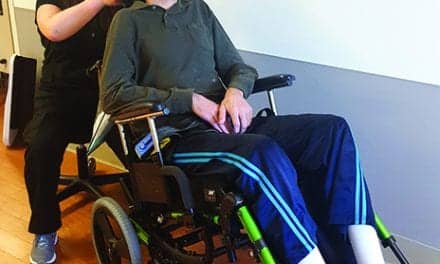
Access to the right power mobility device greatly enhances children’s physical and emotional development by allowing them to actively explore their environment.
By Sarah Murdoch, PT, DPT, ATP, and Alaena McCool, MS, OTR/L, CPAM
Children can benefit from power mobility devices in order to increase their independence within their environment, aiding in their development.
Throughout a child’s first year of life, rapid gross motor, fine motor, cognitive, and social development occurs. Gross motor development documented in research correlates with cognitive and social development. As a child learns to crawl and walk, the child also learns and sharpens his/her attention, spatial skills, and motivation.1 Independent mobility is critical for social participation, interacting with family members and peers, understanding facial expressions and gestures, as well as the non-social environment of awareness of heights, obstacles, and determining object properties.
According to a 2001 article by Hofferth and Sandberg,2 children spend 3.8 hours of their day performing physical activities and another 3.8 hours of their day involved in social participation, including peer interaction at daycare, school, or home; hobbies; and other personal activities. While navigating the environment, the child is exploring multiple solutions in various ways to achieve the overall goal of independence in their familiar environment and to build up their confidence for success in unfamiliar environments. When mobility is limited, the chance to learn and interact within their environment to experience routine and new events is also limited.
Various diagnoses may impair a child’s ability to ambulate independently throughout the developmental age range. Therapists can provide the child and parent the tools to navigate and explore their environment, as well as continue to meet developmental milestones and keep up with peers. It is important to note how this can change throughout a child’s lifetime. Power mobility is an option when there is a loss of independent mobility – from a decrease in long distance ambulation, inability to maneuver a manual chair, or inability to walk in general. Through various literature reviews, power mobility devices are advocated from an early age and highly favorable for infants. As therapists, we first must meet the child where he or she is developmentally, as well as the level of caregiver coping and ability to learn at this time. Research shows that children as early as 8 months of age have the ability to learn and adapt to power mobility, improving vocalization, arm and hand use, motivation to explore, self-confidence, and curiosity.3
The main prerequisite for the child is motivation and caregiver buy-in. However, as healthcare professionals, we also need to understand the psychosocial dynamics of the parent and/or caregiver. This includes the current level of coping and relationship between the caregiver and child. Our job as healthcare professionals is to foster and grow that relationship before any introduction to power mobility in order to ensure success. The child and/or parent may be experiencing sadness for what the child is experiencing, loss of independence, difficulties with environmental barriers, insurance issues, etc. Depending on the setting, another interdisciplinary team member, such as a social worker, may be helpful. Once we identify where the child and parent are in their stage of coping, ability to learn or hear about power mobility options, and motivation, we can begin the introduction and learning stage.
Introduction to Power Mobility
Giving a child a way to navigate his or her environment via power wheelchair options is an important step to help the young child achieve his or her own developmental milestones in a new way and still benefit from the cognitive progression. Powered devices can help the child to “explore their environment in a similar manner to their peers, helping increase play, socialization, and participation in meaningful and age-appropriate activities.”4 Early power mobility training should focus on the initiation of mobility, driving skills, development, and impact of mobility. Depending on the setting, working alongside the seating clinic team or a vendor will be helpful for identifying the type of chair for the child and allowing for trial periods.
The learning period consists of three phases. The initial phase creates a social environment for exploration, including one-on-one instruction that focuses on distinct verbal and non-verbal feedback. In this phase, trials using different drive controls will happen, as well as different setups and appropriateness of additional supports, such as laterals, trunk supports, and/or headrests. The second phase is gaining independent mobility control through power mobility and repeated training sessions in familiar environments. Once the chair is set up in a good position, the child can begin to practice in a consistent and familiar environment. Once the child becomes successful in that environment, the final phase begins. Training takes place in various environments to ensure good carryover throughout the child’s day-to-day life. This final phase can take place through practicing using the chair outside of the familiar area such as at the therapy gym, in a hallway, or trialing outside in the community.5
It is important to note that although there is currently minimal research available on the effects of power mobility on infants and young children with motor impairments, there is research available on children specifically with cerebral palsy and lack of independence in mobility relating to impaired social participation.
Powered Mobility Options
There are many considerations when choosing the most appropriate mobility device for a child. It is important to evaluate the child and discuss with the family their goals for their child’s mobility. There are varieties of different options, and family discussions are key to determine which would be the most beneficial to them in their environment.
