Integrating specialty equipment maximizes knee and lower extremity rehab.
by Robert Babb, PT, MBA
Several years ago, I referred my crosstown brother-in-law to a physical therapy clinic close to his home after knee surgery. At 51 years old, he was the classic weekend athlete Baby Boomer with aspirations to continue recreational sports.
Three weeks and eight therapy sessions go by, and he reported doing a 2-pound straight leg raise since the initial evaluation, and his program had not changed. He was disappointed with the outcome to that point, and told me he was transferring his physical therapy to a different provider. I supported him, and would expect the same from any patient who enters my practice and feels their care has not been managed properly.
As physical therapists(PTs), we are managers. Simply put, quality physical therapists manage a variety of functions during the day, and success in their careers tends to depend on their ability to multitask responsibilities that are required for that success. The physical therapist formula is this: CS = MHR + MPR.
Career success (CS) is directly proportional to a physical therapist’s ability to manage the human resources around them (MHR), and the management of physical resources (MPR). CS cannot be achieved without continuous work and improvement on both. Furthermore, both MHR and MPR are necessary for organizational success and survival. Maximizing human and physical resources is management, and if managing is what we choose to avoid, our patient population and referrals will dwindle.
For the purpose of this article, we will discuss the physical resources from the patient’s viewpoint. For instance, some say we may have only 7 seconds to make an impression (look professional, have patients tour your clean, dust-free, organized clinic). Patients expect you to listen (key to setting up programs and developing goals), and they want your expertise to help them achieve their goals.
Impress them by managing their care with utilization of specialty equipment that helps them meet their performance goals. This can be key in creating a satisfied customer who will recommend your service.
How To Maximize Use of Equipment
Staff orientation to your clinic should include introducing and demonstrating every piece of equipment in the clinic to physical therapists. This will help staff understand the capabilities of the physical resources. Too often, in a multitasking, demanding day, therapists can forget the surrounding widgets and gadgets designed to facilitate a rapid recovery.
For instance, physical therapists in our clinic need to manage availability of the pool and set up plans to maximize the properties of the water including buoyancy (to unload a joint or to provide active assistive motion), viscosity (to strengthen against resistance), or even hydrostatic pressure (to minimize inflammation). Similarly, efficiently progressing patients from simple to complex strength routines on land requires a deep understanding of a multitude of resources (equipment) to meet patient goals and outcomes.
With that being said, simple specialty equipment can make or break a patient’s decision to stay at a clinic, or leave. Add in the patient population that dominates the outpatient physical therapy markets (Baby Boomers), and it quickly becomes understood that weight cuffs, straight leg raises, and bands motivate only a few. It is in a clinic’s best interest to become armed with simple equipment and creative ideas to excite and motivate the achy-kneed Baby Boomer or even the most sophisticated athlete.
As always, we promote active participation in a regular exercise routine that is safe, especially for the aging athletes and sedentary Baby Boomers. Commonly addressed are conditioning routines, flexibility activities, and resistance training (up to 30 to 60 minutes, 3 to 5 days per week). Imbalances identified during the initial visit will determine the level of equipment chosen, demonstrating a physical therapist’s forward-thinking processes as they work to exceed expectations and achieve goals. Some examples of equipment that offer high differentiation—if managed and maximized when appropriate—may include the following:
Conditioning (While protecting the patient’s knees and lower extremities)
Years ago, PTs had limited resources for those who were suffering from joint aches and pains. Treadmills and bikes were staples in most clinics, followed by the introduction of ellipticals in the early 90s. Ellipticals were the foundation of many speciality units that continue to be offered today, all with the aging population and aching joints in mind. Giving that daily use of these devices in a clinic is significantly less than in a health club, savvy PTs can pick up these durable units secondhand at a significant cost savings. From a patient perspective, speciality conditioning equipment offers a change from the ho-hum exercise equipment found in most clinics.
