
As many as 85% of diabetic ulcerations and amputations could be prevented with appropriate education and assessment.
As rehab specialists, we treat patients who have a variety of conditions and work to help them restore maximal function. One medical condition that is increasing in prevalence is type II diabetes. If current rates continue, the CDC predicts that one in three Americans will be diagnosed with type II diabetes by 2050.1 The physiologic changes that occur in the diabetic patient create a unique set of challenges for health care professionals. Long-term hyperglycemia can lead to a variety of pathologies in the autonomic, motor, and sensory systems. These pathologies, coupled with abnormal gait, lead to areas of increased pressure, which place the patient at high risk for diabetic foot ulceration. Treatment of a noncomplicated diabetic ulceration can cost in excess of $7,000.2 Complications increase the cost and may ultimately result in amputation. Development of a diabetic ulceration has both a functional and economic impact for the patient. However, studies show that as many as 85%2 of diabetic ulcerations and amputations could be prevented with appropriate education and an accurate ulcer risk assessment.
As a wound care specialist in a multidisciplinary wound clinic, I regularly treat patients with diabetes and see firsthand the life-changing impact of diabetic foot ulcerations. To facilitate healing of the wound and prevent amputation, we often recommend patients maintain non-weight-bearing status. We accomplish this with a variety of modalities, including total contact casting or other forms of aggressive offloading. However, for many of our patients, the recommendation to remain non-weight-bearing is not possible. We then work closely with the patient to develop a treatment plan that will allow them to perform needed tasks of daily living while optimizing healing potential. Many of the steps we take in evaluating and treating these complex patients can be implemented into general practice and help to prevent patients from developing ulcerations.
The first step we take in developing a treatment plan for a patient with diabetes involves completing a detailed evaluation and assessment. During the evaluation, it is important to obtain a thorough medical and social history. When reviewing the medical history, we note any cardiovascular disease, the presence of retinopathy, or nephropathy, as these often show the level of disease progression. We also ask about most recent hemoglobin A1C value, as this indicates how well the diabetes has been controlled during the past 3 months. For a patient’s social history, we look at ability to perform self-care and availability of resources to assist with care. Obtaining a smoking history is of importance, as vasoconstriction from tobacco will further complicate healing potential.
Following a review of the patient’s medical and social history, we move on to a foot examination. In particular, we assess for any trophic changes, such as thin/fragile skin, thickening of the nails, ingrown nails, dry skin, callus formation, and absence of hair. These findings demonstrate autonomic dysfunction occurring. Over time, autonomic changes can lead to dry cracked skin and a decreased fat pad on bony areas of the foot including the metatarsal heads and heel where high pressure is common with normal gait patterns. Along with foot examination, we palpate for peripheral pulses because it is common for diabetics to have ischemia. The presence of arterial disease increases the potential for ulcerations to develop. If the examination reveals diminished peripheral pulses, we refer back to the physician or complete an Arterial Brachial Index for further assessment.
The next step in our evaluation process is a formal range of motion and strength assessment of the foot and ankle. Along with standard ankle ROM and strength assessment, we include ROM and strength of the toes. Patients with diabetes often develop intrinsic muscle weakness that can lead to visible changes in the feet including hammer toe, claw toe, and bunion deformities. Diabetics often present with hallux limitus, in which the great toe does not extend beyond a neutral position. Hallux limitus can occur as a fixed or functional condition and directly impacts the force a person is able to generate in toe off phase of gait. As the disease progresses, patients can develop decreased dorsiflexion at the ankle, further impacting gait mechanics. A complete assessment helps us to identify underlying changes that are impacting functional mobility.
A critical step in identifying a patient’s risk level for developing an ulceration is the evaluation of the sensory system. We use a 10-point assessment on the plantar aspect of the foot with a 10 gram esthesiometer to objectively identify where the patient lacks protective sensation. A proprioceptive assessment of the ankle, foot, and toes completes our sensory examination and provides information about a patient’s risk for injury in the home. Range of motion and strength deficits coupled with decreased sensation and proprioceptive awareness increase risk for falls. Patients with diabetes are often vision dependent for balance so a review of the home to reduce fall risk is necessary.