There are programs that will adapt ride-on cars accessible by switch control. These allow the child to use a similar mobility device as their typically developing peers, while also introducing powered mobility. There are a variety of ways to activate the switch to meet the child’s needs such as at their head, hand, foot, or other position. Positioning supports can promote improved posture to facilitate the switch access. The adapted ride-on car can encourage transitions, by adapting it to operate in the desired position and to stop in the resting position. For example, when standing the car moves, when seated the car stops.
When considering a manual wheelchair, setup is important in order to protect the child’s upper extremities from overuse injuries. To provide the most appropriate setup, measurements and a comprehensive assessment are important. Power assist devices can also assist in protecting the upper extremities by reducing the number of repetitive pushes the child makes. There are varieties of different power assist devices that, with training, can be appropriate for the child. Additionally, a power add-on device can allow for joystick driving on the manual wheelchair. These options can be beneficial when transportation or home setup is not ideal for a power wheelchair.
When considering a power wheelchair, it is important to consider the different seating functions that are available. For example, a power wheelchair that is able to transition to the floor can help a child participate in floor activities without requiring a caregiver for assistance to transfer them. Seat elevation can also bring the child higher in the seated position to join their family at the table for meals or to participate in school activities at eye level with their peers as they age. Other seating functions such as tilt, recline, and elevating leg rests are important to discuss, as they are important for repositioning, pressure relief, dressing, transfers, and other activities of daily life.
Safety is a key component of powered mobility with a child. There are varieties of products that can improve safety while driving a powered wheelchair. For the caregivers, remote stops are available. This works with a small remote that the caregiver can carry. If a child encounters a situation but is not stopping or is unable to, the caregiver can push the button on the remote to stop the wheelchair. Other products can detect blind spots to avoid collisions; detect drop-offs such as curbs, uneven terrain, or sides of ramps to prevent the wheelchair from tipping; and provide visibility through a backup camera to see what is behind the child.
The Growing Child
When choosing a mobility device for a child, it is important to consider their growth. The mobility device should fit the child appropriately at the time of delivery, but also allow for changes as they grow. Working with a seating clinic can help assess when it is time for new parts or adjustments made in order to promote independence with mobility and optimal posture as the child continues to grow. It is important to document the changes for justification to funding sources. Children may also experience functional changes that require a different mobility device, seating system, or drive control depending on their diagnosis and prognosis. Being able to justify why one device is no longer meeting their needs and why a new device is necessary is also important for funding.
Conclusion
Independent mobility provides a child the ability to interact with their environment in an age-appropriate manner through play and the ability to engage with peers. Despite a mobility impairment, a child can continue to progress toward developmental milestones and social development when given the ability to navigate their own environment and give back independence to their daily routines. RM
Sarah Murdoch, PT, DPT, ATP, has been a physical therapist with the International Center for Spinal Cord Injury (ICSCI) at Kennedy Krieger Institute in Baltimore since 2012. She received her Bachelor of Biology and Health Sciences and Doctorate of Physical Therapy from Duquesne University. Her clinical interests include pediatrics, adapted transportation, and seating and mobility.
Alaena McCool, MS, OTR/L, CPAM, is an occupational therapist at Kennedy Krieger Institute within the International Center for Spinal Cord Injury (ICSCI) in Baltimore since 2018. She received her Bachelor of Arts in Communication Science from University of Pittsburgh in 2011, followed by her Masters of Science in Occupational Therapy from New York University in 2015. Her current clinical interests include pediatrics, behavioral management, and the neurologically impaired upper extremity.For more information, contact [email protected].
References
- Currier BA, Jones MA, DeGrace BW. Experiences of Families With Young Power Wheelchair Users. Journal of Early Intervention. 2019;41(2):125-140. doi:10.1177/1053815118819204
- Hofferth, S. L., Sandberg, J. F. How American children spend their time. Journal of Marriage and Family. 2001;63(2):295–308. doi:10.1111/j.1741-3737.2001.00295.x
- Livingstone R, Field D. The child and family experience of power mobility: a qualitative synthesis. Dev Med Child Neurol. 2015;57(4):317-327. doi:10.1111/dmcn.12633
- Livingstone RW, Bone J, Field DA. Beginning power mobility: An exploration of factors associated with child use of early power mobility devices and parent device preference. J Rehabil Assist Technol Eng. 2020;7:2055668320926046. Published 2020 Jun 17. doi:10.1177/2055668320926046
- Huang HH. Perspectives on Early Power Mobility Training, Motivation, and Social Participation in Young Children with Motor Disabilities. Front Psychol. 2018;8:2330. Published 2018 Jan 9. doi:10.3389/fpsyg.2017.02330