by Marie Spencer, RN, PhD, CRRN; Claudine Bogosian, MHA, OTR/L; and Stephanie Campbell, BSN, CRRN
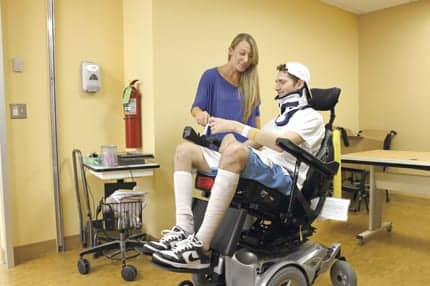 Lindsey Sergeant, MS, OTR/L, Senior Occupational Therapist, helps spinal cord injury patient Luke Moretti achieve the appropriate amount of tilt for pressure relief.In an environment where patients are less mobile and spend a significant amount of time in a bed, wheelchair, or other assistive device, the risk for pressure ulcers is quite high. Recognizing this risk, Burke Rehabilitation Hospital, a 150-bed acute rehabilitation hospital in White Plains, NY, dedicates a wound care team for each patient to prevent and reduce the occurrence of pressure ulcers. The team comprises physicians, nurses, physical therapists and occupational therapists, dietitian, pharmacist, and infection preventionist.
Lindsey Sergeant, MS, OTR/L, Senior Occupational Therapist, helps spinal cord injury patient Luke Moretti achieve the appropriate amount of tilt for pressure relief.In an environment where patients are less mobile and spend a significant amount of time in a bed, wheelchair, or other assistive device, the risk for pressure ulcers is quite high. Recognizing this risk, Burke Rehabilitation Hospital, a 150-bed acute rehabilitation hospital in White Plains, NY, dedicates a wound care team for each patient to prevent and reduce the occurrence of pressure ulcers. The team comprises physicians, nurses, physical therapists and occupational therapists, dietitian, pharmacist, and infection preventionist.
This team approach was instituted as part of Burke’s pressure ulcer reduction standard implemented in 2008. The creation of a standard protocol for assessing and treating pressure ulcers is the first step in improving pressure ulcer prevention and care.
INCREASING PROFICIENCY IN STAGING
In 2007, the National Pressure Ulcer Advisory Panel updated the staging standards for pressure ulcers,1 adding two new stages on deep tissue injury and unstageable pressure ulcers. To keep up with current standards, Burke amended its documentation and staging process to reflect the panel’s new criteria. Using the following guide, therapists and nurses categorize an existing pressure ulcer as:
• Suspected Deep Tissue Injury: purple or maroon localized area of discolored intact skin or blood-filled blister.
• Stage I: intact skin with non-blanchable redness of a localized area, usually over a bony prominence.
• Stage II: partial thickness loss of dermis presenting as a shallow open ulcer with red pink wound bed, without slough.
• Stage III: full thickness tissue loss. Subcutaneous fat may be visible but bone, tendon, or muscle is not exposed. Slough may be present. May include undermining and tunneling.
• Stage IV: full thickness tissue loss with exposed bone, tendon, or muscle. Slough or eschar may be present on some parts of the wound bed. Often includes undermining and tunneling.
• Unstageable: full thickness loss with the base of the ulcer covered by slough and/or eschar in the wound bed.
Increasing proficiency in the staging process, where nurses and therapists determine the severity of a pressure ulcer or the patient’s risk for acquiring a pressure ulcer, was very important in improving pressure ulcer prevention and treatment. However, even with the guide, staging still can be difficult because of its subjectivity.
To address that issue, the Burke nursing department put together a pressure ulcer team that created the Standards of Care, a guide that lessened subjectivity by using standardized checklists such as the Braden Scale2 for determining pressure sore risk and the Burke Skin Algorithm (BSA) flowchart for assessing sores. The BSA also contains prevention measures and treatment options for each stage of the wound. For those without wounds but are at risk for acquiring them, Burke clinicians follow the Braden protocols by level of risk.3 These prevention measures include:
• Using moisture barriers, a combination of hydrofiber and hydrocolloid dressings, to prevent friction;
• Ensuring underpads are not directly on skin;
• Frequent repositioning of patient to relieve pressure;
• Preventing shearing by making sure the head of the bed is not raised more than 30 degrees;
• Making sure shift reports are accurate and all members of the team are updated about the patient’s status;
• Daily heel checks; and
• Using elbow pads, bunny boots, etc.
The team consults with each other about the best approach for preventing pressure ulcers. Having the Standards of Care also enabled pressure ulcers to be treated as needed, without having to wait for a doctor’s order.
This staging process and pressure ulcer assessment is conducted by a nurse upon a patient’s admission and then again after 24 hours and 48 hours. When requested, the wound care team can do the staging during the admitting process. After the first 2 days, the pressure ulcer evaluation or rounds are then done weekly by the nurses, dietician, and physical and occupational therapists who are members of the wound care team.
PREVENTATIVE MEASURES
Along with proper staging, physical and occupational therapists are responsible for positioning the patient in a bed and/or wheelchair to reduce the likelihood of the patient developing pressure ulcers. To determine the best position, therapists take into account the following patient data:
• Medical status—current wound, risk for a wound, blood pressure changes, respiratory compromise, fecal and urinary incontinence, etc;
• Functional status—level of mobility, ability to perform activities of daily living;
• Physical status—posture, balance, muscle tone, range of motion;
• Patient goals—pressure relief, positioning, or a combination of pressure relief and positioning; and
• Patient comfort.
