|
The scene of the accident: the victim’s home.
The victim: male or female, typically elderly or physically impaired, perhaps bruised or frightened that something worse will happen next time.
The suspected causes: the tip of a loose carpet, dark lighting, several bottles of medication, or a vestibular condition.
There is no crime here, but an accident in the form of a person tripping, slipping, or falling at home. When a physician refers a client to a PT or OT for fall-prevention evaluation and therapy, it is the therapist’s task to uncover the true cause—or causes—of the fall or near fall, and to apply solutions that will reduce the risk of another fall happening again.
Lisa Roberts, PT, DPT, GCS, says, “Physical therapists are oftentimes detectives when we investigate the falls: We look at the time of day. Was it a particular action that caused the fall? Was it a certain medication? Was it during the time of eating a meal, drinking alcohol? If we can figure out what caused it, then that can give us a really good clue as to how to prevent the next one.” A thorough investigation that identifies the cause or causes of the fall will then allow the therapist to prescribe the best course of therapy and, if necessary, the right assistive devices or home modifications.
“In a perfect world, we would see a patient even before a fall or near fall occurred,” Roberts says. “I think as PTs and OTs, we really want to encourage physicians to target individuals who are at risk for a fall, so we can see them before something happens and intervention can be given. Falls can be so traumatic, emotionally and physically. They cause fractures, and many individuals who have had falls never quite regain their premorbid state.”
FINDING CLUES FROM A THOROUGH EVALUATION
Fall-prevention detective work begins by a therapist asking a series of questions about the incident. Some of the basic questions a therapist might ask to get the full fall history include:
Where did it happen? Where was the client standing? In the tub? Getting up from the toilet? Being specific will be helpful for suggesting home modifications.
What time of day did the fall occur? At night with low levels of light or in the day when there was supposedly plenty? These questions may include or eliminate poor lighting as a concern.
What was the client doing at the time of the fall? Bending down to reach something? Standing up from a chair? Walking? Climbing or descending stairs?
Did the client feel dizzy before the fall? If so, this may indicate a balance problem or perhaps a need to look at medications, nutrition, or other ailments, such as diabetes. Likewise, it is also important to ask if the patient was drinking alcohol at the time, and if so, how much?
What medications were taken? Were they taken as directed? When?
Does the client wear glasses? Was he or she wearing them at the time of the fall?
Was the client fatigued at the time of the fall?
Does the client remember falling? Getting up?
Could the client get up without help, or was assistance required?
Describe the home environment, both inside and outside. If unavailable for a home visit, can someone take pictures or a video?
Are any assistive devices used, such as a cane or walker?
What shoes or clothes were worn during the incident? Do they fit well? Some patients may be tripping on shoes that are too big or pant cuffs that are hanging lower because of weight loss.
These are but a few of the questions that can provide a full fall history. The answers given may lead a PT to suspect one cause or perhaps several causes.
REVEALING THE PATIENT’S STRENGTHS
After the verbal evaluation, the next step is performing a series of physical tests that will further reveal the patients’ strength, balance, gait, and function. Most of these physical evaluation tests should be familiar to therapists, such as:
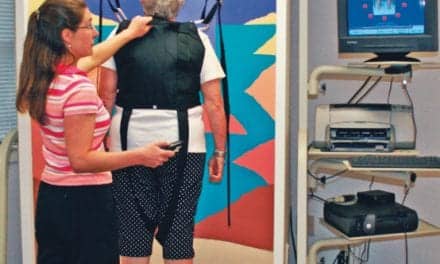
 |
| A significant part of fall prevention is maintaining physical strength throughout life. |
- the manual muscle test;
- the functional reach test;
- the timed get-up-and-go test;
- the Berg balance test;
- the Tinetti balance and gait test; and
- the Dix-Hallpike test for vertigo.
Michelle McCarthy, PT, DPT, OCS, Westwood Physical Therapy, Los Angeles, says she prefers the Berg balance test because it provides a large amount of information through simple exercises, such as standing with eyes open or closed, standing on one foot, sitting, and standing. The Berg test scores the patient’s physical response to each exercise with a value from 0 to 4, with 4 being the highest level of independence, and 0 indicating the lowest ability, possibly with the need for assistance.
Scoring not only provides an indication of the level of disability, but also provides a record of the patient’s abilities before therapy. After therapy is complete, the same tests and scoring can be used as an objective method for measuring improvement.
While many tests require little more than a chair, PTs can also use many common therapy tools to assess patients. Mark Lewis, PT, assistant director of Downeast Rehabilitation Associates, Rockport, Me, uses several tests that incorporate sitting on a therapy ball to observe trunk strength and the patient’s ability to compensate for the ball’s instability. McCarthy often incorporates using a trampoline for both balance-testing and balance-correcting therapy.
Roberts stresses that therapists should be flexible with their testing and adapt assessment protocols to the needs of the individual. For example, while the Berg test may be effective, it requires a great deal of direction that may confuse an elderly patient with dementia or other cognitive disability. Instead, they may do more functional tests, such as simply observing gait, standing up from a chair, sitting, or getting in and out of bed.
