
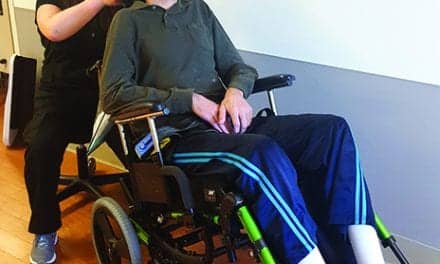
Cara Masselink, MS, OTR/L, ATP, confers with Mary Free Bed Rehabilitation Hospital patient June Bosbous about how power elevating leg rests, along with tilt and recline, significantly reduce pressure.
by Cara Masselink, MS, OTR/L, ATP, and Matthew Lefevre, PT, ATP
Technology only works when it is used correctly. Complexity, user abilities, miscommunication, or lack of education all can contribute to improper use of mobility devices. Since individuals affected by disabilities often have reduced financial means, they may be unable to easily replace or modify ill-fitting or poorly recommended equipment. Because of these circumstances matching mobility technologies to user need—while minimizing risk of abandonment—is an essential part of practice.
In the past 5 years, the wheelchair industry has been significantly affected by technology’s influence. While this is good in many respects, new products and accessories come with additional responsibility. For example, the practicing therapist needs to ensure the equipment will improve independence and function in patients’ lives, seamlessly integrating into their daily routines, roles, and responsibilities. In addition, the consistent change in technology has surpassed the ability to gather and analyze scientific evidence to direct best practices that justify implementation and optimize delivery and training. Because of this, many insurance companies are skeptical about the need to fund new technology.
When considering new equipment for patient use, the therapist’s background interests and personal familiarity with technology is helpful, but lack of specific knowledge of available products and their advantages and disadvantages can lead to inappropriate product recommendation and, ultimately, equipment abandonment. In this article, the current state of manual and power chairs, device and environmental accessibility, and custom products is reviewed, as well as practical points to ensure best outcomes.
Manual Designs: for Better Health Materials Matter
Lightweight and stable are two qualities that manufacturers strive for when designing manual folding wheelchairs. Less heavy materials are being used, including lighter-weight aluminum, carbon fiber, and titanium. Less weight leads to reduced force required when pushing, reducing the risk of shoulder pain or injury due to overuse, and improved ability to propel for longer periods of time. In other countries, lighter-weight wheelchairs are encouraged for the geriatric population in long-term care settings to enable more functional wheelchair mobility. These wheelchairs are expensive but worth the investment if distance is improved and users participate independently in activities over a full day without pain.
While weight is critically important to most users, adjustability also is a vital piece of the manual mobility puzzle. Extremely light chairs often have fixed seat heights that sacrifice adjustability while chairs with full adjustability, including center of gravity and back rest, will be heavier. However, new advances are focusing on providing the user the compact package of a folding wheelchair with the rigidity of the rigid chair with new designs. To meet these needs, new designs include the appearance of dual tube frames and innovative crossbraces engineered to limit flex. Some manufacturers are looking at standing as well.
New models of manual wheelchairs incorporate standing features that the user can manipulate as well, improving health with reduced UTIs, increased bone density, and greater functional reach, as well as other positive effects that come from being at the same level as peers during social interaction. Particularly important for pediatric users has been the focus on chairs that can increase in certain dimensions to accommodate the user’s growth. As insurance companies begin to require a specific amount of growth for pediatric chairs prior to authorizing the equipment, this is a necessary feature.
Power Assist for Manual Mobility
Typically used as an add-on to the manual wheelchair to reduce repetitive upper extremity use, power assist technologies can improve distance and endurance with propelling. Power assist systems have been available for years, but recent advances have improved how they operate. As a result of advances in manufacturing methods, the weight of the systems has decreased, making them more accessible to users. Likewise, at least one manufacturer has used advances in electronics and communications technology to link a wheelchair power assist system to the user’s smartphone via an app. The app enables the power assist wheels to deliver increased power and speed when needed, as well as improve balance assist and power when battery life is low. The app puts control over several key functions into the hands of the wheelchair user, including the ability to control the wheels when the wheelchair is unoccupied. This feature permits the wheelchair user to use the app to retrieve a chair that has been moved out of reach.
Technological advances that have been introduced to power assist systems may also result in improved function with adjustable speed, power, and response that better compensates for variations in surfaces and the environment.

Amy Ortego, OTR/L, ATP, and Andrew Davis, ATP, observe Sylina Pryor testing technology with supervised freedom, which aids users’ decision-making and reduces risk of equipment abandonment.
