 |
Shortwave diathermy, an electrically induced heat application, is thought to be relatively new in the world of rehabilitation and therapy. On the contrary; diathermy has actually been around for quite awhile, although it fell out of fashion for a time. “I was trained as a PT back in the 70s with the full expectation that shortwave would be a part of our treatment regimen,” explains Pat Hoskins, MS, PT, who educates other therapists on treatment modalities in Hallmark Rehabilitation’s Pacific region. “In the mid 80s through the 90s, and even into the early 2000s, it kind of slid out of sight,” Hoskins says. The machines were a little tough to use, but there have been a lot of changes in the technology since then. “Back in the 70s, there was microwave diathermy and you needed to have a special room that would not allow radiation to leak out of it,” Hoskins says. “It was a big deal to do a treatment.” Hallmark Rehabilitation is a contract provider to nursing homes, offering therapy services and related personnel and management.
“Using the machines has become more simplified,” Hoskins says. When she learned to use them, they had to be precisely 6 inches away and perpendicular to the patient. It was complicated and thus fell out of favor. “Today, it’s just as quick and easy, if not easier, to do a treatment as it is the other modalities we might use like ultrasound,” Hoskins says. The reasons to use either treatment are fairly close; there are just different options available today.
HOW IT WORKS
Used to raise the temperature of soft tissue below the skin’s surface, “diathermy is similar to what you’d use a heating pack for, but the concept behind diathermy is a deeper heat,” says Brian Hagen, DPT, MS, OCS, FAAOMPT, clinical assistant professor, regional director, and facility director, CRS/UPMC, and program administrator, UPMC Center for Sports Medicine, Pittsburgh. In shortwave diathermy, he says, the therapist does not actually touch the skin. Rather, the energy field radiates through the tissue and causes electromagnetic heat. “Most [machines] are floor models and have a head that comes in various sizes,” Hagen adds.
In the unit that Hoskins uses, the exposed skin of the patient is protected by a layer of terry cloth toweling and the applicator head or drum is placed against the toweling. “That’s one way to treat somebody with diathermy,” she says. “There’s a second way where we utilize two large rubber pads and lay them on the patient with a little bit of terry toweling [as a barrier].
WHAT IT IS USED FOR IN REHAB
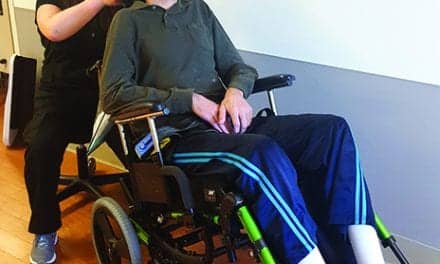
“In our setting, we’re training therapists to use it for increasing the elasticity of soft tissue, particularly in the nursing home, where joints are starting to tighten and you’re losing flexibility,” Hoskins says. “[We use it for] problems like inflammations with arthritis and the pain that accompanies them, damage to a ligament—if somebody twists a shoulder or turns an ankle—that type of tissue healing.” Hoskins notes that patients who have edema or a large amount of swelling from a contusion can benefit from diathermy as well. “Musculoskeletal pain, muscle spasms, chronic back pain that needs a good deep heat treatment,” she adds. “The thing unique to us is that we’re in nursing homes and are using it on a population that is probably not those typically perceived [as undergoing diathermy]. We look at the types of problems specific to an older patient or a more debilitated individual, so it’s not just a treatment for the young,”she says.
Diathermy is also known for increasing blood flow, decreasing pain, and speeding up the healing process, although there is not a lot of data to support its efficacy.
DURATION/FREQUENCY OF TREATMENT
“We’re actually using it as a primary, right-up-front treatment as part of the total plan,” Hoskins says.
Duration/frequency, Hoskins says, varies depending on the specific problem and how long it has been present. “The average treatment is probably somewhere from 20 to 30 minutes and could last over a course of several days if there’s a quick response, or up to several weeks,” she explains.
OTHER APPLICATIONS
“It is the single physical therapy modality that I use the most in my practice,” stresses Nancy Rowan Richards, DC, DABCI, FIACA. Richards is a Glendora, Calif, chiropractor/internist and uses diathermy to treat conditions such as pneumonia, and to help with liver detoxification and sinus infections. “It increases the white blood count and blood flow to the area, and for every 15 minutes of diathermy, you get a one degree increase in body temperature,” she states. “I’ve also been using it with one of my kidney failure patients to keep him from having to go the dialysis route. It’s been working quite well for him.”
