 |
Electrotherapy modalities have long been a viable option for pain management. Decades ago, many physical therapy offices had a room dedicated to a large diathermy machine, which allowed therapists to apply large, heated pads to the affected area on the patient. While not many of these units are in physical therapy offices these days, electrotherapy modalities from ultrasound to transcutaneous electrical nerve stimulation (TENS) to phonophoresis continue to offer patients much needed pain relief.
“Electrotherapy modalities really help in effective pain management,” says Priti Ravishankar, PT, who uses ultrasound, interferential current, and TENS in her office, Quinn Orthopedic Physical Therapy, Cupertino, Calif. A variety of conditions benefit from electrotherapy modalities—the key is to match the patient’s needs to the strengths of a particular method.
EXPLORING MODALITIES
Rodney R. Heschong, PT, is the owner and director of Mill Valley Physical Therapy and Sports Rehabilitation, Mill Valley, Calif. About half of the practice’s patients seek sports-injury rehabilitation, and Heschong says that electrotherapy modalities are ideal for many athletes. For example, these treatments can help baseball players with throwing injuries; volleyball players who experience pain due to repetitive overhead hitting motion; golfers and tennis players with back, shoulder, and elbow problems; skiers who develop knee pain; and bikers or runners with tendonitis or bursitis around the hips, knees, and ankles.
“In the sports world, tennis elbow is a perfect candidate,” Heschong says. “Achilles tendinitis and plantar or fasciitis are other injuries that would be very receptive to this type of treatment.”
For patients who have had a leg or an arm in a cast for several weeks, electrotherapy can help reeducate the muscles supporting the knees or the shoulders. “Electrical muscle stimulation can be used for muscle reeducation as well as muscle spasm and edema reduction,” Heschong says.
Most patients respond well to electrotherapy and find some relief. “Not everybody is going to be 100% cured, but most of the time, we see a decreased swelling from inflammation in the area,” Heschong says. “We see an increase in the elasticity of the tissues and extensibility of the tissues around the joint. Ultrasound, phonophoresis, and muscle stimulations are all very positive modalities to help that occur.”
Different modalities are used for different types of pain and for different parts of the body. “Ultrasound is effective mainly for soft tissue injuries, such as tendonitis or sprains or strains in the muscles, and sometimes to loosen up scar tissue in an area,” Ravishankar says. “Interferential current and TENS are used to decrease pain in conditions such as low-back pain and neck pain.”
While using TENS does not cure the source of the pain, it provides enough relief to help patients recover more quickly. “I’ve had many low-back pain patients who have responded extremely well to TENS units, so they can get through the most acute aspects of their pain,” says Tom Watson, DPT, MED, of Peak Performance Physical Therapy, Redmond, Ore, who is a Diplomate of the American Academy of Pain Management and a member of the Oregon Pain Management Commission. “After a couple of months, they’re pain free—not because of the TENS, but because their back has had a chance to heal, and they’re able to sleep at night, too.”
To treat neuropathies, including chronic regional pain syndrome (CRPS) I and CRPS II, Watson uses a cranial electrotherapy stimulation (CES) microcurrent unit. It resembles a TENS unit, but uses microamps rather than the milliamps used for TENS and interferential current modalities. Microcurrent treatment, which usually lasts 20 minutes per session, is especially effective for clients with fibromyalgia.
“I’ve had several dozen fibromyalgia patients who have had their sleep restored, and they can sleep 6 hours a night,” Watson says. “That’s extremely important for treating fibromyalgia because restorative sleep allows the full gamut of hormones to be released and restored. If you don’t hit your deepest sleep in the first 2 hours, you don’t get all of your hormone restoration, and you’ll end up fatigued, in pain, and tired for the whole day.”
The treatment also has proved to help restore sleep to patients who suffer from stress or anxiety. “If they have insomnia, I do cranial stimulation for 60 minutes, or they can get a unit and do it for 60 minutes at home before they go to sleep,” Watson says.
According to Watson, microcurrent stimulation ranges from 0.5 microamps to 50 microamps. Watson prefers using a low impulse. “The reason it works with neuropathies and in the brain is something called the Arndt-Schultz principle,” he says. “This means a low impulse placed against the body will promote a dramatic change in the body long-term. However, a high impulse, such as galvanic stimulation direct current, will promote a brief change in the cellular area of the body. So, that’s why the microcurrent works.”
Watson also uses interferential current for the shoulders, elbows, back, and neck. “I use interferential current with chronic pain on just about any joint from the neck to the feet,” he says. He notes that this modality allows the treatment to penetrate deeper, although, like TENS, this treatment provides only temporary relief.
“The TENS and interferential current work like eyeglasses,” he says. “You can have them on, and when you take them off, you need to put your eyeglasses back on to see again. What you’ve done with the interferential current and the TENS unit is simply block out the pain.”