Power Mobility Sophistication Grows
Technology has infused today’s power mobility devices with the highest level of performance yet for this category. Manufacturers have focused on structural refinements that improve ride and responsiveness, such as equipping models with fully independent suspension to absorb variations in terrain with minimal translation. In some cases, the chassis has been made more rigid in addition to refinements in center of gravity to create a smooth ride. Improvements such as the ability to make adjustments to shock absorbers while remaining in the chair promotes user independence while technology that assures six wheels remain on the ground during climbs of up to 2 inches helps improve safety.
Drive systems have also advanced, and today’s mid-wheel configurations offer turning radiuses as tight as 20 inches. The power available to drive the devices has also benefited from technology improvements, such as the use of four-pole motors to provide high levels of torque.
Among power wheelchair users, power seating options may be perceived as being equal in importance to the chair’s power base and maneuverability. Significant refinements in seat elevation and anterior tilt have led to improved function and independence for power mobility users. For example, power wheelchair users now have options available that provide higher seat elevation than what was previously available. This feature can provide greater access in the community and improve transfers. Likewise, anterior tilt is a feature that improves transfers and users’ reach that is available on some systems. In terms of control, complex access methods and refined setup processes have resulted in improved functionality of head array, single switch scanning, sip and puff, and chin-controlled joysticks.
Manufacturers are offering greater options in programming that allow equipment to be operated by individuals who, several years ago, would have been unable to do so. Settings and even apps available through certain manufacturers allow the therapist to program the optimal tilt and/or recline combination for maximum pressure relief, as well as notify the person for and time the duration of pressure relief. The position required to achieve optimal pressure relief would be best determined during a clinical session with a pressure mapping system. This reduces users’ questions about how far to tilt and/or recline, as well as for how long. Users and caregivers receive a considerable amount of information when a new wheelchair is delivered and, thus, this reduces an important piece of information that could be forgotten or misunderstood.
Power wheelchair manufacturers are tapping into technology for consumers as well. Many have configured upgraded displays (typically available on wheelchairs that have tilt, recline, or seat elevation) for built-in Bluetooth connectivity and environmental control without additional accessories that would have been required a few years ago. As the accessories were difficult to fund through insurance, this opens access for computer use, tablet use, and phone use through the wheelchair controls for many people. The net result is an improvement in safety and independence as well as the potential for competent users to decrease reliance on caregivers.
Soon to be released are macro buttons designed to be used on the wheelchair display, where a switch can be plugged in to execute a multistep action with one activation. For example, moving the wheelchair into the optimal pressure relief position or answering a phone through Bluetooth will be possible by the user making a single tap. While this is promising and exciting for people with complex limitations, therapists should be aware that functionality across wheelchair providers differs and is limited to the user while in the wheelchair itself.
Custom Creations
While commercial options have greatly advanced in variety and usability in the last few years, some mobility device users need custom equipment to accommodate for significant scoliosis, pelvic obliquity, or other physical abnormalities. When insurance funding is needed, noncustom options must be trialed first. But, if all other “more cost-effective options” have been ruled out and significant medical justification is provided, custom may be an option. Improved processes for capturing unique postures allow for delivery of a customized, shaped product anywhere in the United States. In addition, these products are lighter weight and look polished, a result of manufacturing advances. All of these features lead to better outcomes for the person with documented improved wound healing, temperature regulation, support, and function to reduce equipment abandonment due to improved overall fit of the system.
Equipment options also are expanding for people who are not dependent on insurance reimbursement and instead use payment from independent resources, grants, or crowdfunding. Device or equipment manufacturers as well as some DME companies have technical support ready and willing to delve into custom modifications. If the therapist is knowledgeable about the equipment and able to oversee the project to ensure compatibility with the patient’s need areas, a skilled tradesman without clinical knowledge may be an option. University programs, especially those in engineering and allied health, also seek to work with individuals through whom collaboration may lead to student projects. Pairing energized students with real-life problems brings to life the seriousness of accessibility and the difficulties faced by individuals affected by a disability. Many times these projects are completed in stages and progress along a relatively slow timeline. Thus, they can be a viable option for individuals who lack financial resources but have the potential to become more independent with a custom solution.
Do-It-Yourself and Unconventional Solutions
Along the same lines, a bit of Internet research can lead to do-it-yourself solutions. This “at-your-own-risk” option often involves community individuals or teams of people who come forward through charitable organizations or contests that summon innovative people to create unique solutions. Contests, often run by a local or national sponsor or a disease or disability-related association, aren’t as plentiful, but often progress along a faster timeline-sometimes as short as a weekend. When considering these options, choose reputable organizations and those associated with teams of professionals to ensure the mobility device user’s needs are met sufficiently and safely. Know that there is a variety of equipment, processes, and materials, and be sure to research the options to ensure the safety and function of the end product. Many people have good intentions, but without professional knowledge, the result of their work may be disappointing if not detrimental. It is important to consider follow-up support as well, as most custom equipment needs tweaking if used regularly.