Diathermy means deep heat, but these devices may also be used in a way that causes little or no heating. “You can set it up not to produce heat but still have the physical and mechanical effects inside your body,” Hoskin says. “You can have that very acute injury where traditionally we would say to put ice on it and keep heat away from it,” she says.
“We can still do diathermy very early on and try to control the situation and not let it turn into something that’s a long-lasting complicated-to-heal injury,” Hoskins adds.
CONTRAINDICATIONS
In 2002, the FDA issued a public health notification regarding diathermy interactions equipped with implanted leads and implanted systems with leads. The notice identified a risk of serious injury or death existed for patients with implanted electrical leads who were exposed to diathermy treatments. The FDA received reports in which patients with implanted deep brain stimulators died after receiving diathermy therapy. According to the FDA report, patient had received diathermy following oral surgery and the other for treatment of chronic scoliosis. In both cases, the interaction of the diathermy with the implanted device caused severe brain damage in the area where the lead electrodes were implanted.
“You can get burned,” Hagen says, but there are not many reported cases. “In the right hands, the risks are relatively minimal.
“You wouldn’t want to use it in any patient with metal or foreign bodies in the tissue such as pacemakers, over abscesses, or in those with cancer or metastatic disease, as well as over areas where there are spinal fluids, near the brain, ear, or healing bone, or with people who have sensory issues,” Hagen says.
Richards has a female patient who is paraplegic with an undeveloped sacrum and a rod in her spine. “Of course, she was wheelchair bound. She had a very stubborn kidney infection that would not clear up. We very carefully placed the pads and worked it so there was no danger to her prosthesis and were able to clear up her kidney infection in about a week,” she explains. “Yes, there are limitations to diathermy and you have to be cognizant of your patient’s medical history in order to use it effectively,” Richards advises. “It should not be used casually.”
TYPES OF UNITS
Some shortwave diathermy units are box-like and can be easily carried between treatment rooms when soft-rubber capacitive pads are being used. Others come with optional carts to provide a solid platform for the inductive coil drum electrode. Both of these types of devices have continuous or pulsed modes. Some advanced automatic tuning units have at least eight different treatment applicators, three inductive coil applicators, three spaced condenser sets, and two soft, flexible plate electrodes. Multijointed arms lock in place for ease of use and safety. A membrane panel and intensity control knob make treatment setups quick and easy.
THE FUTURE OF DIATHERMY
Apparently, there few companies that manufacture these devices. Richards has been in practice for 20 years, and early in her practice she bought six or seven of these machines—all the ones in use she could find. “For awhile, they would get repaired. I would order the vacuum tubes from Germany. The tubes were between $600 and $900, depending on which one you needed, and they came with no guarantee,” she says. Then, within the last 5 to 7 years, the German company went out of business and she couldn’t get them fixed anymore. “I teach doctors nationally, and they aren’t able to get the machines,” she says. ” I’m currently trying to negotiate with an engineering company to see if they can bring the technology back.”
AN INTERESTING SIDE NOTE
Shortwave diathermy’s roots actually go back to 1865 when the first studies in this field were made. It was the start of biological experimentation with heat production that resulted in high-frequency alternating current and the possibility of its utilization for medical purposes. The method gradually grew to placing two large flat metal electrodes, in two designated areas, directly upon the body surface. Then, in the 1920s, the object to be treated was put in a condenser through which a high-frequency current was sent. The electrodes were insulated plates, thus introducing a dielectric between the object treated and the metal electrodes. The first therapeutic application in human beings was in treating general paralysis.
When shortwave diathermy was first introduced, its undeniable advantages were constantly denied and its use deprecated by many outstanding physicians. This is by no means unusual. There has never been a therapeutic measure that, in its initial stages, has not had to suffer the skepticism of a conservative profession.
Nina Silberstein is a contributing writer for Rehab Management. For more information, contact .
Resource
de Cholnoky T. Short-wave Diathermy. New York: Columbia University Press; 1937.