Interferential current and TENS units can be purchased for the patient’s home, and some may be covered by insurance companies that offer durable medical equipment reimbursement. “You can go home with a portable unit and wear it 24/7, if you want to, and it will block out much of the pain information—not all of it, but much of it,” Watson says.
The additional benefit is that patients using these units to relieve pain may not be as dependent on pain medications. “The microcurrent for chronic pain patients with fibromyalgia, chronic intractable headaches, and peripheral neuropathy can also reduce the need for opioid medications,” Watson says. He adds that these units can provide pain relief for patients with terminal cancer. “All you’re trying to do is make them comfortable for end of life,” he says.
One promising area for electrotherapy is iontophoresis, which is the use of direct current to deliver pharmaceutical or nutraceutical compounds to the affected area via a dispersive pad. “You actually drive the solution from the dispersive pad, and that can be almost anything,” Watson says. “That can be cortisone, analgesics, muscle relaxants, vitamins, or even a nutritional supplement.” Watson notes that iontophoresis has applications outside of physical therapy as well. Ophthalmologists use it to treat the eyes, and neurosurgeons are able to use it to drive medication to the spinal cord through a patch.
Heschong’s practice has been moving away from iontophoresis because some patients are sensitive to the solutions applied to the pads. “Depending on the sensitivity of their skin, some patients have developed rashes, so we just felt like it potentially created more problems than it solved,” he says. “But, if the physician or patient insists on that modality, no problem, and, hopefully, the benefits will outweigh any negative issues.”
Instead, Heschong and his staff now often use phonophoresis, which employs ultrasound to drive a type of cortisone cream into the skin tissues. “Then the cream is absorbed through the underlying tissues and helps with decreasing inflammation and promotes healing,” Heschong says. “We get a much better response and fewer negative effects from that treatment.” The modality is effective for strains and sprains, particularly for joints, tendons, and ligaments around the joints.
PROCEEDING WITH CAUTION
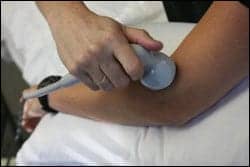 |
| Ultrasound is a favored electrotherapy modality when treating soft tissue injuries, such as tendinitis or muscle strains. |
While electrotherapy modalities can be effective in many situations, there are several contraindications to keep in mind. Women who are pregnant are generally not candidates for this type of treatment, nor are patients who wear pacemakers or who have diabetes, treatable malignancies, or other complications. It is also important to avoid open wounds, open sores, skin rashes, and decubitus ulcers.
The main concern is overheating, which can burn the tissue. This is particularly relevant for patients who have metal screws, plates, pins, or rods that have been placed around the healing area. “You don’t want to heat up the metal plates that would then create a situation where there would be the potential to burn the surrounding tissue,” Heschong says.
When electrotherapy is an option, Heschong stresses the importance of taking a good case history. “There is no cookie-cutter approach,” he says. “Each patient and injury needs to be evaluated, assessed, and then addressed. Take a good history, do a thorough evaluation, and then from that evaluation, choose your modality for what you want to achieve as an end result.”
It is also important to test the modality on the patients in the office before they invest in the device for home use. This gives the therapist the opportunity to see if the patient knows how to set up and use the unit, while the therapist makes sure that the treatment modality works for the patient. “If they’re going to get relief from TENS units, it’s going to happen in the first 10 to 15 minutes,” Watson says. “The microcurrent may take 20 minutes. So, you can usually tell with the first trial.”
ANTICIPATING TRENDS
Currently, neurosurgeons can implant electrodes directly into the brain to help control pain, but Watson hopes a nonsurgical solution will emerge in the future. The ticket is to unlock the secrets of the brain itself so there is a greater understanding of the pain receptor sites. “The body is a series of positive and negative charges,” Watson says. “We still don’t understand that very well, so there is ongoing research to get better input and information into the body to block out pain. We’ve got a long way to go, we’re only at the surface. Remember, pain does not have to be a way of life.”
Heschong believes that the immediate future for electrotherapy is continued research and development as well as refining the production of the existing modalities, particularly lowering prices, so that more patients can afford to have the devices at home. “That would assist the therapist, in the sense that we can spend more of our time with hands-on stretching, strengthening, and stabilization-type exercises in the clinic. We wouldn’t have to spend as much time reducing the swelling or reeducating the muscles because the patient could be taught by the therapist to do that at home,” he says.
Additional information on electrical stimulation can be found by searching our free online archives.
There are also new modalities on the horizon, and Heschong says that the best way to keep up with the field is to attend continuing education seminars and stay abreast of the literature. “Laser therapy is an up and coming electrotherapy modality,” he says. “It’s definitely on the forefront of the rehabilitation future.”
As the field continues to evolve, Heschong has high hopes for the future. “Hopefully, we’ll have better techniques and better equipment, and it’ll be a lot less pain, and a lot less rehab time, making it a lot quicker for the patient to get back on the tennis court and the golf course,” he says.
Ann H. Carlson is a contributing writer for Rehab Management.



