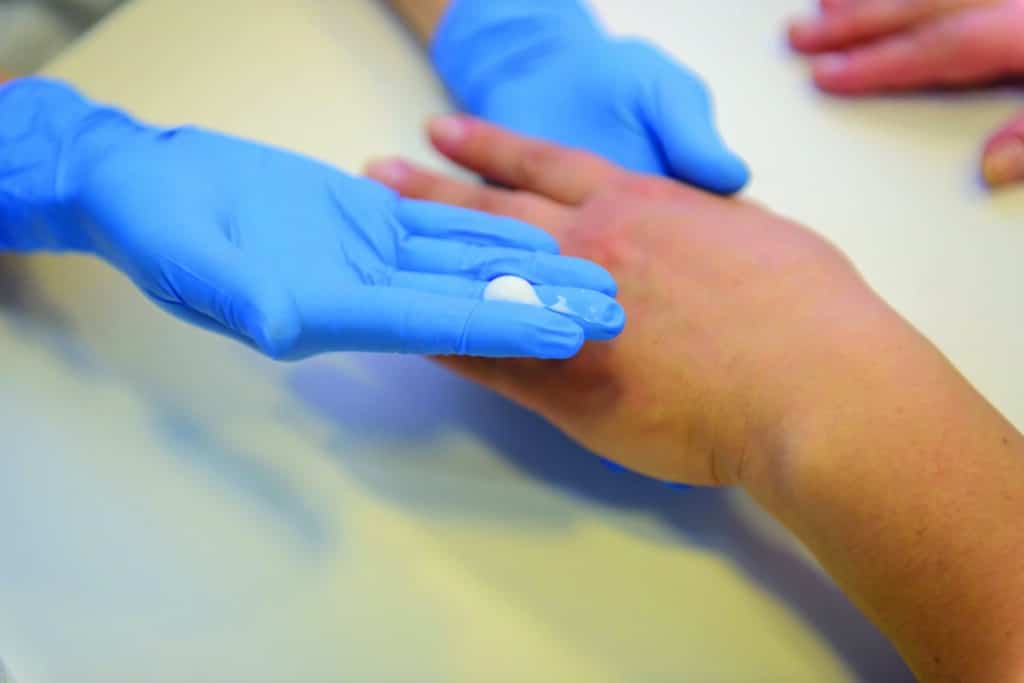
[PHOTO CAPTION: Pain is a complex phenomenon that can be influenced by multiple variables, including biopsychosocial factors. Therapists have many ways to approach pain management, including the use of modalities such as electrical stimulation.]
The purpose of physical therapy is to improve function and restore individuals to the level of activity needed to work, live, and play. Managing pain is a significant component of rehab with many tools to address pain and the perception of disability. Techniques and products created to address pain symptoms include heat and ice, dry needling, topical analgesics, massage, and modalities such as electro-stimulation. The pain-relieving effects of these solutions tend to be short-term. Exercise, stretching, and movement may offer more lasting relief from pain and provide tools that patients can use to self-manage their symptoms. The biggest component of rehab is education about pain and instilling confidence in a person’s amazing capacity to heal.
A Complicated Phenomenon
Relief from pain symptoms is one of the main reasons people seek out physical therapy. A long-held belief is that pain is the result of injury or damage to a person’s tissues, but in reality there is no simple explanation to describe the complicated and multifaceted origin of pain. We know that recovery from joint replacement can be very painful, but why do we feel more pain at night when trying to sleep versus in the day? Why does an old injury become achy when a person has the flu even after that injury has long healed? It is helpful to look at pain and its components to better understand the process and how the parts all contribute to the whole. So how do we feel pain?
Humans have no pain receptors other than the brain. The body’s nerves are designed to collect data and send it to the brain, where sense is made of the information and its meaning is interpreted. Have you ever watched an episode of the Discovery Channel series Shark Week and seen a surfer who reports paddling on the board, feeling a tug on their leg, and then reports feeling terrible pain after looking down seeing a shark biting them? Why was the pain only reported after seeing the shark biting on the leg?
