|
| Brian F. Hagen, DPT, MS, PT, OCS, FAAOMPT (right), confers with patient Broc Hepler. |
The Pittsburgh Steelers can credit their 2006 National Football League Super Bowl victory to a powerful offense, a sterling defense, outstanding coaching, and excellent morale among the players—plus one thing more: unsurpassed musculoskeletal care delivered by the team’s official sports medicine provider, the University of Pittsburgh Medical Center (UPMC) and that institution’s Center for Sports Medicine.
Helping professional athletes achieve optimal performance has been the name of the game at the UPMC Center for Sports Medicine since 1986 (the enterprise celebrates its 20th anniversary this July). In addition to serving as the official rehab providers for the Pittsburgh Steelers, the center works with two other professional sports teams—the Pittsburgh Penguins (hockey) and the Pittsburgh Riverhounds (soccer), as well as the semiprofessional Washington Wild Things (baseball) and, of course, the teams from the University of Pittsburgh. But the list of names passing through the center’s portals is not confined to the superstars of the world of sports. Also coming under its care are a number of dance troupes and some 46 area high schools’ student athletes, not to mention a huge cohort of “weekend warriors.”
“Of the patients we see, approximately 45% are recreational athletes, but we pride ourselves on treating every patient—whether a star athlete or an ordinary Joe—with the exact same intensity and vigor,” says program administrator and facility director Brian F. Hagen, DPT, MS, PT, OCS, FAAOMPT.
The UPMC Center for Sports Medicine—operating on an annual budget of roughly $6 million—handles between 70,000 and 75,000 patient visits each year (that works out to about 450 patients a day), according to Hagen, who also serves as regional director of the UPMC Centers for Rehab Services (a separate but affiliated entity that handles the sports medicine center’s rehabilitation component).
Freddie H. Fu, MD, chairman of the Department of Orthopaedic Surgery at the University of Pittsburgh School of Medicine and a founder of the UPMC Center for Sports Medicine, acknowledges that many sports medicine centers around the country conduct top-notch programs, but believes his remains unique in several respects. “Ours is a one-of-a-kind facility that allows us to take sports medicine to the highest level in order to meet the growing demands for a wide range of services, including comprehensive sports injury and rehabilitation services,” he says. “We were also the first of its kind in the United States to have the resources of a major academic and clinical system with professional and collegiate sports team programs.”
 |
| Center cofounder James J. Irrgang, PhD, PT, ATC (right), evaluates patient Nicholas J. Torquinio. |
Or as center cofounder James J. Irrgang, PhD, PT, ATC, puts it, “We’re combining clinical practice with academic medicine; because of our particular approach, our physical therapists have abundant opportunity to interact with orthopedic surgeons who are on the cutting edge, which exposes the therapists to all the newest surgical procedures and enables them to participate in some rather exciting research.” Taken as a whole, “there is much here that allows us to attract and retain some of the country’s best physical therapists,” says Irrgang, a UPMC Centers for Rehab Services physical therapist and director clinical research in the Department of Orthopaedic Surgery at the University of Pittsburgh.
The UPMC Center for Sports Medicine started out small, but in 2000, growth propelled it into its current home in a complex spread across six acres. On that parcel are situated three buildings. One is occupied by the UPMC Center for Sports Medicine, the second is shared by the Pittsburgh Steelers and the University of Pittsburgh’s own football team (both squads’ training facilities are there), while the third is an indoor football practice field. (Also on the grounds are a quartet of outdoor practice fields.) “The entire complex was built and paid for by UPMC, and the space used by the Steelers and Pitt is provided to them on a lease arrangement,” Hagen explains.
Adds Fu, “The complex is used as a model in more than 15 countries and has been a magnet for more than 400 visiting surgeons and fellows from five continents, including a contingent from Beijing preparing for the 2008 Summer Olympic Games.”