Examples of conditioning units to use in a clinic that offer differentiation, and motivate patients to higher levels of performance include:
Aquatic Therapy: Aquatic routines are designed to fully (deep water) or partially (shallow water) unload the body, and in many cases the therapeutic heat (94 degrees) offers vasodilation of the superficial vessels to permit improved flexibility of the soft tissue. Understanding the principles of water helps with quantification. Those principles include hydrostatic pressure, buoyancy, and viscosity. For use of strengthening, we may consider viscosity: Viscosity = resistance.
Documentation of resistance or supraresistance offers clarity and consistency in routines, in addition to speed against the resistance of the water. As an example, running in water can produce increased heart rate. Monitoring heart rate every 5 minutes is a measure used to motivate the patient to get them to speed up or slow down, depending on the goals. The intensity of running in deep water without joint compression is difficult to attain through traditional land-based exercises.
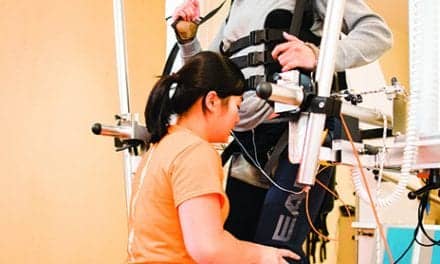
Anti-Gravity Treadmill: Due to pricing, PTs should assess these types of devices firsthand before making a purchase decision. Through air pressure technology, an anti-gravity treadmill will enable the PTs to adjust impact while walking or running (from 30% to 100% weight bearing), allow for quantifiable progressions of speed, build duration and endurance, work on acceleration, and challenge deceleration, while testing the joints on incline or decline. The “unloading” that occurs in water is also applicable on an anti-gravity treadmill, with the added benefit of more specific quantification and documentation. Application is simple, while the instruction is nominal. A pair of spandex shorts simply slides over pants or shorts with a zipper. The zipper attaches to the bubble-like chamber that surrounds the treadmill, sealing the patient in without the risk of him or her falling. If a practice can absorb the expense, it will reap the benefits of this type of conditioning unit through patient testimony and physician referrals.
Cross Trainers, Spinners, and Ellipticals: Several pieces of clinical equipment built to develop conditioning were a result of the aging population. These types of equipment include cross trainers, spinning bikes, and ellipticals. These units are ideal for conditioning with nominal compression and pounding of the joints. They can bridge the gap from unloaded (aquatic) activity, while also offering quantification and programs for documentation and tracking progress. Similar to the way children often seek feedback, encouragement, and acknowledgement of success, a clinic’s patients can become motivated by improving performance factors. In general, it is easy for patients to understand the sequence of unloading to partial loading to fully loaded conditioning exercises. This process is often explained to patients and clinic staff, and parallels the use of specialty equipment. One way to illustrate the process would be to compare unloaded activity with aquatic-based equipment, and partially loaded activity with bike, spinning bike, recumbent cross trainer, elliptical, and treadmill equipment.
In general, conditioning equipment offers increased metabolism and endorphin release to manage pain. It can also target muscle groups (glutes as an example), and provide valued tools for PTs that offer current and future avenues toward higher levels of performance and function. These devices can provide a PT with data about heart rate, total work performed, caloric expenditure, and a host of other quantitative values that can all illustrate improvement to a patient. This data can be used to provide a “report card” that motivates patients to perform on each and every visit. This class of equipment is also typically easy on the joints. With a glut of Baby Boomers continuing to age, a clinic can get repeat active lifestyle customers by maximizing these resources, and in turn getting long-term return on investment.
Flexibility ?(To keep patients’ knees and lower extremities mobile for life)
Muscle and tendon length are critical to joint integrity, function, and performance. Viscoelastic properties of muscle and tendon respond to heat, duration, intensity, and frequency of a stretch: MTL = H + D + I + F.
Given that frequency is often, rudimentary stretching should be part of the patient’s responsibility (at work and home), with more sophisticated stretching (manual and dynamic stretching, use of equipment) performed in a clinic or gym. A patient performing standing hamstring stretches, supine ham and gastroc stretches (leg raise with a cord), McKenzie prone extensions, and cats and camels should be progressed to home as soon as they are independent. Too often, PTs have these simple mat routines performed several weeks into the patient’s case. This can be a de-motivator to patients who are paying high co-pays and deductibles, and who want to learn more and do more. Do not get caught in a plan without progressions, or compliance rates will shrink. So will business.
