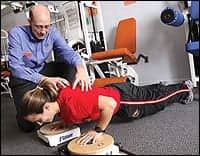
PHOTO CAPTION: Incorporating an aerobic component into treatment sessions can help with pain relief. Aerobic exercise stimulates the release of endorphins, which affects the pain pathway and, thus, reduces the overall level of pain felt.
The right treatment options for the right patients can help the 20% of the population seeking relief from chronic pain.
by Anna Nelsen, PT/DPT, CMPT
Patients with chronic pain disorders can be one of the most challenging patient populations to treat in the field of physical therapy. They may have chronic pain for any number of reasons. Fibromyalgia, complex regional pain syndrome, chronic postsurgical pain, arthritic joints, autoimmune disorders, chronic depression, and longstanding injuries are just a few of the diagnoses that may include chronic pain as a symptom.
Difficulties in the management of chronic pain can also be compounded by several factors, including but not limited to psychological factors, fear-avoidance beliefs, and a too-aggressive approach with therapeutic exercises. A comprehensive approach to physical therapy treatment in these cases is imperative to long-term management. In many cases, it is not feasible to achieve abolishment of the symptoms, but we can provide patients with the tools they need to be fully functional.
Chronic pain, by definition, is pain that is present for longer than 3 months, which is generally accepted as the expected tissue-healing timeline.1 But more commonly, the pain has been present for several months or even years. Chronic pain exists in approximately 20% of the adult population,1 which makes it a common reason for patients to seek pain relief from healthcare practitioners.
In years past, it was more common to prescribe medication and rest as treatment for chronic pain, but the use of exercise and physical therapy has recently become much more influential in the treatment of this patient population. Treatment techniques such as ultrasound, electrical stimulation, manual therapy, dry needling, aerobic exercise, and aquatic physical therapy have all been shown to have some effect on chronic pain. All of these can be found in a physical therapy office, as long as the practitioner is certified in dry needling and aquatics.
Pain Perception
When a pain stimulus is present for long periods of time, it can cause changes in the perception of pain in the surrounding tissues and changes at the local nociceptive level due to the longstanding presence of pain-mediating chemicals. In particular, patients with neurological pain can experience either allodynia (pain in the presence of a non-painful stimulus) or hyperalgesia (exaggerated pain in the presence of a typically painful stimulus).2
Modalities such as ultrasound, electrical stimulation, and manual therapy provide an alternative stimulus to the area which may be effective at decreasing this heightened level of pain sensation. As patients begin to decrease this perceived level of pain, this can increase their tolerance for exercise and daily activities due to an overall lower resting pain level.
Components for Patient Success
As physical therapists, we place a certain importance on progressing our patients toward independence. A large portion of our treatments typically revolve around education of their individual diagnosis and home exercises to continually improve this level of independence. For patients with chronic pain, ongoing education regarding their neuroanatomy and the pain response with a longstanding pain stimulus may be influential in achieving long-term pain management.
In a 12-week randomized controlled trial of patients with chronic lower back pain, patients were separated into groups that received either therapeutic exercise alone, or therapeutic exercises and an education on their neurophysiology. The group who received the education in addition to the exercise had a significantly improved set of outcomes following the study.3 This makes logical sense, owing to the fact that many of us will not participate in a course of treatment until we are given a logical explanation for it.
Aerobics
Incorporating a more aerobic component into treatment sessions of patients with chronic pain may also be influential in long-term pain relief. For example, patients with fibromyalgia may benefit more from aerobic exercise than from resistance exercises.4 Aerobic exercise stimulates the release of endorphins, which affects the pain pathway and, thus, reduces the overall level of pain felt.5
Patients with longstanding pain may benefit from 30 to 60 minutes of low-intensity exercise on most days. This longer bout of aerobic exercise may be too much for patients with acute inflammation, but those with chronic pain actually benefit from longer treatment times at lower intensity. The key is to find a form of aerobic exercise of low intensity that fits each individual patient. Walking may seem like a low-intensity exercise for some, but this may be considered high intensity for those patients with chronic lower back, lower hip, or knee pain.
Dry Needling
Dry needling is another influential modality that can be used for the management of chronic pain, although the research to support its use is limited. Most research which is applied to dry needling consists, in fact, of studies focusing on acupuncture, which has been in use for hundreds of years. Dry needling has been shown, through systematic reviews, to decrease pain and improve mobility in short-term studies,6 but further evidence is required to determine if these effects apply over the long term. However, due to its effectiveness in the short term, it may be a useful tool to enable patients with high resting pain levels to participate in physical therapy sessions.
