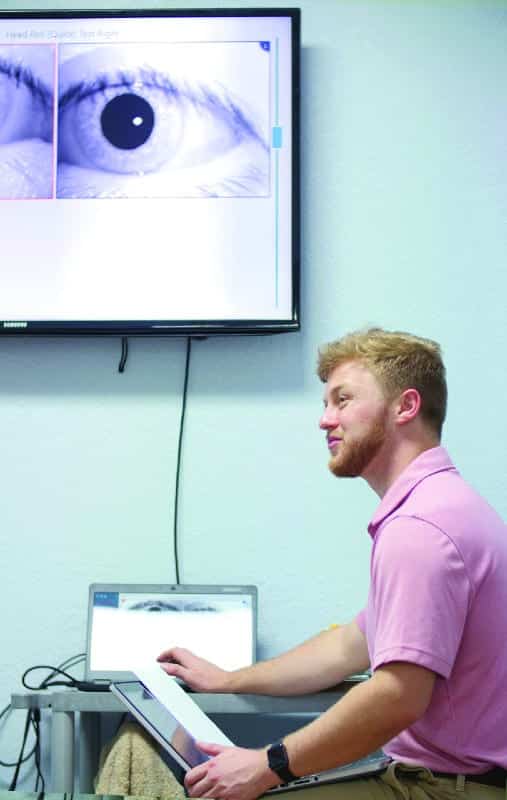
photo caption: Visual assessment being performed by a physical therapist.
by Matthew Aguilera, DPT, PT, Denise Campbell, PT, ATC, Dip. MDT, FAAOMPT, OCS, and David Gallegos, MA, ATC, Cert. MDT
You’re getting ready to discharge your patient who came to you for back pain and as you pull them back for the last time, you notice their unsteady gait and they say to you, “My back is doing great, but lately I’ve been feeling dizzy and fearful of falling.” Now, you wonder, “Is this person safe for discharge?” The clear answer is, “No,” assuming their dizziness and imbalance is amenable to physical therapy (PT). Luckily, your investment in vestibular rehab therapy (VRT) allows you to make that decision.
The vestibular system, located within the inner ear, is responsible for detecting spatial orientation and linear/angular acceleration. The information gathered is then transmitted to the central nervous system and musculoskeletal system to make appropriate postural adjustments to remain upright and stable. Problems arising within this system often manifest as dizziness, imbalance, visual disturbance, and/or disequilibrium. Evidence has shown VRT to be effective in improving many vestibular disorders.1,2 According to the National Institute on Aging and disturbances of the inner ear causing imbalance are among the most common reason older adults seek help from a doctor.3 The purpose of this article is to highlight the opportunities afforded by the “dizzy and/or imbalanced patient.”
Determining the Cause of Dizziness and Imbalance
Symptomatology of the “dizzy” patient is oftentimes difficult for the patient to verbalize. Utilizing bedside testing and various technologies in the industry, the vestibular-trained therapist can conduct a series of tests to aid in the diagnosis of each individual’s cause of symptoms to determine a central or peripheral origin and/or balance impairment.4 Beyond aiding in diagnosis, these technologies can be used for patient education, comparative data, designing individualized programs, and reimbursement justification. Furthermore, the therapist may utilize these technologies to help rule in or out the presence of red flags, which would warrant the need for referral to the appropriate provider.
As physical therapists lobby to gain more presence in direct access, it is important to be able to determine when it is appropriate to treat a patient or refer them based on signs and symptoms. Complaints of dizziness has been shown to account for up to 11% of emergency department visits.5 According to Navi et al, 47 out of the 907 cases (5%) that presented to the emergency department for complaints of dizziness were of serious neurologic pathology.6 Most cases were of benign peripheral origin. Including a vestibular program within your practice to evaluate and treat the dizzy or imbalanced patient allows for a potentially large expansion of your clientele, both from a direct access and referral-based standpoint. Having a sound understanding of evaluating dizziness can streamline the care your patients deserve — reducing the overall cost of care for your patients and the medical system overall, thereby garnering trust within your community.
