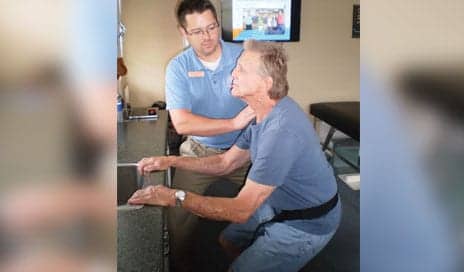
After house call visits, continued management of pain while restoring function is offered in an outpatient setting.
The healthcare and physical therapy industries anticipate significant changes in the near future, including harmonizing services for patient efficiency to improve outcomes, reducing expenses, and promoting self care. As a result, physical therapy outpatient organizations during the past few years have begun to offer house calls and home visits.
Strong evidence points our industry in the direction of our clients’ homes, including the need to help the ever-increasing population of aging clients who are affected by chronic pain, which can result in progressive weakness, loss of balance (frequent falls), and a fall-off in their indicators of general health. Tie that in with increasing numbers of physician-owned physical therapy practices and hospital-owned physical therapy centers—which can be quite difficult to compete with—and the benefits of a house call program begin to emerge.
These programs can serve as a significant competitive differentiator for a practice, if executed and delivered with an evidence-based approach. Although the cost to deliver treatment at a client’s home is higher than what is typically found in an outpatient scenario, a 15% profit margin for home treatment should be achievable.
House Call Services and Differentiating Programs
Typical house call services include therapeutic exercises, therapeutic activities, gait training, manual therapy, and pain management, while differentiating programs might include fall risk assessments and caregiver education.1
Physical therapists in the past have gone into home settings singly focused on the goal of getting the client out of the house, and enabling that client to attend outpatient therapy where more resources are available. Programs often included transfer training, gait training, step negotiating, bathroom transfers, and other tasks expected for home independence.
Nowadays, the profession observes a greater number of strategies directed toward use of outpatient resources such as therapeutic exercise (active, active assist, passive), manual mobilizations and manipulations, therapeutic activities (including bending, lifting, carrying, reaching, and overhead activities) to improve functional performance, and gait training for home management and safety. Ultrasound and electrical stimulation units may come to the home for the purposes of pain management or soft-tissue restrictions affecting function.
Pain Management To Go
Education is an additional component of house calls that falls to the role of physical therapists, most specifically in the area of pain management. Interdisciplinary pain management involves the client’s immediate and extended family, and a team of healthcare providers working directly with the person who is affected by pain with a variety of measurement, interventions, and strategies for self-management. It’s this self-management where physical therapists can make a difference. The types of noninvasive modalities offered to the clients at home include the following:
1) TENS units: for home and self-use, TENS is a noninvasive therapy indicated for the symptomatic relief from, and management of, chronic intractable pain and postsurgical and post-trauma acute pain. TENS is a safe and effective alternative to pharmacological approaches to pain control for many patients, while having it has minimal side effects and is nonaddictive.
2) Neuromuscular Electrical Stimulation (NMES) is a noninvasive, nonaddictive means of muscle rehabilitation after injury, surgery, or disease. Patients who are affected by a wide range of orthopedic and neurologic diagnoses can benefit from NMES, which applies customized electrical stimulus to cause a muscle to contract.
3) Heat therapy: the overall qualities of warmth and heat have long been associated with comfort and relaxation; heat can provide both pain relief and healing benefits for many types of pain. Superficial heat dilates blood vessels, increasing the flow of oxygen and nutrients; and stimulates the sensory receptors in the skin, decreasing transmissions of pain signals to the brain and partially relieving pain, while improving flexibility. Heat therapy in the form of heating pads, heat wraps, hot baths, and warm gel packs is both inexpensive and easy to do, and can be applied for education and offered as an additional revenue source for a house call program.
4) Cold therapy: Ice application slows the inflammation and swelling that occurs after injury; addressing the inflammation helps reduce the pain. Providing pain relief similar to a local anesthetic, ice slows the nerve impulses in the area, which interrupts the pain-spasm reaction between the nerves. An often-used product we are asked to provide and instruct is an aftersurgical cold therapy/vaso pneumatic unit.
Another pain-management solution can be found among topical analgesics. These products are typically easy to use and formulated as creams, gels, and sprays. They are widely available for over-the-counter purchase, and can be used as a convenient and affordable tool in achieving temporary relief from some types of pain.
Developing a House Call Program; Five Steps Toward Success
Implementing a new program within any organization may be the greatest endurance challenge a business owner ever faces. Owners and managers must be prepared to ready the ship fore and aft many times, as new tasks seemingly are added to their plates daily. Focused management on the utilization of the physical and human, while monitoring the processes, will help achieve the desired outcome, but—as Ringo Starr once sang, “It Don’t Come Easy.” Following are five steps that can help get a new house call program off the ground.
1) Find an “a-ha!” moment: In our house call program, smaller “a-ha!” moments occurred with discussions of accountable care organizations, Medicare fall risk information, and patient feedback. In our case, the loudest “a-ha!” occurred after past discussions and a phone call from a patient who was told to come for an office visit, but could not get out of the house.
