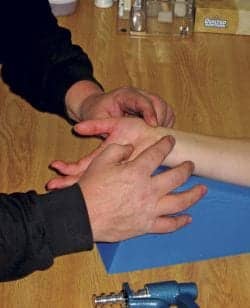
Evaluating a client’s pain and mobility should rule out certain disorders and coexisting conditions.
Photography supplied by Hand Rehabilitation Specialists and DSI Work Solutions
If you are a health professional who believes that there is little to be done for hand arthritis, think again. Osteoarthritis (OA) of the carpometacarpal (CMC), or basal joint of the thumb, is a common and sometimes disabling condition that has been found to occur in 10% of the American population aged 45 to 48 years1 and as high as 25% in postmenopausal women.2 Occupational therapists and certified hand therapists (CHTs) have an opportunity to help improve the quality of life in these individuals, who are rarely aware that there is anyone out there to help them.
Ten years ago, my colleague and I recognized the paucity of treatment being provided to this population, even by fellow CHTs. After a few years of researching the literature on anatomy, pathophysiology, treatment, and surgical procedures, we used our 43 years of combined clinical experience along with networking with colleagues to develop a comprehensive treatment approach to CMC arthritis of the thumb. A poster presentation was given at the Annual Meeting of the American Society of Hand Therapists in 2003. To date, our clinic’s experience with hundreds of clients with CMC OA has taught us that the vast majority of this population can learn to manage their pain.
The long-term goals of the program are to provide pain relief and improve hand function through a multifaceted treatment approach: splinting, modalities as needed to reduce pain and inflammation, education in abnormal pinch biomechanics, muscle rebalancing exercises (stabilization) and ROM exercises, training in joint protection techniques and adaptive equipment, and provision of community resources.3
ASSESSMENT
Evaluation of the client with pain at the base of the thumb should rule out other disorders or coexisting conditions such as carpal tunnel syndrome, deQuervain’s tenosynovitis, flexor carpi radialis tendonitis, wrist synovitis, occult ganglion cysts, thenar muscle trigger points, trigger thumb, and scaphotrapezial arthritis.
Assess the CMC joint for edema, a shoulder sign (prominence along the dorsoradial aspect of the CMC joint as a result of subluxation, osteophytes, and/or effusion), localized tenderness, pain with ligament stress, the grind test for pain with or without crepitus (rotate thumb metacarpal while providing axial compression), Evaluate A/PROM, grip and pinch strength within pain limits, abnormal pinch patterns (especially metacarpo-phalangeal [MP] hyperextension), and quality of movement.
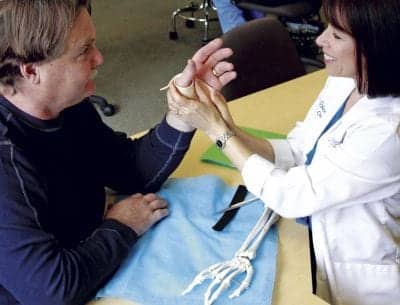
Author Laurie Champagne Roundtree, OTR/L, CHT (right), wraps James Thomas’s thumb CMC joint with a soft support.
REALISTIC GOALS
A frank discussion should take place with the client to assess their expectations verses realistic goals. They must understand that they cannot “cure” their arthritis, but they can learn to manage their pain and reduce the frequency and intensity of exacerbations. Permanent correction of subluxation is not a realistic goal, yet learning to reduce stresses to the joint will reduce the pain of subluxation. “Normal” ROM will not be regained, although they should expect less stiffness and possibly reduced progression of contractures.
PATIENT EDUCATION
Use brochures from the Arthritis Foundation to supplement your education. Describe cartilage and bony changes, the inflammatory process, typical sequelae such as CMC subluxation, CMC flexion and adduction contractures, and MP hyperextension. This sets the stage for understanding the biomechanical rationale behind the exercises and activity modification.
SPLINTING
While the adage “use it or lose it” applies to most arthritic joints, a balance between mobility and stability must be attained with the unstable or painful thumb CMC joint, where stability is primarily dependent upon ligamentous structures. Custom splinting or carefully chosen prefabricated supports are the most practical means of reducing pain and inflammation.3-5 Therapeutic taping is an occasional option.
Your assessment will help determine splint needs: include the MP if it hyperextends or is painful. If there is no MP involvement, consider a Colditz6 design with the MP free. Use a soft support such as a prefabricated neoprene arthritis thumb splint7 for the less involved client. Therapists must sharpen their skills in splint fabrication to assure that they fabricate well-fitting, comfortable, aesthetically acceptable orthoses. Thin Neoplush may be added with narrow strips of Velcro to cushion bony areas such as the dorsal first and second metacarpals. It is frequently appropriate to provide both a custom short opponens and a soft support so that the appropriate orthosis can be used based on the specific activity or the level of pain/acuity.
Splinting is generally recommended full-time for 3 to 4 weeks or until pain is minimal, progressing to night use and for stressful activities.
JOINT PROTECTION
Take the time to research and create a comprehensive joint protection handout including basic principles and tips on modifying an activity or using adaptive equipment. Be specific and give the information necessary to acquire commercial devices. Have items to demonstrate in the clinic. Use a standardized or customized activities of daily living (ADL) checklist to help you focus on each client’s needs—whether gardening, using keys and scissors, or knitting. Also, always include opening jars, bottles, and medicine containers.
Stay up to date with the products available from OT suppliers, local stores, and the Internet. Some of my favorite pieces of adaptive equipment are:
- Paint can openers to release the air seal on new jars. These can be found for less than a dollar at most hardware stores.
- Two squares of nonslip material for opening or turning almost anything: gas caps, bottles, and knobs. Place one on the counter and one on the cap for jars and medicine bottles.
