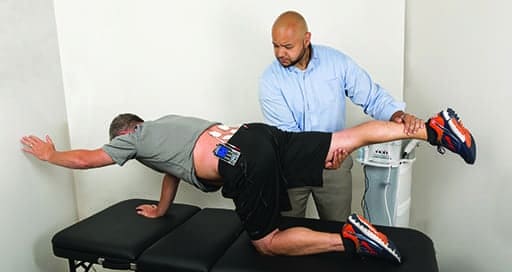
Patient with low back pain being treated with electrical stimulation using a portable TENS device for pain modulation while performing a lumbar stabilization exercise.
by Chad Starkey, PhD, AT, FNATA, and Joseph A. Gallo, DSc, AT, PT
Chronic Pain Treatment
Chronic pain—often identified as pain persisting for 12 or more weeks—can result in prolonged or permanent changes in the peripheral and/or central nervous system. Pain-specific nerves and nerve pathways become oversensitized, causing a pain response in the absence of actual tissue damage. In this case, pain itself becomes the primary problem that interferes with patient function and well-being, more so than the initial cause of the pain.
In some instances, the root cause of chronic pain may be a traumatic injury that directly, or indirectly, stimulates pain pathways, such as spinal nerve root impingement. Systemic diseases, such as rheumatoid arthritis, may also serve as the trigger for this condition. If the source of pain cannot be linked to trauma or disease, neuropathic chronic pain syndrome—an abnormality in pain-transmitting nerves—may be the cause.
Chronic pain interferes with the patient’s activities of daily living, occupational pursuits, and sleep—which can result in decreased quality of life, socioeconomic consequences, and further physical and/or psychological impairments. Patients may exhibit drug-seeking behaviors and/or self-medication using legal medications, illegal drugs, or alcohol. Symptoms of depression, opioid abuse, and self-harm are other far-too-frequent outcomes.1
In the event of acute trauma, surgery is often a first-line option for managing the condition. However, surgery may result in chronic pain. For certain diseases or neuropathic conditions, surgery may be considered as the condition progresses. In some situations, surgery is not an option. Pain medications may also be used, but they carry their own inherent risks such as addiction, incapacitation, and other events that decrease the patient’s quality of life.
Noninvasive Interventions
Clinically, the intervention approach places the primary emphasis on palliative care, although the root cause of the pain must also be addressed, if possible. Often a multimodal, interdisciplinary approach to care is required, including psychological interventions.2 Because of the potentially debilitating nature of chronic pain, home care becomes a centerpiece of patient care planning.
Thermal Interventions
Thermal interventions—heat and cold agents—are inexpensive options for managing pain and are ideal for home care. Cold therapy (cryotherapy) in the form of ice packs or cold water immersion functions to decrease cell metabolism, which slows nerve transmission and increases the pain threshold to produce analgesia. Most cryotherapy techniques are capable of affecting deep tissues. Although cold therapy is initially uncomfortable for many people, its effects are long-lasting compared to heat therapy.
Unfortunately, many people—especially the elderly—do not easily tolerate the cold temperatures used in cryotherapy. Additionally, evidence suggests that using cold therapy too long into the healing process may have detrimental effects.3,4
Heat therapy (thermotherapy) is often preferred by the patient. Taking the form of moist heat pack, paraffin, dry heat (heating pads), spas, or even a hot shower or bath, it acts to increase cell metabolism. Pain is reduced by several mechanisms. The feeling of warmth helps to block the transmission of pain and creates local sedation of the nerve endings. Pain is also further reduced by relaxing muscles, decreasing muscle spasm, and increasing blood flow, which helps to remove certain inflammatory agents that promote pain. Relative to cold therapy, the effects of heat therapy do not affect the deeper tissues and tend to be short-lived following the removal of the heat source.
Therapeutic ultrasound—the use of continuous high-frequency sound waves—can vigorously heat small areas of deep tissue. This heat, combined with stretching and/or other manual therapies, can reduce scar tissue and relieve pressure on the affected nerves. Therapeutic ultrasound interventions are primarily limited to the clinical setting.
Electrical Stimulation
Once considered the stuff of charlatans, electrical stimulation has grown to be a proven, effective treatment option for pain control. Delivered to the body by way of topical electrodes, the electrical current is modified to stimulate sensory nerves, motor nerves, and/or pain nerves affecting the transmission and perception of pain.
One of the first—and perhaps the most common—electrical approach to pain control is Transcutaneous Electrical Nerve Stimulation (TENS). Two or four electrodes are placed around the painful area. Acute pain management is accomplished using short pulses of electrical energy at higher frequency. These pulses are specifically tailored to target sensory nerves, causing a sensation usually described as a strong “tingling.” Similar to rubbing a sore area, activating these sensory nerves helps to block the transmission of painful impulses to the brain (the “Gate Control Theory”). TENS often provides almost immediate pain relief. Depending on the type and location of pain, the post-treatment effects may persist for up to an hour following treatment.