Stretch Cages and Stretch Trainers: Well documented is the loss of viscoelastic properties of both men and women into their fourth, fifth, and sixth (and onward) decades of life. The value of flexibility should be emphasized to patients, as it permits them to remain independent as they age. Maintaining flexibility is also vital for high performance ambitions of aging athletes such as runners, bikers, and basketball players.
Offered in a variety of forms, shapes, and sizes, stretch cages offer a change from the doldrums of stretching. These self-contained devices eliminate the need for floor, mat, and plinth exercises (opening up the plinths for manual skills). In general, this equipment permits more opportunity for form control, such as maintaining the back in neutral while stretching the iliopsoas or quadriceps.
Stretching devices can provide a good way to expose patients to higher levels of stretching, particularly if obesity, lack of mobility in supine to sit, sit to stand, or proper positioning are issues. There are also stretch trainers that require the user to have greater flexibility to obtain starting positions, and offer alternatives for patients to achieve improved mobility.
Strength Training
Surgery, loss of activity, loss of muscle mass, and deconditioning after illness can lead to muscle loss and atrophy. After an ACL surgery, girth measurements are easily obtained at 3-inch and 6-inch suprapatella with decent intra/inter rater reliability (great way to measure progress). Other measures include 1RM, GMT, or dynamometer testing that quantifies levels of strength and offers decisions for progressive clinical plans. A variety of equipment is available to address the needs of this patient population, and keep them progressing and engaged in your clinic. Among this equipment are free-form functional units designed to have small footprints and offered at relatively low cost. Examples of these devices include:
Cable Units: Cable units are self-contained, movable, stable, and highly versatile. The unit can challenge a PT to design plans specific to patient needs, providing options for creativity and allowing variety in patient programs.
Kettlebells: Kettlebells have been available for years, most recently mass produced to add variety and appeal to active lifestyles. Offering a challenge to patients, kettlebells are easy to use, easy to store, highly documented on Internet video for utilization, and great motivators. (As an example, see the functional squat video at http://www.youtube.com/watch?v=i74HRv109Hg.)
Other examples of gear that can offer additional challenges to a clinic’s valued customers include medicine balls, weighted bars, and a variety of weighted vests.
Summary
It is true therapists are in the business of health care, but in direct competition with patients’ disposable incomes. A $50 co-pay may contribute to a patient’s indecision about whether to enter a therapy program since their choices to help them “get better” can include a personal trainer, chiropractor, gym, or spa. With money continuing to be of concern during a sluggish economy, clinic owners may even find their services are in competition with a patient’s choice to have a manicure, see a movie, buy a golf membership, or splurge on a bowl of ice cream. A good PT understands management of physical resources, and how to help patients meet their goals. Leveraging this understanding can make the potential patient’s disposable income decision more clear.
To help battle expanding costs and dwindling reimbursement, many larger, multiple-practice providers set up offices in strip malls and offer therapy with minimally equipped clinics. Forward-thinking physical therapists armed with courage to outfit their clinics with specialty equipment, combined with staff buy-in to customer service procedures and proper management of specialty equipment, will prosper during these times.
As PTs, we are in the business of managing and guiding our patients to higher levels of performance and function, all while utilizing every resource available to achieve performance goals. Those who do not embrace this strategy may stand to lose clients to their competition. By utilizing specialty equipment that helps patients meet their performance goals, PTs can create satisfied customers who enthusiastically endorse their practices for life. RM
Robert Babb, PT, MBA, is founder and president of the Physical Therapy & Wellness Institute in eastern Pennsylvania, a practice that employs eight full-time physical therapists. Babb earned an MBA from Desales University, and has lectured about business management at the APTA Private Practice Section conference. Babb is a licensed physical therapist with 26 years of experience helping individuals with acute and chronic, work-related, and sports injuries. For more information, contact [email protected].