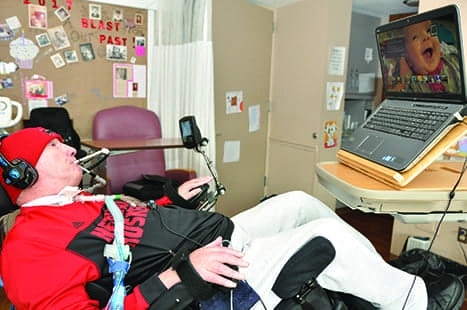
Larry Schroetlin uses speech recognition software to control his computer. The program enables Larry to use his voice to connect with email, search his computer, play games and more. Schroetlin also uses Bluetooth and infrared technology through sip and puff control to operate a smartphone and entertainment devices such as TV, DVD, and cable system controls.
by Wade Lucas, PT, DPT, ATP
Madonna Rehabilitation Hospitals is one of the nation’s leading providers of medical and physical rehabilitation for adults and children. Madonna’s highly trained staff specializes in spinal cord injury, traumatic brain injury, stroke, complex medical, other neurological conditions, and pediatric rehabilitation. In fiscal year 2016, Madonna Rehabilitation Hospitals served patients from 17 US states, including Alabama, Arizona, Colorado, Iowa, Illinois, Kansas, Louisiana, Missouri, Nebraska, New York, North Dakota, Oklahoma, Oregon, South Dakota, Texas, Utah, and Wyoming. Patients rely on Madonna’s expertise to achieve maximal function and independence. A comprehensive, complex rehabilitation technology evaluation is crucial to the care provided to many who seek treatment at the facility, and at the core of this evaluation is the participation of a multidisciplinary rehabilitation team.
Multidiscipline for Maximum Results
Madonna implements and values a systematic, multidisciplinary team approach to meet the patient’s care needs and promote functional independence with the use of complex rehabilitation technology. The interdisciplinary team consists of physician services, rehabilitative nursing, physical therapy, occupational therapy, speech/language pathology, assistive technology specialists, rehabilitation engineer, wheelchair technician, and community-based durable medical equipment (DME) suppliers. The rehab team also relies on equipment manufacturers for continuous training on advancements and capabilities of the complex rehabilitation technology.
The Madonna physicians are the medical coordinators of the rehabilitation process. They initiate the patient’s plan of care and oversee their rehabilitation stay. Physicians collaborate with the entire rehabilitation team and prescribe medical interventions to facilitate functional progress. These interventions may include pain management, increasing alertness, decreasing agitation, managing depression/anxiety, and controlling hypertonicity/spasticity. These factors play a role in the patient’s ability to use and manage complex rehabilitation technologies. The physician also collaborates with the therapy team on the procurement of the patient’s equipment needs.
Members of the rehabilitative nursing staff focus on 24-hour care for the patient. This includes the implementation and consistent use of the complex rehabilitation technology throughout the day. The rehabilitation nursing staff responsibilities include daily setup/access to the complex rehabilitation technology, and medical management to maximize the patient’s ability to utilize this technology. Additionally, they frequently assess the patient’s tolerance of equipment, especially skin integrity and tolerance. Madonna therapists have a wide selection of options to choose from in regard to seating and positioning products. These options include products that distribute pressure by immersion principles (air/foam/gel products), full contact pressure distribution, or orthotic/offloading production to aid in skin protection.
The physical therapist’s (PT) main role involves maximizing and facilitating mobility in all of the patient’s possible environments. Based on the patient’s level of function, various mobility methods can be considered, including ambulation, manual wheelchair propulsion, manual wheelchair propulsion with power assist/add-on feature, or power wheelchair management. The PT is also the team member that focuses on optimal positioning in the seating system to promote mobility, facilitate the use of environmental controls, and decrease the chances of secondary complications (pressure injuries and non-correctible postural deformities). PTs evaluate for optimal drive control options, including various joystick handle shapes, head switch controls, simple switch controls, and breath control systems.
Control Options and Power Assist
Joystick use is the drive method of choice as it is the most intuitive means and easiest to learn. If the patient lacks the ability to effectively and safely manage their mobility with the joystick controls, then the patient is assessed for head array/switch controls or sip/puff means of mobility. Head switch controls are typically the mode of choice at this point if the patient has the head control to manage it. If the patient lacks the head control for head switch management, then a breath control device may be used. If these first three drive methods are deemed unsuccessful, then simple switch controls can be integrated at any given point where the patient can generate a consistent command.
