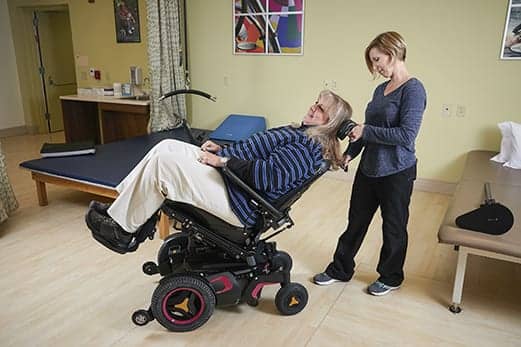
Tilt in space designs can play an important role where positioning is critical to assist with feeding, pressure relief, or holding the head upright. Good Shepherd Rehabilitation’s Maggie Johnsson, MPT, APT, demonstrates this feature, which may be helpful in reducing injury risk during transfer as well as improving the overall comfort the mobility user feels in a seated position.
by Maggie Johnsson, MPT, APT
With science and technology advancing at such a rapid rate, great progress is being made in all areas of medicine. Many individuals affected by disabilities are reaping the benefits of this technological growth and innovation, especially those who are dependent on manual or powered wheelchairs for mobility.
Advances in electronics and the ability to pair devices with powered mobility systems have made it possible to find equipment that can help even the most debilitated patients achieve independence with mobility in their homes and communities—independence that is achieved despite significant disabilities.
With almost 6,000 people diagnosed with amyotrophic lateral sclerosis (ALS) every year, and patients with diagnoses such as muscular dystrophy and spinal cord injury living longer, advances in power wheelchair technology have maximized their independence, mobility, and quality of life.
Mobility Technology
Developments in joystick design, alternative drive controls, and drive input mounting technology have given patients with minimal movement the ability to drive their wheelchairs independently well into their disease progression with proportional drive controls or switch driving.
For instance, alternative driving technology such as mini-proportional (or soft touch) joysticks, touch pads, fiber optic, or infrared switch driving can enable patients with progressive diagnoses to independently drive power wheelchairs after they have lost the strength and/or motor control to do so with a standard joystick. These new devices allow patients with only slight movement to control the wheelchair and operate its power positioning features from any part of their body.

Pressure mapping offers visual feedback on weight shifting and position changes. The data is useful to clinicians when prescribing cushions and seating products.
Additionally, these joysticks can be mounted to any part of the chair to access the patient’s remaining movement, whether it is at their hand, foot, or face. Because they can accommodate many types of weakness and immobility, soft touch joysticks offer independence to even the most debilitated patients. In the same way, tablet drive controls or switch driving can allow for power wheelchair driving with the use of only gross motor control.
For manual wheelchair users, power assist technologies can help maintain independence and reduce shoulder injuries. They are available as lightweight, quick-release wheels in conversion kits that can replace traditional manual wheels, or as a unit with an omni-drive wheel that attaches to the back of a wheelchair.
Sip & Puff technology has also expanded the control wheelchair users have over mobility devices by allowing the functions of inhaling and exhaling to operate switch-activated devices.
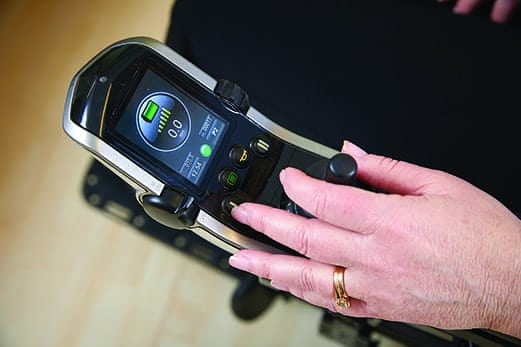
Advances in joystick technology and programming offer helpful functions such as the ability to set custom driving parameters.
Access to the Information Superhighway
It is difficult for most of us to imagine everyday life without smartphones, tablets, and computers, offering immediately accessible information and communication 24/7. In the past, wheelchair users without use of their upper extremities have been isolated from this digital access, making them reliant on caregivers or family members to perform tasks such as dial their phones, turn on their computers, or control their mice for Internet access.
In recent years, however, wheelchair manufacturers have put greater emphasis on the ability to access such technology when developing power mobility and electronic advances. Many manufacturers now offer advanced joysticks that are capable of connecting with smartphones, tablets, or laptop computers via Bluetooth, allowing the patient to use the wheelchair joystick to access and control these devices.
Once connected, the joystick can be used (in the same way they would when driving their chair) to easily and independently send an email, check text messages, or control their computer mouse to search the Internet from the comfort and safety of their wheelchair.
These new products and power wheelchair capabilities are greatly improving the independence and safety of power wheelchair users, and are opening up the world of many wheelchair-dependent people who are homebound and have limited access to their environments.
Seating Advances
In the same way that powered mobility systems are constantly and rapidly improving, advances in seating and positioning have made options for prescribing the appropriate pressure-relieving cushions more numerous than in years past. The industry leaders for skin protection continue to be air cushions, gel cushions, and multi-layer, pressure-relieving foam seating surfaces, but advancements have been made in the customization of all of these types of products to better suit clients’ individual needs. Seating solutions composed of modular, dynamic arrays are also an option for today’s mobility users, and have been developed to provide a high degree of adjustability in shape and size.
Options abound for pressure-relieving solutions for both seating systems and backrests, and pressure-relieving interfaces can be mounted anywhere on a mobility system where excess pressure occurs. Gel- or air-filled supplement pads can be placed on footplates for clients who cannot wear shoes and who are experiencing increased pressure under their feet or on an armrest for a patient with skin breakdown on their elbows. And seating components such as hip guides and lateral support pads can ensure that a patient is adequately supported in an upright and midline position to maximize their function and to prevent postural deformities from occurring.
While tilt in space designs may not necessarily help improve independence, they can play an important role where positioning is critical to assist with feeding, pressure relief, or holding the head upright. This feature, which is available for both manual and power wheelchairs, may be helpful in reducing injury risk during transfer as well as improving the overall comfort the mobility user feels while in the seated position.
Custom molded seating systems will always be a necessity in the field for those clients with fixed and significant postural deformities that cannot be accommodated for or supported by off-the-shelf seating products. The molding systems used to shape and build these seating systems have become more user and clinician friendly, and the process of fitting clients for these custom seating systems has become more streamlined with the use of 3D scanning to provide an intimate fit with maximal support and positioning.
Pressure Mapping
For cushion assessment and to increase the clinicians’ confidence when prescribing cushions and seating products, pressure-mapping systems offer instant feedback and evidence-based support to narrow down optimal seating solutions. A pressure map is a sensor mat connected to a computer that is placed on top of a wheelchair cushion, back, or any support surface. When a patient sits on the mat or leans against it, pressure-distribution data is sent to the computer, which displays color feedback of the area.
This data feedback allows clinicians to accurately and objectively decide which cushions offer the most effective pressure relief and translates to the fewest possible pressure points under a client’s bony prominences. This objective data takes the guesswork out of determining which type of cushion interface will best protect a patient’s skin integrity and can reduce the risk for costly skin breakdown and misprescribing of cushions.
Pressure mapping is also an extremely effective tool for direct patient education, offering immediate visual feedback to a patient as he or she is performing weight shifting and position changes. The computer graphics allow them to see what positions result in the lowest pressure readings and how different types of weight shifting affect their surface pressures. This feedback is especially valuable in patients with new onset spinal cord injuries with loss of sensation, as they can visually see and learn how important weight shifting and position changes are to prevent pressure injuries and skin breakdown.

