS
CPM machines replicate the movements of the body parts, bending and flexing joints at a specific setting over the course of several hours, without patients actively using their muscles. CPM helps alleviate stiffness, swelling, and/or pain in the affected area(s); decreases the potential for developing scar tissue, fluid accumulation, and deep venous thromboses; and increases range of motion—all of which factor into an overall shorter rehabilitation and faster recovery time.
In turn, those benefits increase patients’ adherence with active therapeutic protocols following injury or surgery.
CPM is generally initiated the day of or the day after a surgery to a predetermined setting, which can be adjusted. “Postsurgical procedures, you do want early movement. It keeps the tendons lubricated. It keeps fluid from accumulating in the joints. It lets the body know it’s going to move in a normal direction. It gives good feedback to the brain that this is normal motion,” says Cynthia Bauer, PT, DPT, OCS, director of musculoskeletal outpatient services for Good Shepherd Rehabilitation Network, Allentown, Pa.
“Years ago, after surgeries, they put people in casts and they’d get so tight. We’d be moving from such tight joints, you’d never restore that motion. Today, early motion, early weight bearing, and early function are usually key,” Bauer says.
CPM machines can be used for hours per day, either continually or broken up over periods of time.
While the philosophy behind CPM has not changed over the years, today’s devices have changed in design and availability.
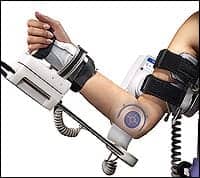
Early versions of CPM devices were bulky and required manual adjustment. Today’s CPM devices are sleeker than their predecessors, with microprocessors controlling the range of motion and force applied, as well as detecting patients’ resistance. The machines provide a more controlled, precise approach to gradually increasing a patient’s range of motion than what human touch can provide.
Among the CPM devices now available are those for the knee, ankle, shoulder, elbow, wrist, hand, hips, and temporomandibular joints. Bauer mainly uses CPM for patients who have undergone total joint replacement of the knee. “For a patient who might have too much discomfort or who is incapable of moving their leg back and forth to keep their knee flexibility, they’re put in a passive motion machine that moves the knee for them,” Bauer says.
At Good Shepherd, a particular CPM device also is occasionally used that provides passive motion and holds a stretch in the direction needed. “What’s nice about those machines,” Bauer says, “is it moves [patients] through a motion and then holds the maximum stretch for a certain period of time—so many seconds—and then releases it and holds it in the other direction [for] so many seconds. The therapist can set the parameters.
“It’s sort of a cross between a prolonged low-load stretch and a quicker stretch. It’s a combination because generally people will do better with a low-load prolonged stretch—such as a brace set in a flexion position over a period of hours—but in the clinic, we can set it for seconds,” she notes.
PATIENT ADHERENCE
The benefits to patients who use CPM can extend beyond physical aspects to financial ones as well. The cost and length of their overall physical rehabilitation is often less when CPM is used. “Usually when [patients] go home from a rehab hospital, they don’t need CPM in the home because by then they’re already moving their leg pretty functionally and then they just need to continue with therapy active motion,” Bauer says.
In some cases, it may even reduce or eliminate the need for surgical intervention.
CPM machines also benefit the rehab therapists who often face the challenge of treating more and more patients in a shorter amount of time. By setting the CPM device to a patient’s individual needs, a therapist is freed to focus attention on other patients who may require more direct treatment from the therapist. Even without additional patients to treat, it would be impossible for a therapist to continuously spend the time performing the movements manually the way a CPM device can for extended periods of time.
As with most therapies, the use of CPM does pose some challenges and limitations.
“It’s just like anything, in my opinion; there are people for whom it is appropriate, and people for whom it isn’t,” Bauer says. “People who are moving their knee freely soon after surgery and are not in excruciating pain [may not need it], but there are people who are in a lot of pain, and those people really benefit from having the knee moved by CPM after surgery. They’re incapable of doing it themselves, or it adds to the recovery.”
Some joints, such as the ball-and-socket joint of the shoulder, are more difficult to set up in passive range devices and get aligned correctly. Hinge joints, such as the knees, are easier.
CPM machines have to be used for a long period of time to be effective, which can affect patient adherence. And because of that extended use, it can also be a challenge to maintain the devices in good condition.
CPM devices also do not come in a one-size-fits-all model, so they must be adjusted to each patient’s needs.
Although the movement is passive, pain is still an issue with patients. It is important to note, however, that the pain may stem from the fact that patients are treated with CPM almost immediately after surgery when they are already often in a great deal of pain—and not necessarily from the motion itself. There also may be a psychological factor at play: Patients may be afraid to move the body part involved for fear of increasing their pain or causing further injury.
As with the use of any equipment, there is always the potential for misuse or abuse. Patients should be advised not to assist nor resist the movements, but rather to let the machine do the work for them. If patients are taught how to adjust the CPM device, they may adjust it too aggressively. Therapists should watch for such problems as skin rubbing or redness, inappropriate fitting, and swelling.
When counseled properly, Bauer says patients are more willing and able to comply with the treatment regimen. “With all avenues of therapy, I think knowledge is the key,” she says. “I like to educate the patient about their condition, about the precautions they have, the benefits of following what we’re recommending, and why they’re going to follow what we’re recommending … If [the patient] understands what the benefit is, you’ll have more adherence and buy-in of the plan.”
Danielle Cohen is a contributing writer for Rehab Management. For more information, contact .