What the shark bite incident demonstrates is that tissue damage may be perceived but may not even tickle a person’s awareness unless the brain decides that it is important. For example, standing causes compression to the tissues in our hips, knees, and feet, but the discomfort goes largely unnoticed with the strain not even registering on the radar of our conscious mind. We simply shift our weight to unload the joints while occupied with whatever task we are doing. While recovering from an injury or when the brain is very wary of an activity, we may be acutely aware of the pressure in the joints even though no actual damage is taking place. Pain is the nervous system’s way of sending a warning that bad things may be happening. Does that mean that pain is not real? Absolutely not.
Pain Is a Learned Experience
Pain is a physiological response to a perceived threat. It is real but not always appropriate. The human body is incredibly well engineered and it can heal or adapt from injury. Pain is completely appropriate to prevent further damage but may no longer be appropriate 6 months or longer after the injury has occurred. This type of pain is “persistent pain” and may require more careful examination into other factors that could be contributing to the pain. If pain is not coming from the tissues alone, where else can pain come from?
Pain is heavily influenced by our emotional well-being and our collected life experiences. Lack of good family support, stress over financial hardship, or fear of re-injury may escalate the perception of pain and complicate recovery. Pain researcher Lorimer Moseley hosted a TED Talk during which he shared a story about walking through the Australian outback, frequently feeling the sensation of brambles irritating his ankle when caught in his sock. One day, his brain was signaled by a sensation in the ankle with his mental map, thinking that he may have another bramble at his ankle. He was shocked to find that he had been bitten by a snake.
His recovery was long and painful, but he was able to return to everyday life, including his nature walks. On one walk, he reported feeling the searing pain of another snake bite only to find that it was just a bramble stuck in his sock. The stored memory of his pain from the bite was now a “lesson” that his brain had learned and the experience that his nervous system was using as the warning sign of potential ankle damage. The neural response was more significant than the less “dangerous” irritation of a bramble. Pain is a learned experience.
Biopsychosocial Factors of Pain
Pain is a unique and individual experience that comes from the brain. It is a response to signals from the body’s nerves, and is amplified or inhibited by the brain by stress and personal history. Pain is a warning sign but not a great indicator of actual damage. We have influence over the biopsychosocial factors influencing pain by seeking help from friends and family, getting good sleep and nutrition, and with introspection as to what is going on in our lives and if the pain we feel is appropriate to the actual harm that may be occurring.
There is no better illustration of how complicated a machine the mind is in mapping pain as “The Rubber Hand Experiment.” For this experiment researchers hide a subject’s hand behind a screen with a rubber hand positioned in view and use a feather to brush the rubber hand while the hidden real hand is also brushed. The subject’s brain associates the visible movement of the feather on the rubber as being done to that person’s own arm. The researchers suddenly take a hammer and smash the rubber hand as subjects perceive a threat of harm along with a physiological response to the rubber hand being hit.
A Great Comfort
The human machine is incredibly well-designed with tremendous capacity to recover and adapt. Most people who have sustained an injury or have had a surgery will recover over time, but there are those who may need a little extra from physical therapy to improve strength, range of motion, and the confidence to return to work, exercise, and daily activities. Physical therapy can be a great comfort to those with persistent symptoms with exercises and education to overcome and adapt to pain. RM
Albert Kaplan, PT, DPT, is originally from Cape Town, South Africa. He studied at the University of Florida earning a Master’s degree in Exercise and Sport Science, a Master of Science in Management, and his Doctorate in Physical Therapy. Kaplan has a passion for Orthopedic rehabilitation, particularly in the area of managing neck and back pain. He considers the interaction with patients as a rich and rewarding experience that fosters his continued practice and appreciation for physical therapy. For more information, contact [email protected].
More About Pain
The author of this article recommends these additional online videos as resources that can help clinicians expand their understanding about pain:
• Understanding Pain and What to Do About It in Less than 5 Minutes https://www.youtube.com/watch?v=cLWntMDgFcs
• Lorimer Moseley ‘Body in mind – the role of the brain in chronic pain’ at Mind & Its Potential 2011
https://www.youtube.com/watch?v=RYoGXv22G3k
• Rubber Arm Experiment | MAGIC FOR HUMANS
https://www.youtube.com/watch?v=xdxlT68ygt8&ab_channel=JustinWillman
Related Content:
Necessary But Insufficient: Guideline-Based Care for Pain Management
Pain Management: A Two-Sided Coin
Evidence Provides Excellence for Pain Management





