by Eric Edelman, PT
There may be no greater equalizer than pain. Each day physical therapists observe patients coming through clinic doors with varying levels of discomfort, frustration, and anxiety written across their faces. And, while pain is a common thread, each patient experiences it in a singular manner and likewise responds differently to varying pain management techniques.
That important factor is not lost on the therapists at Peak Physical Therapy & Sports Performance, who recognize that a “cookbook” approach—that is, using the same techniques and/or treatments across the board for all patients and conditions—is dismissive to individual needs. The human body is complex and while one or a combination of pain management treatments will work well for some, it will not work for all. Many factors must be considered when developing a treatment plan, including the patient’s age, condition(s), level of fitness, diagnosis, psychosocial issues, past medical history, and pre-existing conditions.
When all aspects are taken into consideration, the chance of achieving a successful outcome is greatly improved. A therapist’s knowledge base is another piece in the overall puzzle of treatment, and there are times when a therapist needs to consult with a colleague if dealing with a more complicated case.
Big Picture Perspective
The treatment philosophy embraced at Peak is based on a holistic approach. In brief, the therapists look at the body as a whole; for while a patient may come in with a “frozen shoulder” or a sports-related knee injury, the therapists have the responsibility to consider the condition of the person’s entire body—oftentimes, this includes the patient’s emotional state. As such, the practice’s therapists utilize a wide variety of manual therapy techniques with a range that invariably depends on the therapists’ experience. Likewise, the therapists are guided by the belief that a literal hands-on approach is of utmost importance when determining a patient’s primary issues. Once a solid diagnosis is established, then and only then will the rate of therapy success increase as compared to placebo.
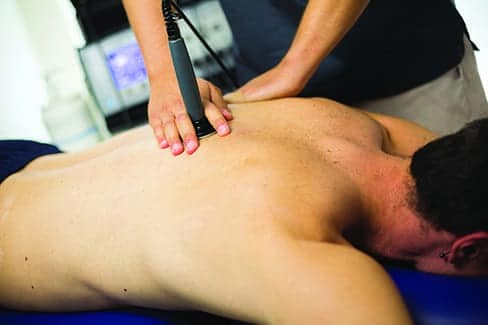
This holistic outlook includes an extensive number of manual techniques and modalities, such as Instrument Assisted Soft Tissue Management (IASTM), joint mobilizations, deep tissue massage, muscle energy techniques (METs), cold laser therapy, ultrasound, dry needling, electrical stimulation, biofeedback, cupping, and aquatic therapy. All have their own merits and are often used in combination, depending on an individual patient’s needs.
[sidebar float=”right” width=”250″]Could Laser Shadow Opioids for the Treatment of Pain?
By Mark Callanen, PT, DPT, OCS
What drives patients to your clinic? While many clinicians like to think it is their expert advice and research-backed exercise programs, the truth is that most patients are seeking clinicians skilled in providing pain relief.
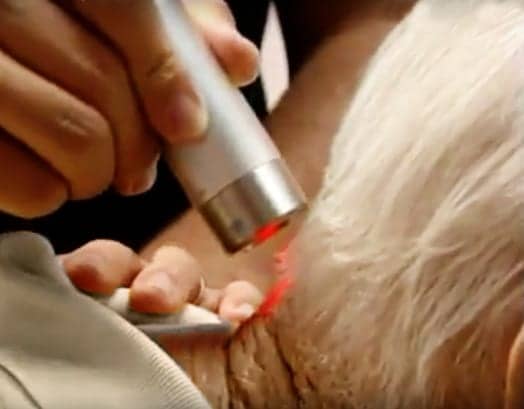
Given the negative press regarding the opioid epidemic, patients are more interested than ever in non-pharmaceutical alternatives for pain management. Therapeutic laser is an alternative that has been utilized in pro and Division 1 training rooms for years, but has only recently been getting traction in the rehabilitation setting. Laser therapy is a non-invasive modality that can have effects on both chronic and acute pain via the process of photobiomodulation (PBM).
PBM occurs when an effective dose of light energy is applied to injured tissue. This creates photochemical stimulation at the mitochondrial level which triggers several positive biochemical changes that can decrease pain1,2, improve inflammation3, and accelerate tissue healing.3,4,5
When acquiring a laser there are a variety of parameters to consider, including the units average power output, therapeutic wavelength(s), pulsing characteristics, and the delivery system, to name a few. Knowing how these factors impact acute, chronic, and deep tissues is important when implementing this modality.
Broadly, in the US market lasers are classified by the output power of the unit. Most lasers fall between Class 2 and Class 4. Regardless of power, PBM is the primary mechanism of action. Where lasers differ significantly is in their ability to create analgesic effects within minutes.
