In the United States, falls are the leading cause of death from unintentional injuries among adults age 65 years or older, according to CDC data.1 In 2010, the direct medical costs of falls, adjusted for inflation, were $30 billion, and by 2020, the annual direct costs are expected to reach $54.9 billion.2 As our healthcare is restructuring, falls are a major focus. As of October 2008, US hospitals and skilled nursing facilities (SNFs) are at risk of losing Medicare reimbursement for the treatment of falls injuries occurring during patients’ stays if the falls were preventable. Other third-party payors are following the Medicare program’s initiative and will no longer pay for certain hospital-acquired, preventable injuries such as those related to some falls. Falls are a common and complex geriatric syndrome that causes considerable mortality, morbidity, reduced functioning, and premature nursing home admissions.3 According to Stevens et al,2 the direct medical cost to treat individuals age 65 years or older who sustained fall-related injuries such as fractures was $19 billion. Last year, more than 340,000 hospitalizations resulting from hip fracture have been reported.4 Up to 75% of individuals with a hip fracture fail to return to their previous level of function, and at 6 months post, only 8% can climb a flight of stairs, and only 15% could walk across a room independently.5,6
More inpatient facilities are going “restraint-free,” and as reporting on falls is becoming a regulatory requirement—and as the aging population is more educated and prefers to age successfully—therapists in all areas of care are cued to develop optimal, effective programs to reduce falls. It is paramount for therapists to develop programs for clients that are sustainable and cost-effective. The most favorable prevention strategies involve multidimensional fall risk assessment and exercise interventions. Incorporating these intervention strategies whenever feasible into a fall prevention program appears to be the most effective way to reduce falls among older adults. According to Rubenstein et al,3 falls usually are the result of interactions between multiple intrinsic and extrinsic risk factors.
Most therapists are aware that leg weakness has been identified as the most potent risk factor associated with falls, increasing the odds of falling by more than four times. Effective exercise prescription can improve leg strength, physical activity, and quality of life. In fact, epidemiological evidence suggests that the incidence of hip fractures in the older population can be cut nearly in half with physical activity throughout life.7
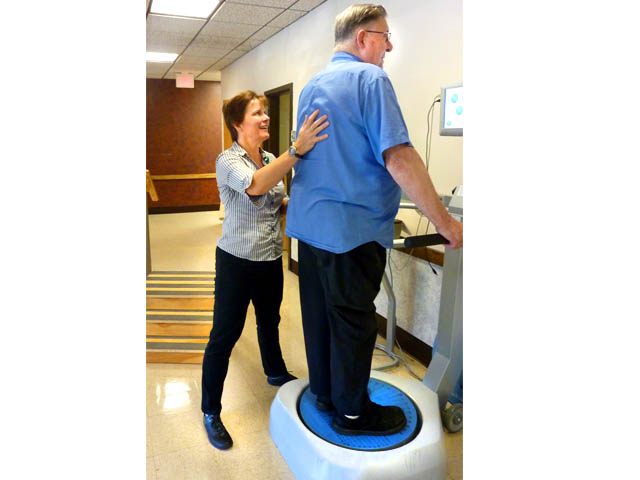
Karen Knoll, PTA, works with a patient, Paul C., using the dynamic plate system and the manufacturer’s recommended fall risk screening tool.
So, if falls are the leading cause of injury and accidental death among adults older than age 65 years, but can be prevented, what tools are needed to gather data and help clients make a quantifiable gain? The answer is the basis of our core college curriculum on exercise prescription, where student therapists learn that intensity must be sufficient to overload the cardiovascular, pulmonary, musculoskeletal, and neuromuscular systems without overstraining. This concept applies to clients of all ages. A simple sit-to-stand exercise can be modified to meet the prescribed intensity simply by cueing the client to hold a half standing position or using a lower seat. Whether performing toe raises, side-lying abduction, or supine straight leg kicks, the key is selecting resistance closer to 1RM (max) that is challenging enough to yield hypertrophy. The right assessment tools, the right exercise prescription, and regular monitoring of the response to exercise are paramount to successful rehabilitation and fall prevention.
Assessing for fall risk
Multiple assessments can be used to assess risk for falls and underlying weakness in adults. These include: TUG, DGI, BERG, BEST, FAB, 30 sit-to-stand (STS) test, hand dynamometer, mCTSM, Romberg, and many more. When choosing a standardized tool to assess a client’s frailty and risk for falls, remember that higher functional adults will fly through TUG and 30STS as well as BERG balance tests, which have a ceiling effect. Choosing assessments such as FAB, miniBEST, or mCTMB can help to better identify risk and impairments. Intelligent equipment and software on the market assist with gathering data and have real-time objective reports. Technological tools that help to assess fall risks include a moving balance plate, computer dynamic posturography (CDP) equipment, and gait analysis systems. One of these systems uses a static or dynamic foot plate and includes a comprehensive fall risk screening and conditioning program and protocol to help the clinician begin a fall program. This technology can compare balance test results to age-dependent normative data as well as assist with selection of G codes and optimal documentation. This system is frequently used at Golden Hill Nursing and Rehabilitation Center (GHNRC), in Kingston, NY. As therapists use this system, the real-time printout of reports is helpful to alleviate nonbillable time spent on documentation. Major brands of CDP systems are used to objectively measure the functionality of GHNRC patients’ three sensory inputs, which include somatosensory, vestibular, and visual systems. This establishes a baseline for patients in their rehabilitation program and enables therapists to retest them after a month to see how they are progressing.