Aquatic PT
Aquatic physical therapy is the practice of physical therapy in a warm therapeutic pool environment. There has been a wide base of literature to support its use in the physical therapy environment.7 In some cases, aquatic physical therapy can be used to effectively control hip and knee arthritis symptoms.8 In a single-blind RCT by Hinman et al, 71 participants with symptomatic hip or knee OA were randomly assigned to receive either 6 weeks of aquatic physical therapy or no physical therapy. Those that received the aquatic physical therapy saw a significant reduction in pain, joint stiffness, and overall improvement in their function.8
Aquatic physical therapy may also prove useful in cases where patients are having pain which is too severe to tolerate land-based therapy. It may be beneficial to recommend aquatic physical therapy to these individuals as a method for their aerobic and/or resistance training. In many cases, patients find that they can, in fact, be more compliant with an aquatic program because it is less painful than a land-based program, and because simply being in an aquatic environment can decrease their overall joint pain, as described above.
Summary
Overall, incorporating a few of the above ideas into treatment may improve your overall outcomes with a patient with chronic pain. To summarize, incorporating modalities such as dry needling or electrical stimulation can decrease the patient’s level of heightened pain response and make it more likely that a patient can tolerate physical therapy. Including an aerobic exercise portion may have significant benefits over a resistance-training-based program, especially in those patients with fibromyalgia. Finally, referring a patient for whom land-based physical therapy is quite painful to aquatic physical therapy may decrease their joint pain and improve their overall function. While each of these ideas may not work for every patient, it does provide us with some options for this most challenging patient population.
Listening as Treatment
In addition to the above treatment techniques, one of the least-discussed treatment techniques is listening to the patient. Most patients who find their way to your physical therapy office have been to many doctors, healthcare professionals, and even other physical therapists, and have tried several treatment methodologies before. There tends to be a significant emotional component inherent with patients with a history of chronic pain,9 so providing emotional support to the patient can go a long way toward building a productive professional relationship. It is our responsibility to reassure the patient that we will work with them to manage their pain. While we may not be able to abolish their pain, we can help them come up with tools for long-term management and support them in any way needed along the way. RM
Anna Nelsen, PT/DPT, CMPT, is a clinic director at ATI Physical Therapy in Chesterton, Ind. For more information, contact [email protected].
References
1. Geneen LJ, Moore RA, Clarke C, Martin D, Colvin LA, Smith BH. Physical activity and exercise for chronic pain in adults: an overview of Cochrane Reviews. Cochrane Database Syst Rev. 2017;4(4):CD011279. Published 2017 Apr 24. doi:10.1002/14651858.CD011279.pub3
2. Jensen TS, Finnerup NB. Allodynia and hyperalgesia in neuropathic pain: clinical manifestations and mechanisms. Lancet Neurol. 2014;13(9):924-935. doi:10.1016/S1474-4422(14)70102-4
3. Bodes Pardo G, Lluch Girbés E, Roussel NA, Gallego Izquierdo T, Jiménez Penick V, Pecos Martín D. Pain neurophysiology education and therapeutic exercise for patients with chronic low back pain: a single-blind randomized controlled trial. Arch Phys Med Rehabil. 2018;99(2):338-347. doi:10.1016/j.apmr.2017.10.016
4. Busch AJ, Webber SC, Richards RS, et al. Resistance exercise training for fibromyalgia. Cochrane Database Syst Rev. 2013;2013(12):CD010884. Published 2013 Dec 20. doi:10.1002/14651858.CD010884
5. Dos Santos I, Lunardi AC, de Oliveira NTB, et al. Effects of aerobic exercise on pain and disability in patients with non-specific chronic low back pain: a systematic review protocol. Syst Rev. 2019;8(1):101. Published 2019 Apr 22. doi:10.1186/s13643-019-1019-3
6. Espejo-Antúnez L, Tejeda JF, Albornoz-Cabello M, et al. Dry needling in the management of myofascial trigger points: A systematic review of randomized controlled trials. Complement Ther Med. 2017;33:46-57. doi:10.1016/j.ctim.2017.06.003
7. Becker BE. Aquatic therapy: scientific foundations and clinical rehabilitation applications. PM R. 2009;1(9):859-872. doi:10.1016/j.pmrj.2009.05.017
8. Hinman RS, Heywood SE, Day AR. Aquatic physical therapy for hip and knee osteoarthritis: results of a single-blind randomized controlled trial. Phys Ther. 2007;87(1):32-43. doi:10.2522/ptj.20060006
9. Sheng J, Liu S, Wang Y, Cui R, Zhang X. The link between depression and chronic pain: neural mechanisms in the brain. Neural Plast. 2017;2017:9724371. doi:10.1155/2017/9724371