The two-story, 36,000-square-foot building in which the UPMC Center for Sports Medicine is housed contains administrative and research offices upstairs, while the ground floor is devoted to clinical services. “We run a number of different entities from our building,” Hagen says. “We have our physician group, headed by Dr Fu. We have radiology—which includes two x-ray suites and an open MRI unit. We have a biomechanics and musculoskeletal research lab. And there is a 10,000-square-foot gym, part of which is sectioned into an open-bay treatment area with 23 tables. For those who prefer privacy, we have eight sequestered treatment rooms.”
As to employees, 190 clinicians and administrators work at the UPMC Center for Sports Medicine—including 60 athletic trainers (they are assigned to the 46 high schools), 18 physical therapists, three physical therapist assistants, eight technicians, seven orthopedic surgeons, four performance specialists, two primary care sports medicine physicians, one nutritionist, and a sports psychologist. “We have a great team of experts, and they work together cohesively to ensure that each patient progresses well and swiftly from injury state through the proper channels until he or she returns to activity,” says Hagen.
EMPHASIZES HANDS-ON APPROACH
Cruciate ligament damage leads the pack as the UPMC Center for Sports Medicine’s most frequently encountered sports injury. However, overuse injuries are coming up fast from behind.
“A surprise is that we’re seeing more and more of these overuse injuries in children,” says Hagen, who additionally holds clinical assistant professor posts at the University of Pittsburgh and in the School of Health and Rehab Sciences divisions of Duquesne University. “Youth athletic organizations typically have rules that prohibit, for instance, pitchers from being on the mound for more than x-number of innings or games per week. Those rules are intended to prevent overuse injuries. But we’re finding that the kids are now playing in multiple leagues concurrently. And because there isn’t any interaction between the leagues, none of them knows the true total number of innings or games Johnny pitched during the week.”
The problem is exacerbated by parents, coaches, and others who tend to view child athletes as miniature professional athletes, and so are inclined to push the players into circumstances and situations where overuse can occur, Hagen contends. “A child who is exceeding the limits of his immature physical structure is a prime candidate to suffer debilitation as an athlete,” he says.
One reason so many athletes—young and old, amateur and professional—turn to the UPMC Center for Sports Medicine is that it is exceptionally good at restoring range of motion, strength, and proprioception, along with providing functional training, so that patients can once more engage in cutting, running, jumping, pivoting, and other high-stress-inducing maneuvers.
Toward this end, the center uses an array of electronics to analyze gait and extremity movement; however, the rehab team there uses modalities only sparingly. “We’re very hands-on oriented here,” Hagen says, “and we take a holistic approach to treating our athletes. We don’t look at the problem as just a knee or a shoulder or what have you. We look at what activity the athlete needs to do to return to function, what requirements the whole body will have. Then, to accomplish that, we use a lot of exercise supplemented with manual therapy. We like using weights, resistance bands, and stabilization-promoting therapy balls—especially in the at-home regimens we give to our athletes.”
Modalities that do get used include heat, cryotherapy, and electrical stimulation (the latter mainly for muscle reeducation). Continuous passive motion is sometimes used postoperatively on ACL and hip arthroscopy patients. There even is a video-game-style functional leg press machine that enables computer-guided isometric and progressive resistance exercises.
Staff physical therapist Erica Baum Coffey, MS, PT, SCS, tells of a recent interesting case in which both the hands-on approach and modalities played a role. The patient was a high school football running back who sustained extensive tears of his ACL, MCL, PCL, and medial and lateral meniscus when a teammate failed to block a hard-charging tackler from the opposing squad. “Following surgery, he was in a telescoping extension lock-splint brace for 8 weeks,” Baum Coffey says. “We began his physical therapy at about 2 weeks postop, and started by providing some ultrasound to help control the pain he was experiencing in his MCL; this allowed him to tolerate the patellar mobilizations and stretching necessary to restore his range of motion.
 |
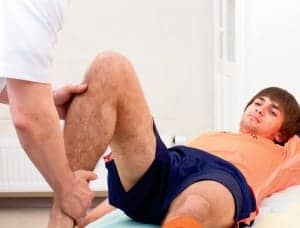
| The staff at UPMC’s Center for Sports Medicine practice a hands-on approach. |
“Throughout the time he was under our care, we also provided some heat therapy and cryotherapy. However, we had a really hard time restoring his motion,” she says. “That led his physician to attempt a manipulation under anesthesia, and I performed patellar mobilizations in the OR after the physician had achieved full range of motion. This then required seeing him every day for about 3 weeks afterward, during which time we did a lot of hands-on things, such as soft tissue and joint mobilizations and, for the strengthening of his quadriceps, some electrical stimulation. Every time he came in, we measured range of motion to monitor his progress and be able to tailor the session accordingly.
“Once we got him to the place where he had sufficient motion to permit the introduction of strengthening work, we had him perform limited-range knee extensions, leg presses, step-downs, and lunges—but no hamstring curls since we needed to protect his PCL repair. Later we added treadmill work, starting with walking and then increasing over a period of time to light jogging—we often use deweighting systems with our treadmills, but didn’t feel it was necessary in this instance. Stationary biking was also part of the therapy mix to condition him and help with range of motion. We eventually got him back to where he needed to be.”
Baum Coffey also treats many dancers and gymnasts. “For them, bracing and taping are used, but not a lot,” she says. “On those occasions when I do use bracing and taping, it’s most often to address ankle sprains and patellofemoral pain.”
KEEPING THE TALK GOING
Much research takes place at both the UPMC Centers for Rehab Services and the UPMC Center for Sports Medicine.
“Each year we try to build on the prior year’s research successes by introducing more innovation in our approaches to rehabilitation generally and sports medicine in particular,” Hagen says.
A notable piece of research recently emanating from the Center for Sports Medicine involved an investigation into the causes and treatment of low-back pain. “We’ve long been exploring the value of tailoring treatment to the individual patient, rather than treating everyone with the identical protocols,” says Irrgang, who, until last September, held the position of vice president for quality improvements and outcomes before agreeing to become director of clinical research for the Department of Orthopaedic Surgery. “We try to classify patients into treatment categories. In December 2004, Annals of Internal Medicine published our paper that detailed a methodology we devised to identify and validate which patients with acute low-back pain would best respond to mobilization or manipulation of the spine.”
Within the parameters of the sports program, Hagen bears responsibility for making most of the day-to-day decisions affecting the center’s conduct of business. He also helps shape its strategic plans in concert with Fu; James Terwilliger, MPH, UPMC vice president of operations; and Paul Rockar, UPMC Centers for Rehab Services Chief Executive Officer.
Among the key challenges being addressed by this leadership team is communication. “Our biggest concern is making sure our multidisciplinary approach is working as it should, that everyone involved is working together to provide a cohesive service,” says Hagen. “The reason it is a challenge at all is that our center providers are essentially independent business units. So, what we find we must do is continually strive to have good, across-the-board communications and encourage our teams to interact through meetings, voice mail, e-mails, Listserv, and any other channels at our disposal. The goal is to have the injured athlete’s full set of needs identified and then bring all appropriate resources into play—which can happen only if we’re all talking to one another.”
REIMBURSEMENT ISSUES
Insurance represents another challenge, although in Pennsylvania the situation is a bit improved since carriers in the Keystone State have switched en masse from requiring preauthorizations to the less cumbersome model of fixed-visit limits. Hagen says, “On the front end, there’s less paperwork before we can start treating the patient. But on the back end, there’s very, very little room for negotiation as far as obtaining insurer permission for additional visits the patient might need. It’s frustrating, but the workaround we’ve adopted involves taking a much closer look at how we can best utilize the allotted visits to get the patient to a functional stage and return him back onto the field. And, again, it’s crucial to have superior communication with all of the providers who will be working with the patient.”
Success begets success, which is why the UPMC Center for Sports Medicine still finds itself in expansion mode. “We’re continuing to open satellites to provide physician and rehabilitation services in more communities surrounding Pittsburgh,” Hagen offers.
Indications are the welcome mat is out for UPMC wherever it goes. Says Fu, “The Center for Sports Medicine attracts local, national, and international patients and hundreds of elite world-class athletes, and we’re proud to be there for them.”
Rich Smith is a contributing writer for Rehab Management.