Benign Paroxysmal Positional Vertigo
Vertigo and dizziness are often used interchangeably; however, positional vertigo is a mechanical issue within the vestibular system involving otoconia (famously known as ear crystals). Benign paroxysmal positional vertigo (BPPV) will be highlighted as it has been shown to be the most common cause of vertigo involving inner-ear issues.7 With positional vertigo, the otoconia become improperly placed within the semicircular canals, changing the dynamics of the fluid-filled canals and its resultant sensory interpretation. This is recognized by the patient and usually described as “spinning” with certain positions of the head. Treating BPPV is extremely rewarding as it has been shown to be highly effective.8
Successful treatment of BPPV lies within the ability to correctly identify the location of the otoconia within the vestibular system as this changes the treatment approach. Utilizing Frenzel lenses or video oculography enable the practitioner to identify nystagmus with more ease as this prevents the suppression of nystagmus and allows for magnification of the eyes and/or playback of the nystagmus. Ultimately, the therapist must determine the sidedness of the issue, which canal is involved, and differentiate between canalithiasis or cupulolithiasis as these help determine the most effective treatment approach.
Successful treatment of vertigo often results in patients who are amazed and wonder, “Is that it?” Following a series of diagnostic tests and failed pharmaceutical management, your treatment alleviated their dizziness. They subsequently inform their doctor and family friend who is also dizzy, and you earn the reputation as the “dizziness person” in your community.
Stats on Falls and Population of United States
The statistics regarding older adults and falls are no secret. According to the Centers for Disease Control and Prevention (CDC), slightly more than one out of four older adults fall each year, resulting in the most common cause of fatal injuries amongst older adults.9 The CDC projects the financial toll of falls will increase as the older population increases — reaching about $67.7 billion by 2020 with Medicaid and Medicare shouldering 75% of these costs.9 Furthermore, by 2030 all baby boomers will be of retirement age, thereby expanding the older population. It is projected that 20% of the US population will be of retirement age and will for the first time outnumber children.10 The growth of the older adult population presents an opportune market for physical therapists.
Falling does not need to be considered a “normal” part of aging. The profession is equipped with the ability to determine falls risk and treat it accordingly. The typical approach is multifactorial, including medical management, vitamin supplementation, and strength/balance exercises. The implementation of a vestibular program within practice enables the skilled therapist to delve deeper into each individual’s ability to utilize and integrate the three systems of balance (somatosensory, visual, and vestibular) and treat the individual accordingly as opposed to a cookie-cutter approach to imbalance. The general outpatient setting will likely see the number of older adult patients increase, thereby comprising a large portion of your caseload. Are you screening your older adults, regardless of their primary complaint, for their risk of falls?
Vestibular Therapy in Sport
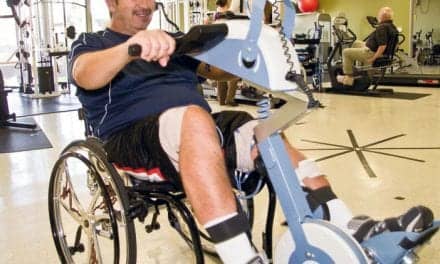
Vestibular therapy is not just for the older adult. Athletes of all ages can benefit from a vestibular training and balance program to improve overall performance, injury prevention, and rehab management. A balance program can benefit the injured and non-injured athlete alike, improving neuromuscular control of the extremities, dynamic stability, hand-eye coordination, and gaze stabilization. Utilizing the same technology previously discussed, the practitioner can obtain baseline results pre-season/training and periodically throughout the therapy/training program to assess improvement or to establish return-to-sport criteria. Of interest includes obtaining baseline dynamic posturography, dynamic visual acuity, and central/peripheral screens for vestibular abnormalities. The obtained data can then be relayed to the athlete and all those involved in the athlete’s care to establish need for therapy pre-injury/season or used as criteria for safe return-to sport following an injury.
Concussion in sports has gained attention both in academia and the media, thereby raising awareness. Dizziness following a concussion occurs in about three-fourths of cases and has been shown to delay recovery.11 Though post-concussion syndrome involves a multi-disciplinary approach to care, physical therapy can examine the vestibular system and oculomotor function to help determine contributing factors to symptoms and help tailor the individual’s program. Furthermore, according to a study performed at the University of Wisconsin-Madison, concussed athletes are almost 2.5 times more likely to sustain a lower extremity injury during the acute phase of returning to sport in collegiate athletes.12 Utilizing the information obtained from this exam, the therapist can develop a tailored program to reduce both symptoms and risk of re-injury.
Vestibular retraining exercises do not have to be included only in the return-to-sport phase of recovery. Though most pre- and post-op protocols do not mention vestibular retraining exercises in the early phases, these can easily be implemented within the program so the athletes do not lose their gaze stabilization and coordination skills. Have you considered performing a bedside vestibular exam to determine underlying weaknesses that can also be treated with the recovering athlete? Including vestibulo-ocular reflex activities in your rehab program can help maintain these skills the superior oculomotor function often observed in elite athletes.13 Providing these evaluations and treatments help establish rapport with parents, coaches, doctors, etc, thereby furthering your outreach and presence in your community.
