Combining high- and low-tech approaches to enahance outcomes in gait and balance training and assessment
by Beth Salvo Myers, MSPT
 Technology has infiltrated almost every aspect of our daily lives. It is not surprising that it also has made its way into our therapy clinics. Technology offers new ways to measure what was previously subjective, and simultaneously provide ways to increase effectiveness of treatment. As physical therapists, we often get referrals for gait and balance training, with the obvious rationale for fall prevention. There is a plethora of techniques employed to address and measure these functional impairments, most of them “low tech.” Assessment and treatment aim to improve functional skills, mostly for the patient’s safety and prevention of falls. Falls are the leading cause of injury and death in adults, and are due to physical and environmental factors. Poor balance and weakness are contributing factors to falls.1 While objective, standardized measures provide good data for insurance companies and for treatment planning, technology has allowed us to take this further.
Technology has infiltrated almost every aspect of our daily lives. It is not surprising that it also has made its way into our therapy clinics. Technology offers new ways to measure what was previously subjective, and simultaneously provide ways to increase effectiveness of treatment. As physical therapists, we often get referrals for gait and balance training, with the obvious rationale for fall prevention. There is a plethora of techniques employed to address and measure these functional impairments, most of them “low tech.” Assessment and treatment aim to improve functional skills, mostly for the patient’s safety and prevention of falls. Falls are the leading cause of injury and death in adults, and are due to physical and environmental factors. Poor balance and weakness are contributing factors to falls.1 While objective, standardized measures provide good data for insurance companies and for treatment planning, technology has allowed us to take this further.
Most physical therapists think of balance as multifactorial, and it is highly correlated to any type of functional mobility. There exist many reliable, low-tech, standardized measurement tools, such as the Berg Balance Scale and Timed Up and Go, which may effectively show progress. But there are also computerized balance systems on the market that can give quantitative data about one’s ability to maintain standing balance. This improves the therapist’s ability to show improvement numerically, which is important for goal setting and reimbursement. It also provides immediate feedback to the patient about performance, providing motivation and kinesthetic awareness. At Kennedy Krieger Institute’s International Center for Spinal Cord Injury, sitting and/or standing balance is part of just about every person’s plan of care. Improved balance means less chance of falls. It also means the difference between independence versus requiring a caregiver.
Integrating Technology to Engage and Streamline Recovery
Use of technology in addressing balance deficits can bring another important component that increases patient engagement: fun. At the center, we have found that it is not only children who will work harder when these methods are used, but the same is true for our adult and elderly population. The use of computerized/video games gives all the components required for engagement and learning, such as realtime feedback (biofeedback), reward systems, and dynamic conditions. The use of computerized games2 has been well documented in therapy literature, and there are many that are accessed via a hand controller, a sensor board, or visual scanning, to pick up on the individual’s movements. We have adapted these for use while sitting or in a supported stander. We also employ the use of a sailing simulator. Patients transfer into a boat connected to a computer screen, which requires the patient to maneuver around dinghies while taking into account the angle of their sail and the wind. Hydraulics on the stationary boat mimic the lateral sway, thus increasing the demand on core muscles to maintain balance. Some of our patients have then gone on to join an adaptive sailing program in our area.
Gait is made up of several complex mechanisms, in which balance plays a large role, specifically in safety during gait. There are several low-tech assessment tools that measure balance and efficiency of walking, including the 10-meter walk test, the 2-minute or 6-minute walk test, and the Dynamic Gait index. A technologically advanced and effective means for analyzing gait is the use of computerized gait mapping. This consists of an approximately 20-foot-long mat with imbedded sensors, connected to a computer program. Through this system, it is possible to obtain quantitative and comparative data about one’s gait. Several parameters can be given numeric value, which is useful in demonstrating improvement and rationale for therapy, goal setting, and justification for services. Many systems also can provide normative data for a patient’s age. When using gait mapping as part of an initial evaluation, it is interesting to note symmetry of gait as indicated by the numbers. In addition, different conditions can be trialed and compared to one another: different types of bracing, or bracing versus no bracing, comparing performance between different assistive devices, or between verbal cues, such as “walk as fast as you can” or “walk at your normal speed.” At reevaluation, it is exciting to compare and see improvements in such areas as cadence, velocity, symmetry, step and stride lengths, and percentage of gait cycle spent in stance or swing. Being able to show improved gait efficiency is powerful supporting data for the justification of ongoing therapy. Some programs also offer the ability to review a trial, in real time or slow motion, to view how pressure is distributed through the foot during a step. This can assist with brace prescription. There may also be the option to video a trial, which can be saved with its respective mapping representation.
