 |
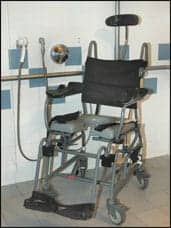
| Tall back commode chair. |
Perhaps the most important part of rehabilitation after a traumatic brain injury or spinal cord injury is to help restore independence in performing the most intimate daily tasks. This is reflected in our mission statement and core values. The mission statement is “To promote optimal health and quality of life for people affected by spinal cord injury and traumatic brain injury.” The core values include fostering independence in those we serve, creating an environment of peer support, developing a family atmosphere where caring for others is contagious, providing each patient and family with individualized care through teamwork and collaboration, educating others about all aspects of life with spinal cord or brain injury, and putting fun into the process of rehabilitation. The following will present how a leading rehab hospital incorporates this mission and these values during rehabilitation, paying special attention to the subjects of bathing and toileting after an injury.
RELEVANCE
Bathing and toileting are arguably some of the most intimate things that we, as humans, do for ourselves on a daily basis that are essential for health, productivity, and well-being. They are tasks that might be done with a significant other on occasion, but for the most part are done privately. After a traumatic brain or spinal cord injury, both of these intimate tasks are rarely accomplished in the private domain. Intimacy must be shared with caregivers. It is up to us as caregivers to remain within the domain of intimacy and privacy as much as possible while fostering as much independence as we can.
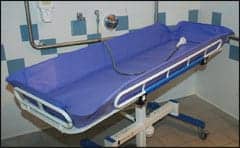 |
| Quad-tub. |
Bathing is important for a patient’s complete picture of health. Proper hygiene contributes to the physical health of the patient’s skin. The skin has a higher likelihood of remaining intact without breakdown if it is properly inspected, cleansed, and moisturized on a regular basis. Equally as important is bathing’s positive contribution to a person’s emotional well-being. Looking and smelling good after a thorough bath can boost a patient’s spirits. Proper management of bowels and bladder greatly contributes to health as it has significant effects on vital organs of the body. Self-dignity is in jeopardy when a patient is incontinent. This creates an atmosphere where proper management of these bodily functions has higher importance. Our staff promotes self-dignity and independence in the two domains of bathing and toileting, ranking them of equal importance with other aspects of a person’s medical plan of care during their rehabilitation. The ultimate goal after inpatient rehab is to foster complete management of toileting and personal hygiene to help allow a patient to return home, to their careers, and to other aspects of their lives that would be in jeopardy if they weren’t managed.
ADMISSION
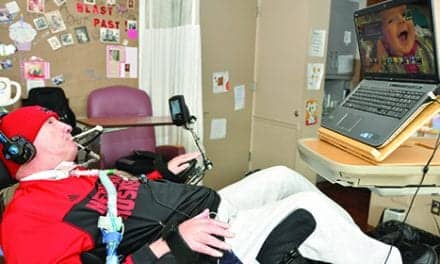
On admission, a patient’s experience may be different from their experiences at other facilities. They are evaluated during the initial period in acute care and then introduced to our facility’s approach to toileting, hygiene, and bathing. Our patients are given showers every other day instead of the common “sponge bath” given at the bedside. We use various types of commode/shower chairs, shower benches, and “quad-tubs” to ensure that even the most acute patient can feel the rush of water over their head and face. For some, the face is the only part of their body that has normal sensation and the rush of warm water is many times comforting and pleasurable. Each morning, and on the days that a patient does not receive a shower, they receive a thorough bath at the bedside, especially focusing on hands, face, groin area, and axillaries. This refreshes them for a hard day of therapy and rehabilitation.
Toileting can occur in a variety of ways, depending on the patient. With severe injuries involving the brain or spinal cord, loss of bowel and bladder control is usually a factor. Having bladder and bowel accidents can greatly decrease the quality of life by causing breakdown and infection of skin, digestion and constipation problems, anxiety and depression, social isolation, and unemployment, among other things. Among all stressors surrounding an injury, our patients appear to worry about bowel accidents most often. Establishing a bowel program upon admission to our facility helps create a situation that promotes independence in this area quickly and effectively. A bowel program trains the bowel to empty at approximately the same time each day with the use of a suppository and, if necessary, the use of digital stimulation. The bowel program’s success is also dependent on a healthy and balanced diet, fluid intake, and the effects of different medications.