2) Assess the need: Evidence remains abundant for the need, and perhaps chief among the pieces of evidence are the dangers of falling. A recent New York Times feature2 emphasized how dangers in the home are real. Deaths that occurred among individuals who experienced a fall reached nearly 24,000 in 2012, the most recent year for which fatality numbers are available. The 2012 statistic is nearly double the figure recorded 10 years earlier.
3) Assess how you can provide solutions: Physical resources are a critical component of a home program. However, the personal engagement skills that are part of the education and training physical and occupational therapists receive is what enables them to help their clients achieve higher levels of performance and function. The Centers for Disease Control and Prevention reports3 that one out of three adults older than age 65 years will fall each year. However, all too often the fall victims do not reveal to their family or health care provider that they have fallen. Physical and occupational therapists can get these folks to open up and talk about the fall, and share critical details associated with it.
4) Plan and implement:
a) Assess the local market: In your market, homecare agencies may dominate, often void of physical therapy pain management strategies or fall risk programs.
b) Assign resources: Physical resources allocated to a house call program may include modalities (ultrasound, electrical stimulations, heat, ice, and instrument assist for manuals), while expensive and sometimes scarce human resources are allocated in an efficient method.
c) Implement: Promotion and marketing begin early, and may or may not include website enhancements, promotional products (provided in-house or through printing services), press releases, open houses, and most importantly, one-on-one meetings with referral sources. Referral sources may include a variety of physicians, community organizations, and complementary businesses.
5) Evaluate: One to 2 months after implementation, perform a thorough evaluation to assess the profitability of the program. A simple SWOT (strengths, weaknesses, opportunities, threats) analysis should be performed to understand where more opportunity exists, and to target weaknesses. Hurdles are identified, policies are adjusted (which insurances may be accepted, and which direct pay programs), while the new evaluative period is established.
Revenue and Feasibility Outlook for House Call Programs
Change in strategies is necessary, since business models are different. Staff costs are higher, and likely a house call program will have the added costs of transportation, electronic documentation devices, and insurance. Strong strategies are necessary to enhance brand recognition and good will, including branded letterhead (card stock, home programs, fall risk assessments, education handouts on house safety, and instruction on pain management strategies and use of equipment).
Typical house call reimbursement will cover a therapist’s time, but managing the fixed costs of each visit will remain management’s largest hurdle to profitability. That being said, house call program profitability of >15% remains achievable in most markets.
Conclusion
For the Physical Therapy & Wellness Institute (PTW), it was our brand recognition and community good will, mixed with our slow afternoons and a meaningful “a-ha!” moment, that propelled us to plan and implement a house call program. The PTW house call program plan was conceived to clearly differentiate ourselves from traditional homecare services, and enable us to offer a program that better fills afternoon clinical hours, during which times the number of clients who come for in-clinic appointments may fall off.
To date the program has contributed to profits, while offering us the opportunity to discuss alternative pain management and home services that our referral sources have not typically had in the past. As in your own success, the success behind the house calls program at PTW will only be determined by the quality of care and solutions we offer our clients. RM
Robert Babb, PT, MBA, is owner and a practicing clinician at the Physical Therapy & Wellness Institute (PTW), with five locations in the Philadelphia region. More information about the organization and the house call program can be found at www.ptwinstitute.com. For more information, contact [email protected].





COMMENTI’ve been experiencing extreme back pain. Luckily, there is such a thing as cold therapy that uses ice, to slow the inflammation and swelling of the injury. I do hope that I will be able to find an in-home physical therapy service around here in San Diego.
Hello Rachel: There are many find PT providers in the San Diego area. I wish you success in finding a solution for your pain symptoms.
—Ed.
I would for someone to come and work with my mother in law at home. She is post CVA and uses a walker.
I would like to get a home physical therapist to come in my home and give my mom some therapist so she can start walking again she’s 90 yrs old.
I need a physical therapist that visit at home because my husband had been in bed for 4 month and he can not stand up. please respond ASAP we will appreciated very much.
my husband has been in bed for 6 monhs because of multiple health problems and has walked independently previously. please respond asap. this will be much appreciated.
We can’t recommend a specific therapist or clinic for this service, but what we can recommend is for you to contact your family’s primary care provider and ask for a referral to a clinic that provides home therapy services.
Best of luck to you.
—Editor
I am looking for a in home visiting physical therapist that accepts Medicare Medicaid insurance
Will Medicare and other insurances reimburse me if the treatment is not performed in my clinic? I assume with commercial payers, it is contract dependent. However, I am having a hard time finding out if Medicare will reimburse me if I am not a home health agency.
Good question, Karla. I will forward your question to the article’s author.
-Editor
Karla, the author provided this URL that responds to your question. Hope you find it helpful. https://www.medicare.gov/coverage/home-health-services.html
-Editor
My nephew has duchenne’s muscular dystrophy and needs PT . Do you know of anyone in Queens ,NY who can provide in home PT.
Thank you,
Bill
Bill, we are prohibited from providing any medical advice but my suggestion would be to contact the New York Physical Therapy Association to find out who provides this service in your area. You might also contact the MDA to ask about resources in your area. Try http://www.mda.org.
-Editor
Made it home help phone number 267 507 8485 name Michael Feinberg