Coauthor Jessica M. Caggiano, DPT, provides mechanical pitching instruction
Over the years, American youth athletics have undergone a fundamental shift. The original intent of a fun, extracurricular activity has now been rapidly converted to a high-pressure feeder system for collegiate and professional athletic programs. With this new youth sport paradigm come the heightened physical expectations and intense training schedules that await these preadolescent and adolescent athletes.
Long seasons, multileague enrollment, multigame-per-week schedules, and a repetitive overhand throwing motion put youth baseball players at high risk for elbow and shoulder problems.1,2 The throwing arm of a youth baseball player is placed under a tremendous amount of stress. Age occurrence of epiphyseal closure shows widespread range at both the humerus, 14 to 20 years old, and elbow, 10 to 17 years old.3 With bone maturation of most of these players still occurring, repetitive stress injuries and soreness at and around the epiphyseal plates are common. The extreme valgus stress on the medial elbow with throwing puts not only pitchers at an increased risk of shoulder and elbow soreness (58%), but catchers (63%) and fielders (47%) as well.4 Youth baseball players noted in recent literature span the ages of 8 to 17 years old1,5-8 and show increased risk of arm injury as age, height, and weight increased.2 Despite youth league restriction efforts with pitch count limits and breaking pitch age requirements, increased rates of adolescent injury are still being seen.3,7,9 Olsen et al7 reported a direct comparison between adolescent pitchers who had elbow/shoulder surgery and those who did not. Pitchers who averaged more than 80 pitches per appearance were nearly four times more likely to require surgery. Those who pitched competitively for >8 months were five times more likely to require surgery. Clinically, we are seeing more and more of these pitchers present in our practices with complaints of shoulder and elbow pain. Although many of these patients may go on to develop further soft tissue lesions, we are seeing a growing number of these throwers present with common diagnoses of “Little League shoulder,” “Little League elbow,” and posterior impingement. We must be prepared to treat these throwers, but, more importantly, to educate them to prevent future injury.
LITTLE LEAGUE SHOULDER/HUMERAL STRESS FRACTURE
This injury on x-ray can show up as a widening of the proximal humeral physis. This gapping of the growth plate is caused by repetitive rotational torque at that humeral physis. Little League shoulder typically presents as proximal humerus pain and arm fatigue while throwing.3,6,8 Patients may present with lateral shoulder palpation tenderness; however, most patients will present without reproduction of pain during the physical exam.
LITTLE LEAGUE ELBOW/MEDIAL EPICONDYLE STRESS FRACTURE
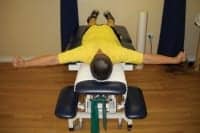
In prone position, scapular retraction, horizontal abduction with external rotation.
This injury on x-ray can also show up as a widening of the growth plate, but at the medial epicondyle physis. While shoulder internal rotation provides the counteractive varus force at the proximal kinetic chain, the ulnar collateral ligament provides this needed counteractive varus force at the elbow. Similar to Little League shoulder, with decreased posterior shoulder strength, posterior shoulder capsule tightness, decreased shoulder internal rotation ROM, and poor throwing mechanics, medial elbow overuse injury can occur. All of these deficits contribute to a decreased varus counterforce at the elbow, causing greater strain at the medial epicondyle.4,6-8,10,11 Little League elbow typically presents as medial elbow pain, arm fatigue, and decreased ball control while throwing. Patients may present with medial elbow tenderness.3 Similar to the physis injury in the shoulder, these patients often do not report pain with clinical exam.
POSTERIOR IMPINGEMENT

Scapular retraction, horizontal abduction on Pilates reformer.
This injury differs from the common subacromial impingement often seen in the average outpatient adult population. Subacromial impingement occurs in the anterosuperior aspect of the shoulder with the rotator cuff being pinched between the humeral head and acromion of the scapula.5 With posterior impingement, the location of the impingement is in the posterosuperior aspect of the shoulder. A pinching occurs between the humeral head and posterior glenoid rim of the supraspinatus tendon. In some instances, the infraspinatus tendon will be impinged as well.6 Increased external rotation range and decreased rotator cuff strength can cause an amplified aggravation from this posterior pinching due to the repetitive nature of the baseball player’s throw.8,12 These patients typically report a “dead” arm when throwing and pain in the back of the shoulder, and often report a loss of velocity. Clinically, they may present with posterior shoulder palpation tenderness; however, as we will discuss later, ROM considerations are key to these patients.