Recent research has shown that higher power densities (irradiance) significantly impacts pain perception via its impact on C and A-delta afferent nerves.1,6 This is a phenomenon that cannot be easily accomplished with lower-powered lasers. Quick analgesic effects from high-powered laser opens the door to more manual options and increased active therapies on the same day. Class 4 laser treatment time is normally equivalent to the time spent providing an ultrasound treatment.
With virtually no side effects and a very short list of contraindications, laser therapy is an emerging player in the pain market and could serve as a game changer in any practice that regularly manages musculoskeletal pain. Special consideration should be given to Class 4 units if the goal is to provide quick pain relief. Understanding the similarities and differences of different laser platforms will help shed light on the best fit for your clinic.
Mark Callanen, PT, DPT, OCS, is the director of clinical development for LightForce Therapy Lasers. He has treated orthopedic patients for 18 years and has been board certified as an Orthopedic Clinical Specialist (OCS) by the APTA since 2003. Callanen earned his doctorate in physical therapy in 2007 from Marymount University.
References
1. Chow R, Armati P, Laakso EL, Bjordal JM, Baxter GD. Inhibitory effects of laser irradiation on peripheral mammalian nerves and relevance to analgesic effects: a systematic review. Photomed Laser Surg. 2011;29(6):365-381.
2. Duchesne E, Dufresne SS, Dumont NA. Impact of inflammation and anti-inflammatory modalities on skeletal muscle healing: from fundamental research to the clinic. Phys Ther. August 2017;97(8):807-817.
3. Stein A, Benayahu D, Maltz L, Oron U. Low-level laser irradiation promotes proliferation and differentiation of human osteoblasts in vitro. Photomed Laser Surg, 2005;23(2):161-166.
4. Mvula B, Mathope T, Moore T, Abrahamse H. The effect of low level laser therapy on adult human adipose derived stem cells. Lasers Med Sci. 2008;23(3):277-282.
5. Dube A, Gupta PK, Bansal H. Modulation of macrophage structure and function by low level He–Ne laser irradiation. Photochem Photobiol Sci. 2003;2(8):851-855.
6. Holanda VM, Chavantes MC, Wu X, Anders JJ. The mechanistic basis for photobiomodulation therapy of neuropathic pain by near infrared laser light. Lasers Surg Med. 2017;49(5):516-524. [/sidebar]
Manual Techniques
Instrument-Assisted Soft Tissue Massage (IASTM) is an advanced soft tissue mobilization technique used at all of Peak’s locations. It utilizes specialized tools to release soft tissue adhesions that may be otherwise difficult to release with traditional massage techniques. Many of the practice’s therapists have specialty training using the Graston technique, which has become a very popular IASTM technique.
Joint mobilization is a manual method on which the therapist positions and moves an affected joint in order to properly stretch the joint capsule. These mobilizations are graded from 1-5 in varying degrees of intensity per a patient’s individual needs.
Deep tissue massage therapy is similar to Swedish massage, but the deeper pressure is beneficial in releasing chronic muscle tension. The focus is on the deepest layers of muscle tissue, tendons, and fascia.
Muscle Energy Technique (MET) is a gentle manual therapy employed to mobilize joints and relax muscles by way of subtle muscle contractions; this method requires active participation of both the therapist and patient.
The MELT Method, a therapy technique for foot and hand issues, is becoming an increasingly popular approach for patients in recovery. This system helps restore support of the body’s connective tissue to eliminate chronic pain and decrease stress caused by repetitive movements and postures. During the procedure, the therapist places a patient in a position that is specific to the dysfunction while the patient applies a small and comfortable muscular contraction against the therapist in a precise direction.
Modalities In the Mix
Cold laser therapy is a powerful modality that employs a class IIIB light cluster to penetrate deep within an affected area; as such, it reduces inflammation and promotes a quicker healing process for all types of soft tissue injuries.
Ultrasound is another commonly used technique to reduce inflammation. This modality, which involves the use of a sound head to administer gel over the affected area, penetrates sound waves to stimulate circulation and/or mechanical changes to speed healing of injured soft tissue.
Dry needling is a form of therapy in which fine needles are inserted into myofascial trigger points (painful knots in muscles), tendons, ligaments, or near nerves in order to stimulate a healing response in painful musculoskeletal conditions. Dry needling is not acupuncture or Oriental Medicine; that is, it does not have the purpose of altering the flow of energy (“Qi”) along traditional Chinese meridians for the treatment of diseases.
