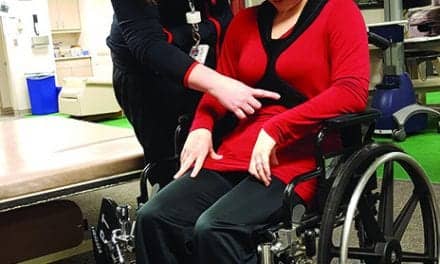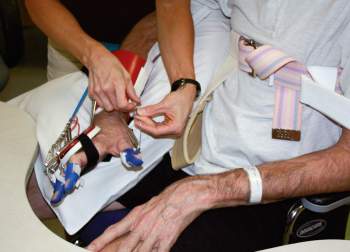
A highly customized dynamic wrist/hand orthosis, designed to accommodate the needs of the neurological population, can help pave the road to successful upper extremity recovery.
Treating the neurologically impaired individual brings many challenges to the client and therapist. There are numerous theories, therapeutic interventions, and approaches to maximize an individual’s function. As an occupational therapist, working with an individual affected by upper extremity weakness (ranging from flaccidity to hypertonicity) challenges the clinician’s knowledge, skills, and handling techniques in every treatment session. Our ultimate goal or sense of achievement is attained when the patient has gained strength, control, and functional use of the arm and hand. At the point in recovery when an individual spontaneously incorporates an extremity into a unilateral or bilateral task and is successful in their attempt to interact with the world, this becomes one of the highest achievements we can strive for in therapy. The road to recovery is long and arduous.
Typically, in the stroke (cerebrovascular accident or CVA) or brain injury population, the ability to regain use and function of a lower extremity exceeds the progress noted in the upper extremity. So, how do we help clients reach their upper extremity goals? I have worked with the neurological population for more than 22 years within the rehabilitation setting (inpatient/outpatient) and have seen or used many of the modalities/devices that are available in the market. A device that I believe is important to mention is the “dynamic wrist/hand orthosis” specifically designed for the neurological population. This splint provides optimal positioning of the wrist and fingers through a custom forearm, dorsal hand piece splint and a set of springs, pulleys, and digit caps that are placed on the fingers (the caps cover the distal interphalangeal joints of each finger). The splint can be used throughout an individual’s entire recovery (from flaccid through the development of tone). To use the splint, the patient must exhibit minimum movement criteria in the weaker extremity: they must demonstrate 15 degrees of active shoulder movement and 15 degrees of active elbow movement, passively move the wrist into at least 15 degrees of wrist extension, and block the metacarpophalangeal joints of the fingers. The patient also must be able to volitionally flex the fingers one-fourth range. The splint can be incorporated into a client’s treatment protocol at any time in the recovery phase (in the acute stage or years after injury or date of onset).
The components of the splint allow the wrist to be positioned in 15 to 30 degrees of extension, and all digits (including the thumb) are extended so the resting position of the wrist/fingers within the splint allows for optimal grasp. All distal control is managed by the splint so this allows the therapist to facilitate proximally to promote forward reach patterns, hand to mouth motions, etc, while the fingers are able to be controlled and move around a large object (usually a 4-inch diameter ball). They can incorporate the use of neuromuscular electrical stimulation (NES) to proximal muscle groups while guiding and facilitating. An additional benefit of this dynamic splint allows for the use of NES at the shoulder or elbow while engaging the hand into gross grasp and release exercises. One of the most positive benefits I have noticed using this splint over the last 7 years occurs when a patient is in the splint and their attention becomes focused on the weaker extremity and the goal that is presented to them (ie, grasping a ball, moving the arm, releasing the ball).
The outcomes are truly based on the commitment. I have found that family/caregiver support is crucial in carrying over the extensive arm training drills required in the home. The splint can be difficult to don, and adjustments are commonly required to maintain optimal positioning, as the alignment of each digit and line of pull through the bead line is crucial for success. The home program encourages high repetition/mass practice of a variety of prescribed arm and hand movements. The client must maintain a record of the amount of time in the splint, movements performed, and number of repetitions completed. The standard recommendation is to perform two 45-minute sessions in the home. I have found that most clients are able to get into the splint once per day, so I encourage performing the prescribed program to the point of fatigue and/or extending the session to 60 minutes.
Forced use and attention to the weakened extremity are capitalized on with each repetition. New motor pathways (neuroplasticity) are being developed with each repetition. There is an amazing moment when the patient moves the hand for the very first time and that moment builds the “buy in” to use the splint as indicated. We have found that clients who meet the minimal movement criteria, have a strong support system, and do not demonstrate hypertonicity, soft tissue tightness, and/or significant visual or cognitive deficits are most successful in using this dynamic splint and gaining volitional movement.
CASE STUDY

A dynamic splint can bolster the blended use of neuromuscular electrical stimulation (NES) at the elbow or shoulder with gross grasp and release exercises.