All three of these injuries in adolescent baseball players will typically show similar preexisting patterns. Decreased shoulder internal rotation, increased shoulder external rotation, and decreased rotator cuff and posterior shoulder/back musculature strength tend to be present in baseball players with elbow and/or shoulder pain.8
KEYS TO TREATING THE ADOLESCENT THROWING ATHLETE
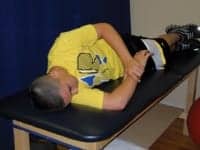
Sidelying internal rotation stretch, “sleeper stretch,” can be used in a home exercise program.
Clinically, these patients typically present with significant internal rotation deficit, poor scapulothoracic control, mechanical faults during throwing, and significant overuse. It is essential for physical therapists who are treating this population to understand the concept of glenohumeral internal rotation deficit (GIRD). Due to the repeated overhead throwing motion (most common in pitchers), an adaptive range of motion change occurs in the throwing shoulder. These patients will present with increased external rotation and a loss of internal rotation, as compared to the nondominant side. The pitching motion often forces the throwing shoulder into >185°, therefore the forces often cause retroversion or rotation of the humerus at the growth plate. Over time, the throwing shoulder will anatomically gain external rotation and lose internal rotation from these osseous changes. However, recent studies have shown that this loss of internal rotation is often associated with increased shoulder and elbow impairments.10,12,13
ADDRESSING THE GIRD
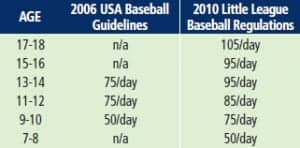
Table 1. Daily pitch recommendations
The key to addressing the ROM considerations is recognizing this shift in ROM by measuring the total motion on both the dominant and nondominant shoulders, often referred to as the total motion concept.14 These patients may present with >20° loss of internal rotation. At this point, it must be determined if this is tightness in the posterior shoulder or an adaptive boney change. Addressing this posterior shoulder tightness is an essential component to getting the throwers back on the mound. This can be accomplished by providing the sidelying horizontal adduction stretch, stabilizing the scapula to the thorax and horizontally adducting until the patient feels the stretch in the posterior shoulder. Patients should also be instructed in the sidelying internal rotation stretch (see photo), which should be a key element in their home exercise program. Finally, this may also be accomplished by manually mobilizing the posterior glenohumeral joint and stretching it into internal rotation. At this point, we do not know what degree of GIRD will predispose a thrower to injury; however, recent studies indicate that keeping the GIRD <15° improves symptoms.10,12,13.
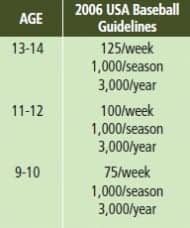
Table 2. Weekly-season-year pitch recommendations.
PROXIMAL STRENGTHENING OF THE THROWING ATHLETE
“The Thrower’s Ten” is a well-known, common list of exercises designed to address many of the muscles used for throwing. Although it can be argued that these exercises are important in the rehabilitation of the throwing athlete, we must first consider the essential component of proximal stability. An EMG study by Gowan et al15 highlighted the difference between professional and amateur pitchers as being amateurs primarily used their smaller rotator cuff muscles, while professionals used larger muscle groups to perform the same activity. We must address these larger muscle groups first, including the latissimus dorsi, pectoralis major, and scapular stabilizers. Strengthening these scapular stabilizers will be the foundation from which all smaller muscle groups can then work off of. Using the evidence from studies by Blackburn et al,16 Moseley et al,17 and Townsend et al,18 we have adapted our “Prone Program” to address the throwers’ scapular stabilizers: prone horizontal abduction with internal rotation, prone horizontal abduction with external rotation (see photo), prone scaption, and prone 90°/90° external rotation. This program should be initiated without weight to ensure appropriate exercise form. Once appropriate form is attained, these exercises should be progressed with dumbbells or cuff weights. This program can be further progressed to a more functional vertical position using elastic resistance or, even more challenging, a Pilates reformer (see photo). Once proximal stability is attained, these patients can move onto more traditional rotator cuff, deltoid, and wrist strengthening.