Low-Tech Approaches for High- Quality Patient Outcomes
To address gait deviations, there are several approaches that do not require technology, but an understanding of how impairment relates to function. Low-tech approaches include pregait activities or breaking an activity down into smaller components, neurofacilitory approaches, and traditional strengthening. At the International Center for Spinal Cord Injury, we use many standard low-tech approaches to addressing gait impairments, coupled with use of functional electrical stimulation (FES). Use of FES for anterior tibialis activation has been well documented in the literature, for patients with any diagnosis that may cause foot drop. There are calf cuff devices that provide stimulation to the anterior tibialis, using a variety of mechanisms to trigger the stimulation automatically during gait. We also use FES for any weakness that may be associated with gait deviations, in any lower extremity muscle. There are some FES devices that allow a wide range of parameter selection and real-time muscle stimulation, with use of a trigger. FES increases muscle fiber recruitment and sensory awareness to get more impact from a functional, therapeutic activity.
Vibration plates have come into vogue recently, and there has been considerable research produced about the use of whole body vibration. There are vibration plates that provide vertical, lateral, or multiaxis motions. There does not seem to be any definitive research at this point about which has the most benefit. At the center, we have the ability to mount our vibration plate to a supported stander for people who may have trouble standing on it safely and independently. Whole body vibration can offer the benefits of modulation of spasticity, and has been shown to improve walking function by increasing cadence, step length, and walking speed in patients with spinal cord injury.3 Other research, on normal subjects, has shown improvements in bone density, muscle strength, and gait symmetry.
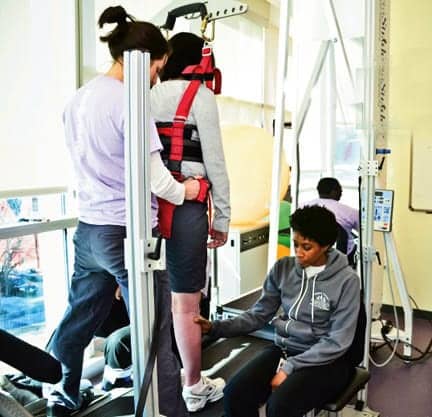
Body weight-supported treadmill systems are used to decrease the effect of gravity on the patient during walking and standing, while applying the principles of locomotor training.4 This enables the patient to practice “normal” gait mechanics, thereby optimizing the nervous system for performance over ground. Patients use muscles and neuromotor circuits in a functional way, with manual assistance as needed—with the goal of more independent walking. Body weight support and speed of the treadmill are adjusted via computer, depending on the goals of the session and the functional level of the patient. Sessions are recorded in the attached hard drive; therefore, incremental change and progress can be demonstrated over time. Assistance level is implied through the amount of body weight support that the patient requires to walk at a given speed. This is impressive supporting evidence for insurance justification. There are also a few body weight support systems on the market that function over ground, using a track system. Because they are not connected to a computer, there is no ability to collect data. For both types of devices, the patient is tethered to the ceiling using a harness, engineered to make the system completely safe. This is also an excellent environment to perform higher level standing balance activities safely, between bouts of walking.
Aquatic Assessment
Aquatic therapy is not a new technology, but is effective in challenging balance and gait training in a safe environment. The facilities in the aquatic therapy center at Kennedy Krieger Institute allow the level of the water to be adjusted, via height-adjustable floors, according to the patient’s level of function—shallower increases gravity’s effect, deeper decreases it. Similar to the body weight support treadmill system, gait training over an aquatic treadmill also has the benefit of adjusting the effect of gravity on the patient. There are also jets in the wall of the pool, to provide balance perturbations and challenges. The pool’s underwater cameras provide anterior and lateral views, which project to screens at the patient’s eye level, giving real-time feedback about performance, and allowing the aquatic therapist to effectively cue the patient or adjust water height or treadmill speed. Many patients have taken their first steps, with the use of this technology, which has been a true landmark in their rehabilitation.
Technology has given us an extra advantage to evaluate and address balance and gait impairments, thus assisting us in decreasing patient risk for falls. It has allowed us to make therapy more reimbursable due to the availability of objective data, and has improved the efficacy of our treatment planning and goal setting. It also increases patient participation, due to the “fun” factor and the ability to demonstrate improvement to the patient, as motivation. RM
Beth Salvo Myers, MSPT, is manager of therapy services at the International Center for Spinal Cord Injury at Kennedy Krieger Institute, Baltimore. She has worked with patients with spinal cord injuries, pediatric and adult, over the past 10 years. For more information, contact [email protected].