 |
Occupational, physical, and speech language therapists are often asked to assist classroom staff, caregivers, and families in toilet training children with cerebral palsy. Here is a quick guide to how we can help.
Most children begin to gain daytime bladder control between 18 and 40 months (average age is 32 months) and bowel control between 16 and 48 months (average 29 months). A child with cerebral palsy usually lags behind these milestones because of poor postural control (inability to sit on a regular toilet), inadequate expressive communication skills, and delayed understanding or interpretation of sensations from smooth muscles.
Begin by charting out when the child urinates or has a bowel movement. By learning the child’s schedule and toileting behaviors, we can increase our success. Look for such things as facial expressions, posturing, and behaviors that precede voiding. Once we see these types of behaviors, or if the child lets the adults know when they are soiled, they are ready for toilet training. When a child reaches the age of 5, it is a good idea to have a trial of toilet training for 3 weeks, even if we have not seen signs of readiness. A severely involved child may have no way of letting us know that they “get it.” Potty training may be the child’s first opportunity to show us that they understand the world around them. If not, at least the child got to practice sitting and transferring.
Once we know when, during the day, the child moves their bowels, we target this time. Every day at the same time, sit the child on the toilet for 3 to 5 minutes. Make sure to record the results and when “accidents” happen. We are looking for a trend that shows we may need to move our trial time. With every success, reward the child.
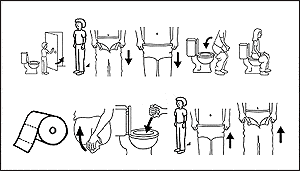 |
| Close door, stand up (from wheelchair), pull down pants, pull down underpants, sit on toilet, relieve self. Take toilet paper, wipe, put paper in toilet, stand up, pull up underpants, pull up pants. |
Never leave the child for an extended length of time (more than 10 minutes). If the child does not go right away, then when they do go, they may not associate the correct sensation with being on the toilet. Do not read books or sing songs, make it about the business of toileting. Breathing exercises may help relax the muscles and allow the sphincters to open. Slow exhalation coupled with slight flexion and forward leaning may help assist in the elimination process. Children with hearing or vision limitations can benefit from olfactory clues. Use a consistent strong smell that they can associate with toileting (eg, a coconut air freshener). Use an assistive communication system to explain the steps to the child. Use a separate system to help the child express their needs to use the toilet.
The Proper Accessories
A potty chair may be needed for children with poor postural control. Models are available with headrests, high trunk support, low trunk support, adductor pads (leg separators), splash guards (for boys), thigh supports, and/or footrests. The child needs to relax in order for the necessary sphincters to open. The first step is to stabilize the pelvis while allowing an open space in the right place. Supporting the thigh bones (femurs) is essential. Next, determine if your child voids best with hip flexion or extension. Many potty chairs position the child in a reclined position, not necessarily the ideal position for voiding. Most people prefer a forward leaning position with a closed hip angle. Firm foot support with mild to moderate knee flexion also seems to help. Sometimes a grab bar can be helpful for you to stabilize yourself, or for the child to do so as well.
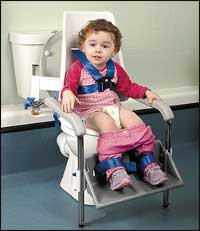 |
| Toilet training should begin early and be practiced often. |
One of the greatest gifts a caregiver can receive from a therapy team is a stand pivot transfer. Toilet training is a great opportunity to practice this. If we lift the child every time they need to get on the potty now, we will be doing it now and forever—when they weigh 80 pounds, and when they weigh 180 pounds. Start early and start now to teach the child to transfer with as little assistance as possible. Motor control researchers suggest that it takes a child at least 1,000 repetitions to learn a new skill. If we do one transfer a day, that means 3 years. If we help the child to transfer six times a day (three times on the potty), we are talking easy transfers in just 6 months!
If the child has been unsuccessful at potty training, another option is the standing diaper change. This technique allows us to change a child’s diaper without having to lift them. This is an advanced technique and takes time to learn (for both the adult and the child!). This is also a nice approach for older children and adults in public restrooms. My biggest nightmare would be to go in a public restroom and have to change a soiled diaper while the child lies on the floor. The best approach is to begin training early and often. The standing diaper change can be taught starting at age 2 to 5. It can be used in combination with potty training. Once the child has sat on the potty, instead of lifting them onto a changing table to put on the clean diaper, we have them stand while leaning on a low counter (or chair) or grabbing onto the transfer bar in the toilet stall.
