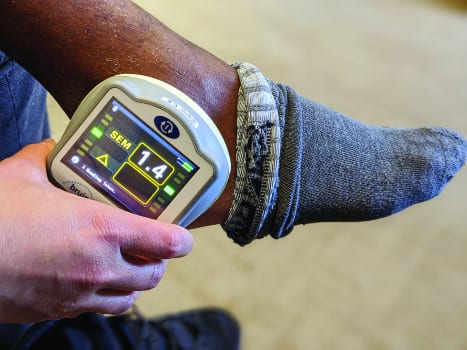
photo caption: Pressure mapping systems can provide active wheelchair users with visual feedback of pressure through the ischial tuberosities and sacrum while they are sitting. They are helpful assessment and education tools for pressure reduction and cushion prescription.
by Quyen Nguyen Catania, PT, DPT, CWS, CLT
In the United States, approximately 291,000 individuals are living with a spinal cord injury (SCI), with 17,730 new cases occurring each year.1 Septicemia, including infections from pressure injuries (PrIs), remains one of the leading causes of mortality in clients with SCI.1 PrIs involve localized damage to the skin and underlying soft tissue, usually over a boney prominence or related to a medical device, as a result of intense and/or prolonged pressure or pressure in combination with shear.2 Clinicians in outpatient settings often lack the required resources and have inadequate support to implement PrI prevention strategies. Once a client discharges to an outpatient setting the focus usually shifts to improving mobility, leaving skin health to become a secondary focus.
Despite these challenges, outpatient clinicians may have the greatest impact as they often follow clients throughout their life spans with regular opportunities to educate and reinforce interventions for PrI prevention. This article will present evidence-based research about methods to alleviate risk of PrI development and provide outpatient clinicians with effective PrI reduction interventions.
Mitigating Risk of PrI
Physical and physiological changes in clients affected by SCI place them at greater risk for PrI development. Decreased strength and range of motion, impaired muscle tone, altered sensation, and increased reliance on a wheelchair for mobility can lead to shear with transfers and seating-related PrIs. Clients with SCI have less muscle tissue volume beneath their Ishcial Tuberosities (IT) while sitting compared to those without SCI.3 This reduction of muscle and fat volumes can cause tissue deformation and ischemia-related tissue damage. A key component to decreasing risk of PrI development in the active wheelchair user is to minimize pressure and/or shear under the sacrum, ITs, and coccyx.
Weight shifting: Weight shifts should occur every 15 to 30 minutes and last for 1 to 2 minutes.4 Weight redistribution can occur in full forward lean, full lateral lean, or use of power seat functions such as tilt or recline. According to a study published in 2014, regardless of the cushion used (air, foam, or gel), pressure-relief maneuvers have been shown to increase blood flow and reduce interface pressures.5
Skin care: Visual inspection is recommended for active wheelchair users.4 A mirror should be used to check boney prominences daily for areas of redness; even blanchable redness should be reported to healthcare providers and monitored closely. Furthermore, education to promote proper skin care should be provided, including using mild soaps and pH-balanced moisturizers to promote optimal skin health.
Wheelchair prescription: It is well established that comprehensive and individualized evaluation is required for prescription of seating surfaces. MRI imaging of six participants and six cushion varieties found great variability in cushion effectiveness.6 Individualized wheelchair systems can decrease PrI risk by reducing tissue strain, regulating skin temperature, and minimizing moisture.7,8
Seated posture: The correct seating system can diminish sitting pressures and correct flexible asymmetries or accommodate fixed ones.7 Decreasing sacral sitting alone can reduce contact pressure on the back and boney prominences on the buttock while sitting in the wheelchair. The improved pelvic posture can also reduce shear forces generated on the ITs during wheelchair mobility.9

Potential Interventions for the Clinician
Outcome measures: Outcome measures should be performed at evaluation to determine a client’s risk for PrI development. The Braden Scale is a commonly used and validated outcome measure for PrI prediction.10,11 Braden subscales shed light into PrI risk areas including sensory perception, moisture, activity, mobility, friction, and shear. The Spinal Cord Independence Measure-III (SCIM-III) is a self-report assessment containing items on self-care, respiration and sphincter management, and mobility.12 These two outcome measures are valuable resources to identify key risk factors to address during the client’s bout of care.
