 |
| Thomas “Ted” Dreisinger, PhD, FACSM |
There is a curious battle playing out among decision-makers who must guide fitness equipment purchases for rehab centers. On one side of the conflict is strong support for purchase decisions built around low-cost, low-tech basics. On the other side, counterintelligence instructs wise money to invest in systems that are impressively advanced.
Somewhere between the two philosophies, perhaps, lies a hint that either approach can create a fiduciary advantage—so long as a facility’s overarching purchase strategy plays to the strengths of its user population.
CHOOSE YOUR WEAPON
“Balls, bands, and tubing: we make a living off of that stuff,” says Chris Graham, MPT, OCS, co-owner of Sports Medicine Institute (SMI), Los Angeles. Graham says basic equipment that never strays far from the fundamentals—and can be had for a handful of cash—plays a significant role in therapy programs at SMI.
“Those little tools are the things that get it done,” Graham says, noting that the 3,000-square-foot facility that serves a largely orthopedic rehabilitation population also hosts a clinical reformer, multi-hip machine, ergometers, and several more sophisticated devices.
“You have one ball in the clinic, for example,” Graham says, “and that one ball can serve a lot of people in one day.”
Graham believes good therapy does not hinge on pricey gear, and he extols the creativity therapists can use to work with low-tech solutions to frame easily understood exercise programs designed for home use. Portability and ease of use, Graham says, create hooks that get clients to buy into critical “homework” programs.
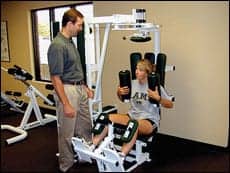 |
| A physical therapist (left) oversees a client’s use of a torso rotation machine. |
“For a client who needs to strengthen something, I can provide a resistance exercise that can be modified many different ways using just basic equipment,” Graham explains, “whether it’s versus gravity or versus a band. You tell a client, ‘If you had this ball, you could do these 10 exercises that we’ve learned here at home.’ This way they can afford to purchase the items themselves, keep consistent, and stimulate the program.”
Graham also considers simple weights go-to equipment, and points out how effectively they remove access barriers for clients willing to work out at home. Graham says free weights can be introduced in-clinic to therapy programs such as those targeted to rotator cuffs—allowing clients who own their own weight sets to work with equipment with which they already are comfortable.
The most basic technologies for fitness equipment may seem practical because of their simplicity and “less is more” appeal. However, some facility directors say the devices fail to capitalize on the human need for accomplishment.
STRENGTH IN NUMBERS
“Let me ask you a question,” says Thomas “Ted” Dreisinger, PhD, FACSM, research coordinator for the US Spine and Sport Foundation in San Diego.
“When you’re doing something, and you can see progress, does that incite you to do more?” Dreisinger asks.
Low-tech equipment can certainly build strength, Dreisinger quickly acknowledges. But he points that in many cases appreciable gains in functional strength are perceptible only to individuals who already are accustomed to exercise. For those who are new to working out, Dreisinger says, an inability to measure progress can lead to a feeling of disenfranchisement.
“Let’s say we’ve got 10 machines and the client lifts 100 pounds 10 times on each machine. That client has just moved 10,000 pounds in 20 minutes,” Dreisinger says.
“If you let a client know he’s just lifted the equivalent of three elephants off the ground in a space of 20 minutes, the way that client thinks about what he’s done is radically different from what it would be if he weren’t able to track his work,” Dreisinger adds.
Adding as little as 2 pounds to a machine can significantly increase a client’s total workout load, creating tangible progress that can be measured and relayed back to the client—solidifying how that client connects with the therapy program.
“In my clinical experience,” Dreisinger says, “this is a phenomenon that goes unnoticed.”
Current technology allows client workout information to be collected through on-board or add-on devices available with equipment such as pneumatic weight trainers, cable machines, and recumbent steppers. Data from this hardware includes statistics for resistance levels, distance, and speed among many other performance indicators. Connectivity to heart monitors or other external sensors is also standard equipment on many of these systems.
Graham, whose father is a PT and previously owned two outpatient rehabilitation clinics, recalls the rush to purchase isokinetic dynamometers in the 1980s. Graham questions the net benefit of the bells and whistles available on current technology.
“We’re a manual and exercise-based facility,” Graham says. “For our little clinical model, those machines where people put in a card and it keeps track of their program are sort of the opposite end of the spectrum.
“Everything we do is geared toward functional outcome. A person comes in and wants to know, ‘Can I raise my arm?’ Well, a person doesn’t need all of this technology to accomplish that,” Graham says.
FOLLOW THE MONEY
The distance Graham maintains from high-tech fitness systems stems less from an aversion to Reagan-era isokinetic behemoths than a nagging question of economics.
“If we’re just doing therapeutic exercise—a knee extension, for example—whether I’m doing that extension versus sandbag weight, regular knee extension machine, or even manual resistance, those all get paid the same. If my machine cost me $40,000, I don’t see where you make that up,” Graham says.
Dreisinger adds up the numbers differently.
Dreisinger points out that clinicians log data from therapy sessions as a matter of course, and whether clients enter information about workouts themselves, or turn the information over to facility staff to enter, the particulars of a client’s therapy assignments must nonetheless be recorded.