Advanced strengthening of these patients should address the stretch-shortening cycle offered by performing plyometric exercise for the internal rotators, external rotators, and scapular stabilizers. By working the active stretch of a muscle followed by its immediate shortening, it will train the muscle to work in a more functional nature. One of the key breakdown moments during the pitching motion is during the “late cocking” phase when the internal rotators change direction from eccentrically elongating to concentrically shortening to deliver the ball. Plyometric training will enhance the body’s ability to perform this action and will also help in training for fatigue. It is encouraged to initiate these plyometrics using larger (basketball)-size weighted balls for trunk rotation exercises and progressing distally with smaller hand-sized weighted balls or kettlebells.
PATHOMECHANICS

Table 3. Little League Baseball rest regulations.
The science of pathomechanics may be beyond the scope of this article; however, it is important to appreciate that extensive research from the American Sports Medicine Institute (ASMI)9 continues to educate us on the kinematic and kinetic implications of injury during the pitching motion. Fleisig et al19 hypothesized eight mechanisms that increase kinetic values and the risk of injury. These implications for injury are well highlighted by Fortenbaugh et al20 and offer the regularly treating clinician another tool to use while evaluating these patients. Most physical therapists do not have access to high-speed, three-dimensional analysis of their throwers like the researchers at ASMI, and picking up small mechanical alterations in a youth’s pitching motion with the naked eye is difficult. By using a standard camera that has video capability, we can detect some of these faulty mechanics by slowly reviewing the video. Small changes can often make the difference between a painful and pain-free delivery.
PITCH LIMIT EDUCATION
Many of the above impairments can be avoided by simply following recommended pitch volumes. The most important aspect to treating these patients is the education on recommended pitch counts and rest periods. Most adolescent pitchers are playing in multiple leagues with multiple coaches who are not aware of how much their pitchers are throwing elsewhere. ASMI has a current position statement that highlights both the 2010 Little League Pitching Limits as well as the 2006 USA Baseball Guidelines. (See Tables 1, 2, and 3.) These recommendations should be offered to each patient as well as their parents. Parents are the key to monitoring these limits.
Treating the adolescent thrower is a unique challenge to any physical therapist. It is essential to understand the common impairments associated with this population and the keys to returning them back to the field. Our key components to getting these players back on the mound are: understanding the unique ROM considerations of these athletes, addressing proximal stability, appreciating the pathomechanics associated with poor pitch mechanics, and finally, educating the parents and patients on pitch count recommendations. By addressing all of these keys components, our pitchers should be back on the mound in no time.
Michael J. Mullaney, DPT, is a research consultant at the Nicholas Institute of Sports Medicine and Athletic Trauma, New York, and the co-owner of Mullaney & Associates Physical Therapy LLC in Matawan, NJ. Jessica M. Caggiano, DPT, is a physical therapist at Mullaney & Associates Physical Therapy. For more information, contact .
REFERENCES
- Lyman S, Fleisig GS, Andrews JR, Osinski ED. Effect of pitch type, pitch count, and pitching mechanics on risk of elbow and shoulder pain in youth baseball pitchers. Am J Sports Med. 2002;30:463-468.
- Lyman S, Fleisig GS, Waterbor JW, et al. Longitudinal study of elbow and shoulder pain in youth baseball pitchers. Med Sci Sports Exerc. 2001;33:1803-1810.
- Ray TR. Youth baseball injuries: recognition, treatment, and prevention. Curr Sports Med Rep. 2010;9:294-8.
- Hang DW, Chao CM, Hang YS. A clinical and roentgenographic study of Little League elbow. Am J Sports Med. 2004;32:79-84.
