It was his first accident in the 15 years he owned his dream motorcycle. Blithely cruising down a windy back road, he did not see a fallen tree branch on the street. He tried swerving, only to slip off his bike and land on the gravel-embedded side road. The helmet saved his life, but it did not protect him from a branch that stabbed him in the right thigh, causing a deep laceration that required immediate attention. Thus began a long trip down a road for him—sans the motorcycle—and his only stop was a hospital, or so he thought.
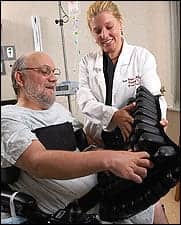 |
| Wound care specialist Gwen Berger, MS, PT, CWS, demonstrates the pressure-relieving capabilities of a high-profile wheelchair cushion to patient Wayne Sigley. |
As it turned out, the laceration, which had extended into the muscle, became infected and resulted in further damage to the muscle and even the bone. Already having difficulty moving from multiple other injuries, he developed a pressure ulcer from a lack of mobility, necessitating a longer hospital stay than anticipated.
These incidents and many others are the ones that wound care-certified professionals at Good Shepherd Rehabilitation Network encounter on a regular basis.
They face a wide gamut of injuries and conditions; from the commonly seen surgical and pressure ulcers, to the not-so-common wound types stemming from calciphylaxis—a rare disorder seen in patients on dialysis that results in plaque-like ulcerations—and necrotizing fasciitis—a rapidly progressing infection of tissue along fascial planes, venous channels, and the lymphatic system that causes extensive necrosis.
Regardless of the severity of a patient’s condition, wound care specialists develop an individualized care management program based on a set of standard procedures. This customized regimen follows vigorous exam with the goal of guiding patients back to a lifestyle similar to a time before their wound. They also educate their patients and involve friends and family members in order to help patients progress and recuperate faster.
ASSESSING THE WOUND: WHERE IT ALL BEGINS
The motorcycle accident patient arrives with a traumatic wound, osteomyelitis—an infection of the bone—as well as a Stage IV pressure ulcer. The sole question running through his and generally every patient’s mind is “How long will it take until this is healed and I can go home?” There is never a simple answer, but with thorough examination, specialists can gain a better understanding of how long the recovery will take.
A wound is assessed by measuring length, depth, width, presence of tunneling or undermining, presence and type of necrotic (dead) tissue, signs of bacterial overload, periwound tissue—skin around the open area—drainage, and odor. Often they will look at the patient’s comorbidities and nutritional and mobility status. Instruments relied on by wound care specialists are few but effective: paper measuring rulers, sterile swabs, a camera, and a Web-based wound care outcome tracking and management system, which is capable of managing such customizable protocols as digital images and custom reports.
Good Shepherd subscribes to a Web-based wound care management system, which serves as an excellent source for understanding a patient’s condition. The program enables specialists to track trends and determine whether the wound is improving, but most important, it aids in initial wound assessment. Specialists enter assessment data into the program once a week for each wound. The program then calculates area and volume and enables therapists to print out various statistical and facility reports. The reports are further enhanced by photos taken with a digital camera. The reports are then printed out and placed on the chart, providing all staff involved with the patient an overall layout of the wound. With a newfound understanding about the wound, physical therapists and nurses create an individualized regimen while relying on a set of standard wound care treatments.
The other clinicians involved in the patient’s care also can adapt their care to the patient’s needs with regard to the wound. For example, physical and occupational therapists often include seating, pressure relief, and increasing overall mobility as part of their treatment, which further enhances wound healing.
ADDRESSING THE WOUND
Wound severity aside, the standard program includes wound dressing type, support surface, nutritional status, treatment of comorbidities that may affect the healing of the wound, and education of the patient, family, and caregivers. Often the program involves consulting plastic surgeons, infectious disease physicians, and vascular surgeons. Wounds can change from day to day, thus leading wound care professionals to treat this as a dynamic art. As the wound changes, the treatment has to change too, and wound care specialists need to observe the wound regularly and closely to implement timely treatment changes to maximize a successful outcome.
Wound care specialists often find themselves with more than one way to heal a wound. Many dressings and modalities exist so that if one treatment does not work, they are guaranteed a Plan B, Plan C, and so on.
While a set of standard practices apply to all wounds, factors such as location and severity of the wound force specialists to reconsider their approach. If the wound is in an unusual spot, specialists must ask themselves what dressing(s) is the most supportive and will likely stay on a patient. They also must question if the dressing may inadvertently cause increased pain or pressure to the area.
A wound with increased complexity or severity causes specialists to prioritize the appropriate steps. The most severe wounds typically have many layered problems that need to be addressed. For example, a wound containing large amounts of necrotic tissue and malodorous copious drainage and has several signs of infection leaves specialists with many goals to accomplish; the specialist has to prioritize the problems so that attention can be given to those requiring immediate service.
Modern technologies, such as the VAC (vacuum-assisted closure), use negative pressure to stimulate wound healing and enable wound care professionals to attack multiple problems all at once. The negative pressure draws out fluid that collects in the tissues surrounding the wound, thereby helping to increase circulation and decrease pain in the entire wound region. This technology can promote granulation, manage large amounts of drainage, aid in the reduction of periwound edema, limit dressing changes to three times per week, and decrease bacterial load simultaneously.
Ideally, it is imperative for specialists to view a wound as having a past, present, and future. Every wound has a past, and these questions must be considered: How did it develop? Is the cause of it still present? What treatments have been tried so far? What else is affecting the patient medically, psychologically, and socially?
Moving onto the present, the wound care team must measure and picture the wound. Through examination, the team discusses the current nutrition status, comorbidities, stress level, and patient mobility status. Specialists determine what characteristic of the wound needs to be addressed most and then move forward. Last, specialists must consider the future of the wound. Because wound healing is a dynamic art, it is crucial to be ready for the next steps in the healing process.
EDUCATING THE SUPPORT GROUP
Getting family and friends involved with a patient’s healing process plays a significant role. Specialists provide them with pictures of the wounds along with progress reports. When treatment is recommended, patients, family, and friends learn about healing stages—how to get through them, what to expect to see as the treatment progresses, and alternative routes to take if a specific treatment proves ineffective. Patients and their supporters often take the healing process on as a project; they take pride in learning what went wrong, how it can be corrected, and how to prevent it from happening in the future.
While patients seek the most complete recovery, Good Shepherd’s wound care specialists offer three valuable pieces of advice. First is to become involved as much as possible, and emphasize that patients should not receive wound care, but rather learn wound care. The more patients understand their condition, the better they are able to take part in the healing process. Second, patients need to decrease stress, which is often the cause of vasoconstriction and starves wounds of blood supply. They need to address anxiety conditions early in the recuperation period for a more fluid and effective recovery. Third, patients are urged to never give up. If one treatment does not work, alternatives exist. The wound might have a temporary effect on the daily routine of their patients, but wound care specialists are adamant about finding the fastest and most effective treatment for them.
Gwen Berger, MS, PT, CWS, is a physical therapist and wound care certified specialist at Good Shepherd Rehabilitation Network, Allentown, Pa.