“Let’s say it costs me $5,000 to outfit 10 machines so they will handle a data chip,” Dreisinger explains. “And let’s say it takes a staff member 30 minutes per day to enter all my clients into a system.
“Figure out what it costs to pay that staff member entering that data, and I guarantee that $5,000 it cost to install the data logging is recovered pretty quickly,” Dreisinger says. “With amortization over 5 years, I’ll spend way more on data entry than I will if I’ve got that chip.”
THIGHMASTER ET AL: THREAT OR OPPORTUNITY?
Consumer fitness equipment manufacturers have targeted home users almost since there have been celebrity endorsers willing to peddle the goods. As consumer gear continues to be directly marketed, the question persists over how the proliferation of fitness equipment inside homes impacts the flow of clients into rehab facilities.
Robert Medcalf, PT, director of spine rehabilitation for Resurgens Rehabilitation Services, Atlanta, observes that some clients who own their own fitness equipment do not understand how to properly use the devices. Medcalf, who is also a member of the teaching faculty for the McKenzie Institute, suggests an opportunity exists for clinicians to instruct clients who own their own equipment on how to use the equipment properly, under the controlled environment of a therapy facility.
“Much of our clientele tends to have home equipment—stationary bikes, treadmills, and now elliptical trainers; they’ve kind of created their own home gyms,” Medcalf explains. “And once we get their condition under control, we’ll confer with the client about how to give them guidance for the safest way to utilize those pieces of equipment with whatever condition they may have.”
Dreisinger senses little cause for therapy clinics to be alarmed by the proliferation of home trainers. The number of bikes and treadmills hawked at local garage sales, he says, addresses the threat directly: “Most people will exercise on that equipment at home for only about a month. Then it sits in the basement.”
 |
| A physical therapist (left) directs her client’s use of a lumbar extension unit, which measures and strengthens lumbar extensor muscles in isolation. |
GOING THE DISTANCE
What seems to unite the schools of high-tech and low-tech is the value each camp puts on a device’s versatility. And versatility can be quantified, Dreisinger says, by treating virtually every piece of exercise equipment as a profit center.
“You don’t buy equipment for a specific population,” Dreisinger asserts. “You buy equipment you can use as many ways as possible with the construct that you’re going to adapt it to special populations.”
Dreisinger suggests facilities that specialize in serving physically disabled clients should build adaptability into their exercise equipment, allowing the devices to be easily reconfigured for use with other populations.
Paraplegics, for example, Dreisinger says, often have good upper-body potential and can build strength by using modifiable machines that perform lateral pull-down, chest press, or rowing. Quadriplegics, too—depending on their level of involvement—can use adapters to allow them to grab hold of certain types of equipment, Dreisinger says. Devices such as arm cranks, he adds, can be made accessible to quadriplegics by applying adaptive hand clasps.
User bases can be extended further to neurologic populations, who Dreisinger says respond well to activities that help build strength. He suggests that rehab directors can service this population by identifying ways to adapt equipment to the level of the person who is doing the work.
Equipment can also be made compatible with amputee populations, according to Dreisinger, who says that if a director consults with a prosthetist prior to an equipment purchase, programs can be designed for both upper and lower extremity amputees that will help grow the overall population that uses a single piece of gear.
But before making any purchase, Dreisinger advises a hands-on assessment should be made by a facility director, trusted staff member, or qualified consultant.
Graham enthusiastically agrees.
“I want to feel the quality of the motion and the ease of adjustment for my fitness equipment,” Graham says. By design, his purchase decisions take into consideration the facility’s subset of Medicare clients who overlap with SMI’s primarily sports-centric clientele. Graham says if a piece of equipment is difficult for him to use, the “little old ladies” taking therapy at SMI will find the device virtually impossible to use.
“Equipment has got to be simple,” Graham says. “It can’t be something that requires you to adjust four different controls and then read something in between.”
COUNT BEANS OR ROLL THE DICE?
Like many clinic owners, Graham laments the drop in Medicare reimbursements that occurred July 1. “And the cap is back in place, which limits what you’re able to do with all these cases,” he says. “People like me will likely slow down and hold back on our purchasing in the coming year.”
Medcalf, like Graham, feels near-term fitness equipment purchases at his Atlanta facility may also be reined in. “So far nothing has been denied, but we may be in for some belt-tightening,” Medcalf says. In the interim the facility plans to get the most out of the equipment it already has by mechanically maintaining the devices and keeping up maintenance contracts, he says
In an environment with a teetering economy and downsized reimbursements, however, Dreisinger sees an opportunity.
He suspects a nationwide uptick is occurring among clients who feel forced by economics to cancel their therapy sessions. As Dreisinger sees it, however, current market conditions actually work to enhance a director’s buying position.
“I’m betting consumer-driven health care is going to be huge. I’m betting that cash payment for medical fitness is going to be huge. Right now, the market is down, so [it would be a good time to buy] equipment, absolutely.”
Dreisinger predicts the costs for fitness equipment will become much more competitive over the next 5 to 7 months, which, he says, will open a window of opportunity for purchasers to bargain for better prices.
“I would offer less and try to get good deals,” Dreisinger says. Then he adds: “I’m a risk-taker though, and I think a lot of people are not.”
Frank Long is the associate editor of Rehab Management. For more information, contact .





