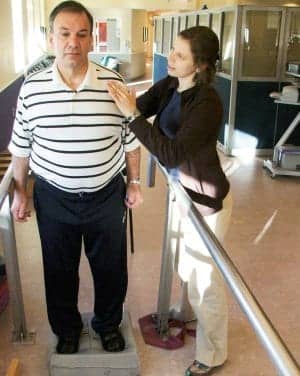
A comprehensive Wellness Program that incorporates all of the components of exercise and provides a social outlet for seniors can be successful in helping them remain healthy both physically and cognitively. Photo by Kerry O’Connor
One in every three people aged 65 years and older will fall. Falls are the leading cause of accidental death among seniors, accounting for more hospital admissions and emergency department visits than any other cause.1 Because of this, prevention of falls has been a main focus of physical therapy programs, but access to skilled therapy services is time limited. Fall prevention needs to be an ongoing focus as people age.
A community-based wellness program is an affordable way for seniors to participate in structured exercise programs that emphasizes fall prevention and balance training. Over the long term, this may help seniors remain in their homes and close to existing social networks, resulting in a better quality of life.
Age-related changes in humans occur throughout various systems in the body, such as changes in the cardiovascular and musculoskeletal systems that affect a geriatric person’s ability to exercise and maintain a healthy lifestyle. The maximal rate of oxygen consumption (Vo2 max) also declines as the aging process continues.2 It is advantageous for seniors to remain active because the Vo2 max can improve with activity and exercise. Pulmonary capacity, too, decreases with age due to lack of elasticity of lung tissue. A decrease in thoracic flexibility and kyphosis contribute to an inability of the rib cage to expand to its fullest potential. This can lead to a decrease in vital capacity.
As the body ages, skeletal muscle begins to decline where there is a loss of muscle mass and a loss of type II or fast twitch muscle fibers.2 Progressive denervation causes a decrease in the response rate for an elderly person receiving any perturbation, leading to an increased risk of falls. Because the response to external stimuli is greatly reduced, the likelihood of falls increases with age. At the intervertebral disc level, there is less water content in the disc material and this can lead to pain, loss of mobility, and loss of physical function.
WELLNESS AND FALL PREVENTION PROGRAMS
Health problems in older adults including osteoarthritis, cardiovascular disease, and diabetes contribute to a decrease in mobility and physical function. The goal of exercise is to break through barriers these diseases can cause and instill a sense of motivation in older adults. An appropriate wellness and prevention program for seniors begins with a multifactorial screening that includes history of falls, medication review, gait/balance assessment, visual acuity, muscle strength and range of motion, and environmental hazards.
Questioning the senior client about recent falls needs to be specific as falls are underreported to health care professionals. Seniors deny falling because it is a reminder of increasing frailty. Another reason falls are underreported is that seniors only consider a fall to the ground as an actual fall. A “near miss” or loss of balance into a strategically placed piece of furniture does not register in their minds as an actual fall. Clinicians should ask about loss of balance or unsteadiness to get a more accurate depiction of how the client is performing functionally at home and in the community. Once an individual has had a fall, the fear of falling again leads to a lack of confidence and often a self-imposed limit on activities, creating a cycle of further loss of strength and function. A comprehensive screen of clients in a wellness program should include a list of medications. Most seniors are taking at least four different prescription medications and another two over-the-counter medications.3 Physicians may not be aware of over-the-counter medications being taken. Age-related changes in the liver and kidney affect how medications are metabolized and excreted in the elderly. Medication, therefore, may remain in the system longer and in higher concentrations. Even at an appropriate dose, medication side effects contribute to falls risk. Commonly prescribed medications have primary side effects of hypotension, confusion, dizziness, fatigue, weakness, and delayed reaction time. Medication classes of antihypertensives, sedatives/hypnotics, antidepressants, and benzodiazepines have been found to increase falls risk.4
BALANCE TRAINING
Balance is maintained using visual, vestibular, and somatosensory systems, all of which change with age. Visual acuity diminishes, and use of bifocals can affect depth perception. In the vestibular system, there is less hair in the semicircular canals with increased age, decreasing the ability to sense changes in movement. Peripheral neuropathy is also common among the elderly, so there is diminished or conflicting information entering the brain that can be processed to maintain balance. Balance can improve with training, but the training needs to include static and dynamic activities as well as task-specific functional training. Static exercises include reaching while decreasing the base of support to progress the exercise. Dynamic activities include turning and stepping. Task-specific functional training incorporates dual task training such as walking while carrying an object.
