Hand surgeons and rehabilitation teams all agree hands down that the distal radius fracture is one of the most common occurring fractures. One-sixth of all fractures found in the acute care setting are fractures of the distal radius.1 The distal radius fracture also remains one of the most complicated to manage despite increased technological and medical advances. It is not uncommon for patients to experience functional limitations following a distal radius fracture, which may persist up to 2 years after the injury. Since the hand is the interface for the majority of activities performed in daily living, a distal radius fracture presents a unique set of challenges for upper extremity surgical and rehabilitation teams. Additionally, the patient needs proper education and motivation to maintain their individual home therapy plan, avoiding further complications and conditions.
COMPLICATIONS
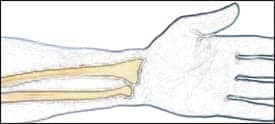 |
Human culture has long recognized the importance of the hand in functional activities. Several occupational performance components may be compromised by an injury to the wrist or hand. Some of the complications associated with this fracture are traumatic arthritis, mid-carpal instability with a deviation in volar inclination of the articulating surface, and an increase in dorsal tilt often inhibiting wrist range of motion.2 Overall grip strength and forceful pinch also may be altered with variations in radial inclination.
The degree of impairment and associated complications depends on many independent factors such as age, hand dominance, and severity of injury.
SUCCESSFUL MANAGEMENT
Hand surgeons and therapists agree that therapy is an integral part of successful management, particularly distal radius fractures requiring some type of surgical intervention. It is a priority to treat these fractures properly, considering that approximately 15% of all fractures across gender and age groups are distal radius.3 This also includes educating and motivating patients to continue their rehabilitation plan at home to prevent potential complications.4
TREATMENT GOALS
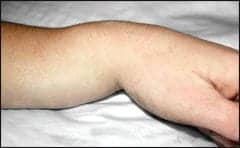 |
| The “dinner fork deformity” is the classic finding in a Colles’ fracture, which is produced by dorsal displacement of the distal fracture fragments. |
Initially, the surgeon seeks to obtain and maintain anatomic reduction. The ability of the surgeon to achieve this goal directly influences the functional goals set by the rehabilitation therapist and patient.
After proper anatomic reduction is maintained, the rehabilitation therapist begins treatment to restore upper extremity function with full range of motion (ROM) to shoulder, elbow, fingers, and thumb with a maximum pain-free wrist and forearm ROM.4 Optimally, treatment begins while the patient’s wrist is still immobilized.5 The benefit of treating the distal radius fracture early is resolution of edema and pain, and achievement of full ROM to fingers and proximal joints before the wrist is ready to be mobilized. At the same time, it also allows for some function in light daily living activities.
MEDICAL TREATMENT
Medical treatment options for a distal radius fracture include either a closed or open reduction. The closed treatment often includes casting or supportive splinting. Open reduction and internal fixation provide many surgical alternatives. These alternatives include stabilization through pins, external fixators, internal plate stabilizers, or various combinations.
Management of a distal radius fracture is dependent on fracture patterns and displacement, so it is important to initially determine if the fracture is stable or unstable. As a general rule, stable fractures present with minimal comminution, less displacement or angulation, and insignificant involvement of the radioulnar and radiocarpal joints.4 A Colles’ fracture is an example of one of the most common stable fractures and is minimally displaced and extra-articular.5
Unstable fractures often require more than casting. They usually present with more complications and come with greater medical and therapeutic needs.4 Unstable fractures tend to have significant volar or dorsal comminution, involvement of the radiocarpal joint with a tendency for lateral displacement of the radial styloid, and depression of the lunate fossa fragment.4 Restoration of normal axial, rotational alignment and length is necessary to prevent inert or incomplete healing.6 More aggressive treatment such as pins and internal fixation prevents displacement and loss of position. Research developments and technological advances have now allowed surgeons to achieve maximum alignment and strong fixation for comminuted fractures. Malunion or nonunion is a complication resulting from the inability to restore any of these factors.