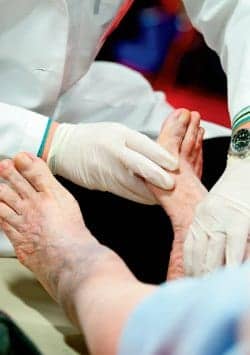
Over time, autonomic changes can lead to dry, cracked skin and a decreased fat pad on bony areas of the foot including the metatarsal heads and heel where high pressure is common with normal gait patterns.
Assessment of the patients’ footwear is the final step of our basic evaluation. Patients with diabetes often wear shoes that are too narrow for their foot, creating pressure points along the medial and lateral borders. Foot deformities such as claw toes place the patient at a higher risk for breakdown on the dorsal aspect of the toes if the shoes do not have adequate depth. Inspecting the shoes and inserts may also show areas of high pressure or wear patterns indicating abnormality in gait. We use this information to help identify areas of concern to monitor when we progress to formal gait assessment.
Once the basic evaluation is completed, a formal gait and balance assessment is done to identify any abnormalities. In our clinic, we utilize pressure mapping technology providing objective data to enhance our assessment. With a diabetic, one of the first things we look for is the areas of peak pressure. We begin with a barefoot assessment, for which the patient stands and walks over a sensor without shoes. The assessment allows us to identify how the foot functions without the accommodation of shoes and inserts. Once the data have been obtained, we progress to an in-shoe assessment. With sensors that are specifically designed to fit inside the shoe, we are able to assess the offloading effectiveness of footwear. We can use the technology to assist with redistribution of pressure by completing modifications to the inserts and loading more pressure tolerant areas, thereby improving the overall distribution of pressure on the feet.
Pressure mapping allows us not only to identify areas of peak pressure but to further assess gait dynamics. This technology enables therapists to complete side by side comparisons of progression from initial contact to terminal stance phase between right and left lower extremity. By comparing the center of force trajectory for asymmetry in timing, a clinician can identify functional muscle imbalances that need to be addressed. Using the technology, we are able to see in real time the effect of changes made to the orthotics with the goal of improving symmetry and redistributing pressure. We also use pressure mapping as a biofeedback tool, which allows patients to see the difference between barefoot walking and using recommended footwear. The ability to see a visual representation of pressure increases the likelihood of patient compliance with the use of diabetic shoesOnce the evaluation is completed, we are able to develop a treatment plan that helps achieve optimal outcomes. It is important to consider the findings from the evaluation when developing recommendations. If patients do not have the mobility to check their own feet, and no one to assist them, they may need to be educated about use of a mirror to complete foot checks. We also work to improve muscle imbalance and make recommendations for modifications to footwear that will reduce unnecessary and excessive torque and stress that occur with abnormal gait. If balance problems were identified, we begin a lower extremity and core strengthening program to improve postural stability and minimize risk of falls. Communication and the patient’s trust are key factors in achieving therapy goals.
The number of patients who have diabetes continues to increase. It is important to establish therapy as part of a patient’s multidisciplinary team. As therapists, we have a unique ability to assess gait and balance as they relate to a patient’s functional abilities. With the unique problems that occur in patients who have diabetes, we can make recommendations that help maintain and/or restore function. We can work in conjunction with patients’ medical providers to reinforce recommendations for daily foot checks and use of appropriate footwear. Together, we help to reduce the negative impacts of ulcerations and prevent amputations in the diabetic population.
Amy Bookless, DPT, CWS, is the lead therapist at Elks Wound Center in Boise, Idaho, where she treats patients who have chronic ulcerations. She is a board-certified wound specialist who has worked in the field of wound care for 4 years, and an APTA-certified clinical instructor. For more information, contact .
REFERENCES
- Centers for Disease Control and Prevention. Get the Facts on Diabetes. Available at: www.cdc.gov/features/diabetesfactsheet/. Accessed January 15, 2012.
- International Diabetes Federation. Position Statement: The Diabetic Foot: Amputations Are Preventable. Available at: [removed]www.idf.org/position-statement-diabetic-foot[/removed]. Accessed January 15, 2012.