- Bigliani LU, Levine WN. Current concepts review—subacromial impingement syndrome. J Bone Joint Surg Am. 1997;79:1854-68.
- Meister K, Day T, Horodyski M, Kaminski TW, Wasik MP, Tillman S. Rotational motion changes in the glenohumeral joint of the adolescent/Little League baseball player. Am J Sports Med. 2005;33:693-698.
- Olsen SJ, Fleisig GS, Dun S, Loftice J, Andrews JR. Risk factors for shoulder and elbow injuries in adolescent baseball pitchers. Am J Sports Med. 2006;34:905-912.
- Trakis JE, McHugh MP, Caracciolo PA, Busciacco L, Mullaney M, Nicholas SJ. Muscle strength and range of motion in adolescent pitchers with throwing-related pain. Am J Sports Med. 2008;36:2173-2178.
- American Sports Medicine Institute, Birmingham, Ala. Available at: [removed]www.asmi.org/asmiweb/usabaseball.htm[/removed]. Accessed September 2010.
- Dines JS, Frank JB, Akerman M, Yocum LA. Glenohumeral internal rotation deficits in baseball players with ulnar collateral ligament insufficiency. Am J Sports Med. 2009;37:566-570.
- Sabick MB, Kim YK, Torry MR, Keirns MA, Hawkins RJ. Biomechanics of the shoulder in youth baseball pitchers: implications for the development of proximal humeral epiphysiolysis and humeral retrotorsion. Am J Sports Med. 2005;33:1716-1712.
- Myers JB, Laudner KG, Pasquale MR, Bradley JP, Lephart SM. Glenohumeral range of motion deficits and posterior shoulder tightness in throwers with pathologic internal impingement. Am J Sports Med. 2006;34:1-6.
- Tyler TF, Nicholas SJ, Lee SJ, Mullaney MJ, McHugh MP. Correction of posterior shoulder tightness is associated with symptom resolution in patients with internal impingement. Am J Sports Med. 2010;38:114-119.
- Wilk KE, Meister K, Andrews JR. Current concepts in the rehabilitation of the overhead throwing athlete. Am J Sports Med. 2002;30:136-151.
- Gowan ID, Jobe FW, Tibone JE, Perry J, Moynes DR. A comparative electromyographic analysis of the shoulder during pitching: professional versus amateur pitchers. Am J Sports Med. 1987;15:586-590.
- Blackburn TA, McLeod WD, White B, Wofford L. EMG analysis of posterior rotator cuff exercises. Athletic Training. 1990;25(1):40-45.
- Moseley B, Jobe FW, Pink M, Perry J, Tibone J. EMG analysis of the scapular muscles during a shoulder rehabilitation program. Am J Sports Med. 1992;20:128-134.
- Townsend H, Jobe FW, Pink M, Perry J. Electromyographic analysis of the glenohumeral muscles during a baseball rehabilitation program. Am J Sports Med. 1991;19:264-272.
- Fleisig GS. The Biomechanics of Baseball Pitching. Birmingham, Ala: University of Alabama; 1994.
- Fortenbaugh D, Fleisig GS, Andrews JR. Baseball pitching biomechanics in relation to injury risk and performance. Sports Health. July/Aug 2009:314-320.
A Gentle Shock to the System
Using FES technology in rehabilitation of the upper extremities in patients who have suffered major neurological events.
By Judy Peck, PTA, CBIS, and Tim Burkhart, MS, OTR/L, CBIS, MBA
While traditional therapy tools have proven useful in helping patients make measurable gains in their independent mobility, new innovations are advancing the ways in which we can treat our patients and help them to regain mobility. One such advance is functional electrical stimulation (FES), a rehabilitation technique that uses a form of electrical stimulation to stimulate nerves in order to create muscle contractions. By combining FES and repetitive, task-specific, functional movement patterns, therapists are able to quickly create the optimal treatment session for individual patients and obtain immediate results.