Gait analysis plates and walkways use ground reaction forces (GRF) and the friction component of those forces to evaluate risk for falls. Tao et al8 has completed a systematic review of wearable sensors and reported that “… gait analysis using wearable sensors provided quantitative and repeatable results over extended time periods with low cost and good portability, showing better prospects and making great progress in recent years.” Though some sensors are worn in shoes and are used throughout the day, others such as gait analysis treadmills and walkways are used for assessment, reassessment, and training by the rehabilitation provider. These walking pathways measure kinetic forces, with focus on GRF to study gait kinetics. By analyzing gait, falls can be predicted and, in some cases, prevented.
Fall Reduction Tools
As healthcare continues to shift, the challenge of caring for a subacute patient after a fall or surgical hip fracture intervention is no longer a hospital’s responsibility. Instead, this challenge cascades down onto skilled nursing facilities and home care. Viable fall reduction programs and solid postoperative rehabilitation programs are the key in reaching clients’ goals and returning them to the prior level of function. According to Hatch and Lusardi,9 regular participation in an individualized wellness program twice weekly for 9 to 12 months protects against functional decline and risk of falls in older adults in assisted living settings. As a key to successful aging, effective fall reduction activities require large energy expenditures and muscle overload. In this context, body weight support systems (BWS) can help clients exercise without worrying about falls. While protected by a harness support system, clients can increase the challenge placed on their bodies. Unweighting capabilities can assist with increased levels of exercise within the available degrees of mobility. BWS systems used over the treadmill typically can offload a percentage of body weight and allow a client to perform higher intensity exercise while keeping up with the predetermined speed of the treadmill. In fact, I was able to engage one of my clients, a 75-year-old female who has lived with Parkinson’s disease for 15 years, to jog at 5.3 miles per hour using one of these systems. On the other hand, using the ceiling track BWS system allows clients to negotiate stairs, and perform step up exercises, challenging balance activities, and so much more, all while being supported and safe, but not unweighted.
Shoe sensors are another example of how technological evolution is focusing on fall prevention. A recent development in these types of sensors allows clients who are losing balance to adjust and avoid a fall. This sensor uses the same system that tells a tablet computer to swing from landscape to portrait at the twist of a hand. Sensors save individual data to analyze gait and anticipate loss problems in the future. Virtual retraining is also being researched. This method uses a sensory weight-shifting mechanism to affect motor control and functions by utilizing information from somatosensory, vestibular, and visual systems. Many inpatient rehabilitation facilities and skilled nursing facilities have implemented fall prevention teams that include a review of the incident, environmental and physical interventions, and care planned means of prevention. A facility’s therapy department may prescribe an assistive device after a fall. Though use of compensatory equipment may be necessary to optimize safety, this strategy should never be used as a first choice for rehabilitation. Education is crucial.
While treating, ask yourself whether returning patients to a “functional” level is the answer to their success? Function is a relatively low level of activity and does not assume a good quality of life. Within functional limits (WFL) doesn’t assume improvement, rather maintenance. I asked 30 residents, ranging from 67 to 96 years of age, the following question: “Would you like to be successful in aging?” Their answer unanimously was “Yes.” As professionals responsible for optimal exercise prescription to promote functionality, therapists must always remember that a client’s engagement in life and higher levels of functional abilities are the fundamental criteria for successful aging. Successful aging yields reduction and obliteration of falls. RM
Viktoriya Friedman, MSPT, is a Regional Director of Rehabilitation Services at VestraCare. Prior to assuming this role in 2014, she worked as a director of rehabilitation services at Susquehanna Nursing and Rehabilitation Center for 8 years. During her career, Friedman has focused on operational management of rehabilitation departments, growth of direct rehabilitation teams, Medicare compliance, clinical reimbursement, and advocating for people living with Parkinson’s disease. She assisted with implementation of a SNF-based telemedicine program in her region, partnering with the University of Rochester to maximize care of clients and community members living with movement disorders. In 2012, these developments were recognized by NYSHFA with an Innovative Practice Award. For more information, contact [email protected]
References
1. Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. Web–based Injury Statistics Query and Reporting System (WISQARS) [online]. Accessed August 15, 2013.
2. Stevens JA, Corso PS, Finkelstein EA, Miller TR. The costs of fatal and non-fatal falls among older adults. Inj Prev. 2006;12(5):290-5.
3. Rubenstein LZ, Josephson KR. Falls and their prevention in elderly people. What does the evidence show? Med Clin North Am. 2006;90(5):807–824.
4. http://www.cdc.gov
5. Weinrich et al. 2004
6. Marottoli et al. 1992
7. Beck BR, Snow CM. Bone health across the lifespan—exercising our options. Exerc Sport Sci Rev. 2003;31(3):117-22.
8. Tao W, Liu T, Zheng R, Feng H. Gait analysis using wearable sensors. Sensors (Basel). 2012;12(2):2255–2283.
9. Hatch J, Lusardi MM. Impact of participation in a wellness program on functional status and falls among aging adults in an assisted living setting. J Geriatr Phys Ther. 2010;33(2):71-7.