by John V. Rider, PhD, MS, OTR/L, MSCS & Kaila Patterson, OTD-S
Powered mobility can promote independence with daily activities, social engagement, and community participation and improve the quality of life for individuals with mobility limitations. Powered mobility devices (PMD), such as power wheelchairs and scooters, can provide independence that may not be otherwise possible for many individuals. However, some individuals may be overlooked when it comes to PMD evaluations due to cognitive impairments.
For example, healthcare providers, including occupational and physical therapists, may perceive individuals with cognitive impairments as unsafe and unable to use a PMD, dismissing the idea or an appropriate referral for further consideration of PMD use. Evidence suggests that cognitive functioning is one of the top concerns when evaluating someone for a PMD.1,2 Despite cognition being a significant concern for therapists, subjective clinical judgment is often the primary tool for determining whether an individual has the necessary cognitive functions for using a PMD safely and independently.1
Cognitive Skills for Driving a PMD
Driving a PMD device is a complex task. While the evidence is limited to what cognitive abilities are necessary for powered mobility independence, multiple cognitive outcomes have been found to be predictive of or associated with PMD use. For example, intellectual functions, visual and visuospatial perception, attention, abstraction, judgment, organization and planning, problem-solving, and memory have been found to have significant relationships with the ability to utilize a PMD for functional mobility.3 Therapists often consider cognitive functions necessary for driving a car—such as reaction time, attention, visuospatial capacities, executive functioning, and memory—when evaluating an individual for a PMD.3
Although specific cognitive abilities have been associated with PMD use, the research is unclear as to what level of cognition is required for the safe use of PMD. Furthermore, current PMD driving assessment tools, highlighted below, focus primarily on motor skills and performance-based outcomes rather than cognitive skills. It is important to assess motor skills and performance-based outcomes, including trialing powered mobility with the client; however, because of the uncertainty surrounding necessary cognitive skills, many individuals are precluded from powered mobility evaluations and trials early on in the rehabilitation process, even when they may have the necessary cognitive functions to use a PMD safely.
Power Mobility Driving Assessment Tools Available Online
- The Power Mobility Indoor Driving Assessment (PIDA)
- The Power Mobility Community Driving Assessment (PCDA)
- The WheelCon
- The Wheelchair Skills Test
- The Power Mobility Road Test (PMRT)
- The Functional Evaluation Rating Scale (FERS)
- The Powered Mobility Device Assessment Training Tool (PoMoDATT)
Initial Cognitive Screening
Suppose you are working in an inpatient or outpatient rehabilitation setting with a client after a cerebrovascular accident (CVA), and you think the client would benefit from a PMD. However, you are also concerned about the client’s cognitive impairments and whether they could safely utilize a PMD. Before dismissing power mobility, you can consider performing a simple cognitive screening.
At the most basic level, clients need to understand and demonstrate cause and effect, stop-and-go concepts, directional concepts, judgment, problem-solving, following directions, and motivation for PMD. Consider assessing these functions in the context of therapeutic activities throughout your treatment session. For example, you can assess cause and effect during a cooking task or a conversation about “what happens if…?” Directional concepts can be screened by having a client describe their home environment or the hospital/clinic. Judgment and problem-solving can be demonstrated through adherence to safety precautions and working through the steps of self-care activities. Simple discussions about how their life would differ with powered mobility and their interest level will help to understand motivation and insight.
If the client demonstrates these basic cognitive functions and would benefit from PMD use, complete a PMD evaluation or ensure a referral is made to the appropriate clinicians if you are not comfortable completing a PMD evaluation yourself. Data gathered from your cognitive screening can then be provided to the assistive technology professional (ATP), referring physician, and wheelchair assessment team and used for further documentation to support the need for PMD.
If you are still concerned about cognitive abilities, consider doing a mock trial in a manual wheelchair. This is a safe and accessible way to screen cognitive abilities related to PMD use. The therapist can act as the “power” for the wheelchair by pushing from behind, and the client can use a mock joystick to control the manual wheelchair. If the purpose is to evaluate cognitive abilities, the client could also indicate actions verbally (e.g., stop, go, forward, left, right, backward, etc.) or with hand signals. The therapist can then simulate the client using a PMD for a functional purpose to evaluate the client’s cognitive abilities in a safe and controlled manner (e.g., maneuvering the wheelchair around obstacles and to another room to retrieve something).
Standardized Cognitive Assessment
In addition to observations of functional performance during therapy and a mock PMD trial with a manual wheelchair, standardized cognitive assessments can be used to understand the client’s cognitive abilities better. Several cognitive assessment tools are available for individuals with neurological injuries or cognitive impairments and have been recommended throughout the literature.