A bladder program will also be established on admission as soon as the patient’s bladder function is determined. This might include an indwelling catheter, trained time voids, or intermittent catheterization. The decision for bladder management is patient centered and considers multiple factors including lifestyle.
 |
| Upright commode chair over toilet. |
DURING INPATIENT REHABILITATION
Throughout a patient’s stay, education about how to increase independence as much as possible with these self-care activities as well as practice time for these activities takes place. This requires a great deal of support and patience. If a patient is unable to perform self-care, a caregiver must be instructed on these important tasks. Acute sensitivity is needed by the staff administering this education due to the intimacy of both bathing and toileting. Emotions are frequently high. For example, if a young man in his twenties must allow his mother to assist him in taking a shower and seeing him unclothed, he may experience emotional distress. It is many times traumatic for a husband to allow his wife to assist him with elimination. Couples fear losing sexual intimacy when one partner becomes involved in the other person’s intimate acts such as toileting. This must be considered when beginning education and training with patients and their caregivers. There are times that insurance will fund home health attendants to do personal care after discharge. However, a family member must be trained in case insurance changes or a hired caregiver fails to show up for work. Unfortunately, issues like this with home health care can be common.
Education and training are tracked meticulously by nursing and the rest of the interdisciplinary team to ensure that everything is well covered before discharge. This includes the patient working with their caregivers to practice self-care. Weekly education documentation is supplemented by care plans with goals and progress toward these goals so that everyone within the care team is on the same page. Weekly patient rounds with the entire interdisciplinary team are a forum where these goals and potential challenges are discussed.
DISCHARGE
Discharge planning will ensure that the level of independence achieved in the hospital setting can be carried over to the home setting. Home modifications may be necessary to ensure that a patient can take a shower at home and have a daily bowel program on a commode chair or elevated toilet seat. Lying in bed during a bowel program is not recommended because it does not coincide with the body’s natural process. Discharge planning includes training not only in bathing and toileting self-care skills, but in other supportive measures such as daily skin checks to prevent breakdown, weight shifts throughout the day, and proper nutrition.
We believe that part of our responsibility is to prepare the patients and their caregivers for bathing and toileting outside of the home. Examples include going on vacations or possible challenges while returning to work. Traveling may not seem like an option for newly injured people after a traumatic brain or spinal cord injury, but it is certainly attainable. Our staff tries to encourage patients to return to as many aspects of life that they enjoyed before their injury as possible, and traveling may be one of them. Flying on an airplane or staying in a hotel may be challenging. Using special equipment and special accommodations may be necessary; however, it is certainly possible. For example, medical equipment can be flown and checked with your baggage, special medical equipment can be purchased that breaks down for the purposes of travel, and in some cases, equipment can be rented and provided by the hotel and awaiting you in your room upon arrival. Nowadays, many hotels have accessible rooms with roll-in showers and wide-enough entryways for even the largest wheelchairs. The staff at Craig Hospital has full responsibility to educate patients on these potential challenges and alternatives in order to maximize functional independence and subsequent mental health.
CONCLUSION
The importance of thorough education and a plan of care surrounding bathing and toileting is clear. Support and empathy are critical while implementing this education and training process. Functional and effective strategies begin in rehabilitation, and skills are honed and adjusted appropriately once the patient is discharged. Toileting and bathing are important and sometimes delicate subjects after a traumatic brain injury or spinal cord injury. This must be understood by all members of a patient’s interdisciplinary team.
CASE STUDY
We had a patient who was in a motor vehicle accident that left him with tetraplegia and dependent on a ventilator to breathe. He spent 2 months in an ICU with medical complications during which time he was barely moved. On a sporadic basis, he was given a sponge bath at the bedside. His hair was rubbed with “no-rinse” shampoo once a week. His skin became dry and flaky. He had frequent bowel and bladder accidents in bed. He never felt clean, and he became self-conscious about the way he smelled. His skin began to break down on his buttocks because he spent so much time immobile and dirty from incontinence.
The patient was transferred to Craig Hospital to begin his rehabilitation process. On the first night he was admitted, he received a shower. His hair was washed using real shampoo and his face was shaved clean. After the shower, his skin was fully inspected and moisturized so that the healing process could begin. The patient vocalized to the staff that it was the first time since his injury that he felt slightly like himself again. Not only did he feel better with improved mental health, his skin was protected and at less risk for further breakdown. He also was started on daily programs for bowel and bladder control. Bowel programs took place in a commode chair, decreasing contact between body fluids and skin. By the end of his stay at Craig, his skin was healed and his bowel movements were controlled. The patient had plans to discharge home where his house had been modified during his stay in the hospital to accommodate his new bathing and toileting needs. His training and education prepared him for re-entering the life he had before his injury more than he could have imagined. Because of his appropriate hygiene and controlled toileting, returning to work and functioning in society could be possible despite needing a wheelchair for mobility.
Jennifer Biggs, RN, BSN, CNRN, has worked at Craig Hospital, Englewood, Colo, for the last 5 years. She is currently one of the clinical nurse coordinators and evening shift nurse managers, and cares for patients with both traumatic brain injury and spinal cord injury. For more information, contact .