Power assist add-on units to manual wheelchairs are frequently used as an alternative to true power wheelchair controls. This drive allows the benefits of accessibility and decreased weight of a manual wheelchair while decreasing the strain on the person’s upper extremities. It is designed not only to decrease strain on the upper extremity, but also to decrease the frequency of push strokes. It allows the transport of the wheelchair out in the community without the added expense for vehicle adaptations that power wheelchairs require.
They also assess for the ideal means of pressure relief completion—teaching the patient various weight shift techniques or using power actuator controls (power tilt, power recline, or power elevating legrests). A manual tilt in space wheelchair may also be recommended if the patient is not safe and able to manage the power wheelchair for mobility and pressure relief completion. The manual tilt in space allows caregiver-assisted mobility and pressure relief completion.
The patient is also evaluated for benefits of alternate power actuator functions, such as power standing features or power seat lift systems. Power seat lift and power standing devices allow added access to the patient’s environment, thus increasing the patient’s independence with activities of daily living. For a social and self-image perspective, both devices also allow the patient the opportunity to be eye level with others that they are interacting with. Both of these devices can be easily controlled and accessed through the patient’s drive control system.
Multiple Clinical Expertise
Occupational therapists (OT) play a key role in maximizing a person’s ability to participate in personally identified, meaningful activities. The OT gauges how the patient will access their technology and implement it in daily life (home, school, work, and other community activities). The OT leads the patient, family, and team with technology that uses phones, computers, and environmental controls. Devices accomplishing these tasks include Bluetooth, infrared, and voice activation technologies.
Speech language pathologists (SLP) play a significant role in the use of complex rehabilitation technology for achieving the patient’s highest level of function and improving quality of life. Their main responsibilities include assessing/treating cognitive dysfunction, augmentative communication, and environmental control access. They use a variety of technologies to maximize function, including head tracking, eye tracking, EMG switches, sensor switches, static/dynamic displays, text to speech devices, and communication applications for tablets. SLPs work closely with physical and occupational therapists to integrate technologies into the patient’s mobility and environmental control devices.
The rehabilitation engineer is a specialized team member who is committed to maximizing independence and improving quality of life for patients. Their main responsibilities are customizing devices and developing new technologies.
Neuropsychology/counseling team members play important roles in the patient’s emotional well-being and ability to cope with traumatic events. They counsel and support the patient in accepting the need for assistive technology.
Recreation therapists (RT) use technology to engage patients in leisure and recreational activities. They train individuals on using adaptive controllers for gaming systems, computers, and tablets. RTs may introduce specialized standing wheelchairs to allow people with impaired mobility to participate in activities such as golf, fishing, archery, and shooting.
DME suppliers, while not employees of Madonna, are important team members in the access and procurement of complex rehabilitation technology. They are involved in the evaluation, trial, funding procurement, delivery, and final fitting of equipment. These suppliers are key in the long-term success of the patient using the technology.
The Inpatient Evaluation Process
The complex rehabilitation technology evaluation process begins the day the patient is admitted to the facility. The daily admission list is screened by the seating and positioning specialist prior to the patient’s arrival. Patients with diagnoses that could potentially benefit from complex rehabilitation equipment have their pre-admission assessment reviewed, and an initial plan for equipment is developed. Once the patient is admitted, the seating and positioning specialist completes a face-to-face screen. This screening involves body measurements, upper extremity function/strength, and cognition. After completing the initial equipment plan, the wheelchair technician assembles the mobility base. The equipment is then delivered to the patient’s room for use in the next day’s therapy evaluations. This process serves multiple purposes. It ensures that functional and safe equipment is available early in their rehabilitation program. It also allows the patient to be out of bed earlier, maximizes efficiency of the primary therapy teams’ evaluation, and permits initial education on the equipment.
The day after admission, the primary therapy team evaluates the patient. At this stage, the initial education on the equipment is completed, and the patient is assisted into the equipment for the first time. Then, the primary therapist and/or the seating and positioning specialist complete adjustments and modifications. Training, adjustments, modifications, or changes to equipment are tweaked (as necessary) throughout the patient’s rehabilitation stay. New features and technologies are also added as the patient gains new skills and progresses toward maximal function.