Liability can be a concern for many clinicians and serve to limit patient outcomes. Liability concerns can be minimized when the following steps are followed:
1) Choose skilled providers. Ensure the professionals enlisted in the project are knowledgeable experts in the area they address.
2) If in doubt at any time, stop. Do not put your patient at risk!
3) Document clearly and concisely. If the custom equipment came under scrutiny, the court would look to ensure the therapist was practicing due diligence to ensure safety and support function for the patient.
To demonstrate, this documentation should include: the person’s needs list, the therapist’s intent for improved function and a logical thought process for how the custom equipment will work for the person, the equipment recommended (both the product names and accessories recommended, as well as modifications to be made), the collaborating skilled providers and their role in the project, training and education provided to the patient and caregiver, as well as demonstration of appropriate use before discharge from therapy.
Minimizing Equipment Abandonment
To reduce equipment abandonment, utilizing a solution-oriented approach is important. Looking at the person first, their specific goals and current problem areas will help the therapist determine what product is going to “fill the gap.” A concrete, measurable “needs list” is important for keeping the patient and therapist on the same page, as well as to balance priorities when considering the options. In the age of technology and branding, it is easy to be swayed by the appeal that can surround new products. The reality, however, is that a patient’s need for consistency supersedes a need for “latest and greatest,” and therefore a healthy skepticism of new products should be applied. That being said, many of the new products can be helpful when provided or recommended without bias.
Throughout the assessment, it also is important to assess for the “worst case” scenario. Wheelchair users often change, sometimes drastically, in their tone, endurance, and posture throughout the day. Positioning accessories, including laterals, hip guides, head rests, and foot plates, can be recommended to support head, neck, trunk, and leg positioning. The hardware on these pieces and parts has improved over time to be more durable and positional. When placing these accessories, it is important to ensure the pressure is distributed on the bony prominences. Positioning components can be used to reduce the patient’s postural deformities within their passive range of motion. When possible, the correction should be toward neutral to reduce forces on the patient’s body and eliminate further progression of the deformity. When placing the components, also consider trunk and hip rotation with lateral deformities. When present, the position of these components may need to be asymmetrical to accommodate for the rotation.

Leo DelCarmen, CTP, and Mary Hamell, COTA/L, ATP, carefully consider arm trough placement to improve comfort and reduce risk of pressure sores.
It Takes a Team
In conclusion, technology advances have refined many of the current options as well as supported the introduction of new products. With each product, always trial with the patient while therapist support is available prior to recommendation to ensure the best outcomes are attained. Remember, advantages and disadvantages exist to all equipment. Awareness, knowledge, and education will ensure the equipment recommended supports the mobility device user’s function and is actively used for many years.
As a mechanism to deliver these principles into practice, Mary Free Bed Rehabilitation Hospital in Grand Rapids, Mich, has established the OrthoSEAT department as a clinical team focused on providing therapeutic technology services. The team consists of professionals who have multiple focuses
yet are similarly minded, including specialists with environmental control and computer access, augmentative communication, driving, and mobility device selection and custom equipment.
A team of occupational, speech, and physical therapists, engineers, technicians, and upholsterers, in conjunction with outside DME vendors and product manufacturers, work with each person’s unique situation and needs to optimize function and independence through trials of commercial, disability specific, and custom equipment. Specializing in complex needs and out-of-the-box thinking, this team exists solely to support people’s comfort, function, and enable
independence. RM
Cara Masselink, MS, OTR/L, ATP, is Team Leader of the OrthoSEAT, Assistive Technology and Augmentative Communication department at Mary Free Bed Rehabilitation Hospital in Grand Rapids, Mich. In addition to performing Assistive Technology and Augmentative Communication evaluations and treatment for outpatients and inpatients, she teaches at Western Michigan University in the Occupational Therapy department part-time and is pursuing her PhD.
Matthew Lefevre, PT, ATP, earned a bachelor of science in biomedical sciences and master of science in physical therapy from Grand Valley State University. He is a physical therapist in the OrthoSEAT program at Mary Free Bed Rehabilitation Hospital. He has been a physical therapist for 11 years and has 8 years of experience in assisting patients with complex seating and mobility needs. He also has received further training and specialization as an Assistive Technology Provider. For more information, contact [email protected].






Such an amazing team at Mary Free Bed! We are so blessed to have them here in GR.