Restoration of the anatomy is critical to the final radiographic and functional outcome.4,5,7 Many credible studies have reported that closed methods and external fixation of displaced, comminuted intra-articular fractures of the distal end of the radius have had unsatisfactory final results.8 Immobilization often causes stiffness with the hand, wrist, elbow, and shoulder. Other complications with immobilization often include infection, loosening of the pins, and loss of reduction. Permanent stiffness and weakness also have been noted in patients receiving external fixators.9 For these reasons, external fixators are not the preferred choice by hand surgeons treating a comminuted fracture of the distal wrist. In their place, internal plate and screw methods have become much more widely adopted. The volar plating systems allow for stable reduction and earlier motion.10 Surgeons continue to develop and refine their fixation technique to restore the distal radius anatomy with better predictability and fewer complications.
REHABILITATION TREATMENT
Therapeutic management for the distal radius fracture is far from simple or straightforward.5 After the physician provides acute care and management, the rehabilitation team begins their work in the recovery process. They aim to achieve rapid, complete, and pain-free recovery of function.
The primary goals for rehabilitation of the distal radius fracture are reduction of edema, strengthening, and increased range of motion. Secondary goals for rehabilitation include wound care, pain management, splinting, scar management, modalities, and resistive exercises. Lastly, it is crucial that the rehabilitation team also educate and motivate their patients effectively to continue the established home program beyond clinical treatment.4,5
EDEMA
 |
| Therapeutic putty exercises can help improve tendon gliding in cases where fractures are more severe and involve damage to tendons or open surgical procedures. |
Soft tissue trauma will cause edema. Treatment for edema always includes elevation of the upper extremity. However, some of the arm positions used for elevating the upper extremity can cause additional problems. Internal rotation and elevation of the shoulder to approximately 90º can cause shoulder impingement.2 Prolonged flexion of the elbow can cause ulnar nerve irritation manifested by increased pain and paresthesias in the small finger. It is critical that the rehabilitation therapist communicates these potential problems to their patient when elevation of the upper extremity is necessary as well as providing proper techniques to prevent problems.
Some other proven ways to help reduce edema are soft tissue massage, electric stimulation, and edema compression sleeves and gloves.2 Maintaining the patient’s shoulder motion also is crucial, not only in preventing stiffness but also for reducing edema. The motion of the shoulder keeps the venous outflow and lymphatic system in the axilla moving freely. This in turn helps reduce the amount of swelling and promotes motion of the hand.
REST AND IMMOBILIZATION
Studies have consistently proven the injurious problems that prolonged rest and immobilization can cause after a patient experiences a traumatic event. Prolonged rest may delay recovery and be detrimental to musculoskeletal tissues.11 Contractures, joint stiffness, overabundant scar tissue formation, muscle atrophy, tendon adherence, and extensive fibrotic and cellular changes are some of the complications associated with prolonged rest.5,6,11,12
In the past, treatment of distal radius fractures required a period of prolonged immobilization. The fracture reductions were maintained through the use of casting, pins, or external fixators that limited the motion of the joints. Limitations in range of motion were due to the inability to restore proper anatomical alignment of the palmar tilt angle or distal radial ulnar joint congruency.4,5,11 Restoring the wrist extension is also difficult secondary to the position of the wrist during immobilization.
RANGE OF MOTION (ROM)
ROM maintains joint capsule and ligament mobility, prevents adherence of soft tissue, aids in the reduction of edema, and increases circulation of nutrients.2 Rehabilitation therapists commonly prescribe active and passive ROM for upper extremity joints for fractures of the distal radius. When prescribed, it is important that the therapist and patient collaborate together to design a home exercise program specific to their needs.
A patient’s home exercise program may include shoulder, elbow, forearm, wrist, and digits. Specific hand exercises may include tendon gliding, metacarpophalangeal flexion and extension, thumb extension and opposition, and web space stretches. Tendon gliding exercises (for flexor digitorum profundus, flexor digitorum superficialis) also have proven to be productive for digital active ROM.3 If joint stiffness persists, then passive ROM may be implemented to promote motion. Passive ROM may be implemented via various stretching techniques as well as custom-fabricated static progressive and dynamic splints.2
STARTING EARLY
Concerns exist regarding the time at which wrist motion should resume after reduction is obtained. Early mobilization is generally advocated by the existing literature.4,5,10,13-15 Beginning wrist and finger motion early prevents complications of stiffness, muscle atrophy, osteoporosis, and degenerative arthritis. An exception is the radioulnar joint, which requires the longest period of immobilization, and thus early range of motion in the wrist is contraindicated.16
STRENGTHENING
Fractures of the distal radius that are more severe and involve soft tissue trauma such as damage to the tendons or open surgical procedures may require resistive forces to improve tendon gliding. Many therapists will incorporate therapeutic putty exercises into the rehabilitation program to improve tendon gliding.17 Exercises such as gripping, rolling, pinching, scraping, full flexion and extension of extrinsic muscles, and looping can all be done with putty.4,17 Intrinsic muscle exercises with putty or rubber bands also should be included in this type of rehabilitation.17 In later stages of healing, the patient can regain strength in their hand and forearm as they increase use in their daily living activities.