Pressure mapping system: In comparison to individuals without neurological injuries who shift weight six to 10 times per hour, individuals with SCI perform on average less than one pressure relief per hour.4 Impaired sensation on the buttock decreases the feedback to move. It also reduces the incentive to offload, as there is little to no relief from moving.4 Pressure mapping not only provides clients with visual feedback to stress the importance of off-loading but also shows them the degree to which they need to offload. Often, effective pressure-redistribution strategies require full forward lean (trunk resting on distal thighs), full lateral lean (full off-loading of ipsilateral buttock), or full recline and tilt using the power functions.5
SEM Scanner: PrI etiology are bottom up rather than superficial top-down tissue injuries. Visual skin assessment (VSA) is often unreliable as it often detects damage too late and has decreased accuracy with patients with darker skin colors.13 The SEM Scanner is a good tool for PrI reduction as it can detect small changes in extracellular fluid, which increases during the inflammatory process of tissue injury. In fact, SEM readings are abnormal 2 days before VSA indicated tissue damage.14 Clinicians can use the SEM Scanner as an assessment tool to determine which PrI-reduction strategy is most appropriate.
Education: In-services are paramount for any setting as staff members can disseminate knowledge to clients and caregivers to mitigate PrI risk in the home and community settings. Wound and skin specialists should promote evidence-based practice to help clinicians identify and deliver individualizing interventions focusing on the PrI risk areas. Increasing awareness of skin integrity and decreasing shear during therapeutic activities, such as wheelchair mobility and transfers, can help to decrease risk of therapy-related PrI. Prophylactic dressings and padding should be used to reduce pressure over boney prominences during therapeutic interventions. Finally, periodic reassessment through use of performance improvement projects can help to create a sustainable PrI-reduction program.
Wound care: Once a PrI has been identified, management and treatment vary according to the characteristics of the wound. Throughout the healing process, the wound should be assessed two to three times per week by a wound care specialist. Dressings are selected to optimize wound closure, decrease maceration, and increase patient comfort. Modifications to the plan of care are often needed to enhance benefits of therapy while protecting the wound. Finally, education is provided to the client and caregiver to improve off-loading in the home and community settings to increase healing time and reduce reoccurrence.
Conclusion
Up to 95% of adults with an SCI will develop at least one PrI in their lifetime.15 In the outpatient setting, comprehensive history-taking and skin assessment can shed light into the client’s daily routines, mobility, and nutritional status to help identify PrI risk factors. PrI development, prevention, and treatment is individualized to each client. Collaboration between the interdisciplinary team, including nursing, medical staff, dietary, physical and occupational therapy, case managers, and social workers, is essential to customize strategies to reduce PrI development while improving mobility to fit each client’s needs. RM
Quyen Nguyen Catania, PT, DPT, CWS, CLT, graduated from University of Notre Dame with a Bachelor of Science and Washington University in St Louis with her Doctorate in Physical Therapy. She obtained her Certified Wound Specialist in 2016 and Certified Lymphedema Therapist in 2017. She is currently a level III physical therapist and has been an integral part of creating and expanding lymphedema and wound care services at Kennedy Krieger Institute, International Center for Spinal Cord Injury. For more information, contact [email protected].
References
1. National Spinal Cord Injury Statistical Center. (2019). 2019 Annual Statistical Report. Birmingham, Alabama: National Spinal Cord Injury Statistical Center.
2. Edsberg L, Black J, Goldberg M, et al. Revised national pressure ulcer advisory panel Pressure injury staging system: revised pressure injury staging system. J Wound Ostomy Continence Nurs. 2016;43(6):585-597.
3. Marin J, Nixon J, Gorecki C. A systematic review of risk factors for development and reoccurrence of pressure injuries in people with spinal cord injuries. Spinal Cord. 2013;51:522-527.
4. Vos-Draper T, Morrow M. Seating-related pressure injury prevention in spinal cord injury: a review of compensatory technologies to improve in-seat movement behavior. Curr Phys Med Rehabil Rep. 2016;4(4):320-328.
5. Sonenblum S, Vonk T, Janssen T, Springel S. Effect of wheelchair cushions and pressure relief maneuvers on ischial interface pressure and blood flow in people with spinal cord injury. Arch Phys Med Rehabil. 2014;95(7):1350-1357.