HOME MODIFCIATION
Along with balance training, modification to the home to eliminate hazards must be addressed. The home is the primary location of nonfatal, unintentional falls, according to American Physical Therapy Association spokesperson Patrice Winter, PT, MPT, MS.5 Hazards include loose carpet and rugs, clutter, and poor lighting. Showers and bathtubs without grab bars and skid mats on the floor pose a great risk for falling. Stairs also pose a hazard in the home. For those with restricted mobility, the use of a stair lift can reduce the risk and lessen the burden on caregivers as well. Older adults are often reluctant to change their living conditions to ensure safety. They are comfortable in their domiciles and don’t always anticipate the consequences that hazards can cause. In one study, modification to the home was found to reduce the rate of falls more than a strength and balance program for seniors who had visual impairment.6
Developing a program for fall prevention incorporates several more components including strengthening, stretching, and aerobic activity.
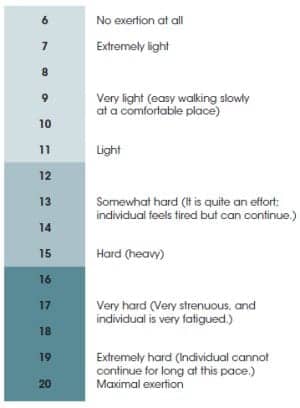

TABLE 1. Rate of Perceived Exertion
Muscle requires overload to become stronger. The starting point for strengthening exercises should be 60% to 80% of the person’s 1 repetition maximum (1RM), which is the ability to lift or perform a movement one time before muscle fatigue prevents lifting of the load or performing the movement through the full range of motion. Strengthening exercises should range from 10 repetitions to 15 repetitions. Rate of perceived exertion (RPE) is used to determine if the intensity is adequate. A laminated copy of the RPE scale in Table 1 can be shown to the client making a goal to work at an RPE of 12 to 13 with greater strength benefits being achieved if the client can work at an RPE of 15 to 17.7 Weight-bearing exercise is important for clients with osteoporosis to help rebuild or maintain bone mass. Strength training should be done 2 to 3 times/week with rest of 24 hours to 48 hours between exercising the same muscle group. Days may be alternated exercising lower extremity muscle groups and trunk/core muscles. Strengthening can be accomplished with free weights or resistance bands with weight machines. Equipment that allows the setup of multiple muscle groups provides the most versatility, especially in limited space. Many available options utilize weights or resistance bands. Equipment with a removable bench allows access for an individual in a wheelchair or scooter.
Stretching is also a key part of the exercise regimen. Stretching should be performed following a brief warm-up and/or after strengthening to avoid muscle tears. The focus of stretching should be the heel cords, hamstrings, and hip flexors. Flexibility exercises should be performed 2 to 3 times/week and stretches held for 10 seconds to 30 seconds. Education about proper hold of the stretch without bouncing to prevent injury should be provided.
Aerobic activity is an integral part of an overall fitness program. Aerobic exercise should be performed 3 days to 5 days/week and can be accomplished with brisk walking, swimming, biking, or water exercise. Recumbent bikes or recumbent cross trainers are good options for clients of all abilities as they allow a low impact aerobic workout that can be made more challenging by adding resistance.
Choosing the correct intensity of exercise for seniors can be challenging. The clients participating in a wellness/prevention program should be educated about the following guidelines. Exercise should not:
- Make an individual’s joints sore or painful for more than 2 hours after activity
- Make an individual feel nauseous
- Make an individual feel extremely fatigued at the end of the day9
Motivation is key to increasing participation of seniors in fitness programs. The AARP, in partnership with the Robert Wood Johnson Foundation, conducted extensive research from 1999 to 2003 about health knowledge, attitudes, and behaviors of people age 50 years and older.10 The study revealed several themes that may assist in the development of fitness programs for the geriatric population. Older adults are motivated by images they can relate to, not to a super athlete, who may cause them to feel insecure and therefore discouraged from participating in a fitness program. According to the report, seniors are looking for guidance about exercising safely, staying motivated, and setting achievable goals. Words have meaning. AARP researchers noted the term “physical activity” was more appealing than “physical exercise.” Per the report, the respondents felt that exercise was “work, associated with exertion and sweating,” and “physical activity” was things they must do anyway as part of life.
In an effort to entice older adults to initiate and adhere to a fitness program, health professions should consider the following suggestions outlined in the National Council on Aging.
- Create messages that associate fitness and the ability to remain independent while recognizing the changes that occur with aging.
- Recognize the influence of negative stereotypes and media images on perceived health status.11
- Work with older adults to set goals that are practical, motivating, and individualized.
- Demonstrating personal relevance is crucial in maintaining exercise adherence for any population, not just older adults.
- Establishing appropriate environments that are well lit and accessible are important in motivating older adults to exercise.12
- Supervision and instruction on all equipment will help to increase self-confidence and decrease the risk of injury and postexercise soreness.