SUCCESS
Intra-articular fractures of the distal aspect of the radius are complex and multifaceted injuries with considerable associated morbidity. Despite excellent or good results, functional difficulties may persist for periods as long as 2 years following the injury.18 This implies that recovery from these fractures is substantial and time-consuming. Maximum improvement for most distal radius fractures will not occur quickly, typically taking several months. Patients are discharged from their managed care environment before maximum improvement is reached.2 For this reason, it is important that rehabilitation therapists successfully educate and motivate their patients to work at their recovery beyond the managed care environment.2 Optimal recovery will occur when patients successfully accept full responsibility for their rehabilitation as well as continue with their home exercise program established for them in managed care.
Sonia Brodeur-Lyons, OTR, CHT, and Matthew W. Oakes, MS, OTR, CHT, are occupational therapists and certified hand therapists at Mary Free Bed Rehabilitation Hospital, Grand Rapids, Mich. For more information, please contact .
REFERENCES
- Morrow D, Knight J. Management of Colles fracture: a primary care approach. Physicians Assistant. 1997;21:81-9.
- Laseter G. Therapist’s Management of Distal Radius Fractures. Rehabilitation of the Hand and Upper Extremity. 5th ed. St Louis: Mosby; 2002:1136-1155.
- Katarincic JA. Fractures of the wrist and hand. Physical Medicine and Rehabilitation: State of the Art Reviews. 1998;12:263-82.
- Laseter GF, Carter PR. Management of distal radius fractures. J Hand Ther. 1996;9:114-28.
- Collins DC. Management and rehabilitation of distal radius fractures. Orthop Clin North Am. 1993;24:365-78.
- Schemitsch EH, Richards RR. The effect of malunion on functional outcome after plate fixation of fractures of both bones of the forearm in adults. J Bone Joint Surg Am. 1992;74:1068-78.
- Hove LM, Furnes O, Nilsen PT, Oulie HE, Solheim E, Molster AO. Closed reduction and external fixation of unstable fractures of the distal radius. Scand J Reconstr Hand Surg. 1997;31:159-64.
- Bradway JK, Amadio PC, Cooney WP. Open reduction and internal fixation of displaced, comminuted inta-articular fractures of the distal end of the radius. J Bone Joint Surg Am. 1989;71:839-47.
- Edwards GS Jr. Intra-articular fractures of the distal part of the radius treated with the small AO external fixator. J Bone Joint Surg Am. 1991;73:1241-50.
- Smith RS, Crick JC, Alonso J, Horowitz M. Open reduction and internal fixation of volar lip fractures of the distal radius. J Orthop Trauma. 1998;2:181-87.
- Buckwalter JA. Effects of early motion on healing of musculoskeletal tissues. Hand Clin. 1996;12:13-24.
- Zemke R. Remediating biomechanical and physiological impairments of motor performance. In: Trombly CA. ed. Occupational Therapy for Physical Dysfunction. 4th ed. Baltimore: Williams & Wilkins; 1995:405-22.
- Bennett GL, Leeson MC, Smith BS. Intramedullary fixation of unstable distal radius fractures. A method of fixation allowing early motion. Orthop Rev. 1989;18:210-17.
- Raskin KB. Management of fractures of the distal radius: surgeon’s perspective. J Hand Ther. 1999;12:92-8.
- Trumble TE, Schmitt SR, Vedder NB. Internal fixation of pilon fractures of the distal radius. Yale J Biology Med. 1993;66:179-90.
- Contesti LA. The radioulnar joints and forearm axis: therapist’s commentary. J Hand Ther. 1999;12:85-91.
- Weinstock TB. Management of fractures of the distal radius: therapist’s commentary. J Hand Ther. 1999;12:99-102.
- Knirk JL, Jupiter JB. Intra-articular fractures of the distal end of the radius in young adults. J Bone Joint Surg Am. 1986;68:647-59.