For example, the Cognitive Assessment for Stroke Patients (CASP) is a standardized test that assesses a range of cognitive functions, including attention, memory, language, and visuospatial abilities, designed for individuals after a CVA and can be used to supplement observations of functional performance. The Repeatable Battery for the Assessment of Neuropsychological Status (RBANS) is another commonly used tool for assessing cognition in individuals with neurological injuries. The RBANS is a standardized assessment tool that measures various aspects of cognitive function, including memory, attention, language, and visuospatial abilities. The RBANS has been validated for use with individuals with a range of neurological injuries, including stroke, traumatic brain injury, and dementia.
Another commonly used tool is the Montreal Cognitive Assessment (MoCA). The MoCA is a quick and simple cognitive assessment tool that evaluates various aspects of cognition, including attention, memory, visuospatial abilities, executive function, and language. The MoCA is widely used in clinical practice and has been validated for use with individuals with neurological injuries. MoCA training and certification are required for the administration of the assessment. In addition to the MoCA, the Trail Making Test (TMT) has also been widely used with PMD assessment. The TMT is a two-part assessment that takes approximately five minutes to administer. Each part requires different skills, such as visuoperceptual abilities, sequencing, working memory, and task-switching. Clients are tasked with connecting numbers in part A and both numbers and letters in part B as quickly as possible while maintaining accuracy.
The results of these assessments can be used to determine the individual’s ability to operate a PMD safely. For example, if an individual has difficulty with executive functioning, they may have trouble with sequential tasks, such as maneuvering the wheelchair through a crowded area. If an individual has trouble with attention, they may have difficulty focusing on their surroundings while operating the wheelchair, leading to a risk of collision. The results can also be used to target and remediate specific cognitive skills in therapy to increase the client’s ability to operate a powered mobility device safely and independently.
While considering cognitive abilities, it is also important to recognize that despite physical limitations, if a client demonstrates sufficient cognitive abilities to operate a PMD safely, there are numerous alternative access controls that allow individuals of all physical abilities to control a PMD (e.g., head controls, chin controls, tongue controls, sip-n-puff controls, etc.).
Summary
This article highlights the importance of assessing cognitive abilities for the safe and independent use of PMDs. Cognitive functioning is a top concern when evaluating someone for a PMD and is often the primary reason healthcare clinicians decide not to pursue further PMD evaluations. Although the research does not provide a clear benchmark for the minimum necessary cognitive functions, occupational therapists can utilize a combination of screening tools, standardized assessments, simulated tasks, and observation of occupational performance to assess functional cognition and initiate the appropriate process for PMD evaluation. Given the importance of functional mobility for independence with daily activities, therapists can address specific cognitive functions necessary for PMD use through a remediation approach to prepare clients for safe PMD use.
John V. Rider, PhD, MS, OTR/L, MSCS, is an Associate Professor at Touro University Nevada in the School of Occupational Therapy and works as an occupational therapist in multiple settings, including primary care, outpatient, and home health. He currently runs a wheelchair clinic, performing complex rehab technology evaluations for clients with neurological involvement.
Kaila Patterson, BS, OTD-S, is an occupational therapy doctoral student at Touro University Nevada interested in functional cognition and improving independence through power mobility devices.
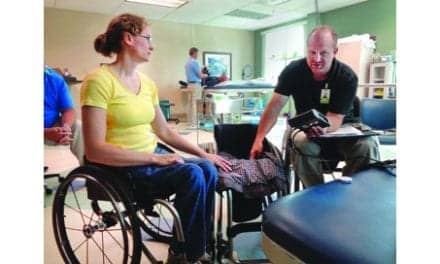
Caption: Testing a person’s cognitive abilities in a manual wheelchair is a safe way to evaluate if they would be able to handle using a powered mobility device. Photo: John V. Rider
References
- Maywald A, Stanley M. Prescribing mobility scooters in Australia: Occupational therapists’ narratives. Australian Occupational Therapy Journal. 2015;62(2), 86-92.
- Mortenson W, Clarke L, Best K. Prescribers’ experiences with powered mobility prescription among older adults. The American Journal of Occupational Therapy. 2013; 67(1), 100-107.
- Pellichero A, Kenyon L, Best K, Lamontagne M, Lavoie M, Sorita E, Routhier F. Relationships between cognitive functioning and powered mobility device use: A scoping review. International Journal of Environmental Research and Public Health. 2021;18(23), 12469.