6. Brienza D, Vallely J, Karg P, Akins J, Gefen A. An MRI investigation of the effects of user anatomy and wheelchair cushion type on tissue deformation. J Tissue Viability. 2018;27(1):42-53.
7. Hsu TW, Yang SY, Liu JT, Pan CT, Yang YS. The effect of cushion properties on skin temperature and humidity at the body-support interface. Assist Technol. 2016;29:1-8.
8. Krey HC, Calhoun C. Utilizing research in wheelchair and seating selection and configuration for children with injury/dysfunction of the spinal cord. J Spinal Cord Med. 2004;27(1):29-37.
9. Kamegaya T. Influence of sacral sitting in a wheelchair on the distribution of contact pressure on the buttocks and back and shear force on the ischial region. J Phys Ther Sci. 2016;28:2830-2833.
10. Mortenson WB, Miller WC. A review of scales for assessing the risk of developing a pressure ulcer in individuals with SCI. Spinal Cord. 2008;46(3):168-75.
11. Garcia F, Pancorbo P, Soldevilla J, Rodriguez M. Risk assessment scales for pressure ulcer in intensive care units: a systemic review with meta-analysis. Gerokomos. 2013:24(2): 82-89.
12. Fekete C, Eriks-Hoogland I, Baumberger M, et al. Development and validation of a self-report version of the Spinal Cord Independence Measure (SCIM III). Spinal Cord. 2013;51:40-47.
13. Kim CG, Park S, Woon Ko J, Jo S. The relationship of subepidermal moisture and early stage pressure injury by visual skin assessment. J Tissue Viability. 2018;27(3):130-134.
14. Gefen A, Gershon S. Measuring subepidermal moisture to detect pressure injury. Ostomy Wound Manag. 2018;64(9):12–27.
15. Marin J, Nixon J, Gorecki C. A systematic review of risk factors for development and recurrence of pressure injuries in people with spinal cord injuries. Spinal Cord. 2013;51:522-527.
Determining the Best Cushion for Your Client
This is what therapists should know about dynamic cushions and the protection they provide against pressure injury
by Justine Kohlman and Siiri Koski
Medical professionals who work with individuals affected by a mobility impairment oftentimes are faced with making equipment recommendations for patients and clients who have complex needs. To satisfy those needs over the long term and optimize quality of life for this population, those medical professionals sometimes will need to recommend vital equipment that includes wheelchairs and wheelchair cushions.
Regardless of whether the wheelchair is a power or manual device, one of the single most important components in the overall seating and mobility solution is the wheelchair cushion. No wheelchair component has such a substantial impact on the end user’s health or is more important in preventing pressure injury. In fact, the cushion often may be the only form of protection between a metal seat pan and the soft tissue of the end user’s posterior and boney prominences.
See the Complete Picture
The therapist or seating specialist must look at each patient individually to assess their overall health in order to determine their specific needs. Once this assessment is completed, the clinicians should investigate what is best for their clients. When choosing a component as important as the wheelchair cushion, decisions should not be made in haste. A cushion should never be recommended based on which cushion is easiest to order or which cushion typically has been recommended in the past. When prescribing a wheelchair cushion, medical professionals must consider the benefits of the cushion as well as the end user’s physical and mental abilities to perform cushion maintenance and pressure relief.
Pressure Injury Can Be Fatal
When adding a static (non-moving) wheelchair cushion, the end user is required to perform effective pressure relief every 20 minutes or as prescribed. They are required to physically lift themselves up to relieve the constant pressure applied by a static cushion. It is important to keep in mind that tilt-in-space or reclining may not provide effective pressure relief. Clinicians must make their clients aware that work is required with static cushions, whether air, foam, or gel. If it is determined that the wheelchair user cannot relieve pressure effectively, relying on a static cushion puts that person at great risk of developing pressure injury. It should be known that pressure injury is caused by unrelieved pressure and can be fatal. Every static cushion—whether air, foam, or gel—requires the end user to generate his or her own pressure relief to avoid pressure injury.
Optimized Pressure Mapping
Pressure mapping is often used to determine which wheelchair cushion should be prescribed. When using a pressure mapping device, it must be properly calibrated to ensure accurate results. An uncalibrated pressure mapping device can skew the results by as much as 50%. Pressure mapping devices need to be calibrated on a regular basis even if not in use. If a cushion decision is made based on inaccurate readings, the resulting decision could have long-lasting negative effects.