During the course of this ongoing evaluation, numerous aspects of the patient’s needs, function, and goals are considered. These individual elements include mobility, positioning, environmental access, community access, social connectivity, and leisure needs. The patient’s positioning support requirements are frequently assessed and modified. Numerous seating and positioning products are available to trial to optimize a person’s posture, tolerance of sitting, and skin protection. Next, interface pressure mapping is completed for anyone who is predicted to use a wheelchair as their primary means of mobility.
As the patient’s mobility, positioning, and technology needs are determined and a discharge plan is established, a formal wheelchair seating and positioning evaluation is scheduled and completed. This evaluation is completed by the seating and positioning specialist with direct input from the patient, primary rehabilitation team (usually represented by the primary PT during the evaluation), the patient’s family/caregivers, and the DME supplier. When the evaluation is completed and the final equipment list is formulated by the supplier, the seating and positioning therapist composes the necessary justification paperwork for the equipment. This paperwork is then reviewed and written concurrence is obtained from the physician. Case management gathers the paperwork and sends it to the DME supplier. Once the supplier obtains all the necessary documents, it is submitted to the patient’s insurance for authorization.
During the authorization process, the patient typically completes the inpatient rehabilitation program and discharges from the facility. Prior to discharge from the facility, the seating and positioning therapist works with the DME supplier on the procurement of appropriate loaner equipment. This loaner equipment is delivered and adjusted to meet the patient’s needs until their personal equipment is approved, ordered, and delivered.
Outpatient and Follow-Up Services
Despite constant effort to increase the efficiency and facilitate timely equipment procurement, rarely does the final delivery of equipment occur prior to patient discharge from inpatient rehabilitation. Consequently, patient accessibility to follow-up services is a key component to the successful outcome of personalizing complex rehabilitation equipment. At Madonna, patients are encouraged to take advantage of these complimentary services. If and when it’s appropriate (based on the patient factors such as home location and access to transportation), delivery of the final equipment is completed at the outpatient seating clinic. This allows the patient, caregiver, DME supplier, and seating therapist to take part in the final fitting and setup of the equipment. With respect to the environmental controls, these devices will need to be set up in the patient’s home.
Despite the recommendations for delivery at the outpatient seating clinic, this is not always feasible. Many of the clients that Madonna serves are from all over the region. In these cases, equipment delivery, fitting, and modifications are completed by the DME supplier in the patient’s home. Follow-up services are highly recommended 3 months after discharge and then yearly. This helps ensure that a patient’s needs are being met in the long term. It also allows them to remain highly functional, decreases the chances of secondary complications, and keeps them current with the latest complex rehabilitation technology.
Case Study
LS is a 66-year-old male who suffered a C3-4 spinal cord injury and resultant tetraplegia in a bicycle accident in 2006. This accident caused severe cervical spine fractures that required surgical stabilization and prolonged immobilization to heal. This prolonged immobilization and surgical intervention caused significant cervical ROM limitations, which ultimately limited the options for wheelchair drive controls and switch access. His injury has also required 24-hours-per-day ventilator support for respiratory function.
LS was admitted to Madonna after an extensive acute care hospital stay. Upon admission to the rehabilitation facility, therapy focused on increasing upright tolerance and initiation of wheelchair management controls. Due to his level of injury and cervical spine range of motion restrictions, sip and puff drive controls were selected. LS progressed quickly in his ability to control the wheelchair functions. He could utilize an infrared proximity beam switch for profile and mode selection in the wheelchair. This beam switch gives him independent access to drive, power actuator/pressure relief, Bluetooth (phone use), and infrared (environment controls such as TV, DVD, and stereo) modes. LS is also proficient with voice activation control of his laptop computer, including use of email, to stay in touch with family and friends. RM
Wade Lucas, PT, DPT, ATP, is a graduate of the Division of Physical Therapy program at the University of Nebraska Medical Center. He works as the Wheelchair Seating and Mobility Specialist at Madonna Rehabilitation Hospitals and has 14 years of experience in the field of mobility. Wade is certified as an Assistive technology Professional (ATP) by the Rehabilitation and Engineering Society of North America (RESNA). He also has experience working as a durable medical equipment supplier. For more information, contact [email protected].