Chronic pain management is accomplished using longer pulses of electrical energy at lower frequencies. This TENS approach targets both motor nerves and pain nerve fibers to produce a rhythmical muscle twitching that blocks pain through the activation of endogenous opioids. This leads to longer pain relief extending to 3 hours or more. In addition to producing muscle contractions, this technique also activates sensory nerves as seen with TENS. The summative effect of sensory stimulation immediately decreasing pain is augmented by muscle contractions that cause the release of the body’s own pain control substances, endorphins, and enkephalins. These substances chemically block pain transmission by binding to receptor sites in the nerve chain. Pain relief obtained by this method may persist for several hours following the treatment.
TENS interventions were once exclusive to the clinical setting. In addition to prescription TENS devices that are issued by health care professionals (Figure 1), the FDA has cleared a number of over-the-counter TENS devices that are now available to the public without a prescription.
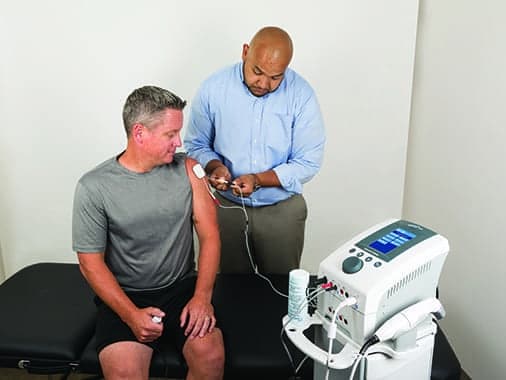
Figure 1. Application of electrodes to a painful stiff shoulder prior to active range of motion exercises and electrical stimulation using a clinical line powered device.
Topical Analgesics
Topical analgesics are readily available over-the-counter pain-relieving (or pain-masking) compounds that provide symptomatic relief. Pain reduction occurs through two mechanisms. One mechanism is blocking the transmission of pain, which is similar to that seen in TENS. The other mechanism is distracting the brain from processing the pain and, instead, focusing on the sensation caused by the analgesic.
The most common type of analgesic causes the feeling of “heat,” although no tissue temperature changes occur. Capsaicin, a compound found in hot peppers, is mixed in a cream that penetrates into the skin. Capsaicin stimulates nerve endings, creating a feeling of heat. Initially, pain may slightly worsen, but with time the nerves reduce their activity, thereby decreasing pain. Other topical analgesics contain menthol that specifically stimulate cold receptors in the skin, leading to a feeling of cold that, in some cases, is followed by a sensation of warmth. Topical analgesics may also contain an anesthetic such as lidocaine to provide longer-lasting pain relief.
Exercise
If the patient is physically able, active exercise in the form of cardiovascular routines (eg, stationary cycling, elliptical devices) and/or resistance training should be incorporated into the intervention plan.5 Active exercise produces results that are at least equally effective in reducing pain and improving function as that seen with clinician-applied manual therapies.6 Active exercises may also include yoga, tai chi, Pilates, or other position-specific exercises and movements that increase strength and flexibility, and emphasize proper body alignment and segmental movement.
Conclusion
Chronic pain is a complex and often debilitating condition. Controlling chronic pain is equally as challenging as the condition itself, often calling upon a team approach between physicians, physical therapists, athletic trainers, psychologists, and exercise specialists. However, the patient is the key player in recovery. Affecting behaviors and providing options to manage pain and reduce the reliance on medications should enhance their quality of life and, hopefully, shorten the recovery period. RM
Joseph A. Gallo, DSc, AT, PT, is a professor and director of the athletic training program at Salem State University, Salem, Mass.
Chad Starkey, PhD, AT, FNATA, is a Professor, Post-professional Program Director, and Coordinator of the Division of Athletic Training, School of Applied Health Sciences, College of Health Sciences and Professions at Ohio University, Athens, Ohio. For more information, contact [email protected].
References
1. Rizvi SJ, Iskric A, Calati R, Courtet P. Psychological and physical pain as predictors of suicide risk: evidence from clinical and neuroimaging findings. Curr Opin Psychiatry. 2017; 30(2):159-167. doi: 10.1097/YCO.0000000000000314.
2. Gatchel RJ, McGeary DD, McGeary CA, Lippe B. Interdisciplinary chronic pain management: past, present, and future. Am Psychol. 2014; 69(2):119-130. doi: 10.1037/a0035514.
3. Houghton PE, Nussbaum EL. Cryotherapy. Physiother Can. 2010;62:55.
4. Hubbard TJ, Denegar CR. Does cryotherapy improve outcomes with soft tissue injury? J Athl Train. 2004;39(3):278-279.
5. Cortell-Tormo JM, Sánchez PT, Chulvi-Medrano I, et al. Effects of functional resistance training on fitness and quality of life in females with chronic nonspecific low-back pain. J Back Musculoskeletal Rehabil. 2017. Epub ahead of print. doi: 10.3233/BMR-169684.
6. Galindez-Ibarbengoetxea X, Setuain I, Ramírez-Velez R, et al. Short-term effects of manipulative treatment versus a therapeutic home exercise protocol for chronic cervical pain: a randomized clinical trial. J Back Musculoskeletal Rehabil. 2017. Epub ahead of print. doi: 10.3233/BMR-169723.




