Why does a gal wearing twin tip skis want to rocket herself 16 feet skyward and propeller into a 900-degree turn, an instant before gravity invites her down to a cushion of frozen snow and dirt? Probably because she is an extreme athlete.
The participants of extreme sports may seem undistracted by the idea that sudden impact can implode the human foot-ankle complex, or shred a meniscus. It’s hard to know what they think as they slingshot across the winter landscape, tempting injury to their lower extremities in a way fate sometimes cannot resist.
Laura Keller, MPT, is director of rehabilitation at The Stone Clinic in San Francisco, and since 2006 has been seasonally drafted into service as a physical therapist by the Honda Ski Tour and the Jeep King of the Mountain Ski Tour. When fate interrupts an extreme skier’s meticulously planned landing, and deposits the person in a way that suggests articular armageddon, Keller takes a central role in the effort to help that athlete recover, retool, and prepare to compete another day.
“In more conventional sports like basketball, a player may suffer just an isolated anterior cruciate ligament injury or meniscal injury,” Keller explains, “but an extreme athlete is more likely to suffer the ‘terrible triad’ of the ACL, MCL, and medial meniscus. Some extreme athletes even experience a full knee dislocation, where all the ligaments of the entire knee are torn.”
Moving a knee out of the calamitous state conferred by the terrible triad does not happen overnight. The injury itself is intensely painful, and, for a high-impact event such as halfpipe skiing, recovery can last nearly a full year—beginning with surgery to reconstruct the ACL, and repair or trim the meniscus via menisectomy. The MCL, which rarely requires surgical reconstruction, typically is left to heal on its own.
Approximately 8 weeks after surgery, the graft begins to function as scaffolding, and soon afterward the body lays down foundation cells that eventually produce collagen fibers that mature into the new ACL.
Keller says that when healing progresses sufficiently, she transitions the athlete to a gait analysis, so that deficiencies that prevent the individual from returning to competition are pinpointed and worked on.
“Gait is the essence of your functional movement, and a practitioner who is fully versed in how to analyze gait can pick up a plethora of dysfunctions just by evaluating it,” Keller says.
“We know the effects of an antalgic or abnormal gait will eventually show up in all of an athlete’s functions, so every patient goes through gait analysis,” she adds.
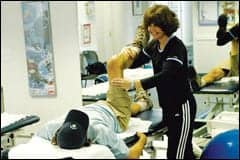 |
| Physical therapist Susanne DeCosterd, MPT, of The Stone Clinic, performs range of motion on a patient post ACL surgery. DeCosterd measures the range using a goniometer. |
THE WAITING IS THE HARDEST PART
An extreme athlete who thrives on speed may expect an injury rehabilitation to be a whistle-stop experience rather than an arduous and structured 16-week program. The expectation can strain the skills—and patience—of some PTs, and Keller cautions clinicians against the pressure that can be brought to prematurely return an athlete to play. She suggests the key to expedience lies among modern technologies and methods developed to safely and efficiently economize the athlete’s return to competition.
One technology Keller says can shorten the athlete’s path to rehab for gait and running is gravity unloading.
“Gravity unloading systems work by allowing the body to reintegrate normal motor patterns before it could under normal gravity—since the joint injury may not allow for fully loading, even when the range and muscle strength are ready for it,” Keller says.
Keller calls on sports taping postoperatively as an adjunct to improve lymph drainage and decrease edema. She feels Kinesio taping works best as a component of manual therapy techniques such as myofascial release and soft tissue mobilization. During more advanced rehab phases, Keller says, sports taping can be used to facilitate a muscle or to inhibit a muscle, depending on how the tape is applied.
“We look at the [taping process] as a way to maintain the progress we get at the end of each treatment, to last to the next treatment,” Keller adds.
A bit of well-placed psychology can also be useful for PTs working with restless athletes who itch for a return to competition. Keller, a veteran clinical therapist, recognizes the sense of urgency that builds within mending athletes, and has learned to cultivate patience by getting an athlete to buy into a complete rehab program. Not only can the buy-in positively skew the outcome of therapy, but it can work in favor of an athlete’s desire to get back into play.
“The PT really has to connect with the athlete so that they will ‘hear’ you when you say that if they shorten the appropriate rehab cycle, they will most likely forfeit their whole career—not just the single season,” Keller says.
“Psychologically, I find that if we involve the athlete in a ‘well body program,’ they do much better,” she continues. “This entails pushing them in workouts that include all of the uninvolved limbs so that they stay in optimal shape. It also allows an outlet for their energy.”
Even with the advantages conferred by top clinical tools and an optimum client state of mind, injury frequency remains a wild card that can significantly impact the probability an athlete will return to play quickly—if at all.
“In general, it isn’t the specific injury that keeps the athlete from returning, but rather if it’s the third or fourth surgery to the involved knee,” Keller says.
 |
| A sports brace is used by an athlete during competition to protect/block the knee. |
INTERPERSONAL DYNAMICS
Susan Sigward, DPT, University of Southern California assistant professor of research physical therapy, agrees with Keller, and underscores the importance of the investment rehab professionals must be willing to make in understanding the cause of a lower extremity reinjury. And the causes are not always obvious.