Therapists integrate all these considerations when determining the most appropriate type of chair cushion, wheelchair, and bed to ensure the patient is in the proper position. Whenever any of these factors change, the therapist will reevaluate the patient to see if their positioning needs to change as well. The therapists also take into account a patient’s nutritional status and hydration, which are additional risk factors for pressure ulcer development.
Therapists use numerous types of cushions—air, air-foam, foam, and gel—to help reduce the risk of acquiring a pressure ulcer and assist in wound care. The patient’s type of wheelchair and wheelchair back—linear or contoured, in a variety of composition types—also plays a factor in determining the type of cushion to use.
Patients have either power wheelchairs or manual wheelchairs that come in standard weight and ultra lightweight models. Both manual and power wheelchairs can be basic or highly customized with recline options as well as tilt-in-space maneuverability or both depending on the patient’s need. The ability to recline and tilt the patient in the wheelchair allows therapists to position them at optimal angles for therapy, mobility, and pressure relief.
Therapists also conduct pressure mapping for patients with stage III or stage IV pressure ulcers using a computerized pressure mapping tool that consists of a computer, pressure mapping software, a flexible sensor pad, an electronic unit, and a power source. This shows areas of pressure when the patient is positioned in their wheelchair and seating system—wheelchair seat, back, and cushion combo—and enables the therapist to determine the best system for each patient. In addition to patients with stage III and stage IV pressure ulcers, pressure mapping is completed for spinal cord and brain injury patients whose prognosis for ambulation is poor; those deemed high-risk for pressure sores; and those who rely solely on wheelchairs for mobility.
Like the wheelchairs, the beds at the hospital are specialized to reduce pressure ulcers. The nurses select the type of bed most appropriate for a patient’s needs and risk level for pressure ulcers. One type of bed4 is an air-filled mattress that uses an integrated pressure sensing system within the surface to redistribute pressure to the largest surface area possible for the patient. This enables pressure to be transferred from weight-bearing, bony parts of the body to other areas that normally do not bear weight, such as the lower back and calves.
The other type of bed5 helps prevent skin breakdown through various mattress options that are each designed for the patient’s level of risk or stage of pressure ulcer. Additionally, it uses nano technology to kill 99.8% of stain- and odor-causing bacteria, mold, and mildew on the surface of the bed. The bed’s repositioning feature also helps reduce shearing by keeping the patient’s hips in place while the back and foot of the bed are moved up and down.
Lastly, occupational and physical therapists regularly educate patients about pressure relief and pressure ulcer prevention.
CONTINUING EDUCATION
Therapists, nurses, and the rest of the clinical staff attend ongoing educational seminars throughout the year, and an annual pressure ulcer prevention day when all clinicians go through testing and educational courses. Continuous improvement goals and education help the clinical staff remain abreast of the latest pressure ulcer prevention and treatment techniques for all types of rehab patients. Burke’s therapists, nurses, physicians, and the rest of the wound care team work with patients who have varying levels of mobility, from all of Burke’s programs—Amputee Rehabilitation Program, Brain Injury Rehabilitation Program, Cardiopulmonary Rehabilitation Program, Single Joint Replacement Program, Neurological Rehabilitation Program, Orthopedic Rehabilitation Program, Spinal Cord Injury Rehabilitation Program, and Stroke Recovery Program.
With education and constant vigilance, the new pressure ulcer reduction program effectively brought the hospital’s acquired pressure ulcer rate to zero by the third quarter of 2011, and helped win the 2011 NDNQI Award for Outstanding Nursing Quality from the American Nurses Association. Burke was one of six hospitals out of 1,800 to receive this award.
Today, there is zero tolerance for acquired pressure ulcers
at Burke.
References
1. National Pressure Ulcer Advisory Panel. NPUAP Pressure Ulcer Stages/Categories. Available at: http://www.npuap.org/wp-content/uploads/2012/01/NPUAP-Pressure-Ulcer-Stages-Categories.pdf
2. Barbara Braden and Nancy Bergstrom, 1988. Braden Scale for Predicting Pressure Sore Risk. Available at: http://www.bradenscale.com/images/bradenscale.pdf
3. Barbara Braden, 2001. Protocols by Level of Risk. Available at: http://www.bradenscale.com/images/protocols_by_level_of_risk.pdf
4. Hill-Rom. The VersaCare A.I.R.TM Mattress Aids in Reducing Facility Acquired Pressure Ulcers. Available at: http://www.hill-rom.com/usa/PDF/142664.pdf
5. Hill-Rom. Easy to use. Safe for you and your patients. CareAssist® ES Bed. Available at: http://www.hill-rom.com/usa/PDF/CTG593.pdf
Marie Spencer, RN, PhD, certified rehabilitation registered nurse (CRRN), currently works as chief nursing officer and senior administrator at Burke Rehabilitation Hospital in White Plains, NY. She has been with Burke for 12 years and handles all aspects of nursing services.
Claudine Bogosian, MHA, OTR/L, is the assistant director of Burke’s Neuro Rehab Services. Bogosian specializes in brain injury and spinal cord injury rehabilitation. She has been with Burke for 16 years.
Stephanie Campbell, BSN, CRRN, assistant director of nursing, has been with Burke for 19 years. For the past 4 years, she has been an active member of the nursing wound care team, with primary focus on prevention and treatment of pressure ulcers. She also helped create the Burke Skin Algorithm, the standard guide to pressure ulcer treatment followed by the wound care team. For more information, contact [email protected].