Good Shepherd Rehabilitation’s Maggie Johnsson helps educate patients about new technology such as advanced joysticks that are capable of connecting with smartphones, tablets, or laptop computers via Bluetooth, allowing the patient to use the wheelchair joystick to access and control these devices.
Insurance Challenges
Funding cuts and insurance reimbursement limitations present challenges throughout the healthcare industry. Therapists and practitioners who specialize in seating and mobility have especially felt the impact of these cuts. Insurance reimbursement has become more diagnosis driven, making it difficult to prescribe higher-level seating and mobility systems for patients with significant disabilities but no neurological or qualifying diagnoses.
Building a positive working relationship between clinicians, equipment suppliers, and manufacturers is crucial to ensure that all avenues are explored when prescribing equipment. It is important for the clinician to do a thorough evaluation so that all of the patient’s limitations and needs are considered and so that the clinician and client have the same goals in mind when selecting mobility or seating equipment.
In the same way, having an equipment supplier who is well-versed in insurance reimbursement and limitations present at the evaluation helps ensure that equipment is not over or under prescribed. Requesting a complex power wheelchair or an ultra-lightweight manual wheelchair for a patient without a qualifying diagnosis only creates frustration for the supplier and ultimately the client who will likely be denied after going through the months-long process to obtain the proper equipment.
It is crucial for the therapist’s and physician’s documentation and supporting justification to be completed proficiently and in a timely manner to best ensure that the prescribed equipment meets all of the insurance provider’s determining factors for approval. Having the clinician and supplier present at the evaluation helps ensure that the therapist prescribes and has the client trial only qualifying equipment, increasing the odds for insurance approval and expediting the entire process. This team approach is essential in getting clients the exact equipment they need in the least amount of time.
The wheelchair mobility and adaptive seating industry is rapidly evolving and growing. Referring patients to a mobility and seating clinic that utilizes a team approach with informed and knowledgeable physical and/or occupational therapists as well as both local equipment suppliers and manufacturers ensures that patients receive cutting edge equipment that meets their needs and maximizes their safety and independence. RM
Maggie Johnsson, MPT, ATP, is a staff physical therapist in the Assistive Technology Department at Good Shepherd Rehabilitation Network in Allentown, Pa. She has been working in the seating and mobility field as a member of Good Shepherd’s Wheelchair Clinic department for more than 15 years. For more information, contact [email protected].




Maggie, Thank-you for your progressive approach to wheelchair assessments. Your mention of drive input mounting technology is of particular interest because it is so often overlooked during an assessment. You may want to consider dynamic pressure mapping of a prospective PWC user driving from an armrest-mounted joystick to see how dramatically a person’s body weight shifts while accessing the joystick. The longterm effect of armrest-mounted input devices is often the development of a muscular-skeletal condition and pain in the shoulder, neck and upper back. Midline positioning of drive controls with lower arm/wrist/and hand support(s)immediately improve posture, pressure distribution, and ease of use, while increasing the functionality of seating products. (See Moss Rehab clinical study at activecontrols.com)
Keep up the good work with embracing technology for your clients!