- Spring-opening scissors, which are available at most craft and fabric stores.
- A keyholder “dumbbell”—a small rod, with balls at either end, that holds multiple keys and provides turning leverage.
- Electric toothbrushes and can openers.
- Cylindrical tubing to help build up the handles of such implements as knives and toothbrushes.
MASSAGE
Self-applied massage is helpful in relieving soft tissue contractures and trigger points. Use of the opposite thumb is generally not recommended due to the likeliness of current or future bilaterality of this condition. Teach safe techniques such as the following:
- Loosen the first web muscles by having the client set the hand on a tennis ball and then use the flexed PIP joint of the opposite middle finger to apply pressure to the dorsal first web;
- Use an empty roll-on deodorant bottle as a massage tool;
- Follow these soft tissue release techniques with pain-free ROM exercises.
EXERCISE
Exercise goals are to reduce pain and improve strength8-10 through the following means: maintain joint mobility, prevent CMC flexion and adduction contractures, and reeducate poor pinch patterns (typically CMC flexion with MP hyperextension and IP hyperflexion). Exercises are always performed in a pain-free range. AROM exercises include palmar and radial abduction, thumb flexion and extension, and opposition. Metacarpo-phalangeal hyperextension is always avoided. Stabilization exercises for rebalancing begin with active “place-hold” in a correct three-point pinch pattern (slight MP and IP flexion) progressing to isometric pinch and putty pinch only if the client can maintain desired biomechanics and perform without pain.
MODALITIES
For clients in significant pain, we often use modalities such as paraffin, light/laser, and/or iontophoresis with dexamethasone. Three to six sessions are often adequate when combined with the entire treatment program.
COMMUNITY RESOURCES
Many of the clients presenting with thumb OA have involvement of multiple joints throughout their body. Education about local community resources may be provided in a time-efficient manner through a simple handout. List Arthritis Foundation activities (including water and land programs), senior center offerings, and possible parks and recreation classes.
MARKETING and ADVOCACY
Consider it your responsibility to be an advocate for this undertreated patient group. Promote referrals by educating your local rheumatologists, hand surgeons, orthopedists, general practitioners, physical therapists, and chiropractors about the benefits of hand therapy for any of their clients who may mention hand arthritis or pain. In addition, show samples of splints, supports, adaptive equipment, and patient handouts. Do not forget to explain your OA program to your own clients attending hand therapy for other reasons. Leave brochures in your waiting room for clients to share with family or friends. Speak at local meetings of the Arthritis Foundation or other arthritis support groups (call your local senior center for this information). Also, the more splints and adaptive equipment that you bring, the better. Remind satisfied clients to inform their doctors of the benefits your treatment provided.
When referral sources send these clients for one visit only, be proactive in educating them about what you have to offer, and request further visits. A single visit is inconsistent with the severity and chronicity of this disorder. Even for early stage OA or synovitis, the preventive aspects of joint protection, external support, and exercise are mandatory. Advocate to the insurance carriers when necessary.
SUMMARY
Occupational therapists and CHTs have a wealth of treatment options to offer individuals with thumb arthritis. With a 10-year history using this comprehensive program, we have found that approximately 75% to 80% of our clients obtain significant pain relief; a small percentage later choose to undergo surgical reconstruction. With modifications, the program is applicable for arthritis11 in the digits as well. RM
Laurie Champagne Roundtree, OTR/L, CHT, has been practicing hand therapy for 30 years and is co-owner of Hand Rehabilitation Specialists in Thousand Oaks and Simi Valley, Calif. She is a charter member of the American Society of Hand Therapists. For more information, contact .
REFERENCES
- Pogrund H, Rutenberg M, Makin M, Robin GC, Steinberg R, Bloom R. Osteoarthritis of the hand and osteoporosis. Clin Orthop Relat Res. 1986;203:239-43.
- Armstrong AL, Hunter JB, Davis TR. The prevalence of degenerative arthritis of the base of the thumb in postmenopausal women. J Hand Surg Br. 1994;19:340-1.
- Berggren M, Joost-Davidsson A, Lindstrand J, Nylander G, Povlsen B. Reduction in the need for operation after conservative treatment of osteoarthritis of the first carpometacarpal joint: a seven year prospective study. Scand J Plast Reconstr Hand Surg. 2001;35:415-7.
- Weiss S, LaStayo P, Mills A, Bramlet D. Prospective analysis of splinting the first carpometacarpal joint: an objective, subjective, and radiographic assessment. J Hand Ther. 2000;13:218–26.
- Swigart CR, Eaton RG, Glickel SZ, Johnson C. Splinting in the treatment of arthritis of the first carpometacarpal joint. J Hand Surg Am. 1999;24:86-91.
- Colditz JC. The biomechanics of a thumb carpometacarpal immobilization splint: design and fitting. J Hand Ther. 2000;13:228-35.
- Weiss S, LaStayo P, Mills A, Bramlet D. Splinting the degenerative basal joint: custom-made or prefabricated neoprene? J Hand Ther. 2004;17:401-6.
- Veitiene D, Tamulaitiene M. Comparison of self-management methods for osteoarthritis and rheumatoid arthritis. J Rehabil Med. 2005;37:58-60.
- Rogers MW, Wilder FV. Exercise and hand osteoarthritis symptomatology: a controlled crossover trial. J Hand Ther. 2009;22:10-18.
- Boustedt C, Nordenskiold U, Nilsson AL. Effects of a hand joint protection programme with an addition of splinting and exercise. Clin Rheumatol. 2009;28:793-9.
- Valdes K, Marik T. A systematic review of conservative interventions for osteoarthritis of the hand. J Hand Ther. 2010;23:334-351.