Conclusion
The purpose of this feature was to highlight the opportunities afforded by including a vestibular program within your practice. Though the majority of patients who complain of dizziness/imbalance are among the older population, these symptoms are not exclusive to this group and can extend across the lifespan. The idea that physical therapy can treat dizziness is not well-known among the general population. However, this is well within our scope of practice, and our profession has been shown to be effective in treating this symptomatology. RM
Matthew Aguilera, DPT, PT, is a physical therapist at FYZICAL Therapy & Balance Center in Las Cruces, NM. He is a 2018 graduate of the physical therapy program at the University of Madison-Wisconsin holding advanced certification in vestibular therapy.
Denise Campbell, PT, ATC, Dip. MDT, FAAOMPT, OCS, is the owner and CEO of FYZICAL Therapy & Balance Centers in Las Cruces, NM, and El Paso, Texas. She is a 1982 graduate of the physical therapy program at Texas A&M holding advanced certification in vestibular therapy.
David Gallegos, MA, ATC, Cert. MDT, is the Deputy CEO and Director of Sports Medicine for FYZICAL Therapy & Balance Centers in Las Cruces, NM, and El Paso, Texas. He is a 1997 graduate of the Athletic Training program at New Mexico State University holding advanced certification in vestibular therapy. For more information, contact [email protected].
References
- McDonnell MN, Hillier SL. Vestibular rehabilitation for unilateral peripheral vestibular dysfunction. Cochrane Database Syst Rev. 2015 Jan 13. doi: https://www.doi.org/10.1002/14651858.CD005397.pub4
- Herdman SJ. Vestibular rehabilitation. Curr Opin Neurol. 2013;26:96-101.
- National Institutes on Aging. Balance Problems and Disorders. Available at: https://www.nia.nih.gov/health/balance-problems-and-disorders. Accessed February 22, 2020.
- Kreinbrook, Susan. Vestibular Therapy: Finding Balance Through Evaluation. 4/5/2018. https://rehabpub.com/conditions/neurological/brain-injury-neurological/vestibular-therapy-finding-balance-evaluation/
- Lammers W, Folmer W, Van Lieshout EM, et al. Demographic analysis of emergency department patients at the ruijin hospital, shanghai. Emerg Med Int. 2011: 748274. doi: https://www.doi.org/10.1155/2011/748274
- Navi BB, Kamel H, Shah MP, et al. Rate and predictors of serious neurologic causes of dizziness in the emergency department. Mayo Clin Proc. 2012:87(11):1080-1088.
- Katsarkas A. Benign paroxysmal positional vertigo (BPPV): idiopathic versus post-traumatic. Acta Otoaryngol. 1999;119(7):745–749.
- Helminski JO. Effectiveness of the canalith repositioning procedure in the treatment of benign paroxysmal positional vertigo. Phys Ther. 2014;94(10):1373–1382. https://www.doi.org/10.2522/ptj.20130239.
- Bergen G, Stevens MR, Burns ER. Falls and fall injuries among adults aged ≥65 years — United States, 2014. MMWR Morb Mortal Wkly Rep. 2016;65:993–998. doi: http://dx.doi.org/10.15585/mmwr.mm6537a2.
- United States Census Bureau. Older People Projected to Outnumber Children for First Time in US History. 3/13/18. Release Number CB18-41. https://www.census.gov/newsroom/press-releases/2018/cb18-41-population-projections.html.
- Valovich McLeod TC, Hale TD. Vestibular and balance issues following sport-related concussions. Brain Inj. 2015;29(2):175-84. doi: https://www.doi.org/10.3109/02699052.2014.965206.
- Brooks MA, Peterson K, et al. Concussion increases odds of sustaining a lower extremity musculoskeletal injury after return to play among collegiate athletes. Am J Sports Med. 2016;44(3):742-747. doi: https://www.doi.org/10.1177/0363546515622387.
- Massingale S, Alexander A, Gerkin R, et al. Gaze stability in the elite athlete: A normative observational study. J Vestib Res. 2019;29(5):221-228. doi: https://www.doi.org/10.3233/VES-190678.





My little sister was playing in a regional high school tennis match yesterday, and while she was serving she got so dizzy that she had to forfeit the match. She is thinking about getting vestibular therapy, and I didn’t realize how many benefits this type of therapy can have! Thank you for explaining that through new technology and testing, a therapist will be able to help my sister find out the cause of her dizziness.
I’m glad the article was helpful to you, Rosie. My best wishes to your sister on her journey to recovery.
—Ed.