In fact, dry needling is a modern, science-based intervention for the treatment of pain and dysfunction in musculoskeletal conditions such as neck pain, shoulder impingement, tennis elbow, carpal tunnel syndrome, headaches, knee pain, shin splints, plantar fasciitis, or low back pain. It is a technique that has resulted in significant pain relief for many of the practice’s patients.
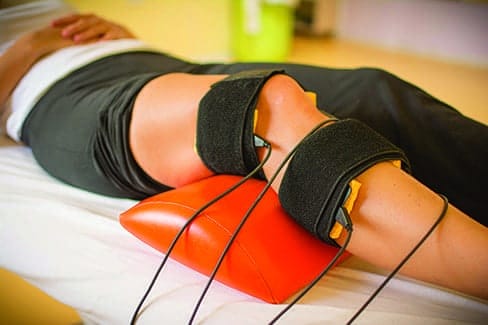
The practice also makes significant use of various forms of electrical stimulation as this is a modality that can be applied for many different reasons.
Different waveforms can be used to decrease swelling (edema), decrease pain, increase range of motion, or increase strength. Some of the types used at Peak include TENS, Russian, Hi-Volt, and Neuromuscular electrical stimulation (NMES).
Transcutaneous electrical nerve stimulation (TENS) is the use of electric current produced by a device to stimulate the nerves for therapeutic purposes. TENS, by definition, covers the complete range of transcutaneous applied currents used for nerve excitation, although the term is often used with a more restrictive intent—namely, to describe the kind of pulses produced by portable stimulators used to treat pain. The unit is usually connected to the skin using two or more electrodes. A typical battery-operated TENS unit is able to modulate pulse width, frequency, and intensity. Generally, TENS is applied at high frequency with an intensity below motor contraction or low frequency with an intensity that produces motor contraction. While the use of TENS has proved effective in clinical studies, there is controversy over which conditions the device should be used to treat. Russian stimulation developed in the former Soviet Union is an aggressive form of electrical stimulation that is usually used in conjunction with therapeutic exercise to develop strength.
High Voltage Pulsed Current (HVPC) can be used for treatment of dermal wounds, edema management, muscle weakness, and pain management depending on the parameters to which the machine is set. HVPC is a twin-peaked, pulsed, direct current. This stimulation modality uses a monophasic pulsed current with the pulses delivered in a doublet. Each pulse is short in duration but at a high peak voltage.
Biofeedback, where a machine is placed on a specific muscle that either works too hard or not enough, continues to be an effective approach. The machine gives signals to the patient and therapist to help them either relax or activate the desired muscle. This is commonly used at Peak for women’s health issues such as urinary incontinence and pelvic pain.
Activity-related injuries often respond well to standard hot and cold packs. Hot packs are frequently used to increase circulation prior to working on the muscles and/or joints that are stiff. Cold packs and ice cups are generally used to reduce circulation in order to minimize pain and swelling after a treatment. Topical analgesics are another tool that can be used to provide temporary pain relief for a number of applications such as sports injuries, joint pain, and loosening tight muscles. Topicals treatments are easy for therapists to use in the clinic and for clients to use at home, and are available in product form that can be dispensed as creams, gels, or sprays.
Outside the Box
And then there is cupping. This modern form of vacuum therapy facilitates deep tissue release through suction. Unlike massage and other fascial release techniques, cupping generates a negative pressure and lifts the skin away from the body by placing a plastic or glass cup on the affected area for a designated time, thereby providing stimulus to promote motion and recovery. This novel form of therapy can mobilize soft tissue, enhance blood flow, and reduce pain.
Aquatic or pool therapy is used in instances where the patient would benefit from being in an environment where the impact of gravity is reduced. For example, it may be used with someone who has had a lower extremity surgery and can’t walk well on the affected joint. It can also be used for conditions such as arthritis, back pain, balance problems, and much more. A physical therapist is actually in the pool with the patient guiding them in the appropriate exercises.
Another pain management technique is Kinesio Taping; this method uses specialized tape to help either relax or stimulate certain muscle groups to achieve a desired result. This is a very popular therapy for athletes as well as for general inflammatory conditions such as patella-femoral syndrome (knee cap issues).
By offering such a wide range of modalities, therapists can stay true to the commitment to treat every patient who walks through the practice’s doors with the specific treatment they need to achieve pain reduction or elimination. RM
Eric Edelman, PT, is the owner of Peak Physical Therapy & Sports Performance with locations in Scituate, Norwell, Quincy, and Hanover, Mass. For more information, contact [email protected].
This article was published in the January/February print issue of Rehab Management under the title “Recipe for Relief.”