THE RUG DID IT … SO DID MY WEAK HIP
After a thorough fall history and physical evaluation, therapists use the test results to pinpoint the cause—or causes—of the fall and work on ways to prevent it from occurring again.
“The causes can be numerous,” McCarthy says. “It could be a peripheral neuropathy, where they can’t really feel their feet very well, or there’s something that’s causing weakness, or they just have simple muscle weakness from less overall activity.”
Other common causes include a vestibular problem, the home environment (poor lighting, and trip and slip hazards) mixed medication, undiagnosed eye disease, the need to change eyeglass prescriptions, or arthritic pain.
The treatment plan that is implemented will be defined by the patient’s history and physical evaluation. For most patients, there will be some component of therapeutic exercise and strengthening, balance and coordination activities, functional training based on the patient’s needs, as well as patient education. Therapists may also have to contact physicians or optometrists if it appears that medication or vision problems are involved with the fall.
In addition to physical therapies and adjusted medical treatments, solutions may include home modification, where grab bars, railings, ramps, and better lighting may be added to various rooms. These suggestions can be made based on a PT visiting the home. However, if that is not possible, a verbal description, photographs, or a video of the home environment may be an adequate substitute for a visit.
STRENGTH TRAINING
Some kind of resistance training will be used to strengthen the weak muscles that were identified in the evaluation. The type of resistance and how much will depend upon the patient and evaluation. In general, therapists work on strengthening the calf, the quadriceps, and the abdominal muscles.
Roberts says, “We do need to stress the system somewhat in order to achieve some gain in muscle strength. So we want to challenge our patients with resistance training, and yet not overtax a possibly fragile system.”
Lewis will often use recumbent stepper machines and treadmills. Therapy balls can also be effective for reaching exercises, as well as working on the lower extremities, having the patient perform ball squats.
BALANCE TRAINING
For balance training, McCarthy says that she will start with some of the basic exercises, such as standing on one leg, and allow the patient to use their hands for support, then gradually let them remove that support.
For more adept patients, therapists can use a trampoline, a rocker board, or closed cell foam to place the patient on an unstable surface. As patients learn to compensate on these unstable environments without help from the therapist, they will feel even more stable performing similar exercises and functions on normal surfaces. When patients become more confident, their balance may become further developed by therapists nudging them or by gently moving the unstable platform.
Exercises that make use of a chair, countertop, or wall may also be valuable because the patient can repeat them at home. For example, the person can stand between two chairs and practice standing on one foot, or do a heel-toe rocking exercise while using the chairs for support. Patients can also place a chair in front of the kitchen counter or other secure surface and practice sit-to-stand exercises 15 to 20 times per day or as many times as possible. Heel-toe walking inside a hallway and without touching the walls unless necessary is another simple balance exercise that patients can practice in therapy or at home.
GAIT TRAINING
“One of the most interesting things that a physical therapist can do is teach someone how to walk again,” Lewis says. “By the time you start breaking the task down and building it back up again, you wouldn’t believe what some of these people look like when they’re walking. You have to be careful not to confuse the issue too, not overthinking every little aspect of it. Teaching people proper gait is sort of an art in and of itself.”
|
To learn more about |
|
For gait training, Lewis encourages his clients to take longer steps. He sometimes sets up a little obstacle course with cones or hurdles so that patients can practice switching directions and stepping over obstacles. Lewis will also observe and give verbal cues, prompting patients to pick up their feet more, or to remind them to put their heel down before the toe.
Some clients may require an assistive device, such as a cane or walker, but Roberts points out that assistive devices need to be measured appropriately and that patients have to be properly trained to use them. She says, “If I gave a person a cane to help their balance, he needs to learn how to use that cane indoors, on tile, on carpet, and I need to take him outside and teach him how to walk on uneven terrain, up and down a curb, up and down the stairs, because that’s what we encounter in day-to-day life.”
CLOSING THE CASE
Therapists should generally like to see fall-prevention clients for three 45-minute sessions per week, lasting for 6 weeks, though some patients may need more time, depending on the issues being addressed. However, the client may not be able or willing to meet those expectations, and insurance and Medicare coverage may also limit coverage.
As clients become stronger at the end of the program, teaching them how to get up after a fall may be one of the last segments of the rehabilitation program. Depending on the abilities of the client, the lessons should include not only how to properly stand to avoid further injury, but also when not to stand.
Roberts says, “If they’re hurt, naturally, I don’t want them trying to get up from the floor.” Instead, Roberts tries to have patients learn to be aware of their abilities and to be prepared for an emergency by having portable phones around the house that are reachable. She also recommends that patients move older phones that are installed on walls to lower table surfaces that can be more easily reached. Another effective, but possibly costly, solution is to have an emergency alert system that is wearable as a necklace or wristwatch.
By the end of a fall-prevention and therapy program, therapists, clients, and other health care providers will hopefully have worked together to correct all the issues discovered in the initial assessment. If clients continue their therapy exercises at home, there is a good chance that a PT will never need to return to another accident scene.
Tor Valenza is a staff writer for Rehab Management. For more information, contact .