Addressing Necessity |
The following protocol should be followed: |
|
Get ready. Put your wipes on the counter, get the clean diaper ready, and know where you are going to put the dirty one. |
|
|
There are a few different approaches here. The two main ones are the A) lean over the counter and B) hang onto the toilet transfer bar. I will describe both. |
|
|
For the counter lean, put down some towels on the counter or make sure it is dry and clean. Lean the child forward and keep your hand in the small of their back for balance. |
|
|
For the bar approach, have the child grab onto the bar, spread their legs slightly apart, and lean forward. |
|
|
Next, know what you are dealing with (urine or feces). If the diaper is soiled, open the fasteners (or tear the sides of a pull up) and let the diaper fall down so the contents aren’t spread around or forced into crevices. |
|
|
Clean and wipe all the places you need to. Boys and girls each have their own special issues. |
|
|
Now to rediaper, put the back panel on and use your knee to stabilize the pelvis while you reach around to fasten the front closures. |
|
|
To finish, dispose of any waste in the garbage can (not the toilet). Remember that it will take you over 1,000 trials to learn this new skill—so be patient with yourself! |
|
|
Don’t forget the transfer! Use a stand pivot approach and support the child as little as possible. This is an investment for the future. The less we lift now, the less we’ll have to lift later. |
|
An essential part of life
 |
| Efficient toilet training and bathing habits are an essential part of every child’s life, particularly those with disabilities. |
In conclusion, potty training is an essential part of life and is an educationally relevant activity. Given the proper equipment and strategy, many children with cerebral palsy can be potty trained. Last year I visited a cerebral palsy center in Dublin, Ireland, and was surprised to find that all the children who attended school were potty trained. This made me rethink my own experiences.
When I came home, I returned to the training I had received as a MOVE International Trainer, and worked with my team to implement a potty training program for all of the children with cerebral palsy. I was not surprised at our 50% success rate in children we had not previously expected to achieve this skill. Think about your case load, and choose one or two children. Over the next 3 months, implement a potty training program that includes minimally assisted transfers, a communication system, a chart that records the data, prizes for success (include Starbucks coupons for the adults doing the work), an appropriate potty chair, and a standing diaper change. Good luck! If you have any questions or can share your outcomes, please e-mail me at .
Ginny Paleg, PT, specializes in pediatric physical therapy in Silver Spring, Md. She works for the Montgomery County Infants and Toddlers Program at the ARC Daycare Center in Rockville, Md. She teaches continuing education courses for various equipment manufacturers and is the reimbursement chairperson for the APTA Pediatric Section. Paleg is a member of Rehab Management’s editorial advisory board.
BATH TIME FUN FOR CHILDREN WITH CEREBRAL PALSY |
|
|
Playing in the bathtub is a right of childhood. Every parent and child deserve the special bonding that occurs with water play and skin to skin contact. Bath time encourages communication, positive interactions, play, and relaxation. Baths have been shown to lower heart rate and blood pressure. Some families need a little help and a lot of physical support to simultaneously enjoy bath time and get clean. The first priority is safety. Safety is just as important for the child as it is for the parent/caregiver. A shower hose is a must for assisting anyone bathing. Remember to make sure sensitive areas never get too much water pressure, and that no-skid bath mats make for safer transfers and tub play time. Some children have trouble integrating sensory information. Warm water and predictable firm towel drying can help children interpret, organize, and tolerate touch and other sensations. If your child is tight, the bathtub is a great time to stretch. Remember that children with tone, spasticity, and/or dystonia need at least 6 hours to benefit from a stretching program, so after a bath is a good time to apply night-time splinting. Between bath and redressing is also a good time for stretching combined with massage. Children with cerebral palsy can benefit most from plantar fascia mobilization, and gastroc/soleus and hamstring stretching. Many children with cerebral palsy experience brief periods of serial casting. Plan ahead so the cast does not interfere with bathing and pool time. Most physicians, if notified ahead of time, can preorder Gortex underwrap. For an extra $40 (on average), this waterproof cushion—combined with a fiberglass cast—means worry-free and waterproof bathing and swimming. This system is not for children with open wounds—and there is an increased risk of skin breakdown—so caution is warranted. There are also reverse pressure cast covers that really work. These covers pump the air out of the cover and create a vacuum that keeps the water from both cast and limb. They are guaranteed to work in the pool, shower, or bath. In summary, bath time should be a fun and relaxing nightly ritual. To ensure safety for the child and caregiver, use an appropriate bath chair and a few simple adaptations to the bathroom. Have fun and splash away!
— GP |