A Rehab Course with Upper Extremity Electrical Stimulation
Patient A is a teenage boy who suffered a cerebrovascular accident (CVA) and was very active in both school and sports. At the initial outpatient evaluation, he presented with 0/5 muscle strength in the left upper extremity for shoulder flexion, elbow extension, and digit flexion/extension. His left arm was paralyzed, and Patient A could not complete daily activities requiring use of this limb. Initially, the primary focus of this patient’s therapy was on stabilizing his left arm, starting at the shoulder and scapular region. FES was implemented in the clinic and at home with an EMPI 300PV unit for direct application of stimulation to the supraspinatous, middle/posterior deltoids, and parascapular muscles. The goal was to attain decreased subluxation at the shoulder and decreased scapular winging. In accomplishing this, a solid foundation was created so that his arm could move with increased quality at the shoulder, elbow, and wrist.
A key point to consider when incorporating FES into therapy is that FES has more value when applied in conjunction with functional tasks. As this patient was unable to participate in contact sports, golf was incorporated to functionally exercise his muscles. As he practiced, FES was applied to his triceps to promote a straight leading arm during the golf swing.
FES was also used to apply grip pressure to his left digit flexors. Applying stimulation during functional patterned movements, along with guidance from his therapist and high levels of repetition, helped to yield amazing recovery of movement in his left arm. This patient was once again able to engage in a wide variety of patterned movements, including picking up and releasing a golf ball, using his own motor control with the adjunct of the FES to complete the motions. Prior to therapy with FES, this would not have been possible.
The NESS H200 Hand Rehabilitation System is designed to help facilitate movement in the hand.
FES Using Neuroprosthetic Devices
As patients progress in motor recovery, flexor tone or spasticity often develops. This causes the hand to clench shut in a fist-like pattern. Innovations in the field of FES have resulted in advancements to address these issues, such as neuroprosthetic devices.
At Total Rehab Care, we use the NESS H200® Hand Rehabilitation System, which is designed to help facilitate movement in the hand. It fits on the arm like a clamshell splint and has customized pads to deliver stimulation to the digit flexors and extensors on two separate channels. FES is delivered through a pulsed mode to the muscles that open the hand while the fingers are stretched open, and can significantly reduce spasticity. Patient A was successful both in the clinic and at home with the use of this technology.
FES and Motor Support Cycling
In addition to the NESS H200, Patient A’s therapy also included use of the RT300 upper body ergometer, which combines dynamic motor support and FES. The RT300 cycle assists the paretic limb through reciprocal movements with each individualized, tailored session by stimulating up to six muscle groups to augment motor recovery.
Seeing Clinical Improvements and Lifestyle Changes
After 15 months of therapy and home exercise programs, Patient A currently demonstrates shoulder flexion, elbow extension, and digit flexion/extension strength of 4/5. Although he had never played golf in his life prior to therapy, he is now a fan of the sport. In fact, combining his intense rehabilitation along with regular golf lessons, this patient made his high school golf team and competed in the first golf match of the school year.
Conclusion
The application of FES can reduce recovery time, enhance movement pattern, and eventually increase muscle strength and mass. FES for upper extremities offers patients exceptional measured functional gains and has allowed therapists to enhance traditional approaches.
Judy Peck, PTA, CBIS, is a physical therapist assistant, and Tim Burkhart, MS, OTR/L, CBIS, MBA, is an occupational therapist at Total Rehab Care of Washington County Hospital in Hagerstown, Md.
Bibliography
- Cycling induced by functional electrical stimulation improves the muscular strength and the motor control of individuals with post acute stroke. Eur J Phys Rehabil Med. 2008;44(2):159-167.
- Foley N, Teasell R, Jutai J, Bhogai S, Kruger E. Evidence-Based Review of Stroke Rehabilitation (EBRSR). London, Ontario; September 2009.
- The effect of the NESS L300 neuroprosthesis on gait stability and symmetry [abstract]. J Neurol Phys Ther. 2006;30(4):195-200. Included in CSM 2007 Platform Presentations.
- Prevention of shoulder subluxation after stroke with electrical stimulation. Stroke. 1999;30:963-968.
- Upper limb electrical stimulation exercises. Salisbury FES Newsletter. January 2002.