- Social support and encouragement from other participants and the fitness staff are fundamental in overcoming challenges and keeping older adults interested and engaged, as does socialization. Active adults who participate in regular physical activity identify the social aspect of exercising as a motivator. The draw to exercise in this age group is often companionship. Social support helps to ensure greater level of self-efficacy and improved long-term benefits.13
A comprehensive Wellness Program that incorporates all of the components of exercise and provides a social outlet for seniors can be successful in helping seniors remain healthy both physically and cognitively. The Baby Boomer generation is looking forward to healthy years as they enter retirement. This generation of seniors recognizes the health benefits of physical activity. It is incumbent upon the providers of such services to educate these consumers so they can make good choices. Integration of the clinical, environmental, and psychosocial components of aging will promote adherence and a successful program. While the short-term benefits are easily recognized, the long-term benefits of less governmental expenditure cannot be emphasized enough.
KEEPING HIM ON HIS TOES
Physical exercise combined with balance and strength training can prevent older adults from falling, enhancing their ability to maintain independence in their own homes—in their own lives—without fear of injury or the need to live in an expensive nursing home.
Vince would be the first to agree. Recently, the 58-year-old suffered three strokes and was living in a nursing home after receiving inpatient care. In February 2011, he began outpatient rehabilitation therapy at Magee Rehabilitation Hospital. Shortly after, Vince suffered a fall while attending church in his community and needed care.
Nine months later, Vince was doing well enough to transition to the Health & Wellness Program at Magee where he followed a schedule of activities and exercises designed specifically for him by his therapists, which included strengthening and balance activities. By the end of the ninth month, Vince was back in his own home with his wife, climbing the stairs several times a day, driving his car, and going to church.
Vince still participates in Magee’s Health & Wellness Program, keeping his muscles strong and his balancing skills sharp. He can use the exercise equipment on his own, which increases his sense of independence.
“The Health & Wellness Program is perfect,” said Vince in between activities at Magee’s new Health & Wellness Center at its Riverfront facility. “I can come daily and focus on all of my different exercises. I do strengthening and balance exercises on my own, but in a safe environment.”
With his chance of falling decreased, everywhere Vince goes can be a safer environment.
Rose Battiato, PT, MPT, is the Director of Outpatient Development and Programs at Magee Rehab Hospital in Philadelphia, Pa. Battiato has been at Magee Rehab for 20 years. She has a Masters in Physical Therapy from Temple University in Philadephia. Battiato specializes in geriatric and neurological physical therapy. She has also served as an instructor for physical therapy programs.
Carol Owens, PT, GCS, is the Therapy Manager at Magee Riverfront in Philadelphia. Owens has 21 years of experience as a physical therapist working in neurologic rehabilitation. She received a specialist certification in geriatrics from the American Board of Physical Therapy Specialties in 1999, and has recently helped launch a Wellness Program for people of all ages and abilities at Magee Riverfront. For more information, contact
REFERENCES
- Falls Among Older Adults: An Overview. Available at: www.cdc.gov. Accessed November 22, 2011.
- Decker AM, Regan G, Thompson CR. Prevention practice for older adults. In: CR Thompson, ed. Prevention Practice—A Physical Therapist’s Guide to Health, Fitness and Wellness. Thorofare, NJ: SLACK Inc; 2007:115-128.
- Beers M. Aging as a risk factor for medication related problems. Modern Medicine. 1999. Available at: www.modernmedicine.com. Accessed November 22, 2011.
- Woolcott J. Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch Intern Med. 1999;169:1952-1960.
- Older Adults Can Reduce Risk of Falls with Physical Therapist-led Programs. 2011. Available at: www.apta.org/Media/Releases/Consumer/2011/9/23. Accessed November 23, 2011.
- Campbell AJ. Randomised controlled trial of prevention of falls in people aged ≥75 with severe visual impairment: the VIP trial. BMJ. 2005;331(7520):817.
- Avers DB, Brown M. White paper: strength training for the older adult. J Geriatr Phys Ther. 2009;32:148-152, 158.
- Borg GV. Psychological basis of perceived exertion. Medicine and Science in Sports and Exercise. 1982;14:377-381.
- Guide to Safe and Effective Physical Activity and Exercise for the Aging Adult. Available at: www.geriatricspt.org. Accessed July 7, 2011.
- Synthesis of AARP Research in Physical Activity: 1999-2003. 2004; 1-15. Available at: www.research.aarp.org. Accessed November 22, 2011.
- Motivating Participants to Be More Physically Active. 2006. Available at: www.healthyagingprograms.org. Accessed November 21, 2011.
- Resnick B, Ory M. Motivating frail older adults to be physically active. Journal on Active Aging. March April 2006:41-46.
- Costello E, Kafchinski M, Vrazel J, Sullivan P. Motivators, barriers, and beliefs regarding physical activity in an older adult population. J Geriatr Phys Ther. 2011;34:138-147.