“In defense of PTs,” Sigward says, “I think it’s sometimes difficult in the atmosphere around competitive sports injuries to make sure athletes are not returning to play before they’re ready.”
Sigward cites the conflicting interpersonal dynamics that sometimes emerge among stakeholders in an athlete’s rehab: coaches, parents, insurance companies—sometimes the athletes themselves —can all potentially complicate the rehabilitation strategy. She believes such complications can raise the probability that a thorough therapy program will be cut short. Sigward laments the trend away from programs that once worked to restore an athlete’s everyday function, and then steadily progressed that athlete back through a continuum of sport-specific rehab. Such programs, she says, have become impractical—eroded mostly by insurance coverage that has reined in the number of therapy sessions a policy will cover.
Yet, Sigward says, clinicians remain able to sustain effective, efficient rehabilitation programs for serious lower extremity sports injuries by adopting current technologies as well as implementing what has been learned through the latest research in physical medicine. Mobilization, she says, is emerging as a key method of shortening healing times and ultimately getting an athlete back to function sooner.
“Years ago, we immobilized these guys who had ACL [injuries] and it was just a nightmare, but healing, we’ve learned, is stimulated by motion,” Sigward says. “And I think for surgeons and therapists there is now the question of ‘How can we allow them to have safe motion and still protect the joint?’ I think the answer to that is always evolving.”
At The Stone Clinic, where Keller performs the majority of her clinical work, allografts have become a staple of ACL reconstruction, and little time passes before motion is worked back into repaired joints. Keller says that a postoperative brace is prescribed for approximately 1 week after reconstructive surgery to ensure that the patient has recovered sufficient muscular control.
“There are some cases where the knee needs to be blocked at a specific angle for proper healing during the first month,” Keller explains, “so in those cases use of the brace is necessary.” She adds that a sports ACL brace can be used by an athlete while training and competing in the at-risk sport for up to 1 year after surgery, by which time the allograft typically has fully matured.
An increase in sports participation across age and gender boundaries is likely behind the recent upward trend in knee injuries, according to Rick Riley, president, Townsend Designs, a provider of custom and off-the-shelf bracing solutions.
“The vast majority of patients are braced following an ACL injury,” Riley says, and suggests it is the size and shape of a patient’s leg—rather than severity of injury—that become the justification for using a custom brace. He says the rigidity, durability, and generally more extensive warranty coverage of custom graphite braces make them the best option for athletes who participate in high-velocity sports.
Riley adds that advances in surgical technique and rehabilitation protocols—as well as limitations created by insurance providers—have touched off a decline in prescriptions for functional knee braces; he believes braces can provide additional stabilization and peace of mind over the long term.
“I have torn my ACL twice, and trust me, you never want to go through the surgery and rehab a second time,” Riley says.
 |
| Karen Corriveau, PT (left), of CATZ Physical Therapy Institute, Pasadena, Calif, oversees soccer player Lindsay Wofford’s therapy, post knee surgery. |
PREVENTION AND SOOTHING
As an advocate of prevention, Sigward urges PTs to recognize that proper mechanics should not be short-sold as a way to stave off catastrophic joint blowouts. She suggests many ankle and knee injuries may actually originate with poor hip strength, and notes that if the hip fails to provide adequate stabilization, the body will rely on the knee and ankle to control and generate motion.
“Keeping a little more of a neutral alignment is really what we think is helpful in decreasing the risk for injury in the lower extremities,” Sigward says. She adds that because young female athletes lack the natural strength of their male counterparts, their therapy should include a focus on restoring strength to the injured areas as well as all the involved joints.
“Reducing ACL injuries even at the younger ages has a lot to do with athletes keeping knees apart, using their butts, using their quads and hamstrings, and using balance exercises,” Sigward says. “Mechanics, strength, power, and a certain level of plyometrics. Those things are all important at all ages.”
The bulk of lower extremity sports injuries, Sigward points out, tend to occur in the ankle, rather than the season-ending knee injuries that have become associated with high-profile collegiate and professional competitors. Treating the strains and sprains suffered by the nation’s countless anonymous athletes—specifically those that do not require surgical intervention—Sigward says is best handled by therapeutic interventions that restore or improve strength, range of motion, or flexibility.
“The important thing is to use the e-stim or ice or massage to help with the symptoms of the injury. If you have an acute injury where there was inflammation or have someone who had severe muscle atrophy and needed early on to stimulate those muscles, cryotherapy or e-stim can typically be used to defeat the symptoms,” Sigward says.
Keller agrees that go-to modalities such as e-stim, aquatic therapies, massage, and cryotherapies are useful, nonsurgical treatment for athletes who are seriously injured, yet have not torn through a ligament or meniscus. Postsurgically, she says, they continue to enhance the outcomes of improving surgical techniques.
“The day these modalities become moot,” Keller muses, “is the day they invent a surgery that does not invade the joint capsule and create the comorbidity of postoperative swelling and neuromuscular inhibition.”
Frank Long is the associate editor of Rehab Management. For more information, please contact .