W.S., a 58-year-old male, was admitted to the hospital on December 19, 2007, after noticing a change in his balance and slurred speech. The CT scan showed left intraparenchymal hemorrhage, and the patient had right-sided weakness. In acute care, he presented with 0/5 manual muscle strength, absent sensation, and a flaccid right upper extremity. He required moderate to maximal assistance with his basic activities of daily living (BADLs) and demonstrated inattention to his right side. During his stay in acute care and acute rehab, W.S. participated in various treatment techniques and use of modalities for the right upper extremity such as Neuro-Developmental Treatment (NDT), NES, proprioceptive neuromuscular facilitation patterns, and vibration/icing, self, and passive ROM exercises in gravity-eliminated planes. On January 8, he demonstrated trace to poor muscle contraction for nearly all proximal to distal muscle groups including even basic shoulder elevation, scapular depression, and elbow flexion. He was fitted with a dynamic wrist/hand orthosis. During the first session using this device, patient was able to grasp and release 12 balls (~4 inch diameter) and place them in a 4-inch box in a 30-minute treatment session. By the time he was discharged from inpatient rehab, W.S. was modified independent for all self-care skills excluding shower and shower transfer. In regard to the right upper extremity, he grasped and released objects from a horizontal surface and transitioned them to a vertical holder with his right hand pronated with moderate assistance. Every movement continued to require assist/facilitation from the therapist during the inpatient therapy stay.
He soon transitioned to outpatient therapy after being discharged home. At the time of initial evaluation, W.S. was completing all BADLs at a modified independent level and had begun making simple microwavable meals, but was completing all functional tasks with the left upper extremity. He demonstrated beginning movements in his right arm in a flexor synergistic pattern (shoulder elevation, abduction, elbow, and wrist and finger flexion). He demonstrated elbow flexion (0-110°) but could not reach his mouth, and showed a forward reach pattern with moderate facilitation from the therapist. The patient continued daily sessions of using the dynamic wrist/hand orthosis, increasing the amount of time in the splint as well as the number of repetitions of the arm training drills. The patient completed basic grasp/release exercises with the number of repetitions continually increasing as the movement patterns became easier. He also progressed to tolerating and completing the full amount of time prescribed/desired with this device (two 45-minute sessions daily).
With this consistent use, the patient was able to report several functional examples of improvement in the right upper extremity on a weekly basis. For example, the patient was very proud and excited when he was able to use his right hand to hold his coat while manipulating the zipper or ripping a paper towel and eating yogurt with his right hand. With the dynamic wrist/hand orthosis donned—and having increased his ease with grasp/release exercises—proximal AROM and strengthening were incorporated into treatment sessions. The “targets” for the patient to reach were consistently increased to challenge his skills. The patient progressed significantly by demonstrating AROM for the right shoulder flexion to ~150-160 degrees at discharge, and reporting being able to change a light bulb at home. Proudly, he stated, “My sister hasn’t seen me since January, and she can’t believe the change in my arm,” and “My brother couldn’t believe how high I was raising my arm.” He began using his right arm again in various functional tasks including being able to button, use a zipper, and don a belt. By the end of his outpatient therapy, the patient could cut peppers, onions, and steak during meal preparation and perform eating activities with the right hand.
He progressed to begin light strengthening and AROM using light weights, wall pushups, an upper body ergometer, and Baltimore Therapeutic Equipment, as well as hand strengthening (grip/pinch exercises). The patient progressed to 43# grip strength from 10# on initial evaluation (February 1 to April 4, 2008, overall ~8 weeks of therapy with patient not attending his last week due to illness). He was incorporating the right hand in all self-care tasks and activities of daily living, was continually working on his handwriting and typing skills, and was beginning to practice his golf swing. The patient committed to using the wrist/hand orthosis daily and was focused on using his right hand again. Despite some frustration along the way as any patient recovering from a CVA may experience, he was able to follow through with all arm training drills beginning with basic grasp/release exercises, up to high level exercises involving shoulder flexion, abduction, circumduction, elbow flexion/extension, and supination/pronation. He began to see the functional change in his arm, motivating him to continue using the device in therapy. A second time throughout his day and as instructed, he continued utilizing forced use practices with the right hand outside of therapy sessions. The patient could not believe the tasks he was able to complete by the middle of February since his right upper extremity was flaccid 1 month prior.
We continued to watch this patient’s progress and excitement through two more months of therapy and use of the device. When we compared formal measurements (manual muscle testing, AROM, and grip/pinch tests) and functional gains (most important to everyone, especially the patient) from using the wrist/hand orthosis from admission to discharge, it truly made the commitment to using this device priceless. He functionally returned to using his right upper extremity in ways he never imagined shortly after being hospitalized and traumatized from having a stroke as a middle-aged male. We watched as he readied himself to continue pursuing the many life goals that this active, highly accomplished man had for himself!
Karen Hookstadt, OTR, CEES, has 23 years of experience in the field and holds certifications in brain injury, NDT, and ergonomics. Hookstadt works at Spalding Rehabilitation Hospital in Aurora, Colo, and specializes in stroke and brain injury.
Meg Filarowicz, OTR, is certified in brain injury and has 12 years of experience. Filarowicz works at Spalding Rehabilitation Hospital and specializes in stroke, brain injury, adolescent population, and work site evaluations.
Jen Rieks, OTR, is certified in brain injury and NDT. Rieks has 9 years of experience and specializes in stroke and brain injury. She works at Spalding Rehabilitation Hospital and serves as coordinator of its Brain Injury Support Group. For more information, contact .