The full scale on a pressure mapping device must be set to 200 mmHg. Professionals should be aware that there are brands of pressure mapping systems that let the operator set or change the scale. Changing the scale of the device offers inaccurate readings to the client. Any device that is not regularly calibrated or full scale serves no purpose in choosing a cushion.
Pressure mapping is truly a snapshot in time. When a therapist manipulates an air cushion—for example, by having the client lean in just the right position to find a favorable pressure reading—that pressure reading will change when the client moves even slightly. Pressure mapping sessions need to be taken over time to allow for immersion or changes in body position. The slightest movement will affect the pressure mapping. Not using a pressure mapping device in the way it was intended is a waste of the client’s valuable time and resources.
A Cushion That Heals
Pressure relief is essential in avoiding pressure injury, and a static wheelchair cushion that by nature is unable to offer any pressure relief is unlikely to offer significant benefit in the fight against pressure injury. Aquila Corporation, headquartered in Holmen, Wis, took up the challenge of developing a wheelchair cushion that could actively work to reduce the development of pressure injuries. As a result, the company has manufactured a wheelchair cushion designed to aid in the treatment and prevention of pressure injury. These cushion systems are designed to provide protections against pressure injury that are not achievable with static cushion technology, and to be particularly useful to mobility device users who cannot effectively perform pressure reliefs.
Aquila cushions are backed by the findings of a substantial number of clinical studies and are documented to have healed pressure injuries of all stages, including stage IV injuries.
A recent article published in Rehab Management examined pressure injury and clinical considerations for wheelchair cushion prescriptions. In their discussion about cushion materials currently available, the authors describe air, gel, foam, and honeycomb—all of which are static cushions. Missing from this discussion was dynamic (moving) cushion technology—an important type of product available for use in complex seating solutions. To offer therapists and medical professionals the full view of wheelchair cushion technologies, it is important to know the risk of pressure injury associated with static cushions and understand the clinical benefits that a dynamic cushion can provide
Mature, Proven Cushion Technology
The Aquila automatic, alternating, custom-fabricated wheelchair cushion has been available for 21 years. It has been the subject of several studies in peer-reviewed journals and has had more clinical studies than any cushion, whether static or dynamic.
One possible reason this category of cushion may be overlooked in clinical discussions about wheelchair seating is that there are ineffective, even harmful versions of alternating cushions on the market. There are meaningful differences in the design, materials, and function among dynamic wheelchair cushions that are currently available, so therapists must be mindful to educate themselves about those differences. This includes reviewing the published data that back up the technology’s performance and supports the effectiveness of its customized features. Even though there are a number of dynamic cushions on the market, what distinguishes the Aquila cushion is that it is the only dynamic cushion that is custom made to offload under an existing pressure injury or compensate for boney prominences. The effectiveness of Aquila’s dynamic cushion is underscored by its use in published clinical studies and the fact that it has been issued a Medicare code. Likewise, the Aquila dynamic cushion is distinctive because it is custom programmed for client weight. All other dynamic cushions apply upward pressure directly to an existing pressure injury, which common sense indicates, will cause the injury to worsen.
Evidence-Based Value
Healthcare professionals who work with mobility device users and make recommendations for wheelchairs and seating products should be mindful that unrelieved pressure to the skin and tissue is the number one cause of pressure injury. It is to the benefit of all therapists to search out wheelchair cushions that have been used in clinical research and proven to aid in the treatment and prevention of pressure injury.
Aquila continues to work to deliver on its mission to offer its clients the cushion that will best meet their specific needs. To maintain a superior level of quality and performance each cushion is handcrafted according to client specifications, which includes building a client’s cushion in any size or shape. The company’s customization service includes hand sealing each bladder in a client’s cushion for the exact size, shape, and location while off-loading under any specific injuries. Customization continues with programming the circuitry to offer three firmness options based on client weight and offer 60-second cycle times. Aquila actively engages in discussion with its clients to fully understand their needs and use their input to build a seating system that is optimized specifically for them. Aquila also maintains a personal file for each client that keeps their vital information available for continuing use. Above all, the company strives to place a singular focus on the